What If You Have Parkinson’s Disease And A Stroke
Stroke is relatively common and so is Parkinson’s disease, so one person can have both. If you or your loved one has a stroke as well as Parkinson’s disease, it is normal for you to be concerned.
The conditions have different causes, but the movement problems of Parkinson’s disease combined with the effects of a stroke can make it even more difficult for you or your loved one to get around than if you only had one of the two problems.
If you have both conditions, it is more important to pay attention to things such as safeguarding your home to prevent falls and getting a walker or a cane in order to avoid falls.
Drug Therapy And Research
If the disease progresses beyond minor symptoms, drug treatment may be indicated. Drug therapy for Parkinsonâs typically provides relief for 10â15 years or more. The most commonly prescribed medication is L-dopa , and this helps replenish some of the depleted dopamine in the brain. Sinemet, a combination of levodopa and carbidopa, is the drug most doctors use to treat Parkinsonâs disease. Recent clinical studies have suggested, in the younger person, the class of drugs called âdopamine agonistsâ should be used prior to levodopa-carpidopa except in patients with cognitive problems or hallucinations. In those older than 75, dopamine agonists should be used cautiously because of an added risk of hallucinations.
Other drugs are also used, and new drugs are continually being tested. It is common for multiple drugs to be prescribed because many of them work well together to control symptoms and reduce side effects. Contrary to past beliefs, starting Sinemet in newly diagnosed people does not lead to early symptoms of dyskinesia . Current knowledge is that the disease progression causes dyskinesias, not a âresistanceâ to the drug.
Quality of life studies show that early treatment with dopaminergic medications improves daily functioning, prevents falls, and improves a personâs sense of well-being.
Maintaining Your Normal Pd Medication Schedule
Maintaining your PD medication schedule is crucial for anyone with PD. The correct timing and dosage are essential to your comfort and well-being. However, oftentimes when undergoing surgery, there may be restrictions regarding when you can and cannot take medications. Here are a few tips to navigate this issue:
Recommended Reading: Parkinson’s Disease Autoimmune
What Are The Signs And Symptoms Of Parkinson’s Disease Dementia
Parkinson’s disease dementia can’t be diagnosed conclusively by a single test. Instead, doctors may use multiple tests and consider a range of Parkinson’s disease dementia criteria, including symptoms like:
- Feelings of disorientation or confusion
- Agitation or irritability
RELATED: 7 Warning Signs of Dementia to Look For in Loved Ones
Not all cases of cognitive impairment are severesome people with Parkinson’s disease can still manage their work and personal life just fine. But once a person has Parkinson’s disease dementia, it usually means that they can no longer go about their daily life as they once did.
Stages Of Parkinsons Disease
Because Parkinsons disease develops over time, there are various stages that help identify how symptoms have progressed and what should be expected next.
Generally, doctors follow a set of five stages as outlined below:
Stage 1
The beginning stage of Parkinsons disease sometimes doesnt show any signs at all. If symptoms are noticeable, theyre usually tremors and affect one side of the body. The symptoms usually dont affect your daily routine, but they should be taken seriously and brought to the attention of your doctor, if they havent already.
Stage 2
During this stage, the disease starts to affect your whole body. The tremors and stiffness cause routine activities to take a little longer to complete, and your overall movement starts to be affected. Your posture and facial expressions may should start to change, which can impact your ability to walk at a normal pace or communicate like you used to.
Stage 3
This stage features a worsening of all the symptoms that started to progressively deteriorate in stage 2, but you also start to experience a loss of balance and coordination, as well as how quick your reflexes are. As these symptoms start to come into the fold, people with the disease start to fall more, which can cause their own injuries and debilitations. Activities like getting out of bed, eating, and getting dressed start to get more difficult.
Stage 4
Stage 5
Read Also: Is Parkinson’s Disease Fatal
Surgery For People With Parkinsons Disease
Deep brain stimulation surgery is an option to treat Parkinsons disease symptoms, but it is not suitable for everyone. There are strict criteria and guidelines on who can be a candidate for surgery, and this is something that only your doctor and you can decide. Surgery may be considered early or late in the progression of Parkinsons. When performing deep-brain stimulation surgery, the surgeon places an electrode in the part of the brain most effected by Parkinsons disease. Electrical impulses are introduced to the brain, which has the effect of normalising the brains electrical activity reducing the symptoms of Parkinsons disease. The electrical impulse is introduced using a pacemaker-like device called a stimulator. Thalamotomy and pallidotomy are operations where the surgeon makes an incision on part of the brain. These surgeries aim to alleviate some forms of tremor or unusual movement, but they are rarely performed now.
How Is Parkinson Disease Treated
Parkinson disease can’t be cured. But there are different therapies that can help control symptoms. Many of the medicines used to treat Parkinson disease help to offset the loss of the chemical dopamine in the brain. Most of these medicines help manage symptoms quite successfully.
A procedure called deep brain stimulation may also be used to treat Parkinson disease. It sends electrical impulses into the brain to help control tremors and twitching movements. Some people may need surgery to manage Parkinson disease symptoms. Surgery may involve destroying small areas of brain tissue responsible for the symptoms. However, these surgeries are rarely done since deep brain stimulation is now available.
Read Also: What Are The Four Cardinal Signs Of Parkinson’s Disease
What Is The Outlook For Persons With Parkinsons Disease
Although there is no cure or absolute evidence of ways to prevent Parkinsons disease, scientists are working hard to learn more about the disease and find innovative ways to better manage it, prevent it from progressing and ultimately curing it.
Currently, you and your healthcare teams efforts are focused on medical management of your symptoms along with general health and lifestyle improvement recommendations . By identifying individual symptoms and adjusting the course of action based on changes in symptoms, most people with Parkinsons disease can live fulfilling lives.
The future is hopeful. Some of the research underway includes:
- Using stem cells to produce new neurons, which would produce dopamine.
- Producing a dopamine-producing enzyme that is delivered to a gene in the brain that controls movement.
- Using a naturally occurring human protein glial cell-line derived neurotrophic factor, GDNF to protect dopamine-releasing nerve cells.
Many other investigations are underway too. Much has been learned, much progress has been made and additional discoveries are likely to come.
Executive Dysfunction In Parkinsons
Executive functions in cognition are higher-order mental processes, including the ability to plan, organize, initiate and regulate behavior to meet goals. Executive functioning is present in activities such as multitasking, switching tasks, and solving problems. The prefrontal cortex of the brain and the dopamine system are responsible for executive function. As PD damages these areas, executive dysfunction occurs, and executive dysfunction is one of the most common cognitive impairments found in people with PD.3,4
Don’t Miss: Can Parkinson’s Cause Hip Pain
Related Diagnosis: Lewy Body Dementia
Current research is helping to differentiate dementia related conditions in relationship to Parkinsonâs disease. Doctorâs use a 12-month arbitrary rule to aid in diagnosis. When dementia is present before or within 1 year of Parkinsonâs motor symptoms developing, an individual is diagnosed with DLB. Those who have an existing diagnosis of Parkinsonâs for more than a year, and later develop dementia, are diagnosed with PDD.
In the simplest terms, Lewy bodies are abnormal clumps of proteins that develop in nerve cells. Cholinesterase inhibitors, medications originally developed for Alzheimerâs disease, are the standard treatment today for cognitive DLB and PDD symptoms. Early diagnosis is important, as DLB patients may respond differently than Alzheimerâs disease patients to certain drug, behavioral, and dementia care treatments.
This challenging, multi-system disorder involving movement, cognition, behavior, sleep, and autonomic function requires a comprehensive treatment approach to maximize the quality of life for both the care recipient and their caregiver. It is very important to pay attention to symptoms of dementia and to search for an expert clinician who can diagnose the condition accurately.
Anesthetic Management For Steriotactic Pallidotomy/thalamotomy
Classically local anesthesia with minimal or no sedation has been used for patients undergoing stereotactic procedures. This allows for patient participation in target localization and immediate observation of effects of test and lesion. Antiparkinsonian mediations are withheld for 1224 h prior to surgery. Therapy for concurrent diseases must be continued till the day of surgery.
Under LA, in magnetic resonance imaging suite stereotactic frame applied. Extra padding and rolls can make the patient more comfortable. Also these patients are very motivated to co-operate, unless there is dementia present. LA again is used to do burr hole and if the patient becomes agitated, midazolam can be titrated to desired effect. It is important that level of sedation does not impair co-operation or interfere with communication between surgeon and patient. Age, varying levels of dementia, fatigue, and cumulative effects of medication make it necessary to titrate the drugs slowly. Since propofol may elicit abnormal movements and may at times improve parkinsonian tremor, it might not be ideally suited for patients with movement disorders undergoing functional stereotactic neurosurgery.
Recommended Reading: What Is The Life Expectancy Of Someone With Parkinson’s Disease
Symptoms And Signs Of Parkinsons Disease
Its difficult to directly diagnose Parkinsons disease. There is no specific test doctors can perform to confirm a diagnosis, which is why its important for research to continue to identify the ever-evolving definition of Parkinsons. In addition to pinpointing many of these symptoms, doctors will also delve through family history and perform an overall examination of the brain to officially diagnose someone.
The rate at which these symptoms onset varies per person, and theres no specific amount of time youre guaranteed to lived once diagnosed. It can develop quickly or you can live 30 years before the worst of the disease starts to show. While Parkinson himself identified six main qualities of the disease when he first detailed it, the symptoms of Parkinsons have developed over time. They include, but arent completely limited to, the following:
Who Gets Parkinson’s Disease

About 1 million people in the United States have Parkinson’s disease, and both men and women can get it. Symptoms usually appear when someone is older than 50 and it becomes more common as people get older.
Many people wonder if you’re more likely to get Parkinson’s disease if you have a relative who has it. Although the role that heredity plays isn’t completely understood, we do know that if a close relative like a parent, brother, or sister has Parkinson’s, there is a greater chance of developing the disease. But Parkinson’s disease is not contagious. You can’t get it by simply being around someone who has it.
You May Like: Sam Waterston Stroke
How Do I Know If I Have A Speech Or Voice Problem
- My voice makes it difficult for people to hear me.
- People have difficulty understanding me in a noisy room.
- My voice issues limit my personal and social life.
- I feel left out of conversations because of my voice.
- My voice problem causes me to lose income.
- I have to strain to produce voice.
- My voice clarity is unpredictable.
- My voice problem upsets me.
- My voice makes me feel handicapped.
- People ask, “What’s wrong with your voice?”
Who Gets Parkinsons Disease
Estimates vary, but about 1 million people are living with Parkinsons disease in the U.S. Doctors diagnose about 60,000 cases a year, most in people over age 60. Younger people can also get Parkinsons. About 5-10% of patients have young-onset Parkinsons disease, diagnosed before age 50.
About 15% of patients have Parkinsons-plus syndromes, also known as atypical Parkinsons. Medications may be less effective for these syndromes, which can lead to disability sooner.
Risk factors for Parkinsons disease include:
- Age: Risk increases with age. Average age at diagnosis is 65.
- Gender: Men are at higher risk.
- Environmental exposure: Lifetime exposure to well water, which may contain pesticide runoff, can increase risk. So can exposure to air particles containing heavy metals, such as in industrial areas.
- Family history: Having a close relative with the disease could increase your risk. Researchers have identified a dozen genes that may be linked to Parkinsons disease.
- Sleep disorder: People who act out their dreams are up to 12 times more likely to develop Parkinsons disease. Its not clear whether this condition, called REM sleep behavior disorder or RBD, is a cause or symptom of Parkinsons disease.
- Head trauma: Traumatic brain injury increases risk of Parkinsons, even years later.
Don’t Miss: What Color Is The Ribbon For Parkinson’s
History Of Parkinsons Disease
Symptoms and possible treatments for Parkinsons were discussed in texts related to Ayurveda, an ancient Indian medical practice thats been around since as early as 5,000 B.C. A Parkinsons-like condition was also mentioned in the first Chinese medical text, Huang Di Nei Jing Su Wen, more than 2,500 years ago.
Parkinsons disease was formally recognized in an 1817 paper, An Essay on the Shaking Palsy, by James Parkinson, MD, a London doctor and member of the Royal College of Surgeons.
Dr. Parkinson observed what are now known as the classic symptoms of Parkinsons disease, including tremors, rigidity, and postural instability. He theorized that the disease developed because of a problem in the brains medulla region.
Parkinsons essay received little attention until 1861, when French neurologist Jean-Martin Charcot and his colleagues distinguished the disease from other neurological conditions and termed it Parkinsons disease.
What Is Parkinsons Disease Symptoms Causes Diagnosis Treatment And Prevention
The causes and symptoms of Parkinsons disease can vary from person to person. While there is no cure, there are medications and treatments to help manage the condition.
Parkinsons disease is a movement disorder that happens when nerve cells in a certain part of the brain are no longer making the chemical dopamine.
The condition is also sometimes known as paralysis agitans or shaking palsy.
The Parkinsons Foundation estimates that 60,000 Americans are diagnosed with Parkinsons every year. However, the true number of people who develop the disease may be much higher.
Recommended Reading: Is Parkinsons Disease Fatal
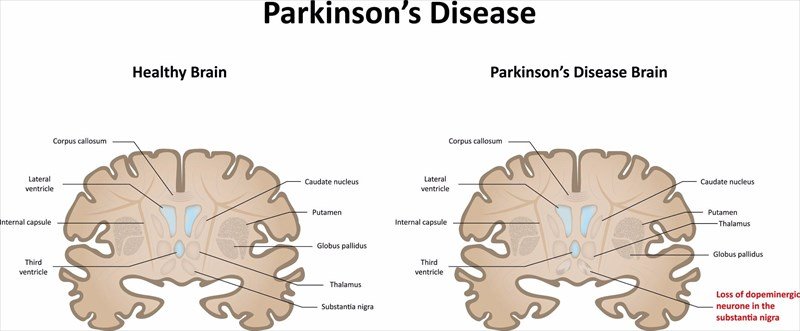
What Does Parkinson’s Do To The Brain
Deep down in your brain, there’s an area called the substantia nigra, which is in the basal ganglia. Some of its cells make dopamine, a chemical that carries messages around your brain. When you need to scratch an itch or kick a ball, dopamine quickly carries a message to the nerve cell that controls that movement.
When that system is working well, your body moves smoothly and evenly. But when you have Parkinson’s, the cells of your substantia nigra start to die. There’s no replacing them, so your dopamine levels drop and you can’t fire off as many messages to control smooth body movements.
Early on, you won’t notice anything different. But as more and more cells die, you reach a tipping point where you start to have symptoms.
That may not be until 80% of the cells are gone, which is why you can have Parkinson’s for quite a while before you realize it.
Understanding The Neurologic Control Of The Cardiac System
Before we explore this issue, lets first learn a bit about the autonomic nervous system and about the cardiac systems place within it. The ANS is part of the peripheral nervous system, a network of nerves throughout the body. The ANS exerts control over functions that are not under conscious direction such as respiration, heart function, blood pressure, digestion, urination, sexual function, pupillary response, and much more. The ANS is further subdivided into the parasympathetic nervous system and the sympathetic nervous system. Both the parasympathetic and sympathetic nervous systems regulate most major organs. Often, they have opposite effects, with the sympathetic nervous system activating a system and the parasympathetic system calming it down.
One of the systems controlled by the ANS is cardiac regulation. Blood pressure sensors, known as baroreceptors, reside in the heart as well as in the carotid artery, the major artery in the neck. If the baroreceptors sense a change in the blood pressure, a signal is sent to particular areas in the brain. From there, the autonomic nervous system sends signals to the heart to control heart rate and cardiac output. Signals are also sent to the blood vessels to change the size of their diameter, thereby regulating blood pressure.
You May Like: Is Parkinson’s Disease Fatal
Learn More About Parkinsons Disease
Parkinsons Disease: The Essentials
If youre new to Parkinsons disease and would like a good overview to help you better understand the disease, please view our Parkinsons Disease: The Essentials presentation. Its a great place to get started with reliable and concise information.
Causes
The exact cause of Parkinsons is still unknown, but there is an enormous amount of research being done to learn more. This research has led scientists to formulate a number of theories on the cause of this disease.
Diagnosing
While there is no definitive test that can be taken to determine whether a person has Parkinsons disease, movement disorder specialists look for symptoms and use brain imaging technology to accurately diagnose Parkinsons.
Symptoms
Even though Parkinsons is classified as a movement disorderand its motor symptoms are the most discussed and well-knownthere are many non-motor symptoms that display in people with Parkinsons as well.
Treatments
As of today, there is no cure for Parkinsons disease. But there are many ways in which the disease can be treated to make symptoms more manageable.
