Theory Of Pd Progression: Braaks Hypothesis
Researchers believe a combination of genetic and environmental factors cause Parkinsons. In 2003, Heiko Braak, MD, hypothesized that an unknown pathogen in the gut could be the cause of PD.
This was followed by a more extensive hypothesis, stating that PD starts in two places: the neurons of the nasal cavity and the neurons in the gut. This is now known as Braaks hypothesis. In this theory, the pathogen enters the body via the nose and/or gets swallowed and reaches the gut. The pathogenic products thus come into contact with the olfactory and/or enteric neurons, triggering the aggregation of an abnormal protein called -Synuclein. The aggregated -Synuclein then spreads toward the central nervous system , and eventually arriving in and causing the degeneration of the dopaminergic neurons in the area of the brain called the substantia nigra.
This theory is supported by evidence that non-movement symptoms, such as a loss of sense of smell, sleep disorders and constipation, may appear several years ahead of movement symptoms. For this reason, researchers focus on these non-motor symptoms to detect PD as early as possible and to look for ways to stop its progression.
Page reviewed by Dr. Jun Yu, Movement Disorders Fellow at the University of Florida, a Parkinsons Foundation Center of Excellence.
Symptoms That Are Commonly Associated With Pd
These symptoms include sleep disorders, abnormalities in blood pressure, urinary problems, constipation, depression, and anxiety. Even though these symptoms are so commonly seen in PD, they are also commonly associated with other issues that have nothing to do with PD, so it is vital to keep an open mind about their cause. If any symptom is new or worsening, it could be an indication of a new medical problem. For example, urinary problems are extremely common in PD, but may be a sign of an enlarged prostate, which can be treated in an entirely different way.
How Do I Take Care Of Myself
If you have Parkinsons disease, the best thing you can do is follow the guidance of your healthcare provider on how to take care of yourself.
- Take your medication as prescribed. Taking your medications can make a huge difference in the symptoms of Parkinson’s disease. You should take your medications as prescribed and talk to your provider if you notice side effects or start to feel like your medications aren’t as effective.
- See your provider as recommended. Your healthcare provider will set up a schedule for you to see them. These visits are especially important to help with managing your conditions and finding the right medications and dosages.
- Dont ignore or avoid symptoms. Parkinsons disease can cause a wide range of symptoms, many of which are treatable by treating the condition or the symptoms themselves. Treatment can make a major difference in keeping symptoms from having worse effects.
Also Check: How Long Does It Take For Parkinson Medication To Work
What Are The Most Common Symptoms
There are 4 main motor symptoms of PD:1
- Tremor at rest, such as a slight tremor in the hands or feet
- Rigidity of limbs, neck, or shoulders
- Difficulty balancing
- Slowness of movement or gradual loss of spontaneous movement
Parkinsons can sometimes be confused with other movement disorders. Doctors begin to think about PD when they see bradykinesia with either tremor or rigidity. These symptoms are seen from the start of the disease.1
Changes In Cognition And Parkinsons Disease
Some people with Parkinsons may experience changes in their cognitive function, including problems with memory, attention, and the ability to plan and accomplish tasks. Stress, depression, and some medications may also contribute to these changes in cognition.
Over time, as the disease progresses, some people may develop dementia and be diagnosed with Parkinsons dementia, a type of Lewy body dementia. People with Parkinsons dementia may have severe memory and thinking problems that affect daily living.
Talk with your doctor if you or a loved one is diagnosed with Parkinsons disease and is experiencing problems with thinking or memory.
Don’t Miss: Can Depression Cause Parkinson’s Disease
Motor Features At Baseline
According to cross-sectional data analysis, untreated Parkinsons disease patients showed an annual decline in UPDRS-III scores of 3.33 points per year of disease duration, with 67% of the variance being explained by the model . After a mean of 7 years from the onset of motor symptoms, 40% of patients had developed postural instability and falls, while 17% had clinically relevant dysphagia and freezing of gait . Baseline features and milestones are detailed in .
Progression of Parkinson’s disease motor disability according to levodopa status and response . Scatterplot of UPDRS motor score at natural OFF and at 1-year follow-up after overnight withdrawal of levodopa . Data are described according to Pearsons statistic and linear regression analysis . Estimation of 12-month and 24-month LDR and SDR to levodopa in different disease duration strata . LDR is calculated as the difference between the natural OFF state and the overnight OFF state, while the SDR is the shift between the overnight OFF and the ON state. White bars represent the changes in UPDRS-III between the natural OFF and the ON state at the first ever levodopa challenge. Trend lines of natural OFF state, overnight OFF and ON state are also included.
Red Flags For Other Parkinsonian Syndromes
Once drug-induced parkinsonism is ruled out, the next step is to discern whether the patient is more likely to have idiopathic Parkinsons disease versus another flavor of parkinsonism , as this distinction influences prognosis, likelihood of response to medication, and how to counsel patients. There are several red flags that point to another parkinsonian syndrome rather than idiopathic Parkinsons disease:
- Early falls as well as abnormal eye movements suggest progressive supranuclear palsy
- Early severe autonomic dysfunction suggests multiple system atrophy
- Early cognitive issues suggests dementia with Lewy bodies
- Very rapidly progressive, debilitating symptoms in a couple years is usually too fast for idiopathic Parkinsons disease
Don’t Miss: How Does Dopamine Affect Parkinson’s Disease
Coping With Parkinsons Hallucinations
Living with hallucinations is difficult. It can make you question whats real and whats not. It can also cause you to develop mental health conditions such as depression and anxiety. While your healthcare provider is in the best place to provide effective treatment, here are ways you can cope with the pressures of living with Parkinsons hallucinations:
- Talk to your family and friends: Letting the people who are closest to you know whats going on can relieve some of the pressure. When the people around you know whats happening, they are more equipped to support you through hallucination episodes.
- Speak to your healthcare provider often: Keep your healthcare provider updated about changes and developments in your condition. If you have a hallucinatory episode even once, dont dismiss it. Contact your doctor about it immediately. The earlier they are aware, the quicker they can get on top of the situation and provide you with efficient and adequate care.
Hallucinations can also be difficult for a person with Parkinsons carer to manage. Knowing how to manage a hallucinatory episode is crucial as a caretaker of a person with Parkinsons disease.
Invalidating the experience of a person having hallucinations or telling them that what they are experiencing isnt real does very little to help them.
Instead, provide support. If they become stressed, try out calming techniques such as deep breathing exercises to help alleviate their stress.
Support For People Living With Parkinsons Disease
While the progression of Parkinsons is usually slow, eventually a persons daily routines may be affected. Activities such as working, taking care of a home, and participating in social activities with friends may become challenging. Experiencing these changes can be difficult, but support groups can help people cope. These groups can provide information, advice, and connections to resources for those living with Parkinsons disease, their families, and caregivers. The organizations listed below can help people find local support groups and other resources in their communities.
Read Also: How To Improve Balance In Parkinson’s Disease
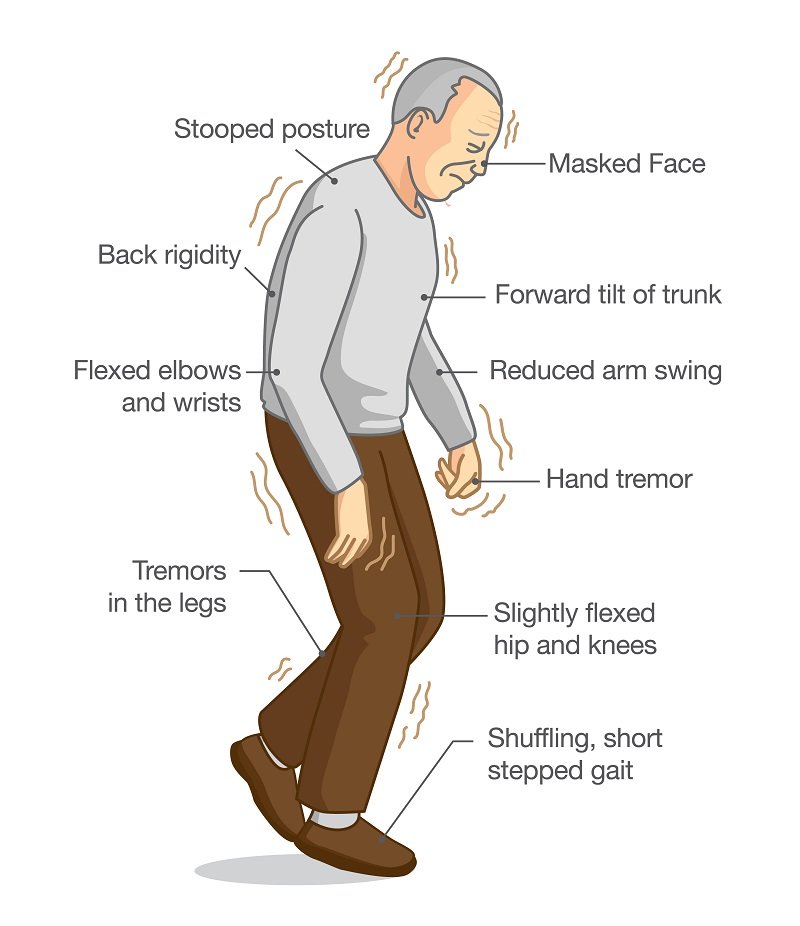
Motor Symptoms Of Parkinsons Disease
The motor symptoms of Parkinsons refer to those signs of the disease that affect the bodys movement. There are four hallmark symptoms that are characteristic of Parkinsons, and are important for diagnosing the neurodegenerative disorder: resting tremor, bradykinesia, rigidity, and postural instability.
People with Parkinsons also may experience other motor symptoms, such as freezing, impaired coordination, and difficulty speaking. There also are non-motor symptoms associated with the disease.
Because Parkinsons is a progressive disease, most symptoms will start slowly, and then get worse as time progresses.
Other Symptoms: Aging Or Pd
Because the biggest risk factor for developing PD is age , skeletal problems associated with aging are often experienced by people with PD. While it is not clear that PD increases the risk or even the severity of these other skeletal conditions, the problems of PD can make the symptoms of these conditions more prominent.
- Osteoarthritis, the joint damage associated with general wear and tear on the joints, is nearly universal in aging. Osteoarthritis tends to affect larger joints such as the hip and knee.
- Arthritis of the spine is also very common. This may contribute to the development of spinal stenosis, narrowing of the canal in the spine that houses the spinal cord. In severe cases, spinal stenosis causes damage to the nerves as they exit the spine or even to the spinal cord itself.
- Disorders of the fibrous discs between the bones of the spine can also cause pain, or limb numbness or weakness.
Don’t Miss: Can Parkinson’s Cause Blindness
Data Synthesis And Confidence In Evidence Statements For Risk Of Icds
-
7. In people with early PD, what is the risk of ICDs with medications used for the treatment of motor symptoms and does the risk differ between drug formulations?
The MCID in the risk of ICDs was determined by consensus to be 2% RDs 1% were considered clinically unimportant.
Confidence in Evidence Statements
What Is Parkinsons Disease
Parkinsons disease is a condition where a part of your brain deteriorates, causing more severe symptoms over time. While this condition is best known for how it affects muscle control, balance and movement, it can also cause a wide range of other effects on your senses, thinking ability, mental health and more.
Recommended Reading: How Do They Test For Parkinson’s
Runny Nose And Parkinsons Disease
Runny nose, or rhinorrhea in medical jargon, is an annoying symptom that has been shown in a number of studies to be more common among people with PD than those without PD. The rhinorrhea of PD is not associated with a viral infection or environmental allergies, or any other common cause of runny nose.
Rhinorrhea can be an early feature of PD, sometimes present at the time of diagnosis. In fact, studies have shown that rhinorrhea is not correlated with disease duration, disease severity, or whether the PD is characterized more by tremor or gait difficulties. One study tested the smell of those with runny nose versus those without and determined that the presence of rhinorrhea did not correlate with deficits in the sense of smell.
There are no studies in the medical literature addressing how to treat the runny nose associated with PD. Ipratropium bromide is an anti-cholinergic medication that does not cross the blood-brain barrier and is available in two forms an inhaled form to treat asthma, chronic bronchitis and emphysema and a nasal spray that is used to treat allergic and non-allergic runny nose. The nasal spray may be worth a try in PD-related rhinorrhea.
How Is Parkinsons Disease Diagnosed
Diagnosis is difficult at every stage of the disease, but particularly in the early stages. No single test can provide a diagnosis. A diagnosis will likely involve physical and neurological examinations, conducted over time to assess changes in reflexes, coordination, muscle strength, and mental function. Your doctor might also see how you respond to medicine.
You may need to have brain imaging tests to rule out other conditions that might be causing your symptoms. Such tests could include MRI and CT scans and possibly some other types of scans. Blood tests may also be done to exclude other illnesses.
You May Like: Does Parkinson Cause Muscle Spasms
How Are Cognitive Issues Diagnosed
Common ways to assess and diagnose cognitive disorders:
- Interview the person with PD.
- Ask family members or care partners about their observations.
- Administer cognitive screening tests such as the Mini-Mental State Examination or Montreal Cognitive Assessment . The neurologist will ask questions that evaluate the persons understanding of where and who they are, the date and year, attention, memory, language and problem-solving skills.
- A neurologist may suggest seeing a clinical neuropsychologist for a more detailed assessment.
- Neuropsychological assessment can be an important diagnostic tool for differentiating PD from other illnesses such as Alzheimer’s disease, stroke or dementia.
Breathing Problems And Parkinsons Disease
Usually, trouble breathing is not thought of as a symptom of PD. Those with PD who complain of this will typically have testing of their heart and lung function. This is necessary since, as we continue to emphasize, a person with PD can develop medical problems unrelated to PD and needs every new symptom evaluated like someone without PD. However, often the testing does not reveal a cardiac or pulmonary abnormality. Could difficulty breathing be a symptom of PD itself?
There are a number of ways in which difficulty breathing may be a symptom of PD:
Shortness of breath can be a wearing-OFF phenomenon
Some non-motor symptoms can fluctuate with brain dopamine levels, which means that they change as a function of time from the last levodopa dose. For some people, shortness of breath can be one of the non-motor symptoms that appears when medication levels are low. However, shortness of breath can be due to anxiety which can also be a wearing-OFF phenomenon. Sometimes it is not possible to determine whether the key symptom is anxiety or shortness of breath. Treatment involves changing medication dosing and timing so that OFF time is minimized. You can view this webinar which discusses the concept of wearing OFF and potential treatments.
Abnormal breathing can be a type of dyskinesia
Restrictive lung disease
Aspiration pneumonia
Sleep apnea
Read Also: Support Groups For Parkinson’s
How Soon After Treatment Will I Feel Better And How Long Will It Take To Recover
The time it takes to recover and see the effects of Parkinson’s disease treatments depends strongly on the type of treatments, the severity of the condition and other factors. Your healthcare provider is the best person to offer more information about what you can expect from treatment. The information they give you can consider any unique factors that might affect what you experience.
Parkinsons Disease For Primary Care With Dr Albert Hung
December 5, 2022 By Matthew Watto, MD
Master the ins-and-outs of Parkinsons Disease! Were joined by Dr. Albert Hung, who teaches us pearls for the initial history and physical exam in a patient with undiagnosed Parkinsons, a framework for management of early and advanced motor symptoms, tips for treating autonomic symptoms and cognitive / psychiatric features, and more.
Claim free CME for this episode at curbsiders.vcuhealth.org!
- Producer, Writer, Show Notes, and Infographic: Malini Gandhi
- Cover Art: Kate Grant
Visit betterhelp.com/curb to save 10% off your first month.
Also Check: Cognitive Exercises For Parkinson’s
Treatment Of Advanced Motor Symptoms
In more advanced Parkinsons disease, patients will often experience a shorter window of time in which levodopa / carbidopa is effective, and tend to develop on / off fluctuations in which they experience wearing off of the medication towards the end of the dose . This is because levodopa has a short half life in the blood while in earlier stages of Parkinsons disease the body can accommodate this, in later stages the accommodation is less robust, and wearing off will occur. Additionally, when patients do take enough medication to achieve an on state, they may exhibit too much movement, known as levodopa-induced dyskinesias , which can include writhing, swaying, and bobbing. Thus, the challenge in managing motor symptoms in advanced Parkinsons disease is trying to strike a balance between wearing off and levodopa-induced dyskinesias When patients reach this point, a movement disorder specialist should be involved in management.
In thinking about management of advanced motor symptoms, Dr. Hung notes that thinking about pharmacokinetics is key: essentially, considering how to stretch out the duration of action of levodopa to prevent so many highs and lows. There are several strategies in treating motor symptoms in advanced Parkinsons disease:
Read Also: Vacations For Parkinsons Patients
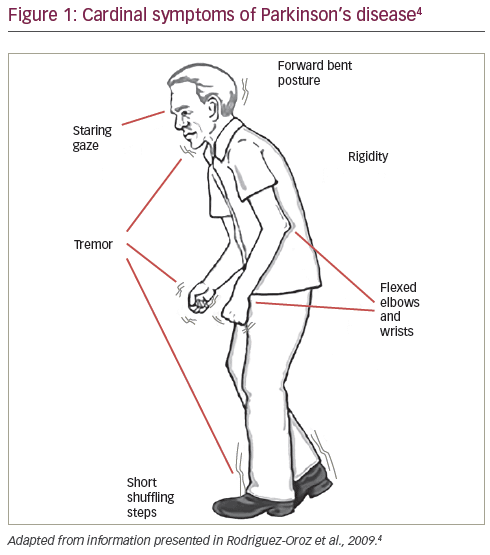
What Are The Symptoms Of Parkinsons Disease How Is Parkinsons Disease Diagnosed

People with Parkinsons disease suffer from motor symptoms as well as non-motor symptoms.
Motor symptoms include intermittent tremors, slow and rigid movements. Non-motor symptoms include loss of smell, pain and even dementia.
In the initial stages of Parkinsons disease a person may experience symptoms such as:
- Slight rigidity in the arms and legs
- unable to change facial expressions according to emotions spontaneously
- Slight back pain due to which the posture of the person may be slightly stooped
- Sudden stiffness in the body at times
- Tremor on one arm on one side of the body
- The symptoms may be experienced only on one side of the body
- Handwriting may get messier and smaller
In the intermediate stage of Parkinsons disease a person may experience symptoms such as:
- Slower movements and therefore takes longer to do the daily work such as combing, dressing etc
- Loss of balance
- May require aids while walking such as a walker
In the advanced stage of Parkinsons disease the symptoms include:
Don’t Miss: Home Help For Parkinson’s Patients
