How Can We Support The Sleep/wake Cycle Of Pdd
For people with PDD who are confused about the day-night cycle, some daily strategies can be helpful. At night, starting a lights out routine that happens at the same hour every day, where all curtains are closed and lights are turned off, can help the person understand that it is sleep time. During the day, opening the curtains, allowing the person with PDD to spend as much time in the daylight as possible, avoiding naps, and organizing stimulating activities, can be helpful. Having lots of calendars and clocks in every room might also help a person with PDD be less confused about the time of day.
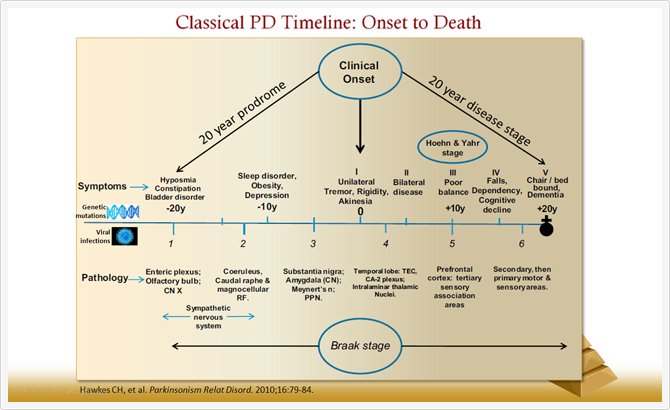
Parkinsons Disease Is A Progressive Disorder
Parkinsons Disease is a slowly progressive neurodegenerative disorder that primarily affects movement and, in some cases, cognition. Individuals with PD may have a slightly shorter life span compared to healthy individuals of the same age group. According to the Michael J. Fox Foundation for Parkinsons Research, patients usually begin developing Parkinsons symptoms around age 60. Many people with PD live between 10 and 20 years after being diagnosed. However, a patients age and general health status factor into the accuracy of this estimate.
While there is no cure for Parkinsons disease, many patients are only mildly affected and need no treatment for several years after their initial diagnosis. However, PD is both chronic, meaning it persists over a long period of time, and progressive, meaning its symptoms grow worse over time. This progression occurs more quickly in some people than in others.
Pharmaceutical and surgical interventions can help manage some of the symptoms, like bradykinesia , rigidity or tremor , but not much can be done to slow the overall progression of the disease. Over time, shaking, which affects most PD patients, may begin to interfere with daily activities and ones quality of life.
What Is The Prognosis And Life Expectancy For Parkinson’s Disease
The severity of Parkinson’s disease symptoms and signs vary greatly from person to peson, and it is not possible to predict how quickly the disease will progress. Parkinson’s disease itself is not a fatal disease, and the average life expectancy is similar to that of people without the disease. Secondary complications, such as pneumonia, falling-related injuries, and choking can lead to death. Many treatment options can reduce some of the symptoms and prolong the quality of life.
Read Also: Cardinal Features Of Parkinson’s
Incidence Of Parkinsons Disease
Its estimated that approximately four people per 1,000 in Australia have Parkinsons disease, with the incidence increasing to one in 100 over the age of 60. In Australia, there are approximately 80,000 people living with Parkinsons disease, with one in five of these people being diagnosed before the age of 50. In Victoria, more than 2,225 people are newly diagnosed with Parkinsons every year.
Stage Three Of Parkinsons Disease
Stage three is considered mid-stage and is characterized by loss of balance and slowness of movement.
Balance is compromised by the inability to make the rapid, automatic and involuntary adjustments necessary to prevent falling, and falls are common at this stage. All other symptoms of PD are also present at this stage, and generally diagnosis is not in doubt at stage three.
Often a physician will diagnose impairments in reflexes at this stage by standing behind the patient and gently pulling the shoulders to determine if the patient has trouble maintaining balance and falls backward . An important clarifying factor of stage three is that the patient is still fully independent in their daily living activities, such as dressing, hygiene, and eating.
Also Check: Parkinson’s Disease Mitochondrial Dysfunction
What You Can Do
As of 2021, there is no definite cure for Parkinsons disease. There is also no definite known cause. Its likely due to a combination of an individuals susceptibility and environmental factors. Most cases of Parkinsons disease happen without a genetic link.
According to research published in 2012, only report having a family member with the disease. Many toxins are suspected and have been studied, but no single substance can be reliably linked to Parkinsons.
However, research is ongoing. Its estimated that
What Happens In Pdd
People with PDD may have trouble focusing, remembering things or making sound judgments. They may develop depression, anxiety or irritability. They may also hallucinate and see people, objects or animals that are not there. Sleep disturbances are common in PDD and can include difficulties with sleep/wake cycle or REM behavior disorder, which involves acting out dreams.
PDD is a disease that changes with time. A person with PDD can live many years with the disease. Research suggests that a person with PDD may live an average of 57 years with the disease, although this can vary from person to person.
Don’t Miss: Parkinson’s Disease Awareness Ribbon
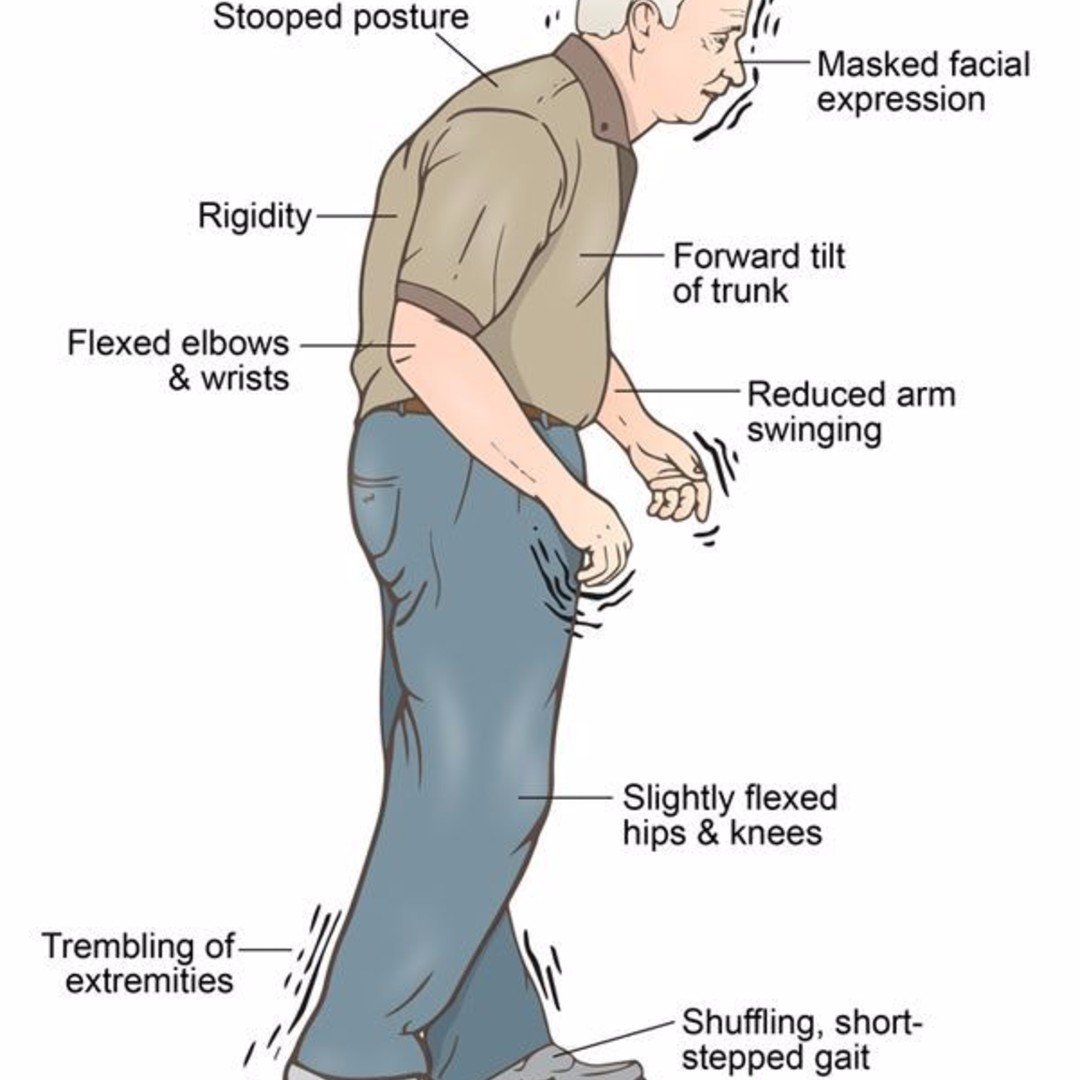
Common Motor Symptoms That Require Management
- Tremor is a prominent and early symptom of PD .
- Slowness, or bradykinesia, a core feature of PD.
- Rigidity is the third prominent feature on examination.
- A combination of bradykinesia and rigidity leads to some other characteristic features of PD, such as micrographia.
- The fourth prominent feature of PD is gait disturbance, although this is typically a late manifestation. Flexed posture, ataxia, reduced arm swing, festination, march-a-petits-pas, camptocormia, retropulsion, and turning en bloc are popular terms to describe the gait in PD. Gait disorder is not an early feature of PD but is frequently described as it is easy to recognize and cinches the diagnosis in later stages.
The rate of progression of the disease may be predicted based on the following:
- Males who have postural instability of difficulty with gait.
- Patients with older age at onset, dementia, and failure to respond to traditional dopaminergic medications tend to have early admission to nursing homes and diminished survival.
- Individuals with just tremors at the initial presentation tend to have a protracted benign course.
- Individuals diagnosed with the disease at older age combined with hypokinesia/rigidity tend to have a much more rapid progression of the disease.
The disorder: leads to disability of most patients within ten years has a mortality rate three times the normal population.
Parkinsons cannot yet be cured . A lot of financial and other resources are being expended on research to find a cure.
What Are The Signs And Symptoms Of Progressive Supranuclear Palsy
If you have PSP, youll likely experience the following symptoms that worsen with time. Youll likely:
- Lose your balance frequently. You may fall, especially backwards.
- Lose the ability to aim your eyes. You might not be able to look up or down, follow something thats moving, or keep your eyes fixed on something still. Your eyelids might retract , giving your face a surprised look.
- Have trouble swallowing.
- Feel stiff muscles and move slowly.
- Have trouble speaking. Your speech might be quieter and slurred, impairing your ability to pronounce words.
- Feel mood changes and observe behavioral changes.
- Experience depression and apathy .
- Get dementia. Your thoughts will be slow, youll have difficulty resisting impulses and you may find problem-solving difficult.
- Have insomnia .
- Feel irritable and agitated.
Read Also: What Are Early Warning Signs Of Parkinson’s Disease
What Is The Difference Between Progressive Supranuclear Palsy And Parkinsons Disease
PSP frequently resembles Parkinsons disease, often making it difficult to distinguish these conditions from one another. Both cause difficulty with stiffness and clumsiness. Both cause slow movement and start later in life. And both show damage to the same areas of the brain that affect movement. In particular, PSP-P can be nearly indistinguishable from Parkinsons disease by clinical examination.
But, PSP and Parkinsons disease are different in several ways. On average, PSP gets worse quicker than Parkinsons and doesnt respond as well to medications. People with Parkinsons usually bend forward, while people with PSP stand very straight, or even slightly backwards. Problems with swallowing and with speaking appear early with PSP and they are far more severe. A tremor is rare with people who have PSP and common in people who have Parkinsons. Motor symptoms, such as slowing and loss of dexterity, typically start very asymmetrically in Parkinsons disease .
Additionally, their underlying pathological processes differ at the molecular level. Abnormalities relating to the protein tau and its effect on brain cells is central to PSP pathology. And, when looked at through a microscope, the damaged brain cells in someone with PSP look different than those of people who have Parkinsons.
How Is Progressive Supranuclear Palsy Diagnosed
PSP is diagnosed on the basis of clinical signs and exam findings, but it often isnt easy to diagnose. Theres no single test that points right at it with certainty. It is often mistaken for Parkinsons disease and it can sometimes take years to distinguish PSP from PD.
If your healthcare provider suspects PSP based on the symptoms you report, he or she will likely send you to get a MRI . This will help to rule out other diseases such as Parkinsons and occasionally it can show shrinking of your midbrain that raises the possibility of PSP in the appropriate clinical setting. Youll also be sent to a neurologist specializing in Parkinsons disease and movement disorders.
Although there are many symptoms of PSP, the one that confirms the diagnosis is trouble moving your eyes up and down. Other common symptoms like falling and difficulty swallowing also point at PSP.
Also Check: Late Stage Parkinson
Is Progressive Supranuclear Palsy Inherited
No, PSP rarely runs in families. If you have PSP, there is very little risk of your other family members having it, and that includes your siblings and your children. Family history of PSP has an almost zero effect on an individuals lifetime PSP risk, meaning people have about the same risk of developing PSP in their lifetime regardless if they do or do not have someone in their family who had or has PSP.
In The Loop: Staying Ahead Of Parkinsons Disease One Ping Pong Game At A Time
Since being diagnosed with Parkinson’s disease, Steve Grinnell has worked hard to stay active, stepping up his table tennis game and, thanks to co-workers, testing his skills outside his home.
Four years ago, Steve Grinnell’s life was forever changed when doctors at Mayo Clinic in Rochester diagnosed him with early-onset Parkinson’s disease. Since that time, the progressive nervous system disorder has begun to take a toll on Steve and his family, just as it does on the millions of other Americans living with the disease. “It has greatly diminished his quality of life, leaving him with tremors, physical exhaustion, impaired balance, troubled grasping things with his right hand, slow right-arm movement and problems sleeping,” the Rochester Post-Bulletin recently reported. “That’s to name just a few of his symptoms.”
Reading that, one might assume the disorder is winning. And to Steve, sometimes it feels like it is. But much of the time, he tells us he also feels like he’s staying one step ahead of the disease by staying as physically active as possible. “Parkinson’s presents such a conundrum because it wears you down physically, and yet exercise is so valuable,” Steve says. “My legs, feet and right arm are always cramping, so it takes mental effort to get moving.”
You May Like: Can Parkinson’s Run In The Family
Signs Of Parkinsons Disease
In 1817, Dr. James Parkinson published An Essay on the Shaking Palsy describing non-motor, as well as, motor symptoms of the illness that bears his name. Parkinsons is not just a movement disorder, explained Dr. Shprecher. Constipation, impaired sense of smell, and dream enactment can occur years before motor symptoms of Parkinsons. The latter, caused by a condition called REM sleep behavior disorder, is a very strong risk factor for both Parkinsons and dementia . This has prompted us to join a consortium of centers studying REM sleep behavior disorder.
What Is The Prognosis
The disease gets progressively worse, with people becoming severely disabled within three to five years of onset. Affected individuals are predisposed to serious complications such as pneumonia, choking, head injury, and fractures. The most common cause of death is pneumonia. With good attention to medical and nutritional needs, it is possible for individuals with PSP to live a decade or more after the first symptoms of the disease appear.
Also Check: Late-onset Parkinson’s
Medications For People With Parkinsons Disease
Symptoms of Parkinsons disease result from the progressive degeneration of nerve cells in the brain and other organs such as the gut, which produce a neurotransmitter called dopamine. This causes a deficiency in the availability of dopamine, which is necessary for smooth and controlled movements. Medication therapy focuses on maximising the availability of dopamine in the brain. Medication regimes are individually tailored to your specific need. Parkinsons medications fit into one of the following broad categories:
- levodopa dopamine replacement therapy
- dopamine agonists mimic the action of dopamine
- COMT inhibitors used along with levodopa. This medication blocks an enzyme known as COMT to prevent levodopa breaking down in the intestine, allowing more of it to reach the brain
- anticholinergics block the effect of another brain chemical to rebalance its levels with dopamine
- amantadine has anticholinergic properties and improves dopamine transmission
- MAO type B inhibitors prevent the metabolism of dopamine within the brain.
Stage Five Of Parkinsons Disease
Stage five is the most advanced and is characterized by an inability to rise from a chair or get out of bed without help, they may have a tendency to fall when standing or turning, and they may freeze or stumble when walking.
Around-the-clock assistance is required at this stage to reduce the risk of falling and help the patient with all daily activities. At stage five, the patient may also experience hallucinations or delusions.
While the symptoms worsen over time, it is worth noting that some patients with PD never reach stage five. Also, the length of time to progress through the different stages varies from individual to individual. Not all the symptoms may occur in one individual either. For example, one person may have a tremor but balance remains intact. In addition, there are treatments available that can help at every stage of the disease. However, the earlier the diagnosis, and the earlier the stage at which the disease is diagnosed, the more effective the treatment is at alleviating symptoms.
Read Also: Can Parkinson’s Change Your Personality
Support For People With Parkinsons Disease
Early access to a multidisciplinary support team is important. These teams may include doctors, physiotherapists, occupational therapists, speech therapists, dietitians, social workers and specialist nurses. Members of the team assess the person with Parkinsons disease and identify potential difficulties and possible solutions.There are a limited number of multidisciplinary teams in Victoria that specialise in Parkinsons disease management. But generalist teams are becoming more aware of how to help people with Parkinsons disease.
What Makes Pd Hard To Predict
Parkinsonâs comes with two main buckets of possible symptoms. One affects your ability to move and leads to motor issues like tremors and rigid muscles. The other bucket has non-motor symptoms, like pain, loss of smell, and dementia.
You may not get all the symptoms. And you canât predict how bad theyâll be, or how fast theyâll get worse. One person may have slight tremors but severe dementia. Another might have major tremors but no issues with thinking or memory. And someone else may have severe symptoms all around.
On top of that, the drugs that treat Parkinsonâs work better for some people than others. All that adds up to a disease thatâs very hard to predict.
You May Like: What Color Is The Ribbon For Parkinson’s
How Is Age Related To Pdd
Both PD and PDD are more common with increasing age. Most people with PD start having movement symptoms between ages 50 and 85, although some people have shown signs earlier. Up to 80% of people with PD eventually develop dementia. The average time from onset of movement problems to the development of dementia is about 10 years.
Experience And Expertise In Diagnosis And Care
Parkinsonism is a shorthand description for body movements that have become slow, small, stiff, shaky, and unsteady. Most cases of Parkinsonism develop after age 50 and are caused by neurodegenerative diseases such as Parkinsons disease . Some Parkinsonisms are the result of strokes, medication side effects, or another neurological condition such as normal pressure hydrocephalus.
UT Southwesterns Movement Disorders team has extensive experience in evaluating and treating Parkinsonism, PD, and other related disorders. Our clinical programs provide patients with access to the latest treatment options and information about medications to manage symptoms, as well as other services as needed.
Recommended Reading: Parkinson’s Plus Life Expectancy
What Are The Symptoms
PSP affects movement, control of walking and balance, speech, swallowing, eye movements and vision, mood and behavior, and thinking. The pattern of signs and symptoms can be quite different from person to person. The most frequent first symptom of PSP is a loss of balance while walking. Individuals may have abrupt and unexplained falls without loss of consciousness, a stiff and awkward gait, or slow movement.
As the disease progresses, most people will begin to develop a blurring of vision and problems controlling eye movement. These symptoms may include:
- Slow eye movements.
Sidebar: Advances In Circuitry Research
The brain contains numerous connections among neurons known as neural circuits.
Research on such connections and networks within the brain have advanced rapidly in the past few years. A wide spectrum of tools and techniques can now map connections between neural circuits. Using animal models, scientists have shown how circuits in the brain can be turned on and off. For example, researchers can see correlations between the firing patterns of neurons in a zebrafishs brain and precise behavioral responses such as seeking and capturing food.
Potential opportunities to influence the brains circuitry are starting to emerge. Optogenetics is an experimental technique that involves the delivery of light-sensitive proteins to specific populations of brain cells. Once in place, these light-sensitive proteins can be inhibited or stimulated by exposure to light delivered via fiber optics. Optogenetics has never been used in people, however the success of the approach in animal models demonstrates a proof of principal: A neural network can be precisely targeted.
Thanks in part to the BRAIN Initiative, research on neural circuitry is gaining momentum. The Brain Research through Advancing Innovative Neurotechnologies Initiative is accelerating the development and application of new technologies that enable researchers to produce dynamic pictures of the brain that show how individual brain cells and complex neural circuits interact at the speed of thought.
NIH Publication No. 15-5595
You May Like: Hemp Oil And Parkinson’s
