Medicines For Parkinsons Disease
Medicines can help treat the symptoms of Parkinsons by:
- Increasing the level of dopamine in the brain
- Having an effect on other brain chemicals, such as neurotransmitters, which transfer information between brain cells
- Helping control non-movement symptoms
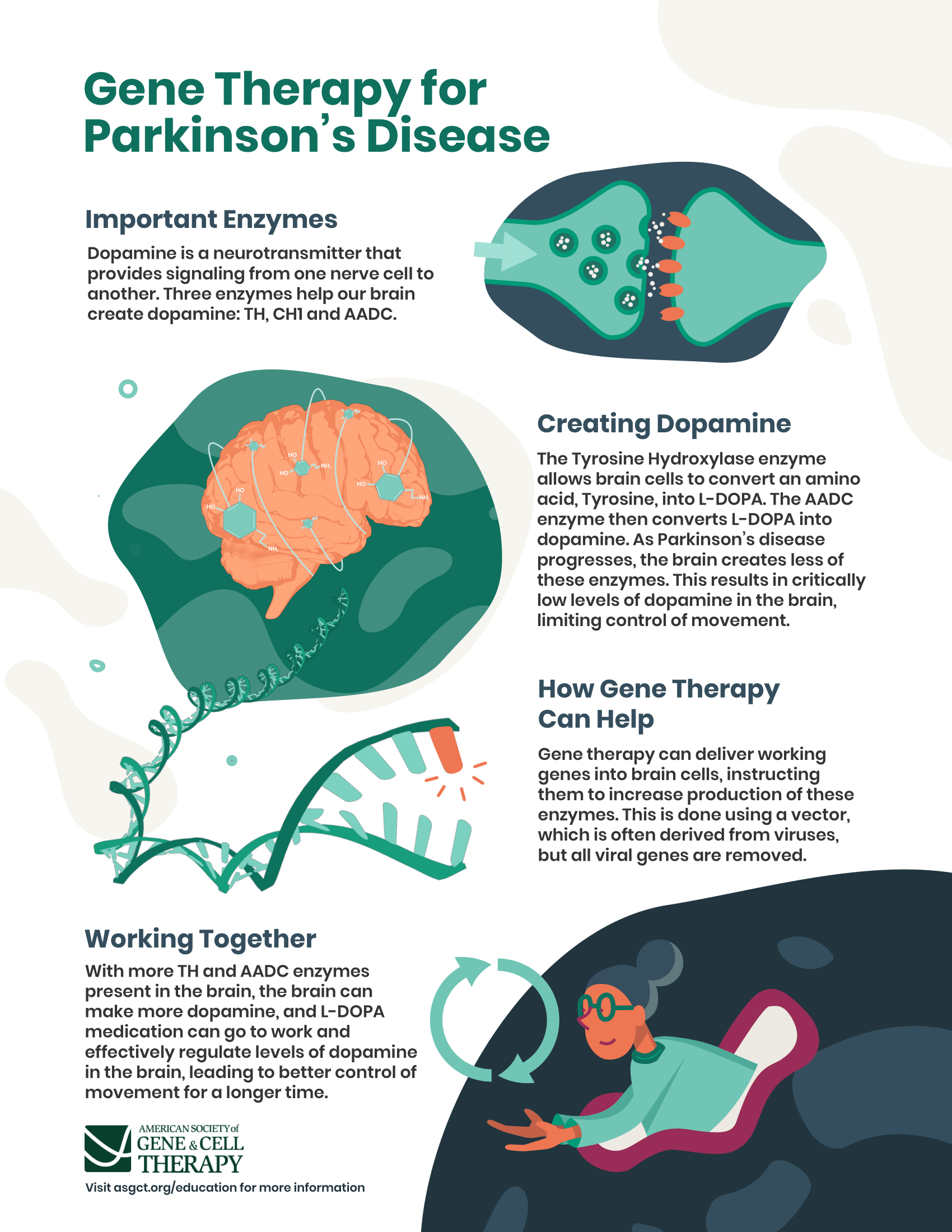
The main therapy for Parkinsons is levodopa. Nerve cells use levodopa to make dopamine to replenish the brains dwindling supply. Usually, people take levodopa along with another medication called carbidopa. Carbidopa prevents or reduces some of the side effects of levodopa therapy such as nausea, vomiting, low blood pressure, and restlessness and reduces the amount of levodopa needed to improve symptoms.
People living with Parkinsons disease should never stop taking levodopa without telling their doctor. Suddenly stopping the drug may have serious side effects, like being unable to move or having difficulty breathing.
The doctor may prescribe other medicines to treat Parkinsons symptoms, including:
- Dopamine agonists to stimulate the production of dopamine in the brain
- Enzyme inhibitors to increase the amount of dopamine by slowing down the enzymes that break down dopamine in the brain
- Amantadine to help reduce involuntary movements
- Anticholinergic drugs to reduce tremors and muscle rigidity
Investigational Treatments For Movement Disorders
At the University of Chicago Medicine, our patients are the first to benefit from leading research to find better treatments for movement disorders. We are designated as a Center for Advanced Research by the American Parkinson Disease Association for our excellence in state-of-the-art patient care and quest to find improved therapies through high-level research.
Our physicians are investigating movement disorders at the molecular level to identify precise causes of these diseases. They conduct clinical trials, regularly publish findings and serve as editors and on editorial boards of respected medical journals.
Sharing knowledge with institutions throughout the world, our physician-scientists work with grant-funded studies, including support from the National Institutes of Health, Michael J. Fox Foundation, and Parkinsons Disease Foundation, among other organizations.
Support For People Living With Parkinsons Disease
While the progression of Parkinsons is usually slow, eventually a persons daily routines may be affected. Activities such as working, taking care of a home, and participating in social activities with friends may become challenging. Experiencing these changes can be difficult, but support groups can help people cope. These groups can provide information, advice, and connections to resources for those living with Parkinsons disease, their families, and caregivers. The organizations listed below can help people find local support groups and other resources in their communities.
Recommended Reading: Is Blurred Vision A Symptom Of Parkinson’s
Apda Parkinsons Research Centers
David G. Standaert, MD, PhD, Director
APDA funding supports:
- Studies of neuroinflammation, protein aggregation and oxidative stress in PD as well as the role of the microbiome
- Multiple clinical trials including those testing novel drugs, DBS techniques and exercise intervention
- An active DBS program with approximately 150 procedures performed per year
- Approximately 6,800 patient visits per year
- Studies that probe the biology of PD-causing genetic mutations
- A biomarker discovery program using specimens from more than 2,700 participants
- A drug discovery program that utilizes technologies such as stem cells and big data analytics
- Approximately 2,200 patients visits each year
- Studies aimed at understanding the brain pathways involved in PD
- Clinical trials investigating treatments for wearing off, hallucinations, low blood pressure, daytime sleepiness and dementia
- An active DBS program and approximately 80-100 procedures performed per year
- Approximately 14,000 patient visits per year
APDA funding supports:
- Studies to identify potential PD biomarkers
- Characterization of PD among various ethnic groups
- Exercise intervention, wearable technology and attention training clinical trials
- Approximately 4,000 patient visits per year
- Studies of genetic and environmental risk factors of PD
- Drug development for neuroprotection in PD
- An active DBS program with 75-100 procedures performed yearly
- Approximately 6,500 patient visits each year
J. Timothy Greenamyre, MD, PhD, Director
What Is Parkinson’s Disease
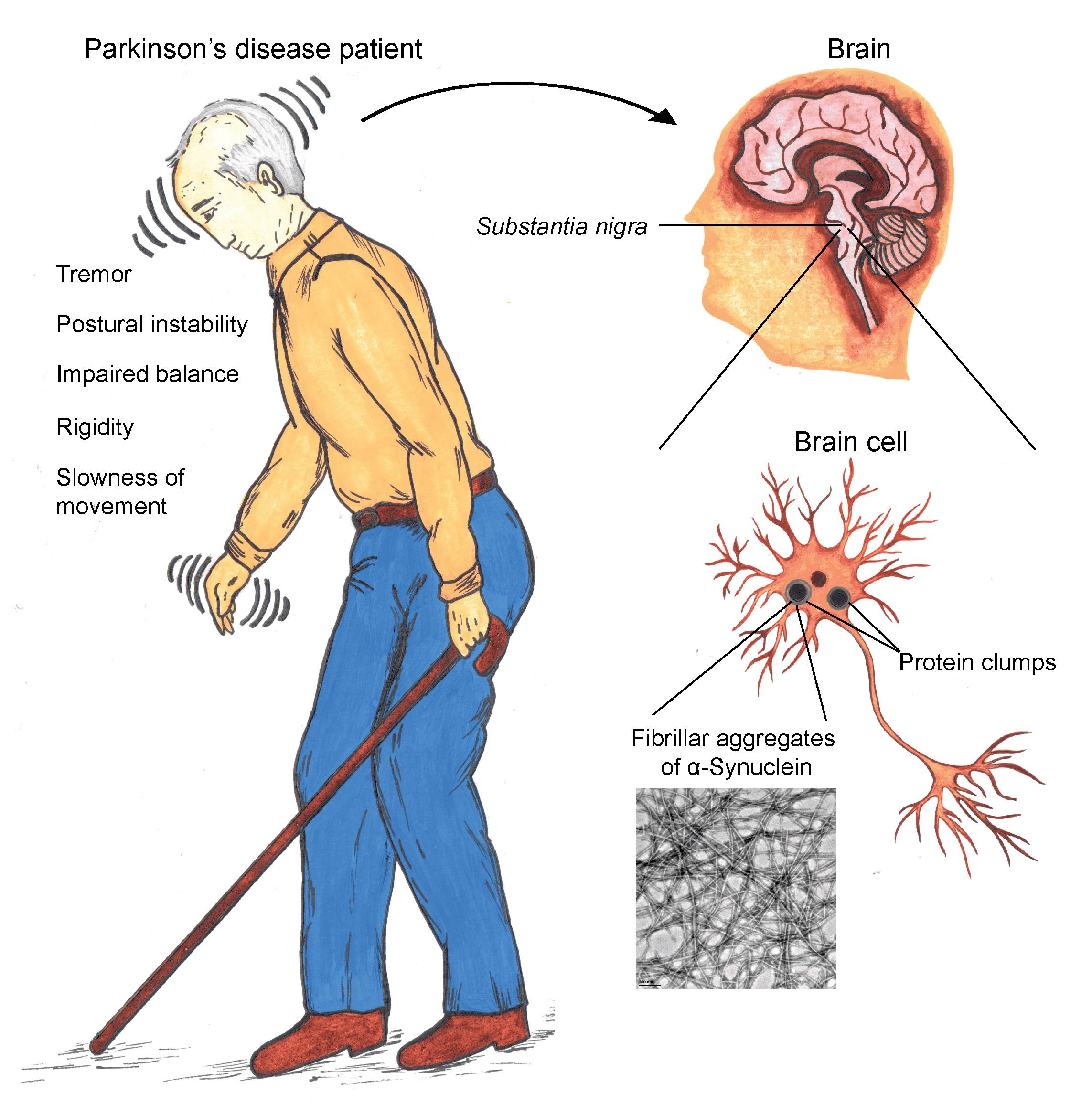
Parkinsons disease is movement disorder of the nervous system that worsens over time. As nerve cells in parts of the brain weaken or are damaged or die, people may begin to notice problems with movement, tremor, stiffness in the limbs or the trunk of the body, or impaired balance. As these symptoms become more obvious, people may have difficulty walking, talking, or completing other simple tasks. Not everyone with one or more of these symptoms has PD, as the symptoms appear in other diseases as well.
No cure for PD exists today, but research is ongoing and medications or surgery can often provide substantial improvement with motor symptoms.
Don’t Miss: Does Jamie Foxx Have Parkinson’s
Establishing Pd Research Priorities
The NINDS-organized Parkinsons Disease 2014: Advancing Research, Improving Lives conference brought together researchers, clinicians, patients, caregivers, and nonprofit organizations to develop 31 prioritized recommendations for research on PD. These recommendations are being implemented through investigator-initiated grants and several NINDS programs. NINDS and the NIHs National Institute of Environmental Health Sciences held the Parkinsons Disease: Understanding the Environment and Gene Connection workshop to identify priorities for advancing research on environmental contributors to PD.
Research recommendations for Lewy Body Dementia, including Parkinsons disease dementia, were updated during the NIH Alzheimers Disease-Related Dementias Summit 2019 .
The Future Of Parkinsons Diagnosis
Right now, a Parkinsons diagnosis is often based on observable symptoms. These observations may be supported by a dopamine scan, sometimes called a DaTscan. Thats because many of the motor symptomslike tremor, slowness of movement, and muscle rigidityare linked to a deficiency in the neurotransmitter dopamine. This scan can show abnormalities in the transmission of dopamine in the brain. So it may be an effective early screening tool.
In the study that we just published last year, we used the DaTscan and smell testing as our screening tool, says Dr. Stern. They found that two-thirds of people who had an abnormality in their DaTscan would go on to develop Parkinsons disease, even if they had no symptoms at the time of the scan.
Researchers are also looking into whether Parkinsons has different subtypes, which Dr. Stern says has the potential to revolutionize diagnosis and treatment. Diagnostic tools in the past were very limited. So he questions how many people have been misdiagnosed based on symptoms that outwardly present as Parkinsons. Because of genetic variability, there were probably a lot of syndromes that we didnt quite recognize that included what looked exactly like Parkinsons disease and responded to therapy like Parkinsons disease, says Dr. Stern.
Recommended Reading: What’s New In Parkinson’s
Apda Centers For Advanced Research Received $800000 In Funding In 2021
The Centers support large research programs which include research trainees, fellowship programs, early-stage discovery programs, and later stage clinical translation. These Centers facilitate research at the forefront of investigations into the causes, treatments, and finding the cure for Parkinsons disease.
Early Detection Of Parkinsons Disease
Parkinsons disease affects about 1% of the population, primarily people in their late 50s and 60s. It is marked by tremor, slowness of movement, and muscle rigidity. Additional symptoms include gait and balance difficulties, speech issues, and bowel and bladder problems.
Dr. Stern noted how far the treatment of Parkinsons disease has come since he first started working in the field. The good news is were very effective now at being able to treat many of the symptoms of Parkinsons disease, and patients can live very long, productive lives with the right kind of therapy, he says.
Current research is paving the way for the early detection of Parkinsons disease. When researchers identify biomarkers, doctors will be able to detect and diagnose Parkinsons earlier. Biomarkers are specific signs that indicate the presence of a disease early on. Early detection can lead to earlier, more effective treatments. It may even become possible to prevent or slow the onset of symptoms.
What Im very excited about is this whole notion of biomarkers that may enable us to make the diagnosis of Parkinsons disease at a time when its not disablingin fact, at a time when there may be no symptoms at alland then intervene when we can make much more of a difference, Dr. Stern says.
Don’t Miss: Can Medications Cause Parkinson’s Disease
What Is The Prognosis
The average life expectancy of a person with PD is generally the same as for people who do not have the disease. Fortunately, there are many treatment options available for people with PD. However, in the late stages, PD may no longer respond to medications and can become associated with serious complications such as choking, pneumonia, and falls.
PD is a slowly progressive disorder. It is not possible to predict what course the disease will take for an individual person.
One commonly used scale neurologists use for describing how the symptoms of PD have progressed in a patient is the Hoehn and Yahr scale.
What Are The Symptoms Of The Disease
The four primary symptoms of PD are:
- Tremor. Tremor often begins in a hand, although sometimes a foot or the jaw is affected first. The tremor associated with PD has a characteristic rhythmic back-and-forth motion that may involve the thumb and forefinger and appear as a pill rolling. It is most obvious when the hand is at rest or when a person is under stress. This tremor usually disappears during sleep or improves with a purposeful, intended movement.
- Rigidity. Rigidity , or a resistance to movement, affects most people with PD. The muscles remain constantly tense and contracted so that the person aches or feels stiff. The rigidity becomes obvious when another person tries to move the individuals arm, which will move only in ratchet-like or short, jerky movements known as cogwheel rigidity.
- Bradykinesia. This slowing down of spontaneous and automatic movement is particularly frustrating because it may make simple tasks difficult. The person cannot rapidly perform routine movements. Activities once performed quickly and easilysuch as washing or dressingmay take much longer. There is often a decrease in facial expressions.
- Postural instability. Impaired balance and changes in posture can increase the risk of falls.
Also Check: Does Weather Affect Parkinson’s Disease
What Causes Parkinsons Disease
The most prominent signs and symptoms of Parkinsons disease occur when nerve cells in the basal ganglia, an area of the brain that controls movement, become impaired and/or die. Normally, these nerve cells, or neurons, produce an important brain chemical known as dopamine. When the neurons die or become impaired, they produce less dopamine, which causes the movement problems associated with the disease. Scientists still do not know what causes the neurons to die.
People with Parkinsons disease also lose the nerve endings that produce norepinephrine, the main chemical messenger of the sympathetic nervous system, which controls many functions of the body, such as heart rate and blood pressure. The loss of norepinephrine might help explain some of the non-movement features of Parkinsons, such as fatigue, irregular blood pressure, decreased movement of food through the digestive tract, and sudden drop in blood pressure when a person stands up from a sitting or lying position.
Many brain cells of people with Parkinsons disease contain Lewy bodies, unusual clumps of the protein alpha-synuclein. Scientists are trying to better understand the normal and abnormal functions of alpha-synuclein and its relationship to genetic mutations that impact Parkinsons andLewy body dementia.
Article Of The Year 2021
Staging Parkinsons Disease Combining Motor and Nonmotor Symptoms Correlates with Disability and Quality of Life
Journal profile
Parkinsons Disease publishes research related to the epidemiology, etiology, pathogenesis, genetics, cellular, molecular and neurophysiology, as well as the diagnosis and treatment of Parkinsons disease.
Editor spotlight
Chief Editor Dr Cristine Alves da Costa is based at Centre National de la Research Scientifique, France. Her research is focuses on Parkinsons molecular and cell biology.
Special Issues
Read Also: How Is Huntington’s Chorea Similar To Parkinson’s Disease
A New Era For Parkinsons Disease Treatment
March 2, 2022 | By
A non-invasive ultrasound treatment for Parkinsons disease that was tested in a pivotal trial led by University of Maryland School of Medicine researchers is now broadly available at the University of Maryland Medical Center .
Howard Eisenberg, MD, Dheeraj Gandhi, MD, MBBS, Paul Fishman, MD, PhD, Bert W. OMalley, MD.
The device, called Exablate Neuro, was approved in November by the U.S. Food and Drug Administration to treat advanced Parkinsons disease on one side of the brain. The approval was based on findings from the UMSOM clinical trial and effectively expands access to focused ultrasound beyond clinical trial participation.
Rapid Reversal of Symptoms
Focused ultrasound is an incisionless procedure, performed without the need for anesthesia or an in-patient stay in the hospital. Patients, who are fully alert, lie in a magnetic resonance imaging scanner, wearing a transducer helmet. Ultrasonic energy is targeted through the skull to the globus pallidus, a structure deep in the brain that helps control regular voluntary movement. MRI images provide doctors with a real-time temperature map of the area being treated. During the procedure, the patient is awake and providing feedback, which allows doctors to monitor the immediate effects of the tissue ablation and make adjustments as needed.
Patient: Focused Ultrasound Changed My Life
A New Era for Parkinsons Disease Treatment
Stay Current On Parkinsons News In Canada
With your support, you inspire the kind of action that will make a profound difference in the well-being of Canadians living with Parkinsons. Together, we will continue the global quest for a cure and create a world without Parkinsons.
Charitable Registration Number: 10809 1786 RR0001
Do you have questions about Parkinson’s?
From coast to coast to coast, we acknowledge the ancestral and unceded territories of Inuit, Métis, and First Nations Peoples.
Also Check: How To Prevent Getting Parkinson’s Disease
What Causes The Disease
The precise cause of PD is unknown, although some cases of PD are hereditary and can be traced to specific genetic mutations. Most cases are sporadicthat is, the disease does not typically run in families. It is thought that PD likely results from a combination of genetics and exposure to one or more unknown environmental factors that trigger the disease.
The protein alpha-synuclein. The affected brain cells of people with PD contain Lewy bodiesdeposits of the protein alpha-synuclein. Researchers do not yet know why Lewy bodies form or what role they play in the disease. Some research suggests that the cells protein disposal system may fail in people with PD, causing proteins to build up to harmful levels and trigger cell death. Additional studies have found evidence that clumps of protein that develop inside brain cells of people with PD may contribute to the death of neurons.
Genetics. Several genetic mutations are associated with PD, including the alpha-synuclein gene, and many more genes have been tentatively linked to the disorder. The same genes and proteins that are altered in inherited cases may also be altered in sporadic cases by environmental toxins or other factors.
Environment. Exposure to certain toxins has caused parkinsonian symptoms in rare circumstances . Other still-unidentified environmental factors may also cause PD in genetically susceptible individuals.
What Genes Are Linked To Parkinsons Disease
Several genes have been definitively linked to PD:
- SNCA. This gene, which makes the protein alpha-synuclein, was the first gene identified to be associated with Parkinsons. Research findings by the National Institutes of Health and other institutions prompted studies of the role of alpha-synuclein in PD, which led to the discovery that Lewy bodies seen in all cases of PD contain clumps of alpha-synuclein. This discovery revealed the link between hereditary and sporadic forms of the disease.
- LRRK2. Mutations in LRRK2 were originally identified in several English and Basque families as a cause of a late-onset PD. Subsequent studies have identified mutations of this gene in other families with PD as well as in a small percentage of people with apparently sporadic PD. LRRK2 mutations are a major cause of PD in North Africa and the Middle East.
- DJ-1. This gene normally helps regulate gene activity and protect cells from oxidative stress and can cause rare, early forms of PD.
- PRKN . The parkin gene is translated into a protein that normally helps cells break down and recycle proteins.
- PINK1. PINK1 codes for a protein active in mitochondria. Mutations in this gene appear to increase susceptibility to cellular stress. PINK1 has been linked to early forms of PD.
- GBA . Mutations in GBA cause Gaucher disease , but different changes in this gene are associated with an increased risk for Parkinsons disease as well.
Read Also: Parkinson’s Caused By Herbicide
Selected Scientific Articles By Our Researchers
Synergy of pandemics-social isolation is associated with worsened Parkinson severity and quality of life. Subramanian I, Farahnik J, Mischley LK. Social isolation was associated with greater patient-reported PD severity and lower quality of life, although it is unclear whether this is the cause or a consequence of the disease. NPJ Parkinsons Dis. 2020 Oct 8 6:28.
REM sleep behavior disorder in Parkinsons disease: effects on cognitive, psychiatric, and functional outcomes. Mahmood Z, Van Patten R, Nakhia MZ Twamley EW, Filoteo JV, Schiehser DM. Disordered sleep is linked to poorer mental function in patients with PD. J Int Neuropsychol Soc. 2020 Oct 26:894-905.
Characterizing dysbiosis of gut microbiome in PD: evidence for overabundance of opportunistic pathogens. Wallen ZD, Appah M, Dean MN, Sesler CL, Factor SA, Molho E, Zabetian CP, Standaert DG, Payami H. There is a significant overabundance of a cluster of opportunistic pathogens in the guts of persons with PD. NPJ Parkinsons Dis. 2020 Jun 12 6:11.
Intestinal Transit In Early Moderate Parkinsons Disease Correlates With Probable Rbd: Subclinical Esophageal Dysmotility Does Not Correlate
Background. Nonmotor symptoms, including constipation and dysphagia, are very common in Parkinsons disease and Lewy pathology is widespread in the gastrointestinal tract, particularly in the lower esophagus. Constipation and REM sleep behavior disorder may present prior to clinical diagnosis. Yet, little is known about esophageal dysfunction and its connection to constipation in early PD. Objective. This study aimed to investigate esophageal and colonic transit in early moderate PD and to study correlations between symptoms and objective measures. Methods. Thirty early moderate PD patients and 28 healthy controls were included in this cross-sectional study. Esophageal transit times were determined by esophageal scintigraphy and colonic transit times by CT after radio-opaque marker ingestion. Olfaction tests, clinical evaluation, and nonmotor questionnaires were also performed. Results. Distal esophageal transit times and colonic transit times were both significantly prolonged in the PD group compared to HC and a moderate-strong positive correlation was found between colonic transit time and RBDSQ score . Significant correlations were also found between CTT and SCOPA-AUT scores as well as between CTT and ROME III functional constipation scores. . Colonic transit correlates with probable RBD and is more severely prolonged in early moderate PD than is the distal esophageal transit time.
You May Like: What Can Cause Parkinson Like Symptoms

