What Happens During The Dbs Procedure
Most DBS procedures are performed with the patient awake under local anesthesia, with their head immobilized in a rigid frame, so that the surgical team can monitor patient response to the electrode placement as it occurs. A few centers are now offering image-guided placement, in which the surgery is performed under general anesthesia without the frame. The pulse generator is usually implanted during a second surgery, scheduled about a week after the first.
Pesticide And Herbicide Exposure
A strong link has been shown between PD and exposure to pesticides and herbicides. We need more Parkinsons-specific research to better understand what causes PD and to work to prevent it and help eliminate the risk of getting the disease, when it comes to all environmental risk factors and whether genetics can cause an increased risk in developing Parkinsons.
One herbicide that has been linked to Parkinsons is paraquat, a widely used commercial herbicide in the U.S. that is banned in 32 countries, including the European Union and China. The Parkinsons Foundation, along with the Unified Parkinsons Advocacy Council, signed two letters to the U.S. Environmental Protection Agency encouraging them to cancel the registration of paraquat based on strong scientific research linking the herbicide to Parkinsons disease. In October 2020, the EPA re-approved paraquat for use in the U.S. Without additional action, paraquat will remain legal for sale and use in the U.S. for the next 15 years.
Read Also: Stretches For Parkinsons Disease
Am I A Good Candidate For Dbs
To determine if you are a good candidate, you:
Page reviewed by Dr. Chauncey Spears, Clinical Assistant Professor and Dr. Amelia Heston, Movement Disorders Fellow at the University of Michigan.
Read Also: Does Parkinson’s Cause Memory Issues
What It Feels Like: Deep Brain Stimulation For Parkinsons Disease
Emma Jones,
Manzil Bacchus was diagnosed with Parkinsons disease in 2008. Initially, he was told that there was nothing he could do to stop the progression of the progressive nervous system disorder that affects movement. Manzil and his wife, Sadia, continued to manage the increasingly worrisome symptoms which included tremors and the growing amount of medication that he had to take each day.
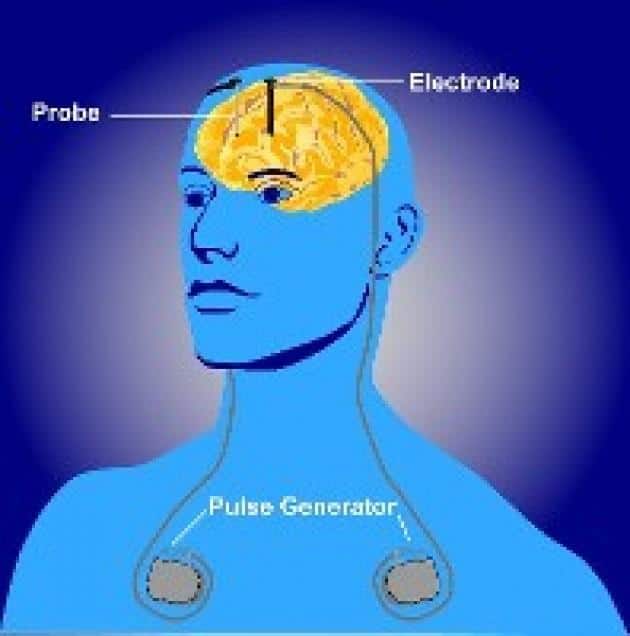
After Manzil was diagnosed with colitis, a chronic digestive disease that has been linked to Parkinsons, the family began investigating a new surgical option. In deep brain stimulation , electrodes are inserted in regions of the brain that have been affected by the Parkinsons, with an impulse generator battery also inserted in another area of the body. When turned on, the electrodes send gentle electrical pulses to help improve symptoms like tremors and motor control.
Manzil and Sadia sat down with Healthing to talk about Manzils experience having brain surgery during the COVID-19 pandemic and the difference that deep brain stimulation has made to his quality of life.
When was Manzil diagnosed with Parkinsons?Manzil: Back in 2007, my hands started shaking. I was volunteering at a mosque, helping people to take a pilgrimage in Saudi Arabia, helping with their application for visas and stuff like that. One of the girls noticed my hand shaking and asked why. I thought I was just tired. After that, I also noticed that my left foot was dragging when I walked.
Sadia: Sadia: Sadia:
Who May Benefit From Deep Brain Stimulation
![[Full text] Dopamine transporter changes after unilateral deep brain ...](https://www.parkinsonsinfoclub.com/wp-content/uploads/full-text-dopamine-transporter-changes-after-unilateral-deep-brain.jpeg)
A number of criteria can help identify people who are good candidates for deep brain stimulation. This includes people who:
- Have been living with Parkinsons disease for at least five years, though the procedure was approved for early symptoms in 2016 and is now being evaluated to see if it offers benefits for people earlier in the disease
- Have symptoms that are not well controlled on medications
- Are responding to Parkinsons medications : The procedure should only be done for people who are responding to this treatment, but the medication effects fluctuate during the day and the effectiveness of the medication is getting shorter.
- Find that the uncontrolled symptoms are lowering their quality of life
- Are doing relatively well cognitively
At the current time, there is no set age limit for DBS, but the effectiveness may be lower in older people.
Also Check: Can Parkinson’s Patients Take Melatonin
Search Strategy And Selection Criteria
References were identified by search of PubMed, Medline, and Scopus electronic databases published before July 2009 with the terms PD and deep brain stimulation, or subthalamic nucleus stimulation, or globus pallidus stimulation. Articles were also identified through examination of the reference lists of relevant publications and a search of the authors’ own reference database. Articles were selected for inclusion only if they provided UPDRS ratings before surgery and follow-up ratings with a final assessment a minimum of 3 years after surgery. Statistical variance, the number of subjects at each assessment period, levodopa-equivalent daily dosage, and stimulation settings were also required.
Thirteen observational studies fulfilled the selection criteria. Two of these studies were excluded16,17 because the population samples were subsets of the populations in 2 other articles that were included because they had larger sample sizes.18,19 Of the remaining 11 studies, 3 examined bilateral GPi, 9 examined bilateral STN stimulation, and 1 study included both STN and GPi target sites.19 In the Lyons et al.20 study, 3 of the 9 subjects had unilateral GPi stimulation but the results lumped the unilateral and bilateral cases. As there were so few studies of the GPi, this study was included but the reported effects may be underestimated for this reason.
Table 1 Clinical baseline characteristics of populations
New And Emerging Targets
Since, there is no consensus on the best target for DBS in PD and because no target is able to effectively manage all the patients symptoms and QoL over a prolonged period, newer targets and dual target stimulation is being investigated to improve PD outcomes in patients with refractory motor and non-motor symptoms.11 Stimulation of caudal zona incerta is associated with better motor control than best medical treatment .46 Dual stimulation of STN and cZI has been tried with better results that targeting individual regions.47 Also, Vim, PPN, and PSA are the newer targets found to be effective in different PD patient populations .11
Don’t Miss: What Is The Difference Between Parkinson’s Disease And Huntington’s Disease
Efficacy Of Local Versus General Anesthesia Techniques
A meta-analysis of 145 studies of DBS in PD showed that the mean target error was not significantly different between LA and GA however the mean number of DBS lead passes were significantly less with GA as compared to LA .62 Post DBS complications were significantly lower with GA . The two techniques did not differ significantly in UPDRS II scores off medication, UPDRS III scores off and on medication or LED. UPDRS IV off medication score decreased more significantly in awake DBS versus sleep DBS cohorts .62 Hence, most DBS procedures should ideally be carried out under LA due to the lower side effect profile.
What Happens During Deep Brain Stimulation
This procedure actually involves two to three surgeries that usually happen at different times. The first one or two procedures are to insert the stimulation leads into each side of your brain at the same or separate times. The second procedure is to implant the stimulator battery known as a pulse generator under the skin of your upper chest.
Before these surgeries happen, your healthcare provider will usually insert an intravenous line to give you IV fluids. An IV also allows them to give you medications during the procedure as needed.
Lead placement
This procedure usually starts with your healthcare provider shaving the hair on your scalp. This makes it easier to place your head into a special frame that will hold your head still. The frame is set with four pins in your skull. This is done while youre under sedation, and you likely wont remember this part.
Once the frame is set, theyll bring in an intra-operative CT scanner to take images of your brain and identify the trajectory used for the electrode placement. Once the CT scan is complete, the entry point is identified, sedation is turned back on and your head is cleaned with surgical prep. Local anesthetic is then injected to numb that area of your scalp and skull. Your neurosurgeon will then make a small cut .
Pulse generator placement
Don’t Miss: Can You Die From Parkinson’s Disease
What Is The Prognosis
Although most people still need to take medication after undergoing DBS, many people experience considerable reduction of their PD symptoms and can greatly reduce their medications. The amount of reduction varies from person to person. The reduction in dose of medication can lead to decreased risk of side effects such as dyskinesia.
There is a 1 to 3% chance of infection, stroke, bleeding in the brain, or other complications associated with anesthesia. It is best to discuss associated risks with your neurologist and neurosurgeon, as diabetes and heart and lung conditions all may influence these risks and the decision to pursue surgery.
Systematic Reprogramming Of Dbs Settings
This study demonstrated for the first time that a systematic evaluation and optimization of stimulator settings is valuable and may result in significant improvements 8 to 15years after surgery. These patients had been followed in our outpatient clinic on a regular basis. Nevertheless, we found an effect on the shortterm outcome, as a positive effect was seen on all UPDRS subitems after 2 to 5weeks.
An effect of systematic reprogramming has previously been reported also by Moro and colleagues14 in a younger group 3.5years after surgery. Of the patients, 89% received a new setting, and a sustained effect was found in more than half of the patients after up to 14months. In contrast, our group was older, and we demonstrated an effect of reprogramming in a group of more advanced patients with a mean stimulation period of 12years. The results have changed the treatment strategy in our clinic, where reprogramming has been implemented more regularly as of today and also after a long treatment period.
Also Check: Long Term Care Insurance Parkinson’s Disease
What Benefits Does The Procedure Offer
DBS is not a cure for Parkinsons, but it may help control motor symptoms while allowing a reduction in levodopa dose. This can help reduce dyskinesias and reduce off time. DBS does not usually increase the peak benefits derived from a dose of levodopa the best levodopa response before DBS is a good indicator of the best response after DBS. But it can help extend the amount of on time without dyskinesias, which may significantly increase quality of life.
DBS does not provide most patients benefit for their non-motor symptoms, such as depression, sleep disturbance, or anxiety. DBS also does not usually improve postural instability or walking problems. If a symptom you have does not respond to levodopa, it is not likely to respond to DBS.
Stereotactic Dbs Vs Interventional Image
Stereotactic DBS surgery requires the patient to be off their medication. During the procedure, a frame stabilizes the head and provides coordinates to help the surgeons guide the lead to the correct location in the brain. The patient gets local anesthesia to keep them comfortable throughout each step along with a mild sedative to help them relax.
During image-guided DBS surgery, such as with interventional MRI or CT scan, the patient is often asleep under general anesthesia while the surgeon uses images of the brain to guide the lead to its target.
Some advanced centers offer both the stereotactic and iMRI-guided options for DBS surgery. In this case, the doctor and patient will discuss which procedure is better based on a number of factors.
For instance, the doctor may recommend an image-guided procedure for children, patients who have extreme symptoms, those who are especially anxious or fearful or those whose leads are going into certain parts of the brain.
Generally, DBS surgery follows this process:
Read Also: Are Hallucinations A Symptom Of Parkinson’s
Conditions We Treat: Parkinsons Disease
Parkinsons disease is a progressive, degenerative disorder that first attacks the motor system the parts of the brain and nerves that allow movement and then goes on to affect thinking, mood and autonomic functions of the body such as heart rate and digestion. The Neuromodulation and Advanced Treatments Center offers state-of-the-art treatments to address Parkinsons disease symptoms, including deep brain stimulation and levodopa infusion therapies.
Also Check: Parkinsons Disease Treatment Guidelines
How Does Dbs Work
In DBS surgery, electrodes are inserted into a targeted area of the brain, using MRI and, at times, recordings of brain cell activity during the procedure. A second procedure is performed to implant an impulse generator battery , which is similar to a heart pacemaker and approximately the size of a stopwatch.
The IPG is placed under the collarbone or in the abdomen and delivers an electrical stimulation to targeted areas in the brain that control movement. Those who undergo DBS surgery are given a controller to turn the device on or off and review basic parameters such as battery life.
Also Check: How Many Kinds Of Parkinson Disease Are There
Preparing For Dbs Surgery
Working closely with your surgeon and your movement disorder clinicians will help you to determine if DBS is right for you. There are currently three DBS systems available that the neurosurgeon should discuss with you ask for details on each device. Not every DBS surgeon works with all three systems, so it is important that you consider your choice of system and surgeon.
It is beneficial to have a family member or loved one attend DBS-related appointments with you. There are a lot of appointments necessary when considering or receiving DBS, and it is helpful to have an extra person to ensure all the details are covered and necessary questions are asked. If you do get the DBS system surgery, it is extremely important that loved ones or care partners understand the DBS system and how it operates. Older age does not exclude those who are otherwise healthy from being a possible candidate for DBS.
Every person will have unique post-surgery goals. If you are considering DBS, have a clear idea of what may or may not be achieved and manage expectations of how DBS will benefit you.
What Are The Risks Or Complications Of Dbs
Because DBS does involve surgery, there are some possible complications and risks. Your healthcare provider is the best person to tell you about the possible risks and complications. They’re the best source of information because they can consider your medical history, circumstances and more.
The possible complications of surgery include:
You May Like: Is There A Definitive Test For Parkinson’s Disease
What Happens During Surgery
For stage 1, implanting the electrodes in the brain, the entire process lasts 4 to 6 hours. The surgery generally lasts 3 to 4 hours.
Step 1: attach stereotactic frameThe procedure is performed stereotactically, which requires attaching a frame to your head. While you are seated, the frame is temporarily positioned on your head with Velcro straps. The four pin sites are injected with local anesthesia to minimize discomfort. You will feel some pressure as the pins are tightened .
Step 2: MRI or CT scanYou will then have an imaging scan, using either CT or MRI. A box-shaped localizing device is placed over the top of the frame. Markers in the box show up on the scan and help pinpoint the exact three-dimensional coordinates of the target area within the brain. The surgeon uses the MRI / CT scans and special computer software to plan the trajectory of the electrode.
Step 3: skin and skull incisionYou will be taken to the operating room. You will lie on the table and the stereotactic head frame will be secured. This prevents any small movements of your head while inserting the electrodes. You will remain awake during surgery. Light sedation is given to make you more comfortable during the initial skin incision, but then stopped so that you can talk to the doctors and perform tasks.
What To Expect After Dbs
Surgery to implant the leads generally entails an overnight stay, while the IPG is usually implanted as same-day surgery. During recovery, your surgeon will talk to you about caring for your wounds, when you can shower, and any activity restrictions. Its usually recommended that any heavy lifting be avoided for a few weeks.
After another two to four weeks, youll return to have your device programmed. This process will continue for several weeks to ensure the stimulation settings are optimal to control your symptoms. During these visits, you will be shown how to turn the device on and off with the handheld device and check the battery level.
Once the programming has been completed, you will have regular follow-up visits to check and adjust the stimulation to maintain the most benefit for your symptoms.
You May Like: Leaky Gut And Parkinson’s
Life After Dbs Surgery
Once the neurotransmitter has been programmed, you are given a handheld controller to make adjustments.
With the controller, you can turn the simulator on or off, select the signal strength, and move across different program types.
If your DBS neurotransmitter has a rechargeable battery, then it will take about two hours for the device to recharge completely.
Make sure to carry your Implanted Device Identification card if you are traveling by air, as Airport Security will detect the device.
