Considering Gi And Non
GI symptoms have a significant influence on the quality of life of those living with Parkinsons, and can reduce the effectiveness of medications such as levodopa. As an example, drooling and difficulty swallowing can result in difficulty taking oral prescriptions. Similarly, gastroparesis can result in changes in response to levodopa treatment by affecting absorption of the drug into the blood stream, and, therefore, into the brain.20,29,39-41 The result of this can be more severe motor-fluctuations in patients, as is also seen in those with other GI conditions that can decrease levodopa absorption, such as small intestinal bacterial overgrowth, or infection with Helicobacter pylori.42 The significance of this is that through appropriate treatment of non-motor and GI symptoms of Parkinsons disease, there is potential for patients to also experience improvement in their response to treatment for motor-symptoms, for a broad improvement in quality of life.
Daniel Levy, PhD, Health Researcher & Writer
First published in the Inside Tract® newsletter issue 211 2019
We thank Maria Marano, Information and Referral Associate, and Julie Wysocki, Director, Research Program, with Parkinson Canada for reviewing this article.
Email News Sign Up
How Can I Help Myself
It is easy to become obsessed with bowel activity, but it is not necessary to have a bowel movement every day it can be quite normal for some people to empty their bowels only three or four times a week. What is important is that passing stools does not cause pain or unnecessary strain. Focus on what is normal and healthy for you and remember that bowel activity is affected by food and exercise, so will vary according to what you are eating and doing.
Remember that learning to manage your bowels will take time and patience, so dont expect to solve problems overnight. It may take a few weeks to adjust diet etc, so be patient. There are also plenty of ways you can help yourself.
The Importance Of Nonmotor Symptoms In Parkinson’s Disease
In the early 19th century , with the publication of An Essay on the Shaking Palsy , Dr. James Parkinson was the first to provide a clear clinical description of the disease that now bears his name . There are currently four motor features characterizing this neurological disorder, namely, muscle rigidity, tremor at rest, bradykinesia, and postural instability . However, a definitive diagnosis of Parkinson’s disease is difficult to establish and can be obtained only postmortem by the demonstration of the presence of Lewy bodies . Therefore, clinicians currently rely not only on motor symptoms manifestations but also on a positive response to levodopa treatment .
Progressive alterations of dopaminergic neurons in the nigrostriatal pathway are at the core of the abovementioned motor symptoms, resulting in a dysfunction of the somatomotor system. The extent of dopamine loss in the substantia nigra is already about 5070% when the first motor symptoms emerge, and although PD is a progressive neurological disorder, DAergic deterioration is usually very slow and varies from one person to another . An early diagnosis of the disease based on the Unified Parkinson’s Disease Rating Scale has a favorable long-term impact on the quality of life of patients .
Read Also: Can Parkinson’s Disease Be Prevented
Parkinsons Disease Is A Neurodegenerative Condition
Parkinsons disease is a chronic condition in which neurons within a region of the brain responsible for the control of movement break down and die. These neuronal cells use a chemical called dopamine to communicate with each other. It is this complex dopamine-based communication between neurons that is responsible for control of movement. Death of these neurons is referred to as dopaminergic neurodegeneration, and directly leads to the movement-related symptoms of the condition . These include tremors, changes in posture, stiffness, and a slowness of movement, also referred to as bradykinesia.1,2
Importantly, and often little appreciated, is the fact that Parkinsons disease can also affect neurons outside of the brain. Neuronal connections are made throughout the body, and connect all parts of the body to the brain and spinal cord, including to the GI tract. In particular, Parkinsons interferes with normal communication between the central nervous system, and the esophagus and stomach.3 Parkinsons can also affect the enteric nervous system, a network of neurons that functions with a considerable level of independence from the brain and central nervous system, and that is highly involved in controlling the intestinal tract and digestion.3,4 By affecting both the central and enteric nervous systems, Parkinsons disease may give rise to an array of GI symptoms.
What Causes Parkinsons Disease
The most prominent signs and symptoms of Parkinsons disease occur when nerve cells in the basal ganglia, an area of the brain that controls movement, become impaired and/or die. Normally, these nerve cells, or neurons, produce an important brain chemical known as dopamine. When the neurons die or become impaired, they produce less dopamine, which causes the movement problems associated with the disease. Scientists still do not know what causes the neurons to die.
People with Parkinsons disease also lose the nerve endings that produce norepinephrine, the main chemical messenger of the sympathetic nervous system, which controls many functions of the body, such as heart rate and blood pressure. The loss of norepinephrine might help explain some of the non-movement features of Parkinsons, such as fatigue, irregular blood pressure, decreased movement of food through the digestive tract, and sudden drop in blood pressure when a person stands up from a sitting or lying position.
Many brain cells of people with Parkinsons disease contain Lewy bodies, unusual clumps of the protein alpha-synuclein. Scientists are trying to better understand the normal and abnormal functions of alpha-synuclein and its relationship to genetic mutations that impact Parkinsons andLewy body dementia.
Recommended Reading: Restless Legs Parkinson’s Treatment
Nausea Vomiting And Gastroparesis
Nausea and vomiting are related, most of the time, to antiparkinsonian medications for motor symptoms, rather than occurring as intrinsic features of PD . Indeed, these side effects generally appear following the initiation of DAergic treatments . However, nausea may likely occur in untreated parkinsonian patients as well, and such cases might be explained by underlying gastroparesis . Also known as delayed gastric emptying, gastroparesis corresponds to decreased stomach motility, which may eventually affect gut transit. In addition to nausea, chronic gastroparesis is characterized by early satiety, a sensation of fullness, weight loss, and abdominal pain and bloating . This phenomenon could well be related to the degeneration of autonomic neurons in the myenteric plexus and brainstem . Moreover, intestinal absorption of L-DOPA and other medications might be slowed by such protracted gastric retention, thus reducing the effectiveness of treatment and preventing the improvement of motor symptoms . PD-associated gastroparesis deserves proper medical attention as its observed prevalence approaches 90% of patients .
Recommended Reading: Does Vitamin B12 Help Parkinsons
Background: The Stomach Parkinson’s And Levodopa
Levodopa is not absorbed from the stomach, but the stomach plays an important role in controlling how levodopa reaches the parts of the small intestine where it is absorbed. Some medicines, including dopamine agonists and anticholinergics, can also delay gastric emptying, as can severe stomach acidity, although over-treatment of this problem can also prevent the break-down of levodopa tablets, leading to incomplete absorption.
Unfortunately, gastric emptying can be delayed by Parkinsons itself or by constipation caused by the colon-gastric reflex. Levodopa tablets may remain in the stomach for a long time, leading to delayed absorption in the small intestine and a delayed response to the treatment.
An enzyme called dopa-decarboxylase that is present in the stomach lining can convert levodopa trapped in the stomach into dopamine, making it unavailable to the central nervous system. Also, dopamine formed in the stomach may stimulate gastric dopamine receptors, leading to stomach relaxation and reduced gastric motility, and this can worsen the problem.
Liquid levodopa may improve motor fluctuations by ensuring better absorption than standard preparations, especially when taken after meals. Subcutaneous infusion of the dopamine agonist apomorphine is effective in controlling motor fluctuations by bypassing the gastrointestinal tract.
Content last reviewed: January 2020
Read Also: How To Handle Parkinson Patient
Exercise For Constipation In Parkinsons Disease
Be guided by your doctor, but general suggestions include:
- Talk with your doctor, physiotherapist, exercise physiologist or healthcare professional when planning your exercise program.
- Aim for at least 30 minutes of exercise every day.
- Spend a few minutes warming up and cooling down. This could include marching in place or stretching.
- Start with the easiest exercises first. Slowly introduce the more difficult exercises as your fitness increases.
- Only exercise when other people are at home who can help if necessary.
- Remember: too little exercise and fluid intake with an increase in dietary fibre can worsen constipation for some people.
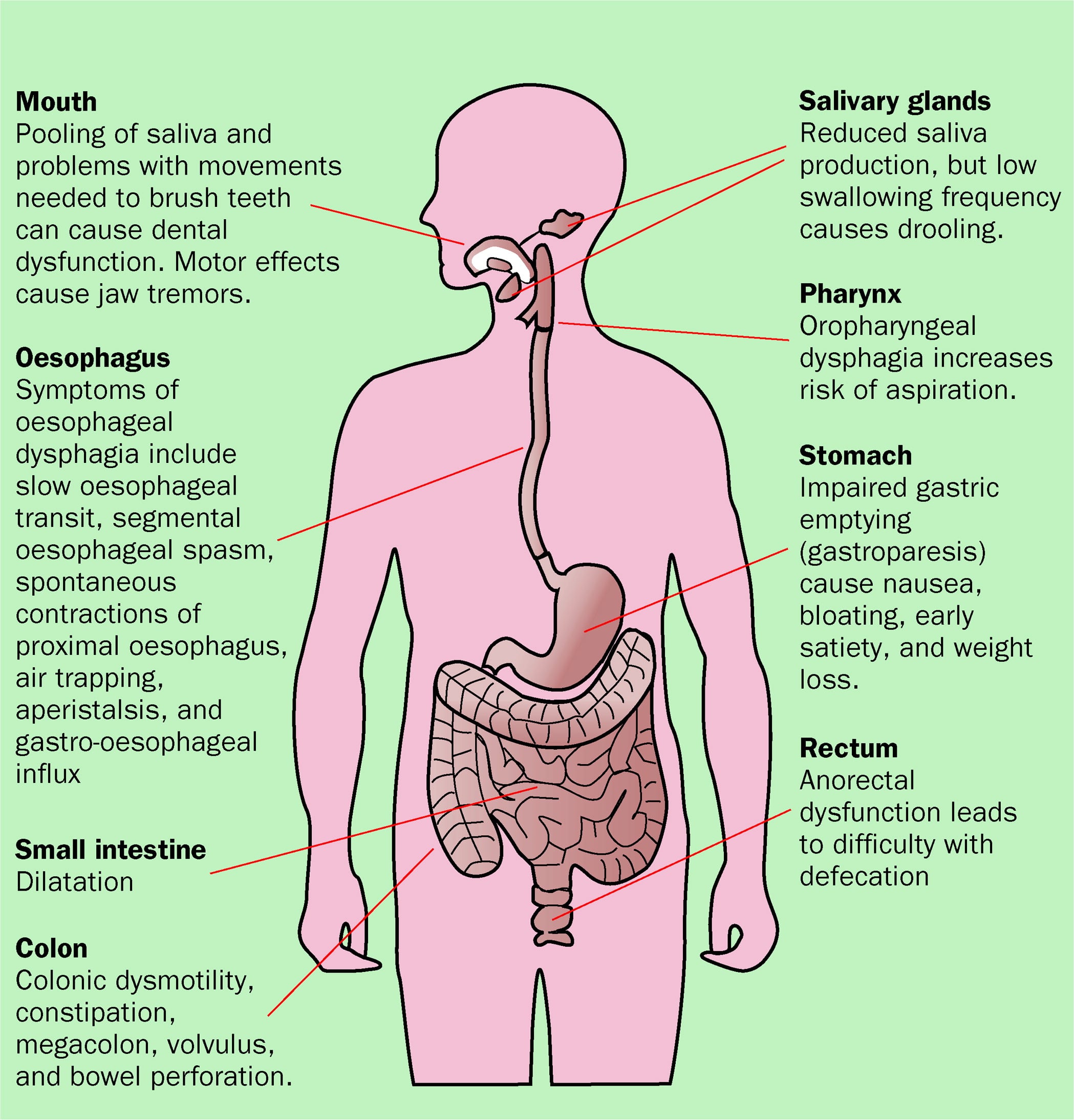
Parkinsons Disease And The Gut
Parkinsons disease is primarily a neurological condition however, symptoms also manifest outside of the brain itself, including within the gut . This article aims to provide a simple background to Parkinsons disease, and some insights into how these GI symptoms may arise and how we can treat them. Increased awareness of these often-overlooked GI issues in Parkinsons might lead to better understanding of the condition by researchers, as well as improved treatment and quality of life for patients.
Also Check: Tests To Confirm Parkinson’s Disease
Are There Medicines To Treat Dlb
Though there is no cure for DLB yet, there are medications that help manage the symptoms. These medications are called cholinesterase inhibitors, and they can help if a person with DLB is having memory problems. Some examples of these medicines are donepezil, rivastigmine and galantamine. If a person with DLB has movement symptoms they may be treated with medications used for Parkinsons disease, such as levodopa. Sleep problems may be managed by sleep medications including melatonin.
Because people with DLB are usually very sensitive to medications, any new medication, even one that is not being used for the brain, needs to be reviewed with the persons provider to avoid potential contraindication.
What Is Parkinsons Disease
Parkinsons disease is the second most common neurodegenerative disorder and the most common movement disorder. Characteristics of Parkinsons disease are progressive loss of muscle control, which leads to trembling of the limbs and head while at rest, stiffness, slowness, and impaired balance. As symptoms worsen, it may become difficult to walk, talk, and complete simple tasks.
The progression of Parkinsons disease and the degree of impairment vary from person to person. Many people with Parkinsons disease live long productive lives, whereas others become disabled much more quickly. Complications of Parkinsons such as falling-related injuries or pneumonia. However, studies of patent populations with and without Parkinsons Disease suggest the life expectancy for people with the disease is about the same as the general population.
Most people who develop Parkinsons disease are 60 years of age or older. Since overall life expectancy is rising, the number of individuals with Parkinsons disease will increase in the future. Adult-onset Parkinsons disease is most common, but early-onset Parkinsons disease , and juvenile-onset Parkinsons disease can occur.
You May Like: Are There Different Stages Of Parkinson’s Disease
Constipation And Parkinsons Disease
Constipation is one of the most commonly reported GI symptoms of Parkinsons disease, affecting 60-80% of patients.17,18 Constipation occurs when movement of material through the GI system slows down. This slowing can result from the direct effects of Parkinsons disease upon the action of intestinal muscles that would normally act to massage material through the intestines in a wave-like action , or indirectly through side-effects of some medications.19 In severe cases, accounting for approximately 7% of those with a parkinsonism, compromised peristalsis can lead to complete gut blockage resulting in further symptoms such as cramping, abdominal pain, vomiting, and bloating.16
What Examinations May I Need To Have
Your GP or specialist will probably ask a series of questions to find out what the problem is. These may include:
- When did the trouble start?
- How often does it happen?
- Can you feel when your bladder or bowel is full?
- Are you having difficulty emptying your bladder or bowel?
- How often are you using the toilet?
Parkinson’s symptoms, such as slowness of movement and rigid muscles, affect the muscles in the bowel wall. This can make it harder to push stools out of the body. You may be asked to keep a chart for several days of how often you use the toilet and how much you drink.
You may also be asked for a urine sample to test for infection and they will normally carry out a physical examination.
Bladder or bowel problems can be complex in Parkinson’s, so sometimes specialist tests or X-rays may be needed. All of these can usually be done in an outpatient department or clinic.
Don’t Miss: Parkinson’s Vs Alzheimer’s Disease
Treatment For Constipation In Parkinsons Disease
Your doctor may suggest various treatments to help combat constipation, including:
- dietary changes, including more fibre rather than refined or highly processed foods, and water
- avoidance of unnecessary medicines that contain substances known to cause constipation
- laxatives, particularly agents that bulk and lubricate the stools
- treatment for any other medical problem that may be contributing to your constipation, such as haemorrhoids .
Take Control Of Your Parkinsons Treatment
OurEvery Victory Counts® manual gives people living with Parkinsons, their care partners and their family members the tools they need to take control of their own Parkinsons treatment through a proactive approach to self-care.
a powerful new print edition
Its jam-packed with up-to-date information about everything Parkinsons, plus an expanded worksheets and resources section to help you put what youve learned into action. Color coding and engaging graphics help guide you through the written material and point you to complementary videos, podcasts and other materials on the Every Victory Counts companion website. And, it is still free of charge thanks to the generosity of our sponsors.
Request your copy of the new Every Victory Counts manual by clicking the button below.
Read Also: Is There Pain Associated With Parkinson’s Disease
Person With Parkinsons Glenda Kahlor 66 Lives In Georgia Usa With Her Family She Was Diagnosed With Parkinsons In 1993 At The Age Of 40
Glenda Kahlor
How did you come to be diagnosed with Parkinsons?
I fell frequently, and felt vibrations in my arm. When I had a massage, the masseuse said my muscles did not feel right and urged me to go to see a doctor. I saw several doctors, and was finally diagnosed with young-onset Parkinsons at the age of 40. Then, around three years ago, it was decided I cannot longer safely live by myself. So, I moved from rural Oklahoma, USA, to live with my daughter, son-in-law, and three teenage grandchildren in the suburbs of Atlanta, Georgia. I miss my home in the country but I love it here too.
Were you told bowel issues can affect people with Parkinsons when you were diagnosed?
In the early years, I dont recall ever having a doctor tell me that Parkinsons patients often have bowel problems.
How have you been affected by bowel issues?
My first major problems occurred in 2000. I had an intestinal blockage, and spent a week in the hospital. Severe constipation has been a problem for me a number of times.
Between the years 2000 and 2016 I was hospitalised or treated for bowel problems multiple times. Since 2016 when I moved to live with my daughter and family I have not been hospitalised. I attribute this improvement in my health to a better diet, and more exercise.
Since 2016 when I moved to live with my daughter and family I have not been hospitalised. I attribute this improvement in my health to a better diet, and more exercise
Fecal Incontinence In Advanced Parkinsons Disease
Fecal incontinence is a very debilitating symptom that can occur in advanced PD and refers to the involuntary release of fecal matter.
Once again, fecal incontinence, especially if it is a new symptom, should be fully evaluated to determine if there is a cause unrelated to PD. Diseases of the gut such as inflammatory bowel disease or compression of the lower spine cord can be the reason.
If related to PD, there are typically two situations to consider. One possibility is that severe constipation with impacted bowel movement allows loose stool from higher up in the gastrointestinal tract to escape around the edges of the obstruction. In this situation, fecal incontinence could be a harbinger of bowel obstruction. Aggressive and continuous treatment of constipation can help avoid this potential scenario.
As with urinary incontinence, frequent and rapid exchange of dirtied incontinence products can keep skin intact and prevent infection.
Tips and Takeaways
Read Also: Alzheimer’s Disease And Parkinson’s Disease
The Gastrointestinal Effects Of Parkinson’s Disease
Surveys show that between 20% and 40% of people with Parkinson’s disease suffer from serious constipation . Larger numbers of people with PD have related gastrointestinal issues such as bloating, a feeling of fullness and nausea. As the disease progresses, all of these GI problems become more common. In rare cases, serious complicationssuch as megacolon and perforation or tearing of the colonmay arise from these GI problems.
The connection between the two may seem odd on the surface, but research shines some light on these unpleasant consequences of the disease.
A large survey of healthy people who were followed over several years revealed that men who reported having less than one bowel movement daily had a 2 to 7 times higher risk of developing PD than that of men who had daily bowel movements their risk was four times higher than that of men who had two or more bowel movements a day.
Dietary Fibre For Constipation In Parkinsons Disease
Be guided by your doctor, but general suggestions include:
- Choose easy-to-eat fibrous foods such as soft fruits. Consider mashing or pureeing fruits to make them easier to eat. Make sure to include the skin, where most of the fibre is found.
- Eat at least two pieces of fruit and five serves of vegetables every day.
- Eat homemade vegetable soups.
- Sprinkle a tablespoon of bran, psyllium husks or chia seeds on your breakfast cereal or add the bran to baked products such as cakes. However, avoid bran if you have swallowing problems.
- Fibre supplements may be helpful, but you must drink enough fluids for these to work properly. Avoid fibre supplements if you have problems swallowing.
- Dont increase dietary fibre too quickly or youll risk bloating and abdominal cramps. If discomfort occurs, cut back your fibre intake, increase your fluid intake, apply a hot water bottle to your abdomen and see your doctor.
Don’t Miss: Can Parkinson’s Cause Death
