What Is Parkinson’s Disease
Parkinson’s disease is a disorder that affects the nervous system and movement.2,3 The symptoms typically begin gradually, and it may take a while for patients to notice them. These symptoms may include tremors, slow movement, rigid muscles as well as speech and writing changes. Patients may also experience impaired posture and balance or loss of automatic movements, such as blinking, smiling or swinging their arms.
Parkinson’s has a variety of risk factors that should be considered. In many cases, Parkinson’s usually affects people who are 50 years of age or older.2,3 However, some patients may experience young onset Parkinson’s disease, also called early-onset Parkinson’s disease, which affects roughly 2-10% of the population with Parkinson’s in the United States.3 Men may be more likely to develop Parkinson’s disease than women.2 If a close relative has Parkinson’s disease, a patient may be more likely to develop the disorder. The risk may still be small unless there are a large number of relatives with Parkinson’s disease. Finally, long-term exposure to herbicides and pesticides may slightly increase a patient’s risk.2
Once the disease has begun to progress, there are five stages that patients may experience.
Insight In Brain Activation Studies For Motor Functions
This is an overview of brain activation studies which describes findings that help in our understanding of the pathophysiology of motor, cognitive, and behavioral symptoms seen in Parkinsons disease PD and the underlying neuronal changes. Activation studies of PD patients have been utilized to see the basal-ganglia-thalamocortical circuit function. Several types of motor tasks have been used in conjunction with different neuroimaging techniques to study the motor circuit in PD.
Most common tests included the repetitive tasks, involving either of these two, one was repeated thumb to other finger opposition movements second was manipulation of a joystick in different directions. When normal subjects did repetitive right-hand joystick movements in different directions while they underwent H2O PET, an increase in regional cerebral blood flow was noted in the contralateral primary sensorimotor cortex and lentiform nucleus. Activation was also noted in the bilateral anterior cingulate gyrus, supplementary motor area , lateral premotor cortex, and dorsolateral prefrontal cortex. Opposite to that, PD patients showed a more complex activation pattern, which showed impaired rCBF changes in the lentiform nucleus, anterior cingulate gyrus, SMA, and dorsolateral prefrontal cortex. However normal activation was seen at the level of sensorimotor cortex, lateral, and parietal premotor cortex when compared with healthy controls .
When Brain Mri Is Recommended To Help Diagnose Parkinsonism
Differentiating atypical parkinsonism from Parkinsons disease can be a challenge in patients presenting with symptoms in early disease stages. A diagnosis cannot be made from a brain magnetic resonance imaging scan, but brain MRI can be of added value when there is uncertainty about the clinical diagnosis.
The appropriateness of and the added diagnostic value of a brain MRI scan in the work-up of parkinsonism is described in a newly published article in the Journal of Parkinsons Disease. Lead author Frederick J.A. Meijer, MD, PhD, a neuroradiologist in the department of radiology and nuclear medicine at Radboud University Medical Center in Nijmegen, The Netherlands, offers advice on the scanning protocol to use, and also discusses its diagnostic value with respect to specific abnormalities that can be seen.
The authors of the article, who also include neurologists from the Radboud University Medical Center and Donders Institute for Brain, Cognition and Behavior, conducted a 3-year long prospective study on the contribution of routine brain MRI to the differential diagnosis of parkinsonism.1 Based on this research, the authors refuted clinical guidelines recommending standard use of cerebral MRI for all patients presenting with parkinsonism.;
3T brain MRI including DTI tractography in a patient presenting with parkinsonism.
Recommended Reading: Is Parkinson’s Dominant Or Recessive
Mri In Parkinsons Testing
One of the more common tests done during a neurologic workup is an MRI scan and one may think that in the investigation of a disease that affects the brain such as Parkinsons, this imaging test would be a necessity. In the context of Parkinsons disease, however, an MRI is not particularly helpful. It looks at the structure of the brain which, for all intents and purposes, appears normal in this disease. An MRI may, however, be indicated when symptoms appear in younger people or if the clinical picture or the progression of symptoms is not typical for Parkinsons. In these situations, MRI can be used to rule out other disorders such asstroke, tumors,hydrocephalus, and Wilsons Disease .
Other Tremor Diagnostic Tools
In addition to using the Archimedes spiral test, doctors might also use other diagnostic and performance evaluations. For example, your physician might ask you to drink from a glass, walk, eat from a spoon, or hold your arms outstretched.
Here are the types of exams you can expect beyond writing tests:
Don’t Miss: Parkinsons And Eyesight
What Is Parkinson’s And How Can Mri Help
More than ten million people are living with Parkinson’s disease worldwide, with about one million cases expected to be in the United States by 2020.1 This is more than the number of people with multiple sclerosis, muscular dystrophy and Lou Gehrig’s disease combined.1 With the rising prevalence of Parkinson’s disease, its important to understand the signs and symptoms of the disease. Likewise, physicians and radiology departments may need to know what role magnetic resonance imaging may play.
Resting State Functional Mri
Resting state fMRI detects blood-oxygen-level-dependent low-frequency spontaneous fluctuations across the brain while an individual is at rest, and can be used to study functional connectivity within and across spatially distributed brain networks. The most validated analytical approach examines the resting state fMRI Parkinsons Disease Related Pattern , which was initially characterized using PET . Similar to PET, there are significant increases in fPDRP expression in PD relative to control subjects , however, further research is necessary to evaluate its utility as a diagnostic and monitoring biomarker. At this time, there are numerous additional analytical approaches taken to examine rs-fMRI in PD, that suggest widespread dysfunction in PD, but also numerous inconsistencies based on recent reviews . This is partially related to the impact of various preprocessing approaches and observations showing rs-fMRI varies as a function of medication status . Further, networks appear to dynamically adapt to disease progression and functional brain circuitry dysfunction may differ dependent on the nature of the motor symptoms . Indeed, investigation of more targeted analytic approaches will be necessary to identify potential diagnostic and monitoring biomarkers, which is discussed further in the next section.
You May Like: How Did Michael J Fox Get Parkinson’s
What Are The Treatments
Currently there is no cure for Parkinsons disease.
Symptoms can be mild in the early stages of the condition and people might not need immediate treatment. Your doctor and specialist will monitor your situation.
There are several different types of drugs used to treat Parkinsons disease. Drug treatments are tailored to each individuals needs and are likely to involve a combination of different drugs. Your medication should be reviewed regularly. It is likely that, over time, changes will be made to the types of drugs you take and the doses you take each day.
The main types of drug treatment for Parkinsons disease are:
- drugs which replace dopamine
- drugs which mimic the role of dopamine
- drugs which inhibit the activity of acetylcholine
- drugs which prevent the body breaking down dopamine
- other drugs such as anti-sickness medication
Everybody is affected differently by medication. The possible side effects of Parkinsons disease drugs include nausea , vomiting , tiredness and dizziness. Some people might experience confusion, nightmares and hallucinations. For some people, dopamine agonists have been linked to compulsive behaviour such as addictive gambling or hypersexuality .
The effectiveness of the main drug treatment levodopa can wear off over time and its long-term use can cause some people to develop involuntary twisting or writhing movements of the arms, legs or face . To reduce the risk, doctors might delay the use of levodopa for younger people.
Neuroimaging In Parkinsons Disease
Over the past decades, neuroimaging studies which include structural, functional and molecular modalitieshave provided priceless understandings about the Parkinson disease . Although PD is very complex, no neuroimaging modalities are specifically recommended for routine use in clinical practice. However, conventional MRI and dopamine transporter imaging are used as adjuvant apparatuses in the differential diagnosis between PD and other causes of Parkinsonism. Single-photon emission CT and PET are equally effective at differentiating between degenerative and nondegenerative causes of parkinsonism; MRI and PET can differentiate between PD and atypical parkinsonism, but need sophisticated enhancement methods . Dopaminergic and serotonergic PET can be used to monitor PD progression, motor and nonmotor symptoms, and complications, whereas cholinergic PET is currently the most sensitive approach for assessing PD dementia. PET and other neuroimaging techniques should have a primary role in the development of protocols for new clinical trials, particularly those investigating cell therapy. Hybrid PET-MRI technology could offer a revolution in PD imaging .
Also Check: Do People Die From Parkinson’s Disease
An Overview Of The Current Clinical Evidence For Morphological Changes In The Brain Associated With Symptoms And Potential Associated Neural Mechanisms
Parkinsons disease is characteristically shown to have motor symptoms including resting tremor, rigidity, and bradykinesia but cognitive and behavioral problems in PD are more common and they have a direct effect on the quality of life.
The estimated prevalence of dementia in patients with PD ranges between 24 and 31% has conservatively been estimated to range between 24 and 31%. Cognitive function in PD patients with dementia is significantly different than that of the cortical dementia of Alzheimers disease . Patients with PDD often exhibit difficulties with executive functions, the retrieval aspects of memory, and visuospatial skills .
Patients with PDD often show a typical pattern of cognitive decline which shows characteristically a subcortical dementia that can be differentiated from AD in which cortical areas are affected early in the disease process and often include clear aphasia, apraxia, or agnosia. Dementia in PD is gradual in onset, and it is typically exhibited years after the onset of motor symptoms.
Evidence has shown widespread cortical cholinergic dysfunction to be factor of cognitive decline in PD.;Adrenergic and serotonergic deficits have also been described in PD but they have been associated with behavioral rather than cognitive function. Regional cortical Lewy body formation, have also been implicated in cognitive decline in PD.
Mri Brain Scans Detect People With Early Parkinson’s
Oxford University researchers have developed a simple and quick MRI technique that offers promise for early diagnosis of Parkinson’s disease.
The new MRI approach can detect people who have early-stage Parkinson’s disease with 85% accuracy, according to research published in Neurology, the medical journal of the American Academy of Neurology.
‘At the moment we have no way to predict who is at risk of Parkinson’s disease in the vast majority of cases,’ says Dr Clare Mackay of the Department of Psychiatry at Oxford University, one of the joint lead researchers. ‘We are excited that this MRI technique might prove to be a good marker for the earliest signs of Parkinson’s. The results are very promising.’
Claire Bale, research communications manager at Parkinson’s UK, which funded the work, explains: ‘This new research takes us one step closer to diagnosing Parkinson’s at a much earlier stage one of the biggest challenges facing research into the condition. By using a new, simple scanning technique the team at Oxford University have been able to study levels of activity in the brain which may suggest that Parkinson’s is present. One person every hour is diagnosed with Parkinson’s in the UK, and we hope that the researchers are able to continue to refine their test so that it can one day be part of clinical practice.’
We think that our MRI test will be relevant for diagnosis of Parkinson’s
Dr Michele Hu
You May Like: Can Parkinson’s Disease Cause Back Pain
Living With Parkinson’s Disease
Coming to terms with a diagnosis of Parkinson’s and living with the disease is challenging and will take a lot of adjustment. There are still things you can do that can help you to feel more in control of your situation and to stay positive. Some things that might help could include:
- choosing to lead a healthy lifestyle
- making informed decisions related to your treatment
- keeping a diary of your symptoms in preparation for meetings with health and social care professionals
- attending a self-management course
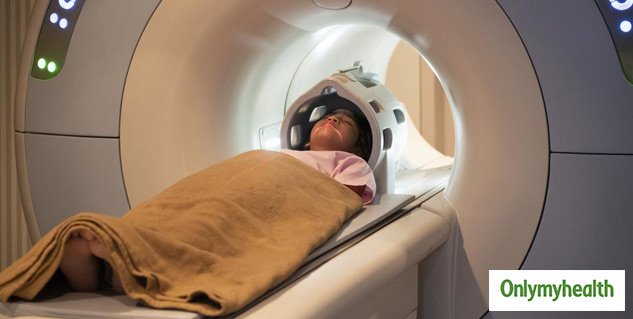
Where To Get A Parkinsons Mri
Your two main choices if youre thinking about a Parkinsons MRI are a hospital and a free-standing imaging center. An imaging center offers you a comfortable environment with the highest quality equipment and technicians who are extremely experienced and focus exclusively on imaging. Imaging centers are also more affordable than hospitals.
Do you need a Parkinsons MRI? Are you a doctor who wants to schedule a Parkinsons MRI for a patient? Then, contact us today. At American Health Imaging, we focus on imaging, and we would love to help you.
Don’t Miss: What State Has Highest Rate Of Parkinson’s
What Tests Might I Have
Your doctor may want to start by testing your or doing a scan to rule out other conditions.
People who have Parkinsons disease dont make enough of a chemical called dopamine, which helps you move. If those first tests dont show a reason for your symptoms, your doctor may ask you to try a medication called -levodopa, which your can turn into dopamine. If your symptoms get much better after you start the drug, your doctor probably will tell you that you have Parkinsons disease.
If the medication doesnt work for you and theres no other explanation for your issues, your doctor might suggest an imaging test called a DaTscan. This uses a small amount of a radioactive drug and a special scanner, called a single photon emission computed tomography scanner, to see how much dopamine is in your . This test cant tell you for sure that you have Parkinsons disease, but it can give your doctor more information to work with.
It can take a long time for some people to get a diagnosis. You may need to see your neurologist regularly so they can keep an eye on your symptoms and eventually figure out whats behind them.
What Causes Parkinsons Disease
We do not know what causes Parkinsons disease. There is some evidence to suggest that there is a genetic factor which increases the risk of Parkinsons disease within some families. Also, there might be an increased risk if people have come into contact with a particular toxin or toxins found in the environment via pesticides and other chemicals used in agriculture. The specific toxin or toxins have not yet been identified but there is ongoing research into this possible cause.
Also Check: How Long Can A Person Live With Parkinson’s Disease
How A Diagnosis Is Made
The bedside examination by a neurologist remains the first and most important diagnostic tool for Parkinsons disease . Researchers are working to develop a standard biological marker such as a blood test or an imaging scan that is sensitive and specific for Parkinsons disease.
A neurologist will make the diagnosis based on:
- A detailed history of symptoms, medical problems, current and past medications. Certain medical conditions, as well as some medications, can cause symptoms similar to Parkinsons.
- A detailed neurological examination during which a neurologist will ask you to perform tasks to assess the agility of arms and legs, muscle tone, gait and balance, to see if:
- Expression and speech are animated.
- Tremor can be observed in your extremities at rest or in action.
- There is stiffness in extremities or neck.
- You can maintain your balance and examine your posture.
Regional Differences In Gmd Slope Directionality
To further test differences in disease progression between early and PD groups, a comparison of the directionality of the early and PD slope parameters for the age and sex adjusted relationships between duration of disease and GMD was performed. For subcortical regions in early PD, one region had a positive slope, compared to 12 regions which had a negative slope. For subcortical regions in advanced PD patients, all 13 regions had a negative slope. For cortical regions in early PD, 13 regions had a positive slope, compared to one region which had a negative slope. For cortical regions in advanced PD patients, all 14 regions had a negative slope. The difference in the distribution of positive and negative slopes for subcortical and cortical regions in early PD is significant . Additionally, the difference in the distribution of positive and negative slopes for cortical regions between early PD and advanced PD is significant .
You May Like: What To Know About Parkinson’s Disease
The Importance Of Early Diagnosis
Early detection and diagnosis is important because the treatments for PD are more effective in the early stages of the disease. In addition, physical therapy and , which greatly improve symptoms and delay progression of the disease, are much easier to perform in the early stages.
Current diagnosis is made through the presence of motor symptoms; however, researchers have found that by the time motor symptoms occur, over 60% of all dopamine neurons in the basal ganglia of the brain have been damaged. Non-motor symptoms become apparent in people with PD long before motor symptoms, including sleep disturbances and loss of the sense of smell.3
Active areas of include looking for markers in the blood, urine, or cerebral spinal fluid that reliably detect PD, called . In addition, brain imaging tests that have high sensitivity for detecting PD are also being actively researched.4
