Shakedown: Side Effects Of Levodopa
Hallucinations
Hallucinations and psychosis are a side effect of levodopa. They tend to manifest as disturbances of perception as opposed to sound. According to a report published last year in Psychiatric Times, Management of Psychosis in Parkinson Disease by Dr. Weiss and Sam Adler, MD, After having Parkinsons for many years, benign hallucinations occur in approximately 10% to 20% of nondemented patients with PD who receive dopaminergic treatments.
Christopher Hess, MD, assistant professor of Neurology at the University of Florida Center for Movement Disorders and Neurorestoration, says that after having Parkinsons for many years, some people feel like there is a presence in the house . Or it may be a passage hallucination, which Hess describes as fleeting images in the corner of the eye.
As dependence on levodopa progresses, visual hallucinations in direct vision occur. If the hallucinations are mild, says Dr. Hess, patients can stay on levodopa. But in rare cases, the hallucinatory experiences become increasingly vivid and frightening thats when the symptoms evolve into psychosis. Suspicions of harmful plots, spousal infidelity and financial impropriety are a common cluster of delusions encountered in patients with psychosis. In those cases, more monitoring is required, as well as a change in medication or dosage.
Typically, you need to hospitalize a patient till they are stabilized, Dr. Hess says.
Wearing Off
Involuntary movements
Treating Dystonia In Parkinsons
Treatment options for dystonia include:
- Dopaminergic medication adjustment as discussed above
- Botulinum toxin injections of the affected muscles
- Physical therapy to loosen and strengthen the dystonic body part
- Trying other medications that target the dystonia directly such as muscle relaxants or anti-cholinergic medications
- Use of a device to provide a sensory trick*.
- Deep brain stimulation can be considered in difficult-to-treat situations
*To minimize their dystonia, some people have success using an interesting tactic called a sensory trick. A sensory trick is defined as a physical gesture that mitigates the production of the dystonia. For example, touching the eyebrow may help keep the eyes open, or touching the chin may keep the neck from twisting. In my clinical practice, one woman wears metals rings on her dystonic fingers to help them assume a more normal position. Another man wears 5-toed shoes to prevent dystonic toe curling
Leg Pain And Parkinson’s
Interestingly enough, one of my early symptoms of the disease was deep searing pain in my left leg, the type of pain my grandma had complained about many times. Initially this type of pain was worst in the morning as well as at night, making me think is was some sort of fasciitis. However not only did typical anti-inflammatories and muscle relaxants not alleviate my pain but pain worsened over time to a constant burning pain that felt as if someone was tearing the muscle and pouring hot oil on it. The pain was so excruciating it was permeating into all aspects of my life. I was constantly in need of deep tissue massage asking my husband to massage my legs just as my grandmother had asked of us time and time again. This helped only temporarily.
Which brings me to the four types of leg pain in PD.
Also Check: Bryant Gumbel Health Parkinson
Second Type Of Leg Pain Is Caused By Dystonia
When related to levodopa, it usually occurs as a wearing off but can also occur at peak dose. In most cases this leg pain is unilateral and has direct correlation to medication intake. When pain is due to dystonia, it is more common in early morning. This type of leg pain is usually accompanied by toes curling and foot abnormally posturing.
The Preponderance Of Injury In The Past Of People With Pd

Neck issues or damage can be caused by injuries, but the injury site doesnt have to be local to the neck itself, since it is an integral part of the kinetic chain of the human body – problems anywhere else which affect posture can, in turn, profoundly affect how we tense our necks and cause strains on it by the way we are holding up the head. Ive frequently asked people with Parkinsons Disease to think carefully about any pains and injuries which they might have incurred either before or concurrent with their PD diagnosis. Ive found that the overwhelming majority of us have suffered a prior accident or physical trauma. Injuries to jaw, neck, shoulders, back, hips, knees or feet predominate. All these severely affect posture and hence the kinetic chain and are liable to make our necks prone to permanent strains and stiffness. So in my view, even if chemical cures were invented tomorrow, people with PD would still present with the postural problems, still suffer from the old injuries which have been masked by the narratives of neurology, and would probably quickly decline into pain and problems again, unless these past injuries are properly attended to.
Read Also: Can Parkinson’s Run In The Family
Low Blood Pressure When Standing
Orthostatic hypotension refers to a persistent drop in blood pressure that occurs when you move from sitting to standing, or from lying down to sitting up or standing. It can cause:
- dizziness
- headache
- feeling faint
OH is defined as a blood pressure drop of 20 millimeters of mercury in systolic blood pressure, or a drop of 10 millimeters in diastolic blood pressure.
How To Cope With Dystonia
I have PD. First thing in the morning as I am getting out of bed, my left foot cramps severely and my toes curl downward, making it very painful to walk. I have found that it helps if I put my feet flat on the floor immediately after sitting up in bed. Also foot massages help. If I can force the cramped foot so it turns outward, my toes uncurl. nelleford
When my dads legs cramp, massage helps relieve them. You can usually feel where the spasms are. Rub your hands together to warm them up first. Start below where the spasm is and work up towards them. With your fingers and palms, give a deep massage where the cramp is. Give your loved one mustard or pickles to relieve the cramp. I know it is weird, but it works. To prevent them, exercise is best. Try to get them to walk every day, even if it is only half a block. This will also help prevent falls. A good multivitamin every day can be beneficial. Look for one with magnesium and potassium in it. These minerals helps to prevent cramping. My dad eats bananas almost every day for this reason. kathyt1
Calcium governs muscle contraction, and magnesium governs muscle relaxation. I take a magnesium supplement if Im having leg cramps. Perhaps have your loved ones levels evaluated with a simple blood test. Potassium can be dangerous if its too high or too low, and too low can often cause muscle cramps. sherry1anne
Read Also: Parkinson’s Dementia Prognosis
What Causes Intercostal Muscle Spasms
According to rayur.com, intercostal muscle spasms can be caused by a wide range of issues from dehydration and electrolyte imbalance to multiple sclerosis, but most are the result of acute injury or chronic anatomical issues including genetics, poor posture, obesity, and weak core muscles.
Causes of injury include sudden or repetitive twisting motions such as swinging a golf club or tennis racquet.
Trauma such as impact with a steering wheel in a collision, or activities that put a significant strain on the chest, like doing bench presses or push-ups, may also be to blame.
In some cases, todays sedentary lifestyles are the problem. In this YouTube video, Dr. Alan Mandell explains how rib pain can occur as the result of sitting hunched over a desk all day, being overweight and having poor muscle tone in the back and abdomen.
Rarely, multiple sclerosis may be the of cause intercostal muscle spasms. According to WebMD, this is known as the MS hug.
Each person experiences this differently and while some people report pressure or a squeezing sensation around the ribs, others report more typical sharp or stabbing pain.
What tends to differentiate an MS hug from simple intercostal spasms is that it encompasses the entire span of the rib cage and is often described as wearing a girdle.
Similarly, muscle pain due to fibromyalgia, dehydration, and electrolyte imbalances are typically not limited to the intercostals.
How To Deal With The 6 Common Causes Of Leg Pain In Pd
Severe leg pain is a common complaint from people with PD. Lately, it is understood that central pain is common to Parkinsons disease, and can even be the first sign of PD, usually bilaterally. This blog post lists six causes of lower limb pain, and the importance of treating it. Treatments depend on properly identifying the source of pain. Some treatment suggestions are included.
Don’t Miss: What Are Early Warning Signs Of Parkinson’s Disease
Exercise Stretch And Strengthen
- Even if you dont feel like it, exercising every day can increase flexibility in your muscles and joints, reduce pain and discomfort, and improve circulation. Exercise can increase the secretion of your happy hormones, improve your mood, and decrease anxiety and depression.
- If you have discomfort in your calves, ankles, feet, or toes, and try the eight exercises physical therapist Sarah King recommends.
Treatment For Dystonia In Parkinsons Disease
The exact relationship between PD and dystonia remains unknown, which makes treatment challenging. The Parkinsons Foundation recommends tracking when dystonia symptoms occur in relation to taking levodopa, the most commonly prescribed medication for PD. If dystonia occurs when levodopa levels are low, such as upon waking in the morning, then your doctor may recommend adjusting the timing or dosage of your medication.
If occurs even when levodopa has achieved peak levels in your body, then your doctor may recommend injections of botulinum toxin to the affected muscles. Botulinum toxin relaxes muscles and makes it difficult for them to contract, even involuntarily. The injections are repeated every few weeks.
also has shown promise for relieving dystonia in Parkinsons disease . However, sometimes DBS can trigger a dystonia, such as eyelid twitching, so this treatment usually is reserved as a last resort.
As a symptom of Parkinsons disease, dystonia can inhibit you from pursuing physical activities you enjoy. But exercise and physical activity are powerful tools in managing PD. Work with your doctor to find medications that improve dystonia symptoms and keep you as mobile as possible. Staying active can help you maintain a high quality of life when living with PD.
Read Also: How Much Mucuna Pruriens To Take For Parkinson\’s
Stages Of Parkinsons Symptoms
Parkinsons symptoms can be divided into three categories or phases: pre-motor, motor, and cognitive. These phases dont necessarily happen in chronological order, and not all Parkinsons patients will experience all symptoms.
The premotor phase is the phase of Parkinsons in which non-motor symptoms are present. These symptoms include:
- loss of smell
- torso
- legs
There are two main categories of tremor: resting tremor, and action tremor. Resting tremor occurs when muscles are relaxed, like when your hands are sitting in your lap, and lessen during sleep or when the body part is in use. Action tremors occur with the voluntary movements of a muscle.
Tremors typically affect only one side of the body but may affect both sides as the disease progresses. Fatigue, stress, and intense emotion may worsen tremors.
What Are The Intercostal Muscles

The intercostal muscles are located between the ribs and stretch from the middle of the chest to the middle of the back.
There is 11 pair on each side of the rib cage and each is composed of three layers: the external intercostal muscles, internal intercostal muscles, and the innermost intercostal muscles.
According to the National Heart, Lung and Blood Institute, their primary function is to lend flexibility to the chest wall to help with breathing.
When air is inhaled, the intercostal muscles lift the rib cage, allowing the lungs to expand. When the muscles relax, the rib cage falls and the air is expelled.
Also Check: What Is Advanced Parkinson’s Disease
How Dystonia Is Caused In Parkinsons Cases
First and foremost, dystonia can be a symptom of Parkinsons disease itself. Particularly in young onset PD, foot dystonia may appear as the first motor symptom that is experienced. If dystonia occurs in isolation, the diagnosis of PD may only become clear as other symptoms appear. If dystonia occurs as the predominant symptom of PD, the patient and his/her doctor must decide how to treat it either by starting dopaminergic medications to see if this helps the dystonia or by targeting the dystonia itself, possibly with Botulinum toxin injections.
Once medications for PD have been started, dystonia may appear when there is a decrease in brain dopamine levels, which could occur first thing in the morning before taking medication or when a dose of medication is wearing off. If this is the pattern that is noted, there are various strategies that can be implemented to decrease OFF time. Depending on when the OFF time occurs, these approaches may include taking a long-acting Levodopa formulation before bed, increasing the number of doses per day or adding a medication to lengthen the amount of time that a dose works.
How Might Dystonia Be Experienced
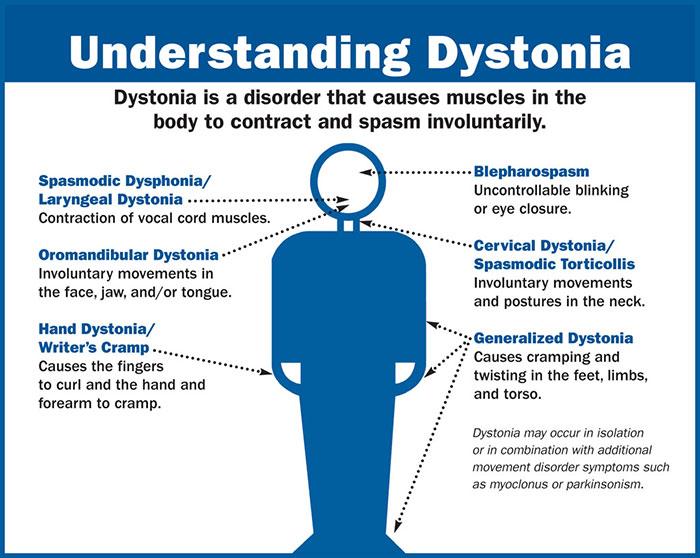
- Feet: people with Parkinsons mainly experience dystonia in their feet. Typically the toes curl up into a claw-like position, the foot turns inwards at the ankle, and occasionally the big toe sticks up. This position, caused by spasms in the calf muscles, can be very uncomfortable and makes it hard to fit feet into tight shoes.
- Hands: writers cramp in the hands only occurs during handwriting.
- Neck: cervical dystonia affects the neck muscles, which causes the head to twist to one side, forwards or occasionally backwards.
- Eyelids: the eyelid muscles may contract and make the eye close involuntarily . This is often experienced as excessive blinking, intolerance to light, a burning feeling in the eye or irritation.
- Vocal cords: dystonia affecting the vocal cords or speech muscles makes speaking difficult or strained.
- Jaw area and side of the face:oromandibular dystonia affects the jaw area, tongue, mouth or one side of the face. The jaw may be pulled either open or shut, and speech and swallowing can be difficult.
Recommended Reading: Parkinsons Disease Deaths
Opening The Medicine Box In The Mind: The Psychology Of Pain
In this 50-minute lecture, Beth Darnall, PhD explains how our experience of pain goes beyond the physical sensation of pain. It has emotional and psychological components that affect our ability to treat pain. She cites research to demonstrate that and shares 13 specific tips to reduce the experience of pain and increase treatment effectiveness. Audience questions follow the lecture.
Urinary Difficulties In Parkinsons Disease
The most common urinary difficulty experienced by people with PD is a frequent and urgent need to urinate. Urinary incontinence, the involuntary loss of urine, is also a symptom of PD. This may occur even when the bladder is not full. Recent research studies estimate approximately 27-39% of people with PD experience urinary difficulties, although urinary incontinence only develops in about 15% of those with PD. Bladder issues usually develop in the later stages of PD.2
There are several medications that can help manage urinary difficulties, such as tolterodine, oxybutynin, darifenacin, and solifenacin. These medications work to block or reduce overactivity in the bladder. However, these medications may make the symptoms of PD worse. It is recommended to discuss these treatments with a movement disorders specialist who has been trained to understand the effects of various medications on the disease.2
Recommended Reading: What Are Early Warning Signs Of Parkinson’s Disease
How Can I Help Myself
You will need to try a variety of sensory tricks to see what works for you as dystonia affects everyone differently.
Spasms may be reduced by touching the affected part of the body either before or during any movement known to trigger dystonia. Although this may not prevent or stop a spasm, touching can distract or trick the brain and reduce the length and intensity of a muscle contraction.
Simple massage exerting pressure on the foot, or the use of a hot water bottle or heated pad can also help, as can movement and exercise – see Coping Strategies – Tips & Tricks.
For eye spasms, some people find lying down, singing, yawning, laughing, chewing, putting pressure on the eyebrows or just talking can help. Spasms in the vocal cords may respond to yawning or sneezing.
Simply relaxing may also help so try taking a bath, having a massage or a calming activity such as yoga.
Pain In Parkinsons Disease
Parkinsons patients suffer from the same pain other people have, often amplified by the motor dysfunction, but they also have additional pain problems unique to PD. Lower back pain and back of he neck pain are most common. Strengthening exercises or stretching may be helpful. Identifying the cause of the pain is essential in treating the pain. Treatments include physical therapy, medications, and alternative therapies like Reiki, acupuncture and massage.
Also Check: What Is The Life Expectancy Of Someone With Parkinson’s Disease
My Parkinson’s Story: Pain
This 10-minute video alternates between an interview with a man and and doctors. The man shares his experience with pain as a symptom of Parkinson’s disease. The doctors explain that pain is common in Parkinson’s disease, often due to rigidity or dystonia, which can be exacerbated by “off” periods. Pain caused by Parkinson’s symptoms can be relieved by Parkinson’s medications, exercise, DBS and botox injections. Pain is an invisible symptom that should be mentioned to your neurologist.
What Are The Different Stages Of Parkinsons Disease
Each person with Parkinsons disease experiences symptoms in in their own unique way. Not everyone experiences all symptoms of Parkinsons disease. You may not experience symptoms in the same order as others. Some people may have mild symptoms others may have intense symptoms. How quickly symptoms worsen also varies from individual to individual and is difficult to impossible to predict at the outset.
In general, the disease progresses from early stage to mid-stage to mid-late-stage to advanced stage. This is what typically occurs during each of these stages:
Early stage
Early symptoms of Parkinsons disease are usually mild and typically occur slowly and do not interfere with daily activities. Sometimes early symptoms are not easy to detect or you may think early symptoms are simply normal signs of aging. You may have fatigue or a general sense of uneasiness. You may feel a slight tremor or have difficulty standing.
Often, a family member or friend notices some of the subtle signs before you do. They may notice things like body stiffness or lack of normal movement slow or small handwriting, lack of expression in your face, or difficulty getting out of a chair.
Mid stage
Mid-late stage
Standing and walking are becoming more difficult and may require assistance with a walker. You may need full time help to continue to live at home.
Advanced stage
Recommended Reading: What Are Early Warning Signs Of Parkinson’s Disease