Difference Between Parkinsons Disease And Als Signs And Symptoms
Parkinsons disease typically begins with tremors, followed by muscle stiffness, difficulty standing or walking, changes in speech, slow movements, impaired posture and balance, loss of automatic movements, and writing changes.
Signs and symptoms of ALS include slurred speech, hoarseness, difficulty swallowing, emotional liability , loss of tongue muscle contour, excess saliva, difficulty breathing, limp muscles or flaccid weakness, muscle wasting, and twitching.
In the early stages of the disease, ALS patients may notice that performing regular everyday tasks has become more challenging. For example, they may experience difficulty climbing steps or getting up from a chair. Symptoms may first begin on one side of the body, but as the condition progresses, they spread to both sides.
As you can see, ALS and Parkinsons disease share symptoms associated with the negative impact of both conditions on movement and muscle function.
Does Medicare Pay For In
Medicare is a form of health insurance provided by the federal government for people over 65 or those under 65 with disabilities. For people with ALS, Medicare covers assessments for speech-language pathology, and physical, occupational, and respiratory therapies. It also covers durable medical equipment , as recommended by a physical therapist. Medicare covers consultations with physical therapists to teach family caregivers and/or personal care assistants how to help with range-of-motion exercises and how to use the DMEs. Hospice care is also covered under Medicare.
There is no 24-month waiting period for people with ALS to receive Medicare benefits. People with ALS, who are deemed to be homebound, will receive Medicare benefits as soon as they receive social security disability benefits. However, Medicare only covers intermittent, short-term care needs. People with ALS typically need long-term, skilled, and personal care that is not covered by Medicare.
Visit medicare.gov for more information.
Consider seeking out respite care for extra assistance.Taking care of yourself will only make you a better caregiver.
New Century Home Health Care
1387 E. 12 Mile Rd.Madison Heights, Michigan 48071
Postmortem Evaluation Of Parkin Solubility
Several lines of evidence suggest that the stability of parkin is fragile. Very minor fluctuations within the parkin sequence or the intracellular environment where parkin is expressed can have profound effects on the solubility and activity of the protein. However, many of the studies reviewed here have made exclusive use of cell culture conditions to explore the stability and solubility of parkin, raising the question of whether parkin solubility is an issue within the normal or diseased human brain. Notably, three studies have explored postmortem human brain, and all three reports have found evidence of pathologic changes in parkin solubility in the neurologic disease samples. Two of these studies reported increased levels of insoluble parkin in PD brain tissue, compared to controls , whereas the third found that parkin was elevated in the insoluble fraction of brains taken from patients with diffuse Lewy body disease , indicating that parkin solubility is affected in human neurologic disease and providing the most tantalizing evidence for some link between parkin and -synuclein. Interestingly, the translocation of parkin from a soluble to insoluble state has also been reported in a rodent model of stroke , as well, and is therefore not limited to human neurodegenerative disorders.
Also Check: What Is The Life Expectancy Of Someone With Parkinson’s Disease
Serotonergic Modulation Of Basal Ganglia And Mesencephalic Dopaminergic Activity In Pd
The basal ganglia are composed of the striatum , subthalamic nucleus , internal and external globus pallidus and SN, and are part of the BG-cortico-thalamic circuits. This highly organized network is important for motor control, emotion, and cognition. It has been firmly established that BG nuclei receive vast serotonergic input mainly coming from the rostral RN clusters , with effects on mesencephalic dopaminergic activity depending on the specific nucleus and its receptor distribution . In PD, lesioning of the RN in addition to DA depletion in the striatum and SNparticularly of the pars compacta are hallmarks of the disease, leading to overactivation of the output regions of the BG, i.e., GPi and SN pars reticulata , which contain large GABAergic neurons. This cascade results in a net decreased activity of the supplementary motor areas, premotor, and primary motor cortices, triggering parkinsonian symptoms . Overall, the loss of 5-HT neurons is not as profound as the loss of DA neurons, and may not be sufficient to cause motor or non-motor symptoms per se, however, both systems closely interact, and combined depletion certainly seems to aggravate the situation, as was shown in a parkinsonian rat model . Moreover, 5-HT and 5-HIAA levels, as well as SERT expression, are reduced in various BG nuclei , and the serotonergic system is strongly involved in the mechanism of action of antiparkinsonian therapeutics, such as levodopa , and high frequency stimulation of the STN .
Als Vs Parkinsons Disease: Symptoms
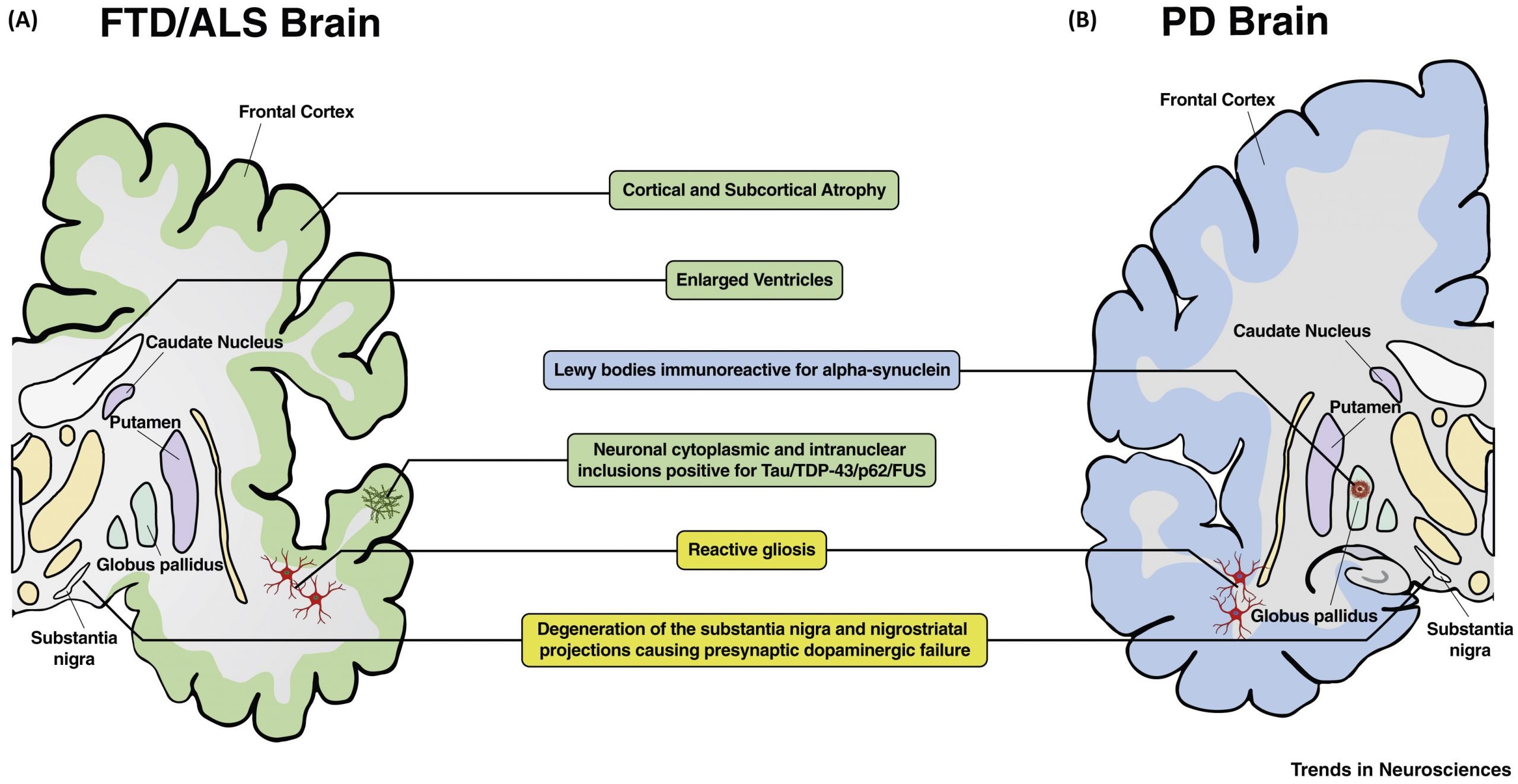
ALS is a neurodegenerative disease that affects the neurons in the body. It usually starts as a localized issue in an area like the hands or legs. A person diagnosed with ALS will often feel weakness in a certain part of the body. The disease destroys the neurons and begins to spread throughout the whole body causing damage elsewhere.
Parkinsons disease is also a neurodegenerative disorder but it actually affects a particular part of the brain rather than all neurons. It specifically attacks parts of the brain called the basal ganglia and the substantia nigra. Early symptoms may include difficulty sleeping and loss of sense of smell rather than loss of motor movement.
Also Check: Late Stage Parkinson Disease
Parkinson’s Disease Drug Proves Effective Against Als In Japan Research Using Ips Cells
May 21, 2021
TOKYO — A Parkinson’s disease drug has been confirmed effective in treating amyotrophic lateral sclerosis , a disease causing gradual loss of muscle strength throughout the body, according to a Japanese research team’s findings announced May 20.
In a clinical trial using induced pluripotent stem cells derived from patients, the team led by Hideyuki Okano, a professor of physiology at Keio University, was able to slow down the disease’s progression. The researchers say it could become a new treatment option for ALS, for which there are few effective treatments, and they aim to apply as soon as possible for its approval as a therapeutic drug.
ALS is an intractable disease that causes gradual loss of motor nerve cells transmitting commands from the brain to muscles throughout the body as it progresses, even breathing becomes difficult. About 10,000 ALS patients live in Japan the disease has no permanent cure.
The Parkinson’s disease tablets confirmed effective in the clinical trial were ropinirole hydrochloride extended-release tablets . The team has been conducting research using iPS cells to understand the cause of the disease and develop new drugs.
Using motor nerve cells generated from patient-derived iPS cells, they reproduced the disease conditions of ALS and added 1,232 types of existing drugs to the cells, through which they found that ropinirole hydrochloride was effective in suppressing cell death.
The Diseases And Your Nerve Cells
“Sclerosisâ comes from the Greek word for âscar.â Both ALS and MS cause scarring of the covering of nerve fibers. But the process of how that happens is different for each.
Nerve cells in your body are wrapped in thin coverings called myelin sheaths. They protect these cells, similar to how insulation protects electrical wires.
When you have MS, your body attacks the myelin sheaths in your brain and spinal cord.
When myelin sheaths are damaged, signals from your brain to other parts of your body get short-circuited.
ALS breaks down the actual nerve cells in your brain and spinal cord. These cells, called motor neurons, are in charge of the voluntary muscles in your arms, legs, face, and diaphragm for breathing.
You lose control of your motor functions, and as the motor neurons break down, the myelin sheaths harden.
Read Also: What Is Life Expectancy Of Parkinson’s Patients
Introduction: Neurologic Disorders Of Movement
More than two million Americans are believed to suffer from some form of neurodegenerative movement disorder, the total cost of which is estimated to exceed $10 billion annually. Because no society on earth is spared the effects of these crippling diseases, the figures for other countries are similar, adjusted for population differences. The neurodegenerative diseases Parkinsons disease and amyotrophic lateral sclerosis are the most important of the movement disorders from a proteostasis perspective. ALS is often classified separately, as a motor neuron disease, but there are a number of reasons for considering them together, of which perhaps the most important is that the two sometimes present together, as in the Parkinsonism-dementia complex of Guam . This movement disorder occurs among the Chamorro populations of Guam and the Mariana Islands and is frequently accompanied by a motor neuron disease resembling ALS. The course of the disease is rapid, with death typically occurring within 5 years .
In the following sections, we will review the evidence that links dysfunction in the proteostasis of certain proteins to the pathology of ALS and PD. Recent data support the notion that at least most forms of Parkinsons disease may be amenable to therapeutic strategies aimed at proteostasis of -synuclein or proteins called parkin or LRRK2, while the situation with ALS is still far from clear.
Parkinsons Disease Vs Als Differences In Symptoms Causes And Treatment
Written byDevon AndrePublished onJuly 25, 2016
Parkinsons disease and ALS can cause difficulties in movement and are both known to be progressive neurological diseases.
ALS is part of a cluster of disorders known as motor neuron diseases that involve gradual degeneration and death of motor neurons. In a healthy individual, messages from motor neurons in the brain are transmitted to the motor neurons in the spinal cord and sent to the particular muscles. In ALS, this communication degenerates and cells begin to die. As a result, the message that is transmitted is incomplete. Unable to function, the muscles begin to weaken and waste away over time. Eventually, communication from the brain to muscles is lost completely.
In its early stage, ALS also known as Lou Gehrigs disease may appear as Parkinsons disease, which is also a neurological disease similar to ALS. Here we will outline the causes, symptoms, and treatment options for both ALS and Parkinsons disease to help you understand the differences between the two.
Don’t Miss: What Are Early Warning Signs Of Parkinson’s Disease
Parkinsons Disease Vs Als: Risk Factors And Complications
Risk factors for Parkinsons disease include being over the age of 50, being male, having a family history of Parkinsons disease, carrying gene variations, experiencing a head injury, being exposed to environmental toxins, and taking certain medications such as anti-anxiety medications or sleeping pills.
Complications associated with Parkinsons disease include difficulty thinking, depression, emotional changes, swallowing problems, sleep problems and disorders, bladder issues, constipation, changes in blood pressure, smell dysfunction, fatigue, pain, and sexual dysfunction.
Studies into ALS have revealed some interesting insight. For example, it may just be that some people with this disease are triggered by certain environmental factors. The environmental triggers under investigation include smoking, lead exposure, and military service. Recent research has indicated that people who have served in the military are at a higher risk of getting ALS.
Studies are also looking at the entire human genome, since research has uncovered a number of genetic variations that people with familial ALS and some with non-inherited ALS have in common. These variations might make people more prone to ALS.
Als As A Disease Of Rna Quality Control
Although ALS research was dominated for many years by the apparent connection between SOD1 misfolding and FALS, the recent discovery of two additional genes, mutations which appear to be associated with both familial disease and increased risk for sporadic ALS, has caused a rethinking of the molecular etiology of most forms of the disorder. In contrast to the antioxidant enzymatic activity of SOD1 and its tendency to form pathological aggregates, these two new genes, TDP-43 and FUS/TLS, encode primarily nuclear proteins that function in RNA biology. As we shall see, they not only raise the possibility that ALS is an RNA-based disease, they also suggest that a broader view of the concept of proteostasis may be valuable for developing new approaches to its treatment.
You May Like: Hemp Oil For Parkinson’s
Posttranslational Modifications That Inactivate Parkin
The reports summarized above raise the intriguing possibility that idiopathic PD pathogenesis or disease risk may arise by processes whereby neuronal stress might inactivate parkin via insolubility and aggregation. As a biochemical phenocopy of PARK2-associated familial PD, a severe loss of active, soluble parkin could compromise the viability of nigral neurons in the sporadic disease.
The one problem with this model is that Lewy bodies have generally not been observed in PARK2-associated familial PD brains, whereas they are almost always present to some extent in postmortem analyses of sporadic PD patients. No biochemical or genetic evidence has yet conclusively tied parkin into -synuclein aggregation, raising the possibility that neither protein is the direct cause of any form of PD, but that each may act independently through either the same or different downstream initiators of cell death. Of course, the other possibility is that macroscopic -synuclein aggregates are not involved in pathogenesis, and that loss of parkin function causes disease by producing whatever the actual toxic -synuclein species is.
So What’s The Difference Between Als And Parkinson’s Disease
Clockwise from top left: Robin Williams had been diagnosed with Parkinsons before his death Stephen Hawking has been living with ALS for 50 years Lou Gehrig brought ALS, now also know as Lou Gehrigs disease, to the publics attention and Michael J. Fox received his Parkinsons diagnosis in 1992.
News that Robin Williams had been grappling with a diagnosis of Parkinsons disease before ending his life has sparked increased interest in the disorder this week. And thats coincided with a fast-rising awareness of a similar disease amyotrophic lateral sclerosis, or ALS due to the Ice Bucket Challenge, a fundraising campaign thats swept social media recently, prompting everyone from Ethel Kennedy to Justin Timberlake to dump freezing water over their heads in the name of research. So how closely linked to Parkinsons is ALS? Both are progressive neurodegenerative diseases, and neither has a cure. But beyond that, the differences are vast.
Both occur because some cells in the brain degenerate, and both are diseases of the motor system, meaning they affect how someone moves, Dr. U. Shivraj Sohur, a movement disorder specialist with the MassGeneral Institute for Neurodegenerative Disease, told Yahoo Health. From there, the separation happens quickly, both from a neurology point of view and from a patients experience.
Related:Robin Williams: Is Parkinsons Disease Linked to Suicide?
Related:#IceBucketChallenge Goes Big on Social Media
Parkinsons disease
Read Also: Is Parkinson’s Deadly
Where Can I Get More Information
For more information on neurological disorders or research programs funded by the National Institute of Neurological Disorders and Stroke, contact the Institutes Brain Resources and Information Network at:
Office of Neuroscience Communications and EngagementNational Institute of Neurological Disorders and StrokeNational Institutes of HealthBethesda, MD 20892
NINDS health-related material is provided for information purposes only and does not necessarily represent endorsement by or an official position of the National Institute of Neurological Disorders and Stroke or any other Federal agency. Advice on the treatment or care of an individual patient should be obtained through consultation with a physician who has examined that patient or is familiar with that patient’s medical history.
All NINDS-prepared information is in the public domain and may be freely copied. Credit to the NINDS or the NIH is appreciated.
Serotonergic Degeneration In Pd And Als
Staging of brain pathology in PD demonstrated an early involvement of Lewy body depositions within the RN. In more detail, Halliday et al. firstly described a 56% loss of serotonergic neurons in the median RN of PD compared to control brain. Afterwards, Braak et al. determined six stages in the evolution of PD-related pathology, with lesions being present in the median RN in the caudal brainstem already from stage two onwards. Furthermore, 5-HT depletion was observed in various target areas of the RN, such as in the basal ganglia, hypothalamus, hippocampus, and prefrontal cortex . This was later confirmed by in vivo imaging studies, revealing new insights. For instance, Politis et al. applied 11C-DASB-PET to early-stage PD patients, and demonstrated reduced SERT binding in the caudate nucleus, thalamus, and anterior cingulate cortex, whereas PD subjects with established disease showed additional 11C-DASB binding reductions in the putamen, insula, posterior cingulate cortex, and, prefrontal cortex. Further binding reductions were noticed in the ventral striatum, RN, and amygdala of advanced PD patients. Interestingly, the loss of SERT binding in the RN occurred in later stages, pointing to an earlier loss of serotonergic projections instead of the neurons themselves.
You May Like: Rapid Onset Parkinsonism
Improving Health And Care Services For People Affected By Parkinson’s
We’ve launched a new report, Nobody really knows us the state of health and social care for people with Parkinsons-related dementia.
The report demonstrates the scale of the challenges that people with Parkinson’s-related dementia face right from the outset of their diagnosis and makes recommendations to improve health and care services.
It’s based on extensive interviews with people with Parkinson’s-related dementia and their carers, and a survey of carers and healthcare professionals, including Parkinson’s nurses, geriatricians, physiotherapists and neurologists.
We were delighted to welcome experts from across the health and social care sector to the report’s launch on 23 November, including representatives from dementia charities. The meeting heard from:
- Rachael Maskell MP, Shadow Minister for Civil Society, about the opportunities for change the report presents and the challenges she has seen as a constituency MP
- Caroline Rassell, Parkinsons UK’s CEO, who shared the key findings of the report and urged decision-makers to take action on them
- Admiral Nurse Rachel Thompson, who spoke about how reform can support better Parkinson’s dementia care
- Barbara Deering, who gave a powerful account of her experience of caring for her husband Barney, who lived with Parkinson’s-related dementia
