Practical Tips For Caregivers Of People With Parkinson’s Psychosis
This 2-page tip sheet has bullet point suggestions for what to do if the person you care for experiences hallucination, delusions or confusion, or becomes agitated or aggressive. In addition, there are tips for how to best be prepared for a doctors appointment when you bring this behavior to the attention of your medical team.
How Can You Tell If Someone Is Hallucinating
Sometimes the person may appear to be hallucinating, but there is another cause . The following tips can help to identify hallucinations:
- Hallucinations differ from misperceptions or misidentifications. Listen to what the person is describing, and check if anything could be causing what they are experiencing. For example, if they describe a swarm of insects, and there is a busy pattern on a carpet, it may be a misperception. By changing or covering the carpet, the misperception may stop.
- If the person seems to be having auditory hallucinations , arrange to have their hearing checked. If the person wears a hearing aid, check that it is working properly at the right setting, and encourage them to wear it. The person may be having problems with their hearing, rather than hallucinating.
- If the person seems to be having gustatory hallucinations , make sure they are getting regular dental check-ups to rule out other causes such as tooth decay or denture cream. For more information see Dental care and oral health.
The Bottom Line On Pd Psychosis
While it can be tricky to balance treating your motor symptoms of Parkinsons disease with treating symptoms like psychosis, working closely with your health care team can help you find the right combination of medications and lifestyle management skills for you. And remember: As with many aspects of this disease, early intervention is best. Psychosis in Parkinsons disease is something that, as providers and family members, important to screen for early on so we can monitor it, says Dr. Pan.
-
Parkinsons Information: National Institute of Health. Parkinsons Disease.
-
Psychosis in Parkinsons Information: The Michael J. Fox Foundation for Parkinsons Research. Ask the MD: Parkinsons Disease Psychosis.
-
Hallucinations and Delusions in Parkinsons: Parkinsons Foundation. Hallucinations/Delusions.
-
2017 Psychosis in Parkinsons Study:Parkinsons Disease. Management of Psychosis in Parkinsons Disease: Emphasizing Clinical Subtypes and Pathophysiological Mechanisms of the Condition.
You May Like: Early Parkinsons Symptoms In Young Adults
Read Also: Does Parkinson’s Affect Memory
What Makes Some People With Parkinsons More Susceptible To Parkinsons Disease Psychosis
Not everyone living with Parkinsons will experience hallucinations and/or delusions, but there are several things that can increase your risk. Here are a few to look out for. Be sure to speak to your doctors and care partners if you notice any changes.
- Increased sleep disturbances such as REM Sleep Behavior Disorder, sleep apnea, vivid dreaming and sleep interruptions
- Vision problems such as blurry or double vision
- Hearing problems
- Medication changes such as new medication, dosage changes and drug interactions
- Disease progression
Visual Integrity And Visual Perceptual Scores
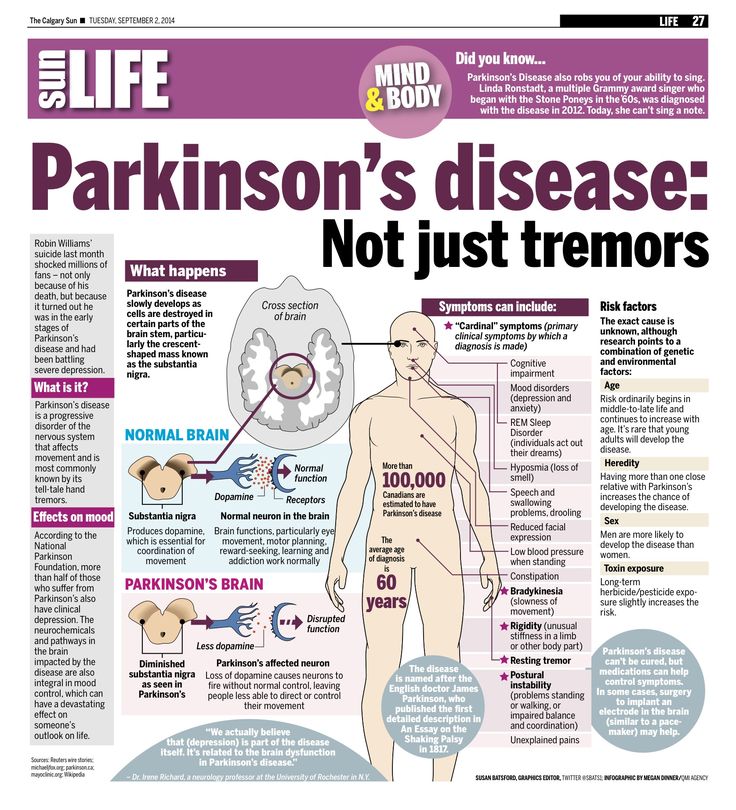
Cataracts were reported by 20% of the recruited participants while 19% of the participants had cataracts removed . Other ophthalmological history reported include glaucoma by two participants , macular degeneration by one participant , and laser treatment .
Visual acuity and perceptual scores are summarized in Table 1. There was a pattern of overall decline in visual integrity within the PDD patients relative to the control group, characterized by a significant reduction in LOGMAR measurements of visual acuity. As expected, PDD-CVH patients showed a characteristic significant increase in the number of false perceptions reported during the pareidolia task compared to PDD-NCVH patients. Interocular latency differences were significantly higher in PDD-CVH compared to the PDD-NCVH group.
You May Like: How Do They Test You For Parkinson’s Disease
How To Treat Parkinsons Psychosis
Parkinsons psychosis can be caused by changes in the brain chemistry caused by Parkinsons disease. But it can also be caused by the medications that treat Parkinsons disease. Because of this, treatment for psychosis will begin with adjustments to the patients current medications to find a combination that improves movement without causing symptoms of psychosis.
If this adjustment in medication doesnt work, an antipsychotic medication may be added.
How To Cope With Parkinsons Psychosis
Caregivers of people with PD and other neurological conditions that cause hallucinations and delusions can engage in a variety of behavioral interventions to keep their loved ones calm and in control during a psychotic event. However, the effectiveness of approaches like redirection and validation therapy depend on the severity and frequency of ones episodes. While these techniques may prove helpful from time to time, Dr. Dewey believes that these efforts are generally unsuccessful over the long term. The best step is to notify your loved ones doctor at the first sign of new or worsening psychotic symptoms to avoid unnecessary injury, stress and even placement in a long-term care facility.
It is important to maintain an honest relationship with your loved one, asking often about any abnormal ideas and experiences they may be having. Family members are usually surprised to learn that their loved one is experiencing these episodes, because many patients with PD are reluctant to divulge this information unless specifically asked.
Remember that not all PD patients will experience severe hallucinations or delusions. If your loved one seems to be doing well, exercise caution when any dosages are changed or medications are added or discontinued. Tweaking a medication regimen should ideally happen one change at a time in order to pinpoint positive and negative effects of a single variable.
Read Also: What Medication Does Michael J Fox Take For Parkinsons
Recommended Reading: Parkinson’s Disease And Hearing Loss
They Mistake Objects For People Or Animals
The most common symptoms of Parkinsons related psychosis are visual illusions and hallucinations, says Dr. Barrett. These can start out mild, with the person looking at an object but seeing something else. For example, they might mistake a lamp for a human or think the mailbox is a deer. These are early, minor hallucinations that may evolve to be more bothersome or pervasive, says Barrett.
Search Strategy And Selection Criteria
Suitable studies for this review were identified by searches of MEDLINE until January 2010 using the following terms:
Parkinsons disease or parkinsonism or parkinsonian
Psychosis or drug-induced psychosis or hallucinations or delusions
The key term quetiapine was cross referenced with the results of . The reference lists of all trial reports were examined. Only papers published in English were reviewed.
Read Also: Vascular Parkinsonism And Cognitive Impairment
Read Also: How Prevalent Is Parkinson’s Disease In The Population
Causes Of Resting Tremors In Parkinsons Disease
Resting tremors are among the most noticeable features of Parkinsons disease . The tremors are believed to be caused by complex interactions between a number of factors. Alterations in the activity of several areas of the brain including the substantia nigra, the basal ganglia, and the thalamus, as well as changes in the level and action of the neurotransmitter dopamine, are all related to each other and to the production of the tremors.
You May Like: Music Therapy For Parkinsons
Network Changes And Thalamic Drivers
Visual hallucinations have fascinated neurologists and neuroscientists for many years, with their tantalisingly rich and often narrative detail. Due to their transient nature, they have been challenging to investigate, with no clear mechanism found, but many theories have been proposed. Previous models for visual hallucinations considered them as cortical release phenomena, where spontaneous activity occurs in the absence of visual stimuli. Alternative models suggested that hallucinations arise due to incorrect binding of objects into visual scenes.
Advances in computational modelling and network neuroscience have opened up approaches to understanding the brain in new ways. Recent models suggest that Parkinsons hallucinations could arise due to a shift in dominance of difference networks. Specifically, there is thought to be a breakdown in those networks directed to attention and perception, and overactivity of the default mode network ,, a large-scale network that becomes activated during rest, and in day dreaming and mind-wandering. Indeed abnormal levels of default mode network activation are seen in patients with Parkinsons hallucinations.
Adapted from Zarkali A, Adams RA, Psarras S, Leyland LA, Rees G, Weil RS. Increased weighting on prior knowledge in Lewy body-associated visual hallucinations. Brain Commun. 2019 1:fcz007. doi:10.1093/braincomms/fcz007
Also Check: Parkinsons Staring Into Space
Don’t Miss: Does Gabapentin Help Parkinson’s
What Causes Parkinsons Disease Psychosis
Parkinsons is a brain disorder associated with a loss of dopamine-producing nerve cells deep inside the brain. Dopamine is a neurotransmitter that helps regulate the bodys movement, and it also allows us to think clearly and regulate our emotions. When you try to replace the dopamine thats been lost in a person with Parkinsons, it can cause the system to get out of whack which can impact thinking, how visual things are processed and more. Parkinsons disease psychosis is therefore typically a side effect of the disease itself or the medications used to manage it.
As a result, its an ongoing balancing act for Parkinsons doctors to prescribe enough dopamine to control a person with Parkinsons motor symptoms, but not so much that the person experiences hallucinations and/or delusions.
They Hear Noises Or Voices That Arent There

People with Parkinsons related psychosis commonly report hearing footsteps, a shutting door, or creaking in the house that others dont hear, says Barrett. These auditory hallucinations are less common than visual hallucinations, but sometimes they occur in tandem, especially in those with more severe psychosis.
Also Check: Botox Salivary Glands Parkinson’s
Memory Problems And Dementia
Research shows that hallucinations and delusions often happen when someone with Parkinsons also has problems with memory, thinking problems or dementia.
If you experience hallucinations at an early stage of Parkinsons, it could be a sign of another medical condition, such as dementia with Lewy bodies.
Parkinsons Disease Psychosis: Hallucinations Delusions And Paranoia
As part of Parkinsons Disease and its treatment, hallucinations, illusions, delusions, suspiciousness and paranoid behaviors occur in over 50% of patients. In this 1-hour webinar Dr. Christopher Goetz suggests lifestyle changes, medication adjustments and a recently FDA approved drug to specifically treat psychosis in Parkinsons Disease.
Read Also: Prayer For Parkinsons Disease
Also Check: In Home Care For Parkinson’s Patients
Hallucinations And Delusions In Pd
Hallucinations and delusions are collectively referred to as psychosis.
Visual hallucinations are the most common type of hallucination. In a visual hallucination, someone sees things that are not actually there. There can also be auditory and olfactory hallucinations. Often hallucinations are not alarming to the person experiencing them.
Delusions are when there is an alternative view of reality: an entire irrational story is created. Paranoia is a common type of delusion. Capgras delusions are a specific type of delusion where the person believes that a spouse, adult child, or other family member has been replaced by an imposter.
Also Check: How To Control Parkinsons Tremors
How Is Parkinsons Disease Dementia Diagnosed
No single test can diagnose Parkinsons disease dementia. Instead, doctors rely on a series or combination of tests and indicators.
Your neurologist will likely diagnose you with Parkinsons and then track your progression. They may monitor you for signs of dementia. As you get older, your risk for Parkinsons dementia increases.
Your doctor is more likely to conduct regular testing to monitor your cognitive functions, memory recall, and mental health.
Recommended Reading: Va Parkinson’s Disability Rating
Get The Every Victory Counts Manual For Care Partners
Do you have the Every Victory CountsManual for Care Partners! Released in 2021, this resource is available at no cost in print and digital versions. To learn more and request your copy, .
This content was supported in part by Acadia Pharmaceuticals. To learn more about Parkinsons disease psychosis, visit moretoparkinsons.com
Pathology Of Neurotransmitter Pathways In Pd Psychosis And Relevance Of Medications
The distribution of pathology in PD involves key components of dopaminergic and other important neurotransmitter pathways implicated in PD psychosis. Dopamine is synthesized in the substantia nigra, with projections to the striatum, limbic system and frontal lobe , and five recognized dopamine receptors with broad distribution throughout the brain and peripheries at varying levels of expression . It is known that dopaminergic medications have differential actions across these receptors, and, similarly, antipsychotic medications display different binding affinities for individual dopamine receptors .
While loss of dopaminergic neurons within the substantia nigra is a central pathological feature of PD , neuronal loss also occurs in multiple other subcortical nuclei with projections to cortical, limbic, and basal ganglia regions. These include the dopaminergic nuclei of the ventral tegmentum, noradrenergic locus coeruleus, serotonergic raphe nuclei, histaminergic tuberomammillary nucleus of the hypothalamus, and cholinergic nucleus basalis of Meynert and the pedunculopontine nucleus . LB deposition and neuronal loss in the locus coeruleus occurs earlier and is more prominent than PD pathology in the substantia nigra, with some evidence that pathology in this region may contribute to subsequent dopaminergic cell loss, because noradrenergic neurons directly innervate the substantia nigra .
Don’t Miss: Physical Therapy For Parkinson’s Patients
Showing Up As Your Best Self
Caring for someone with a progressive condition like Parkinsons disease can be challenging. Hallucinations only add to the stress of caregiving, especially if the person youre caring for doesnt have insight into what theyre experiencing.
The more you understand about your loved ones condition, the easier itll be to care for them. Talk to their doctor and read up on Parkinsons disease so youre better equipped to respond when hallucinations occur.
Dont forget to take care of yourself as well. Take regular breaks from caregiving to relax and do the things you enjoy. By tending to your own needs, youll have more energy to devote to your loved one.
Similar Articles Being Viewed By Others
Carousel with three slides shown at a time. Use the Previous and Next buttons to navigate three slides at a time, or the slide dot buttons at the end to jump three slides at a time.
09 September 2021
Ning-Ning Che, Qiu-Huan Jiang, Hong-Qi Yang
15 June 2022
Yael Lustig-Barzelay, Ifat Sher, Ygal Rotenstreich
volume 10, Article number: 21110
You May Like: Crafts For Parkinsons Patients
Read Also: Parkinson’s And Dental Extraction
The Cause Of Parkinsons Delusions And Hallucinations
Some risk factors associated with the development of psychosis in Parkinsons disease include:
- Age: Parkinsons disease usually occurs in people over age 60.
- Duration and severity of Parkinsons disease: Psychosis is more common in advanced or late-stage Parkinsons disease.
- Later onset: Occurring later in life
- Hyposmia: A decreased sense of smell
- Cognitive impairment: Problems with thinking, including trouble remembering, difficulty learning new things, difficulty concentrating, problems making decisions that affect everyday life
- Depression: People who have both depression and Parkinsons disease are at a greater risk of developing psychosis.
- Diurnal somnolence: Daytime sleepiness
- REM sleep behavior disorder: A sleep disorder in which you physically act out dreams involves making vocal sounds and sudden, often extreme, arm and leg movements during REM sleep
- Visual disorders: Impaired vision
- Severe axial impairment: Speech, swallowing, balance, freezing of gait
- Autonomic dysfunction: Impairment of the autonomic nervous system , which controls involuntary or unconscious actions such as heart rate, breathing, body temperature, blood pressure, digestion, and sexual function
- High medical comorbidity: The existence of more than one condition or illness in the same person at the same time with Parkinsons disease, may include conditions such as dementia, depression, and sleep disorders
Risk Factors And Conceptual Models For Visual Hallucinations In Pd
Several disease-related and other factors have been linked to visual hallucinations in PD. The presence of visual hallucinations is associated with the duration of PD , older age, disease severity, and the presence of motor fluctuations . Other established risk factors include female sex , visual impairment , cognitive impairment , REM sleep behavior disorder , autonomic dysfunction , depression , apathy , and anxiety . A bidirectional association between visual hallucinations and cognitive impairment has been observed in PD, with the presence of minor visual hallucinations often preceding any significant cognitive decline and visual hallucinations representing a risk factor for later development of PD dementia .
Studies of the etiological basis of visual hallucinations in PD psychosis have focused on both the role of individual risk factors and the interrelationships between multiple factors. Explanatory models have emphasized dysfunction of components of attentional and perceptual processing or dream imagery intrusion with dopaminergic and other medications as likely playing a modulating role .
Dysfunctional attentional network interactions have also been demonstrated in DLB , which may be associated with the generation of visual hallucinations . In addition, thalamo-cortical dysfunction, with decoupling between thalamic nuclei and the DMN, has been proposed to underly psychosis in DLB and PD .
Don’t Miss: What Does Parkinson’s Disease Look Like
What Should I Do Once The Hallucination Passes
After the hallucination passes, you can try to talk through the experience together. If the person has insight, it may be easier for them to understand and talk about what just happened.
Write down what happened during the hallucination. Note the time of day and what the person was doing when it started.
Taking notes each time it happens can help you identify the triggers. It could be related to the timing of medication, and your loved one might feel a sense of relief and control in knowing that pattern.
Ask what you can do to stop it from happening again. This might include adjusting their medication dosage or adding an atypical antipsychotic drug to their medication regimen.
Sleep Problems At Later Stages Of Pd
In addition to the conditions already mentioned, during the later stages of PD, you also may experience sleep problems related to higher doses of medications, such as hallucinations.
As many as 33% of Parkinsonâs patients during mid and later stages of the disorder experience hallucinations, related to medication side effects. Hallucinations tend to occur visually rather than hearing them . They are frequently associated with vivid dreams.
- Cartwright, R. . Dreaming as a mood regulation system. In: Principles and Practice of Sleep medicine. 4th edition, pps 565-572.
- Kumar, S., Bhatia, M., & Behari, M. . Sleep disorders in Parkinsonâs disease. Mov Disord, 17, 775-781.
- Larsen, J. P., & Tandberg, E. . Sleep disorders in patients with Parkinsonâs disease: epidemiology and management. CNS Drugs, 15, 267-275.
- Olson, E. J., Boeve, B. F., & Silber, M. H. . Rapid eye movement sleep behaviour disorder: demographic, clinical and laboratory findings in 93 cases. Brain, 123 , 331-339.
- Pappert, E. J., Goetz, C. G., Niederman, F. G., Raman, R., & Leurgans, S. . Hallucinations, sleep fragmentation, and altered dream phenomena in Parkinsonâs disease. Mov Disord, 14, 117-121.
- Stacy, M. . Sleep disorders in Parkinsonâs disease: epidemiology and management. Drugs Aging, 19, 733-739.
Recommended Reading: Strange Behavior With Parkinson’s
