Stage Three Of Parkinsons Disease
Stage three is considered mid-stage and is characterized by loss of balance and slowness of movement.
Balance is compromised by the inability to make the rapid, automatic and involuntary adjustments necessary to prevent falling, and falls are common at this stage. All other symptoms of PD are also present at this stage, and generally diagnosis is not in doubt at stage three.
Often a physician will diagnose impairments in reflexes at this stage by standing behind the patient and gently pulling the shoulders to determine if the patient has trouble maintaining balance and falls backward . An important clarifying factor of stage three is that the patient is still fully independent in their daily living activities, such as dressing, hygiene, and eating.
The 5 Stages Of Parkinsons Disease
Getting older is underrated by most. Its a joyful experience to sit back, relax and watch the people in your life grow up, have kids of their own and flourish. Age can be a beautiful thing, even as our bodies begin to slow down. We spoke with David Shprecher, DO, movement disorders director at Banner Sun Health Research Institute about a well-known illness which afflicts as many as 2% of people older than 65, Parkinsons Disease.
What Is Advanced Parkinsons Disease
The traditional classification and disease progression of Parkinsons disease orient on disease milestones that can be most obviously followed along motor domains. In this sense, the topography and severity of segmental motor symptoms, followed by more bilateral segmental involvement, finally appearance of gait disturbance, postural impairment and bedridden immobile states provide well defined but also in some way broadly scaled categories of disease stages. Although this and similar classifications are valuable to approximate and describe the motor severity over time, the classifications fall short to comprehensively describe and characterize the full, continuous and multidimensional spectrum of disease-related motor and non-motor symptoms. In recent years, diverse non-motor domains, quality of life, psychosocial burden and stigma have received major attention as determinants of PD disease course and outcome parameters of clinical trials . Diversity in neurodegeneration patterns and involvement of several neurotransmitters and their contribution to motor and non-motor symptom parallel the phenotypic variability .
Characterizing PD patients on such broad scales is essential, since the phenotype of individual patients varies substantially. This diversity leads to ultimate differences in patients therapeutic requirements, and will very differentially affect patients subjective well-being, self-perceived disease-related impairments, and health-related quality of life.
Recommended Reading: What Is The Life Expectancy Of Someone With Parkinson’s Disease
First Signs Of Impaired Righting Reflexes This Is Evident As The Patient Turns Or Is Demonstrated When He Or She Is Pushed From Standing Equilibrium With The Feet Together And Eyes Closed
Loss of balance, with the inability to make the rapid, automatic and involuntary movements necessary to protect against falling, is one of the most troubling and dangerous aspects of Parkinsonism and one of the least easily treated. Even when manifested by only slight unsteadiness, it is the criterion separating Stage II and Stage III. All other aspects of Parkinsonism are evident and usually diagnosis is not in doubt.
However, the most important factor identifying Stage III is that the patient is still fully independent in all activities of daily living Although somewhat restricted, has work potential depending upon the type of employment. A normal life can be.
Parkinsons Disease Symptoms Of Dementia

Up to one-third of people living with Parkinson’s disease experience dementia, according to the Parkinson’s Disease Foundation. Problems with dementia may include trouble with memory, attention span, and what is called executive function the process of making decisions, organizing, managing time, and setting priorities.
RELATED: 12 Famous People With Parkinson’s Disease
Also Check: How To Donate To Parkinson’s Research
What Is Parkinson’s Disease
Parkinson’s disease is the second most common neurodegenerative disorder and the most common movement disorder. Characteristics of Parkinsons disease are progressive loss of muscle control, which leads to trembling of the limbs and head while at rest, stiffness, slowness, and impaired balance. As symptoms worsen, it may become difficult to walk, talk, and complete simple tasks.
The progression of Parkinson’s disease and the degree of impairment vary from person to person. Many people with Parkinson’s disease live long productive lives, whereas others become disabled much more quickly. Complications of Parkinsons such as falling-related injuries or pneumonia. However, studies of patent populations with and without Parkinsons Disease suggest the life expectancy for people with the disease is about the same as the general population.
Most people who develop Parkinson’s disease are 60 years of age or older. Since overall life expectancy is rising, the number of individuals with Parkinson’s disease will increase in the future. Adult-onset Parkinson’s disease is most common, but early-onset Parkinson’s disease , and juvenile-onset Parkinson’s disease can occur.
Is Parkinsons Disease Inherited
Scientists have discovered gene mutations that are associated with Parkinsons disease.
There is some belief that some cases of early-onset Parkinsons disease disease starting before age 50 may be inherited. Scientists identified a gene mutation in people with Parkinsons disease whose brains contain Lewy bodies, which are clumps of the protein alpha-synuclein. Scientists are trying to understand the function of this protein and its relationship to genetic mutations that are sometimes seen in Parkinsons disease and in people with a type of dementia called Lewy body dementia.
Several other gene mutations have been found to play a role in Parkinsons disease. Mutations in these genes cause abnormal cell functioning, which affects the nerve cells ability to release dopamine and causes nerve cell death. Researchers are still trying to discover what causes these genes to mutate in order to understand how gene mutations influence the development of Parkinsons disease.
Scientists think that about 10% to 15% of persons with Parkinsons disease may have a genetic mutation that predisposes them to development of the disease. There are also environmental factors involved that are not fully understood.
You May Like: What Is The Life Expectancy Of Someone With Parkinson’s Disease
Practical Aspects For The Implementation Of Advanced Treatments
In the past few years, the treatment of PD has become increasingly complex and it is expected to be more individualized in the future, which implies novel strategies for best practices to define and convey best treatment options to patients with advPD. Current guidelines are a helpful tool in the diagnostics and therapeutic decision making in the early stages of disease however, there is not enough reliable information on how to implicate the suggested strategies in the everyday neurological practice. In addition, there is little specific information on possibilities of influencing the course of disease progress. In addition to the usage of the oral medication in the early stages of the disease, there has been an increase in application of the interventional therapies such as deep brain stimulation and pump therapies. These highly specific treatment options are mostly implemented in specialized clinics or practices for movement disorders. Here, the optimal timing for initiating advanced therapies to improve the quality of life and prevent complications is critical and requires an early information of patients and caregivers about the later stages of the disease with its complications.
Two Types Of Parkinsons Disease
By Amanda Butas 9 am on July 8, 2019
Parkinsons symptoms develop when approximately 80 percent of the neurons that produce dopamine become damaged or die. Statistics indicate approximately one million adults in the United States live with the debilitating disorder. While many people have heard about Parkinsons, few may realize there are two types of the disease.
You May Like: Can Parkinson’s Run In The Family
What Is Your Advice For People With Parkinsons Who Are Preparing For End Of Life
It is very important for people with Parkinsons disease and their families to be informed. They must recognise the personal needs that need to be managed, and consider incorporating palliative care.
For the best care, trustworthy multidisciplinary support can be very helpful particularly from healthcare professionals who specialise in solving broad-based problems. This might include a movement disorder physician, nurse, physiotherapist, occupational therapist, speech therapist or, importantly, a psychologist or chaplain to help manage psychosocial and spiritual problems, taking into consideration cultural and social specificities.
Palliative Care And Parkinsons Disease
The aim of palliative care is to improve quality of life for a person with Parkinsons disease, along with their family members and carers. As a holistic approach to treatment, palliative care aims to address emotional, psychological and spiritual needs while supporting a patients control and choice over certain aspects of care. Anyone at any stage of an illness can receive palliative care, but it is particularly important towards the end of life.
To find out more about Parkinsons later in life, please visit the EPDA website.
Read more:
Read Also: What Is The Life Expectancy Of Someone With Parkinson’s Disease
Symptoms Of Parkinsons Disease
Parkinson’s disease has four main symptoms:
- Tremor in hands, arms, legs, jaw, or head
- Stiffness of the limbs and trunk
- Slowness of movement
- Impaired balance and coordination, sometimes leading to falls
Other symptoms may include depression and other emotional changes difficulty swallowing, chewing, and speaking urinary problems or constipation skin problems and sleep disruptions.
Symptoms of Parkinsons and the rate of progression differ among individuals. Sometimes people dismiss early symptoms of Parkinson’s as the effects of normal aging. In most cases, there are no medical tests to definitively detect the disease, so it can be difficult to diagnose accurately.
Early symptoms of Parkinson’s disease are subtle and occur gradually. For example, affected people may feel mild tremors or have difficulty getting out of a chair. They may notice that they speak too softly, or that their handwriting is slow and looks cramped or small. Friends or family members may be the first to notice changes in someone with early Parkinson’s. They may see that the person’s face lacks expression and animation, or that the person does not move an arm or leg normally.
People with Parkinson’s often develop a parkinsonian gait that includes a tendency to lean forward, small quick steps as if hurrying forward, and reduced swinging of the arms. They also may have trouble initiating or continuing movement.
When To Seek Hospice Care
When you or your loved one have a life expectancy of six months or less, you become eligible for hospice care a type of comfort care provided at the end of life for someone living with end-stage Parkinsons disease. Hospice provides extra support so your loved one can live as comfortably as possible.
If you have experienced a significant decline in your ability to move, speak, or participate in activities of daily living without caregiver assistance, its time to speak with a hospice professional.
Read more: What is hospice care?
Some of the things that determine whether your loved one with end-stage Parkinsons is eligible for hospice include: difficulty breathing, bed bound, unintelligible speech, inability to eat or drink sufficiently, and/or complications including pneumonia or sepsis.
If you live in South Jersey, our nurse care coordinator can answer your questions and decide if your loved one is ready for hospice care. Call us 24/7 at 229-8183.
Don’t Miss: Can Parkinson’s Run In The Family
Two Areas In Which Parkinsons Disease May Bring About Death
I. Falls
PD patients are at an increased risk of falling and bad falls can lead to death. This usually occurs as a complication of a fall that requires hospitalization, particularly if it involves surgery. While most people do not fracture their hips when they fall, some do, and hip surgery, while routine, is still major surgery. It carries the risk of infection, delirium related to pain medications and anesthesia, heart failure, pneumonia, blood clots in the legs that then go to the lungs, and general weakness from immobility. Hip fractures are probably the main cause for death for those who fall, but people can fracture other bones and require surgery. They may fracture their ribs, which leads to reduced coughing, because of the pain, and an increased risk of lung infections . It is surprisingly uncommon for Parkinsons Disease patients to die from brain injuries related to falls, but it still may occur.
II. Pneumonia
PD patients also may develop pneumonias completely unrelated to difficulties with swallowing, just like their non-PD friends and relatives.
Stage Two Of Parkinsons Disease
Stage two is still considered early disease in PD, and it is characterized by symptoms on both sides of the body or at the midline without impairment to balance. Stage two may develop months or years after stage one.
Symptoms of PD in stage two may include the loss of facial expression on both sides of the face, decreased blinking, speech abnormalities, soft voice, monotone voice, fading volume after starting to speak loudly, slurring speech, stiffness or rigidity of the muscles in the trunk that may result in neck or back pain, stooped posture, and general slowness in all activities of daily living. However, at this stage the individual is still able to perform tasks of daily living.
Diagnosis may be easy at this stage if the patient has a tremor however, if stage one was missed and the only symptoms of stage two are slowness or lack of spontaneous movement, PD could be misinterpreted as only advancing age.
Also Check: Is Parkinsons Fatal
Is Parkinsons Disease Fatal
Parkinsons disease itself doesnt cause death. However, symptoms related to Parkinsons can be fatal. For example, injuries that occur because of a fall or problems associated with dementia can be fatal.
Some people with Parkinsons experience difficulty swallowing. This can lead to aspiration pneumonia. This condition is caused when foods, or other foreign objects, are inhaled into the lungs.
Challenges To Classify Disease Stages At The Boundary Of Advpd And Atypical Parkinsonism
During disease progression and based on the predominant motor and non-motor features associated with advPD, the separation from atypical parkinsonism may be difficult and overlap syndromes like minimal change multiple system atrophy or progressive supranuclear palsy with predominant parkinsonism have been described . AP includes a heterogeneous bunch of syndromes, all characterized by clinically manifest parkinsonism in combination with other clinical features and a poor therapeutic response to dopaminergic medication. Only post-mortem analyses can clearly differentiate from advPD, as their neuropathology is characteristically different: in MSA, alpha-synuclein accumulation is found and defines an alpha-syncleinopathy as PD, but mainly in glial cells as cytoplasmic inclusions . In contrast, PSP and corticobasal degeneration are referred to as tauopathies due to characteristic intraneuronal tau aggregation and some TDP-43 proteinopathies might also develop clinical parkinsonism .
In this context, technical tests might further improve the quality of differential diagnosis. Autonomous tests, such as tests for cardiovascular, urinary, thermoregulatory or gastrointestinal dysfunction can be helpful for the diagnostic differentiation PD versus AP. Due to a marked overlap, the combination of several tests such as urodynamic investigation, tests for orthostatic dysregulation, RR-intervals and sympathetic skin response can contribute to support the correct diagnosis.
Read Also: What Is The Life Expectancy Of Someone With Parkinson’s Disease
What Are The Stages Of Parkinson’s Disease
Parkinson’s disease is a progressive neurological disorder. There are five generally recognized stages of Parkinson’s disease. The progression of the disease may vary from one patient to the next, and not all patients will experience all five stages of Parkinson’s disease in their generally accepted order. Symptoms may also vary throughout the progression of Parkinson’s disease.
While doctors have currently identified five distinct stages of Parkinson’s disease, not all patients will experience a straightforward disease progression that passes through all five stages, one after the other. Nor will all patients remain in all stages for the same length of time. The five stages of Parkinson’s often vary in duration from patient to patient. Disease progression is generally considered impossible to predict, with some patients experiencing all stages while other patients skipping from an early stage to an advanced stage without passing through the stages in between.
End Of Life Care Can Be A Difficult Topic To Discuss Do You Have Any Advice On Starting Or Having Conversations On This Subject
I agree, end of life discussions are not easy. We are often not used to thinking about death.
Conversations about end of life must respect patients readiness to discuss these delicate topics, step by step. There should be a choice to make, or not to make, decisions. After identifying care needs in a person with Parkinsons disease and providing suggestions for their management, healthcare professionals can share how the condition may progress when the patient is ready. This conversation might be about complications of late stages of the condition, and how specific palliative applications can help manage these problems.
Conversations might involve identifying the persons wishes about medical and non-medical aspects of end of life preferences for living at home or being cared for in a care home treatment preferences, including resuscitation wishes for the last moments of life and even funeral wishes. There might be a need to appoint a personal representative to the person with Parkinsons disease.
You May Like: What Is The Life Expectancy Of Someone With Parkinson’s Disease
What Are The 5 Stages Of Parkinson’s Disease
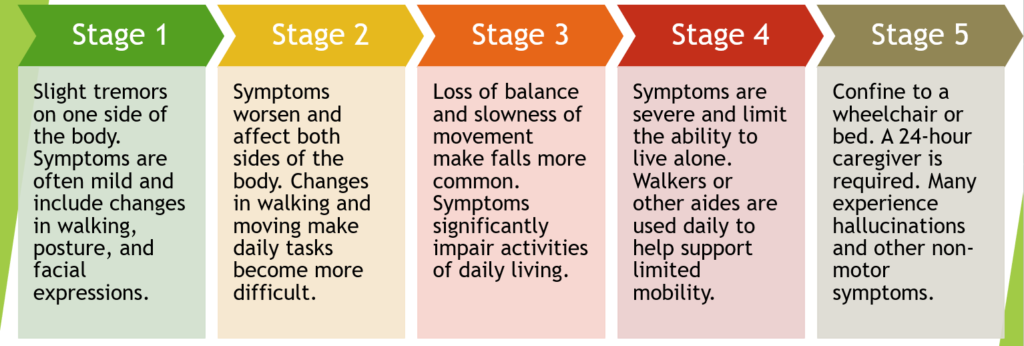
Parkinson’s disease is a neurological movement disorder that’s progressive, meaning symptoms worsen over time. According to the Parkinson’s Foundation, most people move through the stages of Parkinson’s disease gradually .
There’s no lab test that can tell a person which stage their disease is in. Instead, it’s based on how severe a person’s movement symptoms are, and how much the disease impacts their ability to go about daily life.
While the stages of Parkinson’s disease can look a little different for everyone, here’s a typical pattern of the disease, per the Parkinson’s Foundation:
