Complications Related To Parkinson’s Can Affect Survival
Claudia Chaves, MD, is board-certified in cerebrovascular disease and neurology with a subspecialty certification in vascular neurology. She is an associate professor of neurology at Tufts Medical School and medical director of the Lahey Clinic Multiple Sclerosis Center in Lexington, Massachusetts.
Parkinson’s;is a common neurodegenerative disease, and although it is not fatal, research suggests it may influence life expectancy.
A 2012 study in Archives of Neurology examined the six-year survival of nearly 140,000 Medicare beneficiaries with Parkinson’s disease in the United States. During the six-year period, 64% of the participants with Parkinson’s disease passed away.
The risk of death of those with Parkinson’s was then compared to Medicare beneficiaries who did not have Parkinson’s or any other common diseases, including:
When controlling for variables like age, race, and gender, the six-year risk of death among people with Parkinson’s was found to be nearly four times greater than those Medicare beneficiaries without the;disease or other common diseases.
At the same time, the rate of death among those with Parkinson’s disease was similar to those with hip fracture, Alzheimer’s dementia, or a recent heart attackalthough it was higher than those who had been newly diagnosed with either colorectal cancer, stroke, ischemic heart disease, or chronic obstructive pulmonary disease.
Is Parkinsons Disease Fatal
Parkinsons disease itself doesnt cause death. However, symptoms related to Parkinsons can be fatal. For example, injuries that occur because of a fall or problems associated with dementia can be fatal.
Some people with Parkinsons experience difficulty swallowing. This can lead to aspiration pneumonia. This condition is caused when foods, or other foreign objects, are inhaled into the lungs.
How Is Parkinson’s Managed
There is currently no cure for Parkinsons but there are medications and therapies that can help to manage Parkinsons symptoms.
Medicines that increase the level of dopamine in the brain are the main treatment used to manage the;symptoms of Parkinson’s. Medicines are tailored to each individuals needs.
Symptoms will get worse when someones Parkinsons medicines are wearing off and improve again after Parkinsons medicines are taken. If people with Parkinsons dont get their medication at the right time, it leads to their motor symptoms becoming uncontrolled. It can take some time to get their symptoms under control again.;If you work in a hospital or care home, it is important to be aware that medicine timings will vary from person to person and may be different to ward medicine rounds.
As well as medicines, surgical options are available for some people with;Parkinson’s, depending on their symptoms.
Treatments can help to manage the symptoms, but may become less effective in the later stages of the condition.
Parkinsons UK ; has more information on how Parkinsons affects people and how it can be managed.
Also Check: What Is The Life Expectancy Of Someone With Parkinson’s Disease
Causes Of Parkinsons Disease
At present, we do not know the cause of Parkinsons disease. In most people there is no family history of Parkinsons Researchers worldwide are investigating possible causes, including:;
- environmental triggers, pesticides, toxins, chemicals
- genetic factors
- combinations of environment and genetic factors;
- head trauma.
Do All Parkinsons Patients Develop Dementia
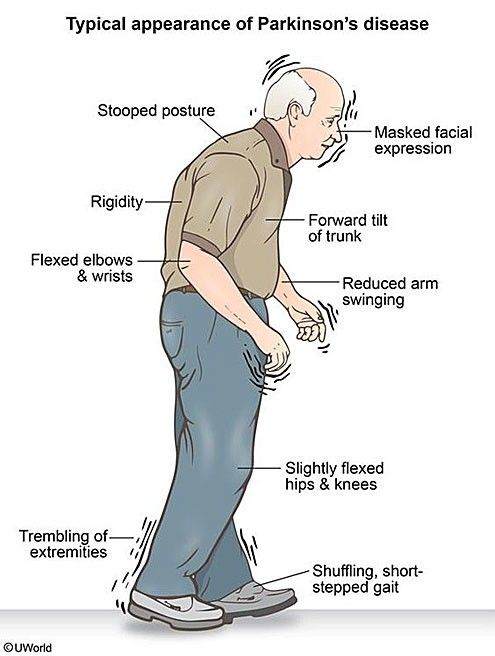
Although dementia is a hallmark of Alzheimers disease, dementia may occur in Parkinsons disease affecting approximately 70% of the patients.
Dementia describes a set of symptoms that cause is a significant loss in brain function. It produces a greater impact on patients on patients with Parkinsons than in Alzheimers patients as they have to deal with motor and cognitive impairment.
Alzheimers affect memory and language in general terms. Still, in Parkinsons, it affects problem-solving capacity, speed of thinking, memory, and they run with mild cognitive impairment.
Notably, Parkinsons disease dementia is a common thing among patients with this condition. The vast majority of them may experience some form of cognitive impairment over time.
Though it is a unique process for each person, several risk factors may lead to dementia symptoms and dementia itself.
- Increasing age.
- Exposure to psychological stress
- Low education level and low socioeconomic status
Disease duration has as well a direct correlation with the development of dementia on these patients. The more time the patient has this disease, the risk of developing dementia increases.
Also, Parkinsons dementia has a direct correlation with Lewy bodies. Most people develop dementia as a progression of the disease rather than having Parkinsons and Alzheimers. Nonetheless, a doctor with a neurology specialist should examine the patient to give an assertive diagnosis to the condition.
Also Check: What Is The Life Expectancy Of Someone With Parkinson’s Disease
Theory Of Pd Progression: Braaks Hypothesis
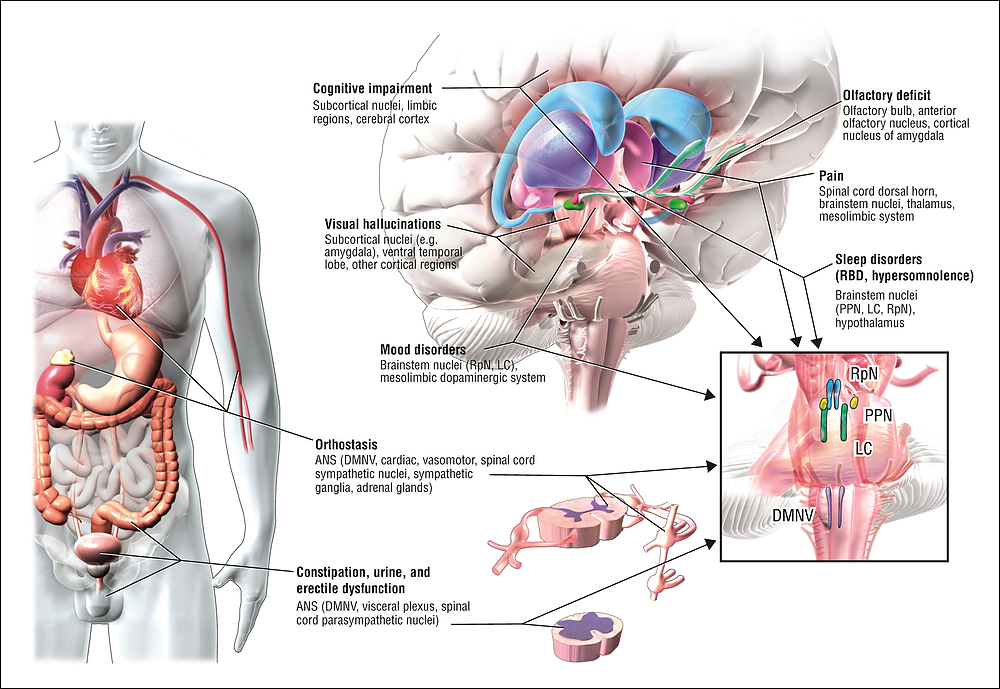
The current theory is that the earliest signs of Parkinson’s are found in the enteric nervous system, the medulla and the olfactory bulb, which controls sense of smell. Under this theory, Parkinson’s only progresses to the substantia nigra and cortex over time.
This theory is increasingly borne out by evidence that non-motor symptoms, such as a loss of sense of smell , sleep disorders and constipation may precede the motor features of the disease by several years. For this reason, researchers are increasingly focused on these non-motor symptoms to detect PD as early as possible and to look for ways to stop its progression.
Page reviewed by Dr. Ryan Barmore, Movement Disorders Fellow at the University of Florida, a Parkinsons Foundation Center of Excellence.
*Please note that not all content is available in both languages. If you are interested in receiving Spanish communications, we recommend selecting both” to stay best informed on the Foundation’s work and the latest in PD news.
Can You Die From Parkinson’s
Advanced symptoms of a long-term condition like Parkinsons can make people more vulnerable to poor health and increased disability. These complications can sometimes result in someone dying. When this happens, Parkinsons can be recorded as a cause of death.
Complications can include:
- aspiration pneumonia
- falls
- chest infections and pneumonia;
This is one of the reasons why its important to manage your condition as well as you can, with the support of specialist healthcare professionals.; ;
Recommended Reading: Differences Between Huntington’s And Parkinson’s
Skin And Sweat Glands
The autonomic nervous system also controls the sweat glands of the skin. Both excessive sweating and a decrease in sweating are common Parkinsons symptoms. This may be due to a compensatory reaction to a decline of nervous function in extremities. However, Parkinsons patients with anhidrosis are rare, but it can happen.
Caring For Your Health With Parkinson’s Disease
In addition to caring for your Parkinson’s health, it is also important to care for your overall health. This means visiting your primary care physician periodically for preventive care like the annual flu shot and cancer screeningsfor example, a mammogram for breast cancer screening and a colonoscopy for colon cancer screening.
A primary care physician can also evaluate for risk factors related to heart attacks and strokes, and;provide counseling on exercise, smoking, alcohol use, depression, or other mental health concerns. Regular visits to your primary care physician or neurologist will also allow them to catch bacterial infections like urinary tract infections before they get serious.
Don’t Miss: What Color Represents Parkinson’s Disease
What Happens In Stage 5 Parkinson’s
Stage 5Stage 5stageParkinson’s
When patients reach stage five the final stage of Parkinson’s disease they will have severe posture issues in their back, neck, and hips. In end–stage of Parkinson’s disease, patients will also often experience non-motor symptoms. These can include incontinence, insomnia, and dementia.
One may also ask, how long does a person live with stage 5 Parkinson’s? Parkinson’s Disease is a Progressive DisorderIndividuals with PD have a somewhat shorter life span compared to healthy individuals of the same age group. Patients usually begin developing the disease around age 60, and many live between 10 and 20 years after being diagnosed.
Herein, what happens in stage 5 of Parkinson’s disease?
Stage Five of Parkinson’s DiseaseStage five is the most advanced and is characterized by an inability to arise from a chair or get out of bed without help. They may have a tendency to fall when standing or turning, and they may freeze or stumble when walking.
What do Parkinson’s patients usually die from?
But the most common cause of death in those with Parkinson’s is pneumonia, because the disease impairs patients‘ ability to swallow, putting them at risk for inhaling or aspirating food or liquids into their lungs, leading to aspiration pneumonia.
Identifying Newly Diagnosed Pd Patients And Matched Controls For Each Pd Patient
The study population comprised newly diagnosed patients with PD and their matched controls. First, we identified PD patients using the registration code for PD in the program for rare, intractable disease from January 1, 2004, to December 31, 2006, and we defined the index date as the date of the earliest claim with the V124 code. To remove any prevalent cases, we excluded patients who had PD diagnostic codes or PD registration codes before January 1, 2004. As the V124 registration criteria did not exclude atypical Parkinsonian syndromes, we excluded patients diagnosed with atypical parkinsonism during the entire study period, from 2002 to 2017. Moreover, we excluded patients under 40;years of age. Lastly, we excluded patients whose total number of days of antiparkinsonian medications was less than 180;days. The list of the antiparkinsonian medications used in this study is given in Supplementary Table .
Then, we selected up to four controls for each PD patient matched by sex and age at the index date. Previous studies reported that matching 4 controls to 1 patient can minimize the bias in measuring treatment effect in the maximum number of matched controls,. Individuals who had the registration code for rare, intractable disease for PD , had any diagnostic code for Parkinsonism , or had been prescribed an antiparkinsonian drug during the study period were not recruited as controls.
Don’t Miss: How To Treat Parkinson Disease Naturally
What Are The Symptoms Of Parkinson’s
The main motor symptoms of Parkinsons are:
- tremor
- slowness of movement
- problems with balance.
However, the condition doesnt only affect movement. People living with the condition can experience a range of non-motor symptoms that can often have a greater impact on their lives than movement difficulties.
Non-motor symptoms include:
- urinary urgency, frequency
- pain.
These non-motor symptoms are present at all stages of the condition but they can become more severe in the later stages of Parkinsons and have a major impact on quality of life.
Parkinsons gets worse over time and it can be difficult to predict how quickly the condition will progress. For most people, it can take years for the condition to progress to a point where it can cause major problems.;For others, Parkinsons may progress more quickly.
What Causes Parkinson Disease
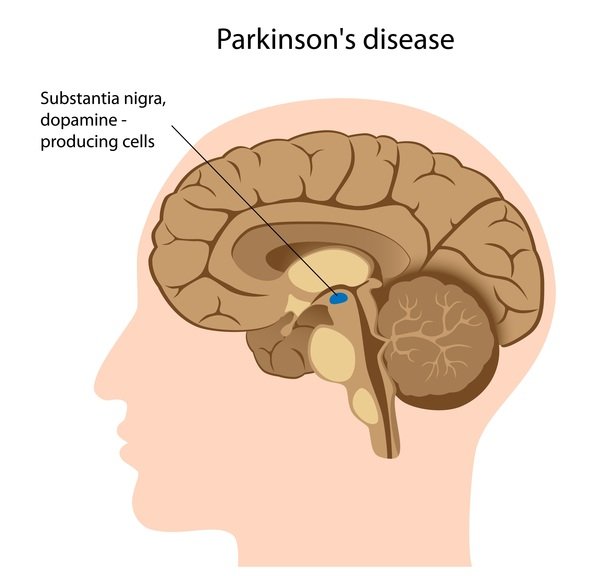
Parkinson disease arises from decreased dopamine production in the brain. The absence of dopamine makes it hard for the brain to coordinate muscle movements. Low dopamine also contributes to mood and cognitive problems later in the course of the disease. Experts don’t know what triggers the development of Parkinson disease most of the time. Early onset Parkinson disease is often inherited and is the result of certain gene defects.
Read Also: Is Parkinson’s Disease Always Fatal
What You Can Do
As of 2021, there is no definite cure for Parkinsons disease. There is also no definite known cause. Its likely due to a combination of an individuals susceptibility and environmental factors. Most cases of Parkinsons disease happen without a genetic link.
According to research published in 2012, only report having a family member with the disease. Many toxins are suspected and have been studied, but no single substance can be reliably linked to Parkinsons.
However, research is ongoing. Its estimated that
How Is Parkinsons Diagnosed
Doctors use your medical history and physical examination to diagnose Parkinson’s disease . No blood test, brain scan or other test can be used to make a definitive diagnosis of PD.
Researchers believe that in most people, Parkinson’s is caused by a;combination of;environmental and genetic;factors. Certain environmental exposures, such as pesticides and head injury, are associated with an increased risk of PD. Still, most people have no clear exposure that doctors can point to as a straightforward cause. The same goes for genetics.;Certain genetic mutations are linked to an increased risk of PD. But in the vast majority of people, Parkinsons is not directly related to a single genetic mutation. Learning more about the genetics of Parkinsons is one of our best chances to understand more about the disease and discover how to slow or stop its progression.
Aging is the greatest risk factor;for Parkinsons, and the average age at diagnosis is 60.;Still, some people get PD at 40 or younger.
Men are diagnosed with Parkinsons at a higher rate than women and whites more than other races. Researchers are studying these disparities to understand more about the disease and health care access and to improve inclusivity across care and research.;
Aging is the greatest risk factor;for Parkinsons, and the average age at diagnosis is 60.;Still, some people get PD at 40 or younger.
The Michael J. Fox Foundation has made finding a test for Parkinsons disease one of our top priorities.
Read Also: What Are The Four Cardinal Signs Of Parkinson’s Disease
Two Areas In Which Parkinsons Disease May Bring About Death
I. Falls
PD patients are at an increased risk of falling and bad falls can lead to death. This usually occurs as a complication of a fall that requires hospitalization, particularly if it involves surgery. While most people do not fracture their hips when they fall, some do, and hip surgery, while routine, is still major surgery. It carries the risk of infection, delirium related to pain medications and anesthesia, heart failure, pneumonia, blood clots in the legs that then go to the lungs, and general weakness from immobility. Hip fractures are probably the main cause for death for those who fall, but people can fracture other bones and require surgery. They may fracture their ribs, which leads to reduced coughing, because of the pain, and an increased risk of lung infections . It is surprisingly uncommon for Parkinsons Disease patients to die from brain injuries related to falls, but it still may occur.
II. Pneumonia
PD patients also may develop pneumonias completely unrelated to difficulties with swallowing, just like their non-PD friends and relatives.
What Are The Risks Of Not Receiving Any Dopaminergic Medication
There is the possibility of neuroleptic malignant-like syndrome , a life-threatening and distressing condition resulting in rigidity and fever, from withdrawal of therapy.31;This can also occur with sudden cessation of Deep Brain Stimulation .32,33,34;To reduce the risk of this, dopaminergic therapy at the end of life should be continued.27;It should also be noted that in a patient dying of another condition, whose PD is still responsive to dopaminergic medication, the cessation of this also risks aspiration pneumonia.35;Transdermal rotigotine can be used in patients in whom a NG tube may cause excessive distress or is not possible. The dose should be calculated with an accepted converter.36
Don’t Miss: Parkinson’s Awareness Color
If You Live In South Jersey And Have Questions About The Final Stages Of Parkinsons Disease Or Hospice Care For Your Loved One Please Call Samaritan At 229
Samaritan is a member of the;National Partnership for Healthcare and Hospice Innovation, a network of not-for-profit hospice and palliative providers across the country. If you know someone outside of our service area who is living with advanced illness and can benefit from hospice or palliative care, please call;1 -GET-NPHI; for a referral to a not-for-profit provider in your area.
What Symptoms Can Be Expected In Advanced Pd
- Pain 86%
- Shortness of breath 54%
- Problems in swallowing 40%14
In an analysis of 339 death certificates and medical notes in the UK, pneumonia was found to be a terminal event in 45%.13
Caregiver distress with choking and the risk of choking to death is also mentioned in a separate study in to experiences regarding all stages of PD.4
In a survey of symptoms and their association with quality of life, in those patients with advanced disease, uncontrolled pain, anxiety and hallucinations were significantly associated with poor quality of life.9
Seizures are also noted in a description of the last phase of Parkinsonian syndromes,15;and in retrospective studies of PD patients overall.16,17
These above symptoms often occur on the background of weight loss, pain, and cognitive impairment. It is important therefore to note which medications given at the end of life may exacerbate these symptoms, and which should be considered in anticipation of them.
Recommended Reading: Is Parkinson’s Disease Deadly
Can A Patients Ability To Make Decisions In The Last Days Of Life Be Impaired And How Is This Managed
In a North American study of 47 carers of idiopathic PD patients in the last months of life most described the goal of care as comfort, and almost half of the patients were described as unable to make any decisions in the last month of life. 10
When presenting, the patient may already be unable to communicate their symptoms and care preferences due to cognitive impairment and confusion. Also, there might be a physical difficulty in communication from severe rigidity. Care should be taken in considering the presence and consequent treatment of an intercurrent illness, and whether dopaminergic medication is exacerbating confusion due to hallucinations and/or psychosis.27;
Continued attempts at verbal and non-verbal communication should be made throughout given the often fluctuating symptoms associated with PD and possible improvement in the intercurrent illness. In the absence of a next of kin or other person who is able to inform the clinical team, decisions should be made on a best interest basis as recommended in end of life care guidance.30
What To Do With Deep Brain Stimulation At The End Of Life
Deep brain stimulation uses an Implantable Pulse Generator, usually placed in the infraclavicular area, connected to leads within the brain. There is a remote programmer, and also a charging unit in the case of a rechargeable device, which are given to the patient and their carer. It improves dyskinesias and also has a levodopa sparing effect.37
Deactivation of DBS may lead to increased symptom burden as mentioned in the section above and so awareness of features of PHS should be considered if there is failure at the end of life. Supportive treatment should be given if possible,38;and anticipation of symptoms of distress from rigidity and fever.
After death, deactivation of the device with the patients handheld programmer is required before removing the pulse generator and battery in the case of a cremation.
Don’t Miss: Parkinsons Heritability
