Can Stress Make Parkinsons Disease Worse
Stress is according to the researches, the pervasiveness of various diseases. There is ample evidence that the symptoms of Parkinsons disease worsen with stress. The impact of psychological stress on Parkinsons disease is essentially adversely negative, making the progression of the disease faster.
What Medications Are Used To Treat Parkinsons Disease
Medications are the main treatment method for patients with Parkinsons disease. Your doctor will work closely with you to develop a treatment plan best suited for you based on the severity of your disease at the time of diagnosis, side effects of the drug class and success or failure of symptom control of the medications you try.
Medications combat Parkinsons disease by:
- Helping nerve cells in the brain make dopamine.
- Mimicking the effects of dopamine in the brain.
- Blocking an enzyme that breaks down dopamine in the brain.
- Reducing some specific symptoms of Parkinsons disease.
Levodopa: Levodopa is a main treatment for the slowness of movement, tremor, and stiffness symptoms of Parkinsons disease. Nerve cells use levodopa to make dopamine, which replenishes the low amount found in the brain of persons with Parkinsons disease. Levodopa is usually taken with carbidopa to allow more levodopa to reach the brain and to prevent or reduce the nausea and vomiting, low blood pressure and other side effects of levodopa. Sinemet® is available in an immediate release formula and a long-acting, controlled release formula. Rytary® is a newer version of levodopa/carbidopa that is a longer-acting capsule. The newest addition is Inbrija®, which is inhaled levodopa. It is used by people already taking regular carbidopa/levodopa for when they have off episodes .
Recommendations For Future Studies
Future trials should be adequately powered to demonstrate a clinically meaningful difference between a mindfulness and control intervention . The optimal control intervention should have a similar duration and amount of personal contact as mindfulness and should not differ in degree of physical exercise. When investigating the effect of mindfulness on disease progression, it is possible that interventions longer than 8âweeks are needed . Promising outcome measures include anxiety and depression , and it might be considered to test the merits of mindfulness in a sample of patients with PD scoring high on these symptoms. It would also be informative to assess effects on other nonmotor symptoms, such as pain, sleeping problems, and digestive issues. Any effects on motor symptoms are currently less clear, and these may be better investigated using wearable devices to identify even subtle improvements or using functional outcome measures. Specifically, such functional measures could include brain imaging , activity of the HPA axis , or inflammatory markers , and these may help to better understand the underlying working mechanisms. Follow-up should ideally be 6âmonths or longer, because the effects of a mindfulness-based intervention may consolidate with longer follow-up.
Read Also: Alice Waters Parkinson’s
Identify The Cause Of Stress
Thiss the first step in dealing with stress. There could be many things that trigger stress in Parkinsons disease. It could be related to your symptoms like specific movements, difficulty in talking, eating, and falling sleep or it could be due to other problems. If you can recognize them, you can learn to address them.
Depression And Parkinsonism In An Animal Model Of Neurodegeneration
Early post-natal maternal separation is widely used to create an animal model that exhibits some depressive/anxiety-like behaviors . This established model of depression is useful to study 6-OHDA lesion of the medial forebrain bundle to lesion nigrostriatal DA neurons. We recently investigated the antiparkinsonian effects of Fluvoxamine maleate in a parkinsonian rat model of neurodegeneration associated with anxiety/depressive-like behaviors . Although these studies were a small exploratory open-label trial, they anticipated outcomes on a larger double-blind placebo-controlled study that include non-depressive animals with Parkinsonism. Fluvoxamine maleate treatment has shown potential in decreasing dopaminergic neuronal loss as well as potential to regulate neuronal pro- and anti-inflammation markers in the striatum . Therefore, a combined animal model of chronic stress-induced depression with a 6-OHDA lesioned parkinsonian animal model is an appropriate model to investigate the relationship between depression and PD. This association suggests that the stressor needs to be applied prior to the injection of the neurotoxin 6-OHDA to combine depressive-like behaviors with a potential risk of developing motor-symptoms that characterize Parkinsonism. This combination showed the double advantage of investigating a non-motor symptom as part of an early onset of PD together with the neuroprotective effects of a treatment on the development of the disease.
Also Check: Adderall For Parkinson’s
An Integrated Review Of Psychological Stress In Parkinsons Disease: Biological Mechanisms And Symptom And Health Outcomes
Kim Wieczorek Austin
1Virginia Commonwealth University School of Nursing, 1100 East Leigh Street, Richmond, VA 23219, USA
2Virginia Commonwealth University Parkinsons and Movement Disorders Center and VCU Health Neuroscience, Orthopaedic, and Wellness Center, 11958 West Broad Street, Richmond, VA 23233, USA
Abstract
1. Introduction
The unpredictable and debilitating nature of the symptoms associated with PD combined with the inability to halt or slow disease progression has the potential to result in psychological stress. Psychological stress is a complex phenomenon that involves cognitive, emotional, behavioral, and biological responses to events or experiences that are perceived as threatening . An individuals ability to cope with and adapt to psychological stress can be influenced by the number and significance of stressful events experienced within a given period of time, the degree to which stressors are perceived as threatening or harmless, and biological responses designed to promote adaptation . The inability to cope with or adapt to psychological stress has been associated with poorer symptom and health outcomes that may be relevant in PD. For example, in non-PD populations, significant relationships have been demonstrated between psychological stress and increased motor symptomology , pain , fatigue, , cognitive decline , and functional disability .
2. Methods
3. Results and Discussion
4. Conclusion
Disclosure
Competing Interests
References
Other Causes Of Parkinsonism
“Parkinsonism” is the umbrella term used to describe the symptoms of tremors, muscle rigidity and slowness of movement.
Parkinson’s disease is the most common type of parkinsonism, but there are also some rarer types where a specific cause can be identified.
These include parkinsonism caused by:
- medication where symptoms develop after taking certain medications, such as some types of antipsychotic medication, and usually improve once the medication is stopped
- other progressive brain conditions such as progressive supranuclear palsy, multiple systems atrophy and corticobasal degeneration
- cerebrovascular disease where a series of small strokes cause several parts of the brain to die
You can read more about parkinsonism on the Parkinson’s UK website.
Page last reviewed: 30 April 2019 Next review due: 30 April 2022
Don’t Miss: Weighted Blanket Parkinson’s
Noradrenaline Hypothesis Of Depression
Noradrenaline is known to play a role in the regulation of emotions . The deficiency of noradrenaline/norepinephrine mainly produced in the locus coeruleus and affecting certain brain areas such as the prefrontal cortex, the hippocampus or the hypothalamus has been associated with depression . Studies have shown that exposure to chronic stress including early maternal separation decreases noradrenaline levels within the brain leading to depression . This explains why selective norepinephrine re-uptake inhibitors , a new class of antidepressants that work by increasing norepinephrine levels in the brain, have been used to treat depression .
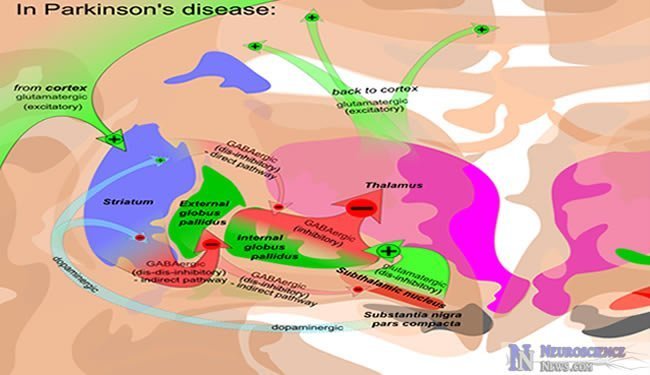
Dopamine Hypothesis Of Depression
Dopamine is produced in the substantia nigra pars compacta in the midbrain. Dopaminergic projections in both the mesocortical and the mesolimbic systems are known to be disturbed by stress . Dopaminergic pathways are part of the reward system and the effects of chronic stress on reward perception that lead to depression can occur because of the interaction between the dopaminergic system and the HPA axis and between the dopaminergic system and the serotonergic system . Studies have demonstrated that early psychological stress that activates the HPA axis, exacerbates DA depletion and is associated with a decrease in DA synthesis in the brain . Auffret et al. and Leentjens, have shown that symptoms of depression can be improved by administration of DA agonists highlighting the possibility of antidepressant drugs to have an affinity to DA receptors. Since DA depletion may accompany depression, some antidepressant drugs may act on both dopaminergic and serotonergic systems to exert their antidepressant effect . Therefore, DA deficiency resulting from early life stress may in some instances predispose an individual to depression and eventually to neurodegenerative diseases such as PD.
Recommended Reading: What Essential Oils Are Good For Parkinson’s Disease
The Five Environmental Causes Of Parkinsons Disease
Parkinsons disease is a brain disorder that develops and becomes worse over time. The typical symptoms of the disease include tremor, stiffness, slowness of movement, and balance problems. These symptoms develop when the brain lost its ability to produce a sufficient amount of dopamine, a neurotransmitter responsible for controlled body movement.
Researchers have identified a variety of environmental factors that are linked to Parkinsons disease. Some of these factors may directly cause the disease symptoms, others may increase the risk of developing it.
Here are the 5 main environmental factors that are linked to Parkinsons disease development.
What Are The Symptoms Of Parkinsons Disease
Symptoms of Parkinsons disease and the rate of decline vary widely from person to person. The most common symptoms include:
Other symptoms include:
- Speech/vocal changes: Speech may be quick, become slurred or be soft in tone. You may hesitate before speaking. The pitch of your voice may become unchanged .
- Handwriting changes: You handwriting may become smaller and more difficult to read.
- Depression and anxiety.
- Sleeping disturbances including disrupted sleep, acting out your dreams, and restless leg syndrome.
- Pain, lack of interest , fatigue, change in weight, vision changes.
- Low blood pressure.
Don’t Miss: Mild Atrophy Of Brain
Thanks For Signing Up
We are proud to have you as a part of our community. To ensure you receive the latest Parkinsons news, research updates and more, please check your email for a message from us. If you do not see our email, it may be in your spam folder. Just mark as not spam and you should receive our emails as expected.
What Are The Different Stages Of Parkinsons Disease
Each person with Parkinsons disease experiences symptoms in in their own unique way. Not everyone experiences all symptoms of Parkinsons disease. You may not experience symptoms in the same order as others. Some people may have mild symptoms others may have intense symptoms. How quickly symptoms worsen also varies from individual to individual and is difficult to impossible to predict at the outset.
In general, the disease progresses from early stage to mid-stage to mid-late-stage to advanced stage. This is what typically occurs during each of these stages:
Early stage
Early symptoms of Parkinsons disease are usually mild and typically occur slowly and do not interfere with daily activities. Sometimes early symptoms are not easy to detect or you may think early symptoms are simply normal signs of aging. You may have fatigue or a general sense of uneasiness. You may feel a slight tremor or have difficulty standing.
Often, a family member or friend notices some of the subtle signs before you do. They may notice things like body stiffness or lack of normal movement slow or small handwriting, lack of expression in your face, or difficulty getting out of a chair.
Mid stage
Mid-late stage
Standing and walking are becoming more difficult and may require assistance with a walker. You may need full time help to continue to live at home.
Advanced stage
Don’t Miss: 4 Cardinal Signs Of Parkinson’s Disease
How Do I Prevent Falls From Common Hazards
- Floors: Remove all loose wires, cords, and throw rugs. Minimize clutter. Make sure rugs are anchored and smooth. Keep furniture in its usual place.
- Bathroom: Install grab bars and non-skid tape in the tub or shower. Use non-skid bath mats on the floor or install wall-to-wall carpeting.
- Lighting: Make sure halls, stairways, and entrances are well-lit. Install a night light in your bathroom or hallway and staircase. Turn lights on if you get up in the middle of the night. Make sure lamps or light switches are within reach of the bed if you have to get up during the night.
- Kitchen: Install non-skid rubber mats near the sink and stove. Clean spills immediately.
- Stairs: Make sure treads, rails, and rugs are secure. Install a rail on both sides of the stairs. If stairs are a threat, it might be helpful to arrange most of your activities on the lower level to reduce the number of times you must climb the stairs.
- Entrances and doorways: Install metal handles on the walls adjacent to the doorknobs of all doors to make it more secure as you travel through the doorway.
Stress Takes Its Toll In Parkinson’s Disease
- Date:
- Northwestern University
- Summary:
- A stressful lifestyle could lead to the premature death of a group of neurons, whose loss triggers the symptoms of Parkinson’s disease, according to a new study. Isradipine, a drug already approved for human use by the FDA, has been shown in preclinical studies to reduce the stress on these neurons and rejuvenate them. Scientists currently are conducting a clinical trial to find out if isradipine can be used safely and is tolerated by patients with Parkinson’s.
We all know that living a stressful lifestyle can take its toll, making us age faster and making us more susceptible to the cold going around the office.
The same appears to be true of neurons in the brain. According to a new Northwestern Medicine study published Nov. 10 in the journal Nature, dopamine-releasing neurons in a region of the brain called the substantia nigra lead a lifestyle that requires lots of energy, creating stress that could lead to the neurons’ premature death. Their death causes Parkinson’s disease.
The good news is preclinical research shows this stress can be controlled with a drug already approved for human use. By preventing calcium entry, the drug isradipine reduced the mitochondrial stress in dopamine-releasing neurons to the levels seen in neurons not affected by the disease.
Story Source:
Materials provided by Northwestern University. Original written by Marla Paul. Note: Content may be edited for style and length.
Journal Reference:
Cite This Page:
You May Like: Is Parkinson’s Disease Fatal
Environmental Toxins And Parkinsons Disease
Neuronal cell death in PD may also be triggered by exposure to toxic substances or environmental factors which precipitate the symptoms of the disease as they render the brain vulnerable to subsequent physiological chronic stress . The environmental cause of PD mainly refers to exposure to dopaminergic toxins 6-hydroxydopamine , 1-methyl-4-phenyl-1,2,3,6-tetrahydropyridine , paraquat and rotenone as these toxins are known to induce formation of reactive oxygen species and oxidative stress which may result in neuronal cell death .
DA is one of the common neurotransmitters present in most parts of the central nervous system . The mesocortical, mesolimbic, nigrostriatal and tubero-infundibular pathways are the four main pathways that play a key role in dopaminergic signaling . DA cannot cross the blood brain barrier, therefore, it is synthesized from tyrosine which is carried into the brain via amino acid transporters . At the dopaminergic neuron level, tyrosine is then converted into dihydroxyphenylalanine by tyrosine hydroxylase then finally into DA by aromatic L-amino acid decarboxylase . DA is then stored in the vesicle until an action potential allows the vesicle to be discharged into the synapse . Monoamine oxidase is the enzyme that is responsible for breaking down excess DA and is known to similarly act on 6-OHDA inducing oxidative stress resulting in apoptosis .
Do You Need Help With Symptoms And Stress From Parkinsons Disease
Parkinsons disease is a slowly progressing and long-lasting condition that can cause many challenges to those diagnosed and their families. In addition to affecting muscle movement, it can impact mood and cognitive abilities involve pain cause sleep disturbances and other distressing symptoms. While its not curable, much can be done to manage the disease and its symptoms. For example, patients and families can ask for a referral to a palliative care team a medical team that focuses on improving quality of life and relief of symptoms and stress caused by living with serious illnesses.
An Extra Layer of Medical Support for the Long Term
Palliative care is provided by a specially trained team of doctors, nurses and other specialists who work together with a patients other doctors to provide an extra layer of support. It is appropriate at any age and at any stage in a serious illness and can be provided along with treatment geared to the Parkinsons disease . The team will work with you and your family for as long as you want.
When to Consider a Medical Referral to a Palliative Care Team?
The short answer about when to seek a palliative care referral is the sooner the better. Although living with PD is difficult, your burden may be easier with palliative care involved.
Palliative Care Shows Benefits Specific to Those with Parkinsons and Their Caregivers
How to Find Palliative Care
Reminder: Stay Safe from COVID-19
Tags
Read Also: Essential Oils For Parkinson
Oxidative Stress Neuroinflammation And Parkinsons Disease
Oxidative stress is the result of an imbalance between the production of reactive oxygen species and the body capacity to counteract their harmful effects through neutralization by antioxidant defenses . Brain neurons are constantly exposed to reactive oxygen species and reactive nitrogen species as a result of endogenous or exogenous exposure to oxidative stress . Chronic psychological stress increases neuroinflammation which may facilitate nigral cell death in PD . For instance, under stress conditions, there is evidence that dysfunction of inflammatory markers such as tumor necrosis factor -, interleukin -1, IL-6, IL-10, transforming growth factor – in microglia of patients with depression participates in worsening PD symptoms .
PD research is often directed towards the prevention of DA neuron degeneration . However, all current treatments only address the symptomatic effects of the disease, none of which neither halt nor retard DA neuron degeneration . About 95% of PD cases are sporadic hence caused by environmental factors versus 5% that are inherited . The point of view in favor of exposure to stressful events early in life predisposing an individual to develop neurodegenerative disorders later in life seems to emphasize that PD is much more than just a DA-dependent motor deficit.

