Types Of Pain In Parkinsons
One review classified the types of PD pain as follows:
- musculoskeletal, in which the pain results from problems with the muscles , bones or joints
- dystonic, which is due to abnormal muscle contractions caused by PD or the medications used to treat it
- radicular pain or nerve pain
- central pain, which is poorly understood and thought to be due to abnormalities in the brain itself
Since A Back Injury In 1985 John Has Experienced Multiple Types Of Pain Some Of Which Have Been Triggered By His Parkinson’s He Was Diagnosed With The Condition In 2016
Ive been experiencing varying degrees of pain since injuring my back, which caused me to have lower-back pain, which continues to this day. Since then, I have also developed pain in other parts of my body due to Parkinsons, including my hands, ribs, upper back and shoulder.
The pain in my ribs is deep, aching and constant, and I get internal tremors in this area. However, the pains in my legs are sharp, intermittent and become very rigid, especially in my calves.
When I walk, the pain can get so bad that I end up having to stop and rest. On really bad days, I use a wheelchair. When Im in a lot of pain, it affects my Parkinsons symptoms even more, and also my spatial awareness, that I tend to lose my balance and fall or freeze.
I was referred to a pain specialist…who enrolled me on an 8-week pain management course led by a Parkinson’s-trained physiotherapist. Now I do an hour of gentle movements and stretching every morning.
I cant stand for long enough to wash and have a shave, or to wash the dishes, so I use a perching stool. I can no longer carry out my hobby of canoeing to the same degree. While I use to be able to do it all day, I’m now lucky if I can do it for an hour.
I was referred to a pain specialist, who prescribed me medication, and advised on workable changes to my lifestyle and diet. They also enrolled me on an 8-week pain management course led by a Parkinson’s-trained physiotherapist. Now I do an hour of gentle movements and stretching every morning.
Introducing Unlock Your Hip Flexors
Unlock Your Hip Flexors gives you a practical, easy-to-follow program you can use today for instantly releasing your hip flexors for more strength, better health and all day energy.
Working with Rick, weve created a great program that is quite simply Done-For-You.
Rick has pulled together a sequential flow designed just for you composed of 10 carefully selected exercises, including PNF Stretching, Static Stretching, Dynamic Stretching, 3-Dimensional Core Stability Exercises, Mobility Exercises, Fascia Stretching and Muscle Activation.
Unlock Your Hip Flexors DVD Video
Weve shot these 10 exercises with explanations from Rick on perfect form and exactly how to target that hard-to-reach psoas muscle. The video content is split in two:
The first is a Coaching Instructional Video where Rick takes you in detail through each exercise, so you fully understand why youre doing that exercise, the best form to take and how it should feel. The second video is a Follow Along format designed so you can perform the flow alongside the video without breaking for explanation.
Unlock Your Hip Flexors Manual
Youll receive a highly targeted manual with greater depth about the psoas muscle and the effects of its shortening on your health and well-being. It also includes detailed descriptions of the exact exercise movements with pictures.
You will experience immediate results the very first time you go through the program.
But first a warningthis isnt for everyone.
Recommended Reading: Does Lack Of Sleep Cause Parkinson’s
Join The Parkinsons Forums: An Online Community For People With Parkinsons Disease And Their Caregivers
Chronic pain between the two groups was assessed using the Brief Pain Inventory , which measures pain severity , pain interference and pain frequency. A qualitative description of pain was also conducted.
Patients described pain as exhausting,tiring,penetrating,miserable and unbearable significantly more often than controls.
Among patients, those with depressive symptoms as evidenced by a score of eight or higher in the Hospital Anxiety and Depression Scale reported pain as tender more frequently than those without depression. Controls with depressive symptoms were more likely to report pain as stabbing, tender and tiring compared to those without evidence of depression.
These descriptions indicate a significant impact of pain on the psychological well-being of the patient, the researchers wrote.
Subsequent analysis showed that patients overall scored higher than controls in worst pain felt since last week and in global pain severity. Among all participants with depressive symptoms, those with Parkinsons had higher scores of worst pain felt and average pain felt since last week, as well as higher reported pain levels at the time of assessment and global pain severity than those in the control group.
Symptoms of depression led to similar differences plus an additional higher impact on social relations between patients and controls. Of note, depression was associated with greater difficulties in walking in the group without Parkinsons.
Shooting Pain And Paraesthesia
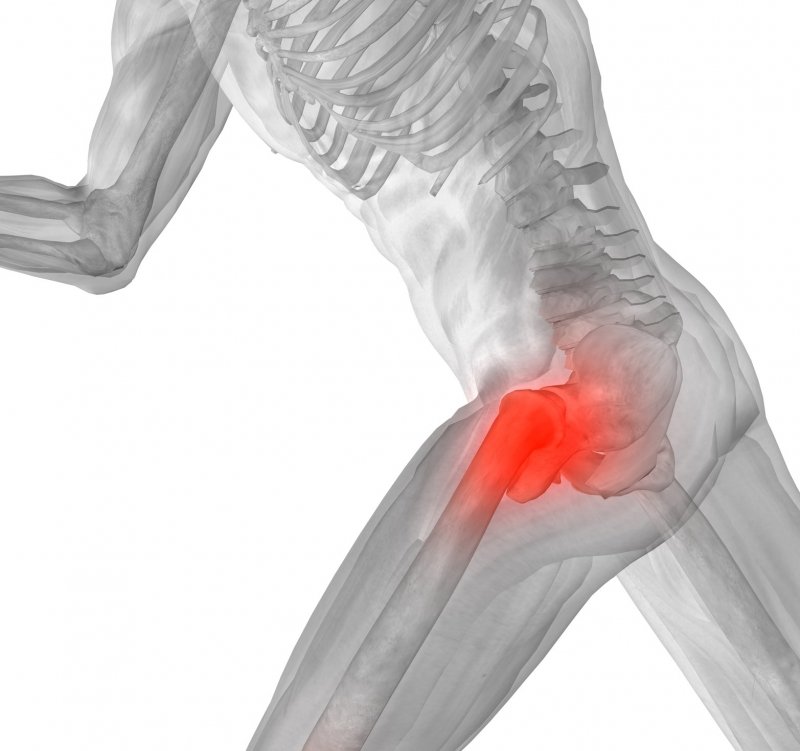
Radicular pain is a sharp pain that shoots down a limb and often affects fingers or toes. Paraesthesia is sometimes described as a feeling of pins and needles or perhaps numbness in a limb which has fallen asleep. Such pain is usually related to trapped nerves in the spinal cord and can feel similar to an electric shock, a tingling or a burning sensation.
Treatment: Painkillers and exercise will generally settle the pain. If not your specialist may refer you for tests such as an MRI scan to check for a trapped nerve in the spinal cord.
Don’t Miss: What Is Shuffling Gait Parkinson’s Disease
Which Type Of Hip Replacement Should I Have
Your surgeon will discuss this with you. It will depend on who you are. In other words, how old you are, whether you have any other medical conditions and what you want to be able to do once you have had your hip replaced. It will also depend on what types of hip replacements your surgeon is used to performing and which ones are used in their hospital. In the UK the National Institute for Health and Care Excellence only recommends devices that are known to last at least 10 years in 95 out of every 100 people who have that type fitted.
All hip replacements can be divided into either cemented or uncemented.
Dont Miss: Best Walking Cane For Parkinsons
James* Was Diagnosed With Parkinson’s In 2011 His Pain Has Worsened As His Condition Has Progressed
When I was diagnosed with Parkinson’s, I initially felt little to no pain. It’s only now, in the advanced stages of the condition, that I’ve started feeling pain, coupled with the normal ageing process.
One of the worst pains I experience is dystonia and dyskinesia of the upper body, especially in my neck and head. It usually starts with a pulsing headache, followed by jerking of the muscles in my face, neck, upper torso and hands. It’s particularly severe in my arthritic finger and my neck. It can be severe to mild, often very distressing, and can last up to 2 hours.
I also have mild to moderate, uncontrollable movements or swaying associated with dyskinesia. It’s more prominent when I’m sitting down at a table or working on my laptop. Strangely, I feel this pain at its worst when I’m on the phone, or trying to explain something, or if I’m feeling over-excited or anxious which is when I become severely dyskinetic. There’s now a dull, continuous pain in my neck, caused through the movement, which gets sharper during bouts of the symptom.
I also experience pain when standing, mostly during a ‘wearing off’ period. My knees pull towards each other and the pain is so severe that I can’t walk. Luckily it only lasts a minute or 2, but the pain can be distressing.
To ease the pain, I take paracetamol as and when, occasionally co-codamol, and very occasionally an anti-inflammatory, for the arthritis. I previously tried cannabis oil but it was of no benefit to me.
Also Check: What Tests Are Done For Parkinson’s
These Symptoms Can Interfere With Daily Activities
Poston notes that the numbness in your hands could be so severe that it can make you unable to sense an object in your hand, which could result in difficulty eating, getting dressed, and holding objects. OBrien also says that people who suffer from these symptoms sometimes cant perform everyday tasks from writing or typing to picking up objects. If you find that youre experiencing numbness or tingling thats getting in the way of your daily activities, you should talk to your doctor immediately.
RELATED: For more health content delivered straight to your inbox, .
Recommended Reading: Does Alcohol Affect Parkinsons Disease
The Varieties Of Lower Back And Hip Pain
|
Many of my clients experience lower back and hip pain simultaneously. But all too frequently they receive inadequate guidance from their physicians about possible causes and about how to relieve it in a lasting way. |
When X-rays and MRIs come back negative, a physician without adequate training in the musculoskeletal system may not know what to prescribe other than physical therapy exercises.
The problem with this strategy is that PT can aggravate certain conditions. Ill go into this in more detail with each of the conditions listed below.
The most frequent regions of pain I hear reports about include
|
You May Like: Does Parkinson’s Affect The Eyes
Can Parkinsons Be Genetic
According to the researches done so far it has been found that there is a possibility of some form of Parkinsons disease due to genetic mutations. However, the hereditary causes of this disease are quite rare. Around 15% of patients having Parkinsons disease are seen to have a family history of the same. It has been seen that a history of Parkinsons disease running in the family may increase the risk of a person to get it. Having a first-degree family member with Parkinsons essentially raises the risk to 3%. The statistics show that having a parent or sibling with Parkinsons disease may slightly increase the risk.
Managing Pain In Parkinson’s
This article summarizes the incidence, types, and causes of reported pain in Parkinson’s Disease . A table of recommendations on how to involve patients with Parkinson’s in their own pain management is provided, along with approaches to pain assessment. Finally, there is a discussion of pain management principles in PD, including optimization of dopaminergic medications, use of analgesics, and innovative treatments for pain management .
Don’t Miss: Do Women Get Parkinson’s
Painful Symptoms Of Parkinsons Disease
Pain can sometimes be an early symptom of PD. For example, a person may complain of a painful shoulder and be diagnosed with an orthopedic condition such as a frozen shoulder, only to develop a rest tremor on that side at a later point. The painful shoulder was in fact not a frozen shoulder after all, but rather pain due to the rigidity of PD. Now of course, sometimes a frozen shoulder is really just a frozen shoulder, so theres no need to jump to conclusions when you are experiencing pain. Not every ache and pain is a sign of PD, but it is important for you to educate yourself, be aware of the possible connections, and be proactive about seeking medical attention for any notable pain you are experiencing.
If you have PD and develop pain, it is important to first bring this to the attention of your doctor. The pain may be related to your PD, or the pain may be due to a common problem such as arthritis which is exacerbated by your PD. However, in some cases, it may be a symptom of a more serious medical problem. So do not assume that the pain is related to your PD before getting an appropriate medical workup.
Signs Of Parkinsons Disease
Parkinsons disease tends to be a very frightening disease to be diagnosed with. Knowing what it is and what the symptoms are will help you to catch it in the early stages and begin treatment right away.
What is Parkinsons Disease?
When brain cells deteriorate, Parkinsons disease is the result. It is considered a chronic condition, as opposed to acute, because it has no cure and doesnt go away by itself. It is also a degenerative disease, meaning that it breaks down the body of the person it attacks. Muscle control is lost due to a lack of dopamine in the brain and, because of this, a difficulty in walking, coordination, and severe shaking develop.
Characteristics and Signs of Parkinsons
Some of the signs of Parkinsons to look out for include:
Tremors or Trembling: for nearly three quarters of patients diagnosed with Parkinsons disease, the appearance of tremors or trembling is the first noticeable symptom.
Muscle stiffness -Parkinsons patients experiencing stiffness or rigidity may not notice any other symptoms of this characteristic. In fact, the person may not even notice the signs of rigidity unless a physician notes it during a physical examination.
The presence of physical rigidity, such as decreased arm swing, is especially useful in helping medical personnel establish a diagnosis of Parkinsons disease.
Lacking coordination
If you have concerns, consult your doctor.
Read Also: Are There Any New Drugs For Parkinson’s
Physical Therapy And Exercise
In addition to medication, physical therapy can help with muscle cramps, and regular exercise and stretching are beneficial to strengthen muscles and maintain flexibility.
Trying to move throughout the day can reduce symptoms. Exercises such as yoga, tai chi, and weight lifting have also been shown to help. The more high intensity the exercise is, the more beneficial it is at alleviating symptoms. Assistive devices such as walkers or canes can also be helpful.
For some people with PD whose symptoms are not adequately controlled with medication and/or exercise, surgery to perform deep brain stimulation may be an option. As with medication and exercise, surgery does not cure or change the course of the disease progression, but it may help with the symptoms of PD.5
Engage with the community by asking a question, telling your story, or participating in a forum.
Dont Miss: Acupressure Points For Parkinsons Tremors
Pain Sites And Assessments
All patients were asked to indicate the distribution of pain sites, duration of pain, and rate average pain intensity over the past 3 months on an 11-point numeric rating scale , with 0 indicating the absence of pain and ten indicating the most intense pain imaginable. The patients reported NRS scores in both the ON and OFF states of motor function on the same day. NRS scores were then transformed into WHO severity stages of mild , moderate , and severe , respectively . MSP responsiveness to Levodopa was defined as a 30% reduction in NRS scores from baseline, 2 h after taking the medication . Data regarding multiple types of pain were also recorded. The ID-pain scale detected central parkinsonian pain.
Don’t Miss: What Mimics Parkinson’s Disease
Can The Sources Of Pain Be Pinpointed
Aware state surgical examination enables the patient to give the surgeon feedback, guiding him or her to the point that is responsible for the pain. This live approach allows the causal level in Parkinsons Syndrome Sufferers to be accurately defined and then viewed using endoscopic instruments through a tiny incision. In this way, neural anomalies and strange nerve combinations can be detected and diagnostic errors regarding the disc level responsible for the pain, avoided. Thus, the surgeon is guided to the precise source of pain at that specified inter-vertebral point and the understanding of the actual mechanisms underlying the causation of Parkinsons Syndrome Sufferers.
My Parkinsons Story: Pain
This 10-minute video alternates between an interview with a man and and doctors. The man shares his experience with pain as a symptom of Parkinsons disease. The doctors explain that pain is common in Parkinsons disease, often due to rigidity or dystonia, which can be exacerbated by off periods. Pain caused by Parkinsons symptoms can be relieved by Parkinsons medications, exercise, DBS and botox injections. Pain is an invisible symptom that should be mentioned to your neurologist.
Read Also: What Does A Parkinson’s Tremor Feel Like
Other Symptoms: Aging Or Pd
Because the biggest risk factor for developing PD is age , skeletal problems associated with aging are often experienced by people with PD. While it is not clear that PD increases the risk or even the severity of these other skeletal conditions, the problems of PD can make the symptoms of these conditions more prominent.
- Osteoarthritis, the joint damage associated with general wear and tear on the joints, is nearly universal in aging. Osteoarthritis tends to affect larger joints such as the hip and knee.
- Arthritis of the spine is also very common. This may contribute to the development of spinal stenosis, narrowing of the canal in the spine that houses the spinal cord. In severe cases, spinal stenosis causes damage to the nerves as they exit the spine or even to the spinal cord itself.
- Disorders of the fibrous discs between the bones of the spine can also cause pain, or limb numbness or weakness.
What Are The Treatment Options For Parkinsons Disease
When a person suffers from Parkinsons disease, the nerve cells fail to produce enough dopamine to send signals to the brain to control conscious and unconscious actions. The condition gets progressively worse over time.
However, there are means through which one could reduce the impact of this condition to a certain extent. Such treatment options include medication, surgery, and physical therapy.
Medication
As the symptoms such as tremors, muscle stiffness, and walking issues start to appear, doctors may prescribe certain commonly regarded medications such as Levodopa, MAO B Inhibitors, Dopamine Agonists and Antivirals.
These medicines are, however, more useful at the initial stages of the disease. After time elapses, these medications start to lose the effectiveness they had at earlier stages.
The prescription and dosage depend on the severity of the condition.
Surgical Procedures
In the case of Parkinsons disease, a surgical procedure known as Deep Brain Stimulation has provided patients with good results.
A wire is placed inside of the patients brain and helps the brain more effectively receive electrical signals. If effective, this improves the functioning power of the brain.
Physical Therapy
Physical therapy can help patients deal with the effects of Parkinsons disease. Specially designed exercises such as breathing, stretching, rhythmic, static and dynamic exercises are implemented to relieve some of the pain experienced by the patient.
Read Also: What Is The Difference Between Ms And Parkinson’s Disease
