What You Need To Know
- Surgeons implant one or more small wires in the brain during a surgical procedure.
- The leads receive mild electrical stimulation from a small pulse generator implanted in the chest.
- Proper patient selection, precise placement of the electrodes and adjustment of the pulse generator are essential for successful DBS surgery.
- DBS does not fully resolve the symptoms of PD or other conditions, but it can decrease a patients need for medications and improve quality of life.
Am I A Good Candidate For Dbs
To determine if you are a good candidate, you:
Page reviewed by Dr. Chauncey Spears, Clinical Assistant Professor and Dr. Amelia Heston, Movement Disorders Fellow at the University of Michigan.
How Deep Brain Stimulation Works
Exactly how DBS works is not completely understood, but many experts believe it regulates abnormal electrical signaling patterns in the brain. To control normal movement and other functions, brain cells communicate with each other using electrical signals. In Parkinson’s disease, these signals become irregular and uncoordinated, which leads to motor symptoms. DBS may interrupt the irregular signaling patterns so cells can communicate more smoothly and symptoms lessen.
You May Like: Does Parkinson’s Qualify For Disability
Mechanism Of Action Of Dbs
Current hypotheses on the action mechanism of DBS include depolarization blockade , synaptic inhibition , synaptic depression , stimulation-induced disruption of pathological network activity , and stimulation of afferent axons projecting to the STN . Depolarization blockade and synaptic inhibition are likely to explain the similarity between the therapeutic benefit of DBS and lesional surgery. Recordings of decreased somatic activation in the stimulated nucleus favor these hypotheses . However, the increased output of projection neurons does not seem to be mediated by these phenomena . Another and currently favored hypothesis is that DBS overrides abnormal spike train patterns by an unphysiological, high-frequency pattern, and thereby masks pathological signals, which cause dysfunction of the remaining elements of the basal ganglia-thalamo-cortical and brainstem motor loop . The exact nature of the abnormal signals and the interaction between stimulation-induced neuronal responses and intrinsic brain activity remains elusive, but abnormalities of the firing rate and pattern of basal-ganglia neurons, changes in oscillatory activity and excessive synchronization at multiple levels of the motor loop have been proposed as pathophysiological correlates of motor symptoms in PD .
The Case For Doing Dbs Sooner Rather Than Later
In many cases, movement disorder patients only turn to DBS after their medications are no longer working as well as in the past. However, at Neurology Solutions, our position is that movement disorder patients who qualify for DBS should consider getting the procedure done sooner rather than later.
There are a few good reasons why doing DBS earlier might be beneficial, including:
- The brain stimulation inherent to DBS is potentially beneficial to the patient .
- A successful DBS procedure may allow the patient to substantially reduce their medications thus reducing potential long-term toxicity.
- Studies have shown that performing DBS earlier helps the patient have a better long-term outcome.
Also Check: Does Parkinson’s Make You Mean
Clinical Experience With Deep Brain Stimulation
The advent of modern DBS led to a major change in the therapeutic armamentarium for movement disorders. DBS rapidly overtook lesioning as the surgical treatment of choice for refractory movement disorders due to a number advantages: it is nondestructive and several stimulation parameters, including the location, size, intensity, and the shape of the stimulating current field can be adjusted following surgical implantation. These properties allow clinicians to program the DBS device in such a way as to maximize motor benefits while minimizing side effects, most of which are caused by the inadvertent stimulation of structures adjacent to the intended target. Perhaps most importantly for patients with PD, DBS has a lower reported complication rate when used bilaterally .
Since the first application of DBS for PD in 1993, several thousand patients worldwide have undergone surgical implantation. While many studies have reported the benefits and durability of this therapy , six large-scale, randomized, controlled clinical trials have been performed . Given the pervasive nature of this disease, the end points of these trials have appropriately included quality of life measures, the severity of motor symptoms in the medication off state, and time spent in the on state without troublesome motor symptoms .
Living With A Stimulator
Once the DBS has been programmed, you are sent home with instructions for adjusting your own stimulation. The handheld controller allows you turn the stimulator on and off, select programs, and adjust the strength of the stimulation. Most patients keep their DBS system turned on 24 hours day and night. Some patients with essential tremor can use it during the day and turn off the system before bedtime. Your doctor may alter the settings on follow-up visits if necessary.
If your DBS has a rechargeable battery, you will need to use a charging unit. On average charging time is 1 to 2 hours per week. You will have a choice of either a primary cell battery or a rechargeable unit and you should discuss this with you surgeon prior to surgery.
Just like a cardiac pacemaker, other devices such as cellular phones, pagers, microwaves, security doors, and anti theft sensors will not affect your stimulator. Be sure to carry your Implanted Device Identification card when flying, since the device is detected at airport security gates.
Don’t Miss: Can Stress Cause Parkinson’s
What Happens During Dbs
Implantation of a DBS lead generally requires a hospital stay of a day or longer. Procedures may vary depending on your condition and your healthcare providers practices. The lead and neurostimulator may be implanted at the same time, or the neurostimulator may be implanted in a separate procedure after the lead is implanted. Talk with your healthcare provider about what you will experience during your procedure.
Generally, surgery for DBS follows this process:
Deep Brain Stimulation For Movement Disorders
Deep brain stimulation has been approved for the treatment of movement disorders since the 1990s. Numerous studies have proven this surgerys superiority to medical therapy alone. The time to consider DBS surgery is when the quality of life is no longer acceptable on optimal medical therapy as administered by a movement disorder specialist. DBS surgery is very safe and recent advancements in device technology have improved patient outcomes as well.
You May Like: What Chemicals Cause Parkinson’s Disease
Who Should Get Deep Brain Stimulation
This is a common question with a surprisingly simple answer: Anyone who would get significant benefit from the treatment and can undergo the operation with minimal risk. It is not necessary to suffer for years after diagnosis, trying every known combination of medicine, before DBS can be considered. DBS is a surgical option that is known to improve quality of life for patients with movement disorders, so when ones quality of life is dramatically affected by the disease or by medication side effects, its time to consider DBS.
What Happens During Deep Brain Stimulation
This procedure actually involves two to three surgeries that usually happen at different times. The first one or two procedures are to insert the stimulation leads into each side of your brain at the same or separate times. The second procedure is to implant the stimulator battery known as a pulse generator under the skin of your upper chest.
Before these surgeries happen, your healthcare provider will usually insert an intravenous line to give you IV fluids. An IV also allows them to give you medications during the procedure as needed.
Lead placement
This procedure usually starts with your healthcare provider shaving the hair on your scalp. This makes it easier to place your head into a special frame that will hold your head still. The frame is set with four pins in your skull. This is done while youre under sedation, and you likely wont remember this part.
Once the frame is set, theyll bring in an intra-operative CT scanner to take images of your brain and identify the trajectory used for the electrode placement. Once the CT scan is complete, the entry point is identified, sedation is turned back on and your head is cleaned with surgical prep. Local anesthetic is then injected to numb that area of your scalp and skull. Your neurosurgeon will then make a small cut .
Pulse generator placement
Read Also: Side Effects Of Parkinson Medications
What Risks Come Along With Doing Deep Brain Stimulation
DBS is a surgical procedure. As with any surgery there are some risks associated with it. Some of the risks of DBS include infection and bleeding. Your neurosurgeon may discuss some additional risks with you. Studies have shown that any risks are relatively small, but they should be kept in mind when considering DBS.
Suggested Criteria For Surgical Eligibility
1) High level of certainty about the diagnosis of idiopathic PD using the Queen Square Brain Bank diagnostic criteria3333. Hughes AJ, Daniel SE, Kilford L, Lees AJ. Accuracy of clinical diagnosis of idiopathic Parkinsons disease: a clinico-pathological study of 100 cases. J Neurol Neurosurg Psychiatry. 1992 Mar 55:181-4. https://doi.org/10.1136/jnnp.55.3.181 or the new international Parkinson and Movement Disorders Society criteria22. Postuma RB, Berg D, Stern M, Poewe W, Olanow CW, Oertel W et al. MDS clinical diagnostic criteria for Parkinsons disease. Mov Disord. 2015 Oct 30:1591-601. https://doi.org/10.1002/mds.26424. An alternative diagnosis of atypical or secondary parkinsonism should be carefully excluded
2) Clinical progression for a minimum of four years is additionally useful for improving the certainty of a clinical diagnosis of idiopathic PD
4) Exceptions to the need for levodopa responsiveness include patients with severe disabling resting tremor, resistant to dopaminergic therapy. In these patients, the symptomatic benefit is likely, regardless of the levodopa challenge test response
8) The following attributes give support to the surgical eligibility: young age onset, severe tremor, need to reduce medications, nocturnal akinesia.
Recommended Reading: Does Parkinson’s Disease Affect Memory
What Are The Risks Or Complications Of Dbs
Because DBS does involve surgery, there are some possible complications and risks. Your healthcare provider is the best person to tell you about the possible risks and complications. They’re the best source of information because they can consider your medical history, circumstances and more.
The possible complications of surgery include:
The Key Is The Activation Of Ppn Neurons
In Parkinsons Disease, nerve cells that produce dopamine progressively die. Since the 1960s, doctors have relied on medication to replace the missing dopamine, but it is notoriously difficult to fully control symptoms as the disease progresses.
In many people the movement symptoms do not respond well to medical treatment in the later stages of this disease, so there has been done a lot of research into alternative treatments, including a search for optimal targets for deep brain stimulation, explains Postdoc Debora Masini, first author of the new study, which included several different strategies to substantiate their findings.
When we stimulated these specific neurons in the caudal area of the PPN, the animals were able to walk normally, across longer distances and with normal walking speed, as opposed to before the stimulation, where they would display symptoms of Parkinsons Disease, says Debora Masini.
We systematically compared stimulation of different locations and cell types in a series of complementary experiments. And they all pointed towards the same conclusion.It strongly indicates these excitatory neurons in the caudal PPN are an ideal target for recovery of movement loss, she says.
The researchers hope that the new study could aid clinicians when they pick the exact location for DBS in the brainstem.
Also Check: Do Both Hands Shake With Parkinson’s
When Should I Call My Healthcare Provider Or Go To The Hospital
Because DBS involves surgery especially the procedure on your brain there are some warning signs you shouldn’t ignore. You should call your healthcare provider immediately or go to the hospital outside of business hours if you have the following symptoms:
- Severe headache that happens suddenly or wont go away.
- Bleeding from your incisions.
- Redness, swelling or unusual warmth which are signs of infection around your incisions.
- Sudden changes in your vision, such as seeing double, blurred vision or loss of vision.
- Fever of 101 degrees F or higher.
Why Should A Movement Disorder Patient Consider Dbs
Many more movement disorder patients qualify for a deep brain stimulation surgery than actually go through with the procedure. But why is that?
For starters, DBS is literally brain surgery, and for many people, that is simply a bridge too far. While DBS is generally considered a safe procedure, DBS can nonetheless have potentially serious side effects, such as bleeding or a stroke during the surgery itself. Less serious side effects can result from the device needing an adjustment.
On the other hand, DBS can be extremely effective at helping the patient control their symptoms. One study has shown that 87% of the individuals who had undergone DBS showed improvement in motor control within one year after surgery. Also, DBS has been shown to reduce the need for medications in movement disorder patients a benefit thats over and above what it can do for the inherent motor symptoms.
But its important for people to understand that DBS is not a cure. The goal is to help manage a patients symptoms, and perhaps, to slow the progression of some movement disorders.
Read Also: Nursing Diagnosis For Parkinson’s Disease
How Does Deep Brain Stimulation For Parkinsons Work
Deep brain stimulation works by modifying abnormal electrical activity in the brain. It was first approved for Parkinsons tremors in 1997 and has become an established treatment to control additional motor symptoms of Parkinsons disease.
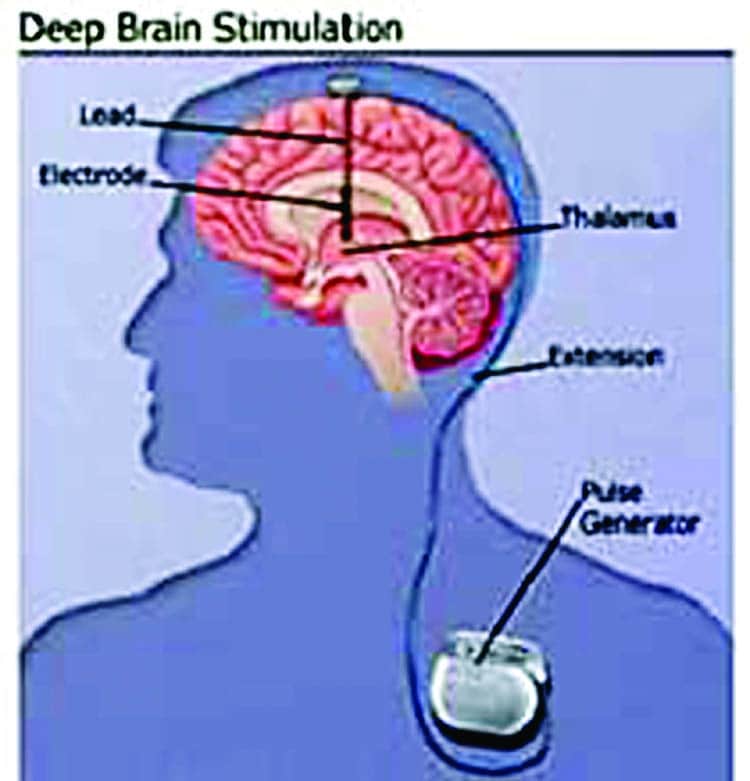
DBS involves three main components:
- Leads: Leads are implanted in the brain in a region responsible for motor activity.
- Implantable pulse generator : A separate procedure is performed to implant a battery-operated device in the chest or in the abdomen. An IPG is similar to a pacemaker for the heart and has been coined by some as a pacemaker for the brain.
- Extension: A thin, insulated wire is passed beneath the skin between the leads and implantable pulse generator to deliver the electrical stimulation from the pulse generator to the leads.
The target area in the brain is first identified by magnetic resonance imaging or computed tomography . Then, the leads are placed via small holes that a surgeon drills in the skull.
This is considered a minimally invasive surgery that is done in the operating room with local anesthesia. It usually requires an overnight stay.
The IPG is inserted in a separate surgical procedure in the operating room roughly a week later.
After a few weeks, a neurologist begins to program the unit. This process can take several additional weeks to months. When this is completed, people are able to manage the device with a handheld remote control.
The Symptoms That Dbs Treats
Deep brain stimulation is used primarily to treat the motor symptoms of Parkinsons disease, but this can vary somewhat between the different placement sites. Symptoms treated include:
- Abnormal movements : Dyskinesias are often a side effect of medications for Parkinsons disease and include involuntary movements such as twisting, head bobbing, squirming, and more.
DBS is not usually helpful with walking problems or balance, though improvements in the symptoms above can indirectly affect walking. It also does not provide significant benefits for non-motor symptoms of Parkinsons such as cognitive changes, mood changes , or problems with sleeping.
The benefits of DBS can be estimated by looking at how a person responds to levodopa. Symptoms that respond to levodopa will often respond to DBS . But symptoms that are not changed with levodopa are unlikely to be improved by DBS.
DBS often allows for a reduction in the dosage of levodopa, which in turn can result in fewer involuntary movements and a reduction in off time. The result is often improved quality of life.
Read Also: What Is The Typical Treatment For Parkinson’s Disease
Remote Brain Stimulation: A New Treatment For Parkinsons Disease
figures by Daniel Utter
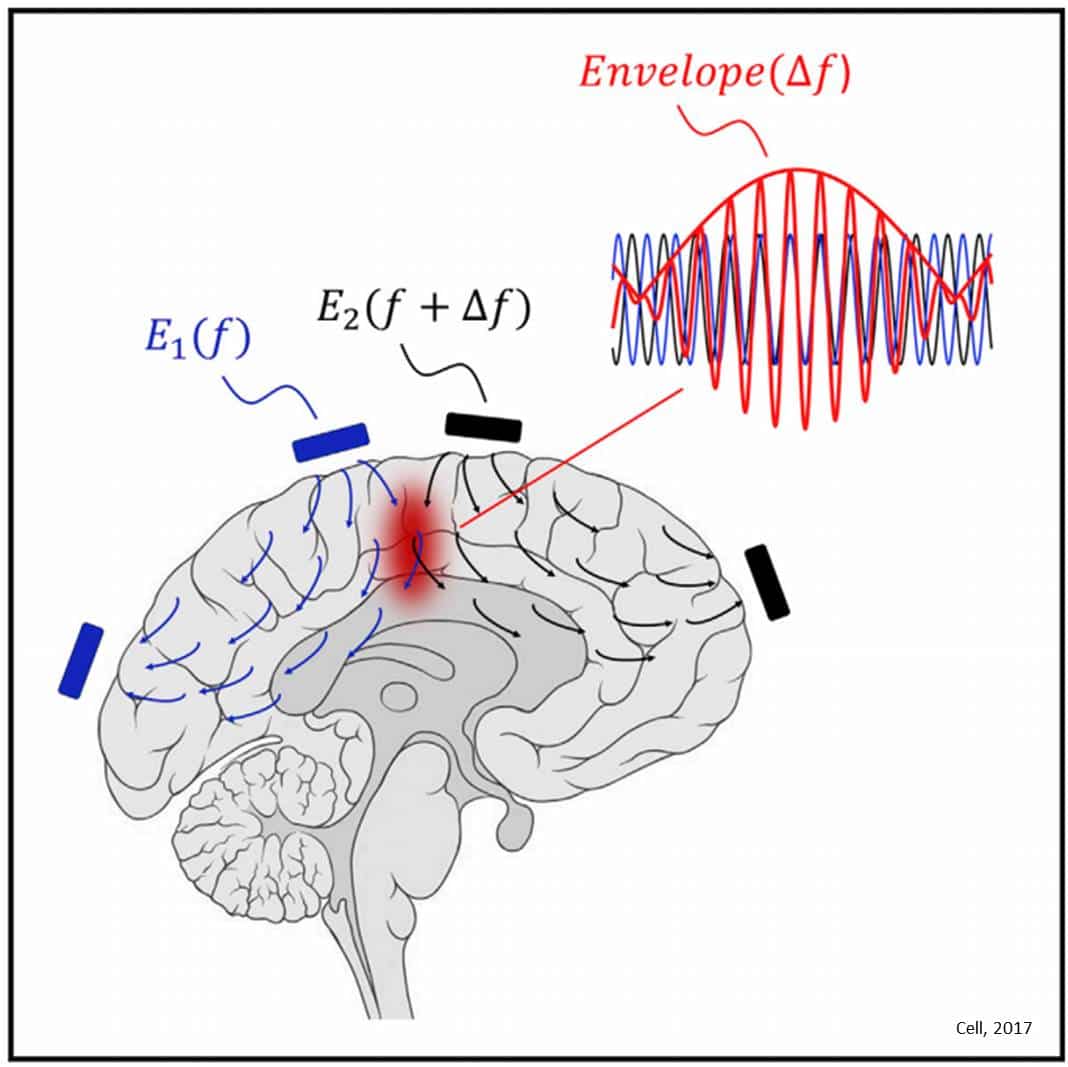
What do you think of the idea of inserting a long metal wire into your brain? Thats what doctors have done to ease the symptoms of Parkinsons disease over the past 20 years. Sound scary? A new technique called temporal interference stimulation is exploring the possibility of achieving the same effects by attaching electrical stimulators to the outside of the skullno brain surgery or metal wires required.
How Is The Surgery Performed
UPMC was one of the first centers to use ROSA robotic assistance for the placement of DBS electrodes. ROSA is similar to a GPS device for the brain. It provides the surgeon with a roadmap to reach the intended brain targets. The patient is sedated for the beginning of the surgery while we make a small opening in the skin and bone at the surgical site. The patient will not feel or remember this part of the surgery, but once these steps are complete, he is awoken for the remainder of the surgery.
Brain MappingWe use neurophysiology recordings from very thin electrodes inserted into the brain to map activity in the intended target and confirm the best spot for the DBS electrode. It is important for the patient to be awake during this part of the surgery so we can obtain the best recordings possible, which will aid in the most accurate placement of the DBS electrode. The brain mapping is not painful and the surgical team will be available to provide reassurance and feedback the entire time.
Intra-Operative Stimulation TestingWhen the best site is identified from the brain mapping, the DBS electrode is inserted and tested. We monitor the patient for improvement in his symptoms, for example tremor, and also ask him to report any new sensations he experiences. Again, this part of the procedure is not painful, but provides valuable feedback to the surgical team.
Recommended Reading: Does Parkinson’s Cause Tinnitus
