Gut Dysfunction In Parkinson’s Disease
Correspondence to: Shyamal Kumar Das, MD, DM, Professor, Head, Department of Neurology, Bangur Institute of Neurosciences and Institute of Post Graduate Medical Education and Research, 52/1A Sambhu Nath Pandit Street, Kolkata, West Bengal 700025, India.
Telephone: +91-33-22230003 Fax: +91-33-22236677
What Are The Symptoms Of Parkinsons Disease
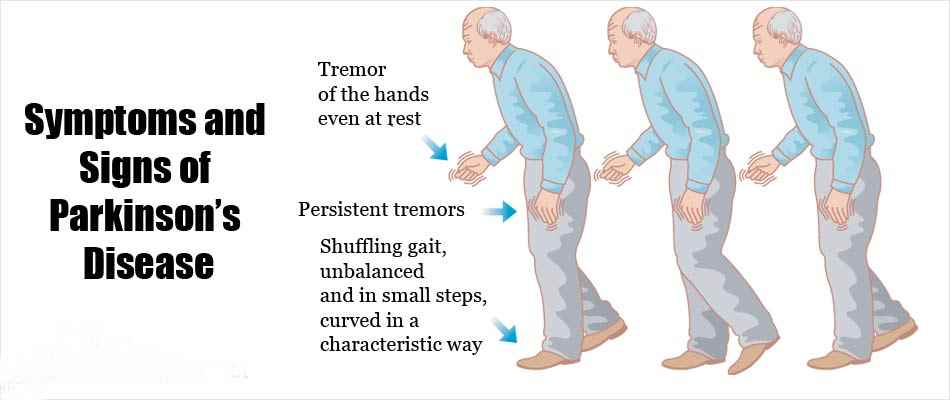
Symptoms of Parkinsons disease and the rate of decline vary widely from person to person. The most common symptoms include:
Other symptoms include:
- Speech/vocal changes: Speech may be quick, become slurred or be soft in tone. You may hesitate before speaking. The pitch of your voice may become unchanged .
- Handwriting changes: You handwriting may become smaller and more difficult to read.
- Depression and anxiety.
- Sleeping disturbances including disrupted sleep, acting out your dreams, and restless leg syndrome.
- Pain, lack of interest , fatigue, change in weight, vision changes.
- Low blood pressure.
Oral And Dental Disorders
Patients with PD have poor oral hygiene. They have fewer remaining teeth, more caries, gingival recession, and increased tooth mobility. The poor oral health may be because of lower frequencies of tooth brushing, motor impairment, apathy, depression, and cognitive impairment. There are reports of PD being associated with bruxism, temporomandibular disorders, and subjective taste impairment. Burning mouth syndrome is more common in PD and this could be because of decreased dopamine levels and dopamine dysregulation. A patient was found to develop burning mouth syndrome with carbidopa/levodopa, which improved when this was replaced with pramipexole.
Recommended Reading: What Are The Side Effects Of Too Much Carbidopa Levodopa
What Causes Parkinsons Disease
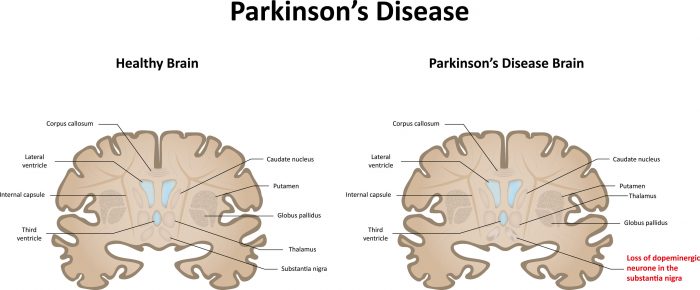
Parkinsons disease occurs when nerve cells, or neurons, in an area of the brain that controls movement become impaired and/or die. Normally, these neurons produce an important brain chemical known as dopamine. When the neurons die or become impaired, they produce less dopamine, which causes the movement problems of Parkinsons. Scientists still do not know what causes cells that produce dopamine to die.
People with Parkinsons also lose the nerve endings that produce norepinephrine, the main chemical messenger of the sympathetic nervous system, which controls many functions of the body, such as heart rate and blood pressure. The loss of norepinephrine might help explain some of the non-movement features of Parkinsons, such as fatigue, irregular blood pressure, decreased movement of food through the digestive tract, and sudden drop in blood pressure when a person stands up from a sitting or lying-down position.
Many brain cells of people with Parkinsons contain Lewy bodies, unusual clumps of the protein alpha-synuclein. Scientists are trying to better understand the normal and abnormal functions of alpha-synuclein and its relationship to genetic mutations that impact Parkinsons disease and Lewy body dementia.
Who Develops Parkinsons Disease
PD mainly develops in people over the age of 50. It becomes more common with increasing age. About 5 in 1,000 people in their 60s and about 40 in 1,000 people in their 80s have PD. It affects men and women but is a little more common in men. Rarely, it develops in people under the age of 50.
PD is not usually inherited and it can affect anyone. However, one type of PD, which appears in the small number of people who develop it before the age of 50, may be linked to inherited factors. Several family members may be affected.
Read Also: Corpus Callosum Coronal
Don’t Miss: Levodopa-induced Dyskinesia
Introduction: The Polyvagal Theory
The different Nervous Systems can also have their own “sub-programs”. For example, the Para-Sympathetic NS includes the Vagal Nerves and other Cranial Nerves. These sub-systems may themselves branch in multiple ways too, conveying different information and affecting different parts of the brain and body through their own instruction sets. The “Polyvagal Theory” of Dr Stephen Porges reveals how the Vagus Nerve has a multiplicity of branches . Application of this theory provides us the required framework of understanding, which for the first time, allows us to explain Parkinson’s Disease completely and coherently. In this article, I would like to try to provide as clearly as possible the explanation, in order to help other people with PD ease their suffering.
Porges’ original paper is very long and full of unfamiliar jargon, and the theory has evolved over time with the originator’s own understanding, however our focus here is firmly on the pragmatic application of the theory to Parkinson’s Disease, not on the intricacies of the theory itself. The aim is to:
-
break Porges’ original work down in to a much more readily understandable form
-
provide simple and elegant explanations for people with PD, which we can apply in real life
-
avoid getting bogged down in technical details or exactitude
-
cover only the original, basic version of the theory, as this is more than sufficient at this stage.
How Does Parkinsons Disease Affect Balance And Posture
Problems with unsteady balance and posture may make it hard for a person with Parkinsons disease to sit down in a chair or to rise from one. Walking is accomplished with small, shuffling steps and a stooped posture, usually without the normal arm-swinging motions. Bradykinesia can affect the facial muscles,
You May Like: Parkinson’s Disease Mayo
When Parkinsons Interferes With Gastrointestinal Function
This 63-minute audio with slides by Dr. Peter A. LeWitt discusses the effect of Parkinsons disease on the gastrointestinal system, with particular focus on constipation. Improving GI function can have a positive impact on the consistency of benefit from Parkinsons disease medications. Highlights of recent research into Parkinsons disease originating in the GI tract, developing biomarkers for early diagnosis, and others.
Caregiving For People Living With Parkinsons
Caring for a loved one with PD can be a challenging job, especially as the disease progresses. Former caregivers of a loved one with PD suggest doing the following : Get prepared, Take care of yourself, Get help , Work to maintain a good relationship with your loved one, and Encourage the person with PD for whom you care, to stay active.
Preparing for caregiving starts with education. Reading this fact sheet is a good start. More resources are available to you in theResources section of this fact sheet. Early Parkinsonâs disease usually requires more emotional support and less hands-on care. It is a good time for family members/caregivers to educate themselves about the disease.
You May Like: Does Prevagen Help With Memory Loss
You May Like: Parkinson’s Disease Genes
How Is Parkinsons Disease Diagnosed
Diagnosing Parkinsons disease is sometimes difficult, since early symptoms can mimic other disorders and there are no specific blood or other laboratory tests to diagnose the disease. Imaging tests, such as CT or MRI scans, may be used to rule out other disorders that cause similar symptoms.
To diagnose Parkinsons disease, you will be asked about your medical history and family history of neurologic disorders as well as your current symptoms, medications and possible exposure to toxins. Your doctor will look for signs of tremor and muscle rigidity, watch you walk, check your posture and coordination and look for slowness of movement.
If you think you may have Parkinsons disease, you should probably see a neurologist, preferably a movement disorders-trained neurologist. The treatment decisions made early in the illness can affect the long-term success of the treatment.
What Kind Of Pain Does Parkinsons Cause
The types of pain associated with Parkinsons include: aching or burning pain from muscles or skeleton, sharp pain from a nerve or nerve root, numbness or pins and needles pain also radiating from a nerve or nerve root, pulsing or aching pain that results from tightness or ongoing twisting and writhing movements (
Also Check: What Happens In Stage 5 Of Parkinson’s Disease
The Role Of Other Cranial Nerve
In humans, the Vagal NS is also inter-linked with other Cranial Nerves, including the trigeminal, facial, accessory and glossopharyngeal nerves. These nerves control muscles and sensation in the face, biting, chewing, the tongue, tilting and rotation of the head, shoulder movements, ear membranes, sucking in air, and muscles in the throat for vocalization and swallowing.
The Smart VN systems in humans therefore integrates functions such as head rotation to orient the senses toward the source of stimulation, mastication to ingest food, salivation to initiate digestive processes, facial expression and creating noises for purposes of social communication.
Furthermore, in evolutionary terms, the voluntary muscles supplied by these five Cranial Nerves evolved from regions in the body which were gills in early stages of life, and hence were, and remain, strongly associated with oxygen supply and chemically sensing oxygen and carbon dioxide levels in the body. They influence the rate of rhythmic movements such as heart beat, impacting on states of stress or relaxation, via the voluntary control of breathing, and are also responsible for voluntary control of the volume and tone of vocalizations .
Hence the overall Smart VN System is also strongly associated with movement, emotion, and communication, contributing to the unique social and survival behaviors observed in mammals.
Treatment For Constipation In Parkinsons Disease
Your doctor may suggest various treatments to help combat constipation, including:
- dietary changes, including more fibre rather than refined or highly processed foods, and water
- avoidance of unnecessary medicines that contain substances known to cause constipation
- laxatives, particularly agents that bulk and lubricate the stools
- treatment for any other medical problem that may be contributing to your constipation, such as haemorrhoids .
Read Also: Parkinson’s Stages Life Expectancy
How Does Alcohol Affect Parkinsons Medication
The interaction between Parkinsons medications and alcohol is a common topic on MyParkinsonsTeam. I miss my red wine and whiskey on occasion, one member wrote. I found that it just makes my meds stop working. Another member said, My husband has been told he shouldn’t drink with his meds.
Alcohol can exacerbate the side effects of one of the most common Parkinsons medications, levodopa/carbidopa. Many neurologists recommend avoiding alcohol while taking this drug.
I have to limit myself to one Scotch on the rocks now, a MyParkinsonsTeam member said. I used to have three or four, but the side effects are too bad. Another wrote, Never really a good idea to mix alcohol with meds.
Whether you decide to continue your current drinking habits, cut down, or eliminate alcohol altogether, its important to listen to your body and have open conversations about these topics with your neurologist.
If you find yourself drinking alcohol to cope with other issues, such as depression and anxiety, you may find that healthy practices such as physical activity can help. In addition, participating in activities such as tai chi, yoga, and meditation may help ease the symptoms and complications of PD.
How Do I Prevent Falls From Common Hazards
- Floors: Remove all loose wires, cords, and throw rugs. Minimize clutter. Make sure rugs are anchored and smooth. Keep furniture in its usual place.
- Bathroom: Install grab bars and non-skid tape in the tub or shower. Use non-skid bath mats on the floor or install wall-to-wall carpeting.
- Lighting: Make sure halls, stairways, and entrances are well-lit. Install a night light in your bathroom or hallway and staircase. Turn lights on if you get up in the middle of the night. Make sure lamps or light switches are within reach of the bed if you have to get up during the night.
- Kitchen: Install non-skid rubber mats near the sink and stove. Clean spills immediately.
- Stairs: Make sure treads, rails, and rugs are secure. Install a rail on both sides of the stairs. If stairs are a threat, it might be helpful to arrange most of your activities on the lower level to reduce the number of times you must climb the stairs.
- Entrances and doorways: Install metal handles on the walls adjacent to the doorknobs of all doors to make it more secure as you travel through the doorway.
You May Like: Pontine Syndromes
Leaky Blood Brain Barrier And Parkinson’s Disease
which explains how both the blood brain barrier and the gut lining can lose their protective functions in a variety of ways. Given that leaky gut and leaky brain are both heavily implicated in the disease, the road blocks between chemicals produced in the gut reaching the brain is not so assured for people with Parkinson’s. For example, unusually high levels of histamine, which is naturally produced in the gut as part of digestion, have been found in the brains of people with PD
Who Gets Parkinsons Disease
About 1 million people in the United States have Parkinsons disease, and both men and women can get it. Symptoms usually appear when someone is older than 50 and it becomes more common as people get older.
Many people wonder if youre more likely to get Parkinsons disease if you have a relative who has it. Although the role that heredity plays isnt completely understood, we do know that if a close relative like a parent, brother, or sister has Parkinsons, there is a greater chance of developing the disease. But Parkinsons disease is not contagious. You cant get it by simply being around someone who has it.
You May Like: Does Jamie Foxx Have Parkinson’s
Can Parkinsons Disease Be Prevented
Unfortunately, no. Parkinsons disease is long-term disease that worsens over time. Although there is no way to prevent or cure the disease , medications may significantly relieve your symptoms. In some patients especially those with later-stage disease, surgery to improve symptoms may be an option.
Constipation And The Gut In Parkinson’s
One of the effects Parkinsons has on the autonomic nervous system seems to be the slowing of food through the gastrointestinal tract, which can result in constipation . As many as 80% of people with PD have constipaiton. In this 1-hour webinar Cherian Karunapuzha, MD, shares how you can best manage your bowel and urinary symptoms to live well with Parkinsons.
Also Check: How Long Does Parkinsons Take To Progress
Constipation And Parkinsons Disease
Constipation is one of the most commonly reported GI symptoms of Parkinsons disease, affecting 60-80% of patients.17,18 Constipation occurs when movement of material through the GI system slows down. This slowing can result from the direct effects of Parkinsons disease upon the action of intestinal muscles that would normally act to massage material through the intestines in a wave-like action , or indirectly through side-effects of some medications.19 In severe cases, accounting for approximately 7% of those with a parkinsonism, compromised peristalsis can lead to complete gut blockage resulting in further symptoms such as cramping, abdominal pain, vomiting, and bloating.16
Medication Side Effects And The Gut
The interactions between PD medication ingestion and the gut can play a major role in motor fluctuations the phenomenon in which a patients response to Levodopa varies widely during the day. A recent APDA webinar helps to explain this interplay.
Delayed gastric emptying
Delayed gastric emptying can interfere with medication absorption. Medication doses that are ingested by mouth may sit in the stomach before being transported to the small intestine where they are absorbed. Delayed gastric emptying could be responsible for dose failures when a dose of medication does not have a robust enough effect.
Protein effect
Levodopa crosses the wall of the small intestine via a molecule in the intestinal wall that transports amino acids, the building blocks of protein. When dietary protein is also present in the small intestine, then there are fewer transporters available for Levodopa to use. A patient may therefore experience the protein effect, in which he or she feels that medication is not as effective after a high-protein meal. Sources of dietary protein include: beef, chicken, pork, fish, eggs, nuts and dairy.
Helicobacter pylori and small intestinal bacterial overgrowth
About a third of PD patients are infected with Helicobacter pylori, a common bacteria which can cause gastritis and ulcers. Infection with Helicobacter pylori has been linked to worsened motor fluctuations. It can be diagnosed with a urea breath test that analyzes exhaled air.
Read Also: Michael Bolton Plastic Surgery
Parkinsons And Difficulty Sleeping
More than 75 percent of people with Parkinsons disease report sleep problems. You may experience restless sleep, where you wake up frequently during the night.
You may also experience sleep attacks, or episodes of sudden sleep onset, during the day. Talk with your doctor about treatment methods, such as taking an over-the-counter or prescription sleep aid to help you regulate your sleep.
The Heart Of The Matter: Cardiovascular Effects Of Parkinsons Disease
It has long been understood that Parkinsons disease does not just cause movement symptoms, but also causes a litany of non-motor symptoms with effects throughout the body. One of the organ systems that is affected is the cardiac system, encompassing the heart, as well as the major and minor blood vessels. I received this topic as a suggestion from a blog reader and we will be discussing this important issue today. Please feel free to suggest your own blog topic.
Don’t Miss: Restore Gold Supplement For Parkinson
Background: The Stomach Parkinson’s And Levodopa
Levodopa is not absorbed from the stomach, but the stomach plays an important role in controlling how levodopa reaches the parts of the small intestine where it is absorbed. Some medicines, including dopamine agonists and anticholinergics, can also delay gastric emptying, as can severe stomach acidity, although over-treatment of this problem can also prevent the break-down of levodopa tablets, leading to incomplete absorption.
Unfortunately, gastric emptying can be delayed by Parkinsons itself or by constipation caused by the colon-gastric reflex. Levodopa tablets may remain in the stomach for a long time, leading to delayed absorption in the small intestine and a delayed response to the treatment.
An enzyme called dopa-decarboxylase that is present in the stomach lining can convert levodopa trapped in the stomach into dopamine, making it unavailable to the central nervous system. Also, dopamine formed in the stomach may stimulate gastric dopamine receptors, leading to stomach relaxation and reduced gastric motility, and this can worsen the problem.
Liquid levodopa may improve motor fluctuations by ensuring better absorption than standard preparations, especially when taken after meals. Subcutaneous infusion of the dopamine agonist apomorphine is effective in controlling motor fluctuations by bypassing the gastrointestinal tract.
