What Is The Best Way To Communicate With A Person With Pdd
PD-related mood and motor changes can impact communication cognitive changes and Parkinsons disease dementia can further these difficulties.
- It is not usually helpful to try to reason or argue with someone experiencing a hallucination or delusion. Stay calm and be patient. If the person is frightened by the hallucination or delusion, try to redirect their attention to something else.
- You may find acknowledging what the person is seeing, even if you do not see it, can reduce stress.
- Speak slowly and at eye level. Communicate in simple sentences.
- Ask one question at a time and wait for an answer.
- Limit distractions. Turn off the TV or radio before asking a person with PDD to do something.
- Consider causes behind disruptive behavior: the person may be hungry, thirsty, tired, in pain, frustrated, lonely or bored.
- If the person is stuck on an idea, try agreeing with them, then changing the subject.
- Its OK to use humor to diffuse stressful situations but avoid negative humor or sarcasm these can be misunderstood.
Page reviewed by Dr. Jori Fleisher, MSCE, Assistant Professor, Department of Neurological Sciences at Rush University Medical Center, a Parkinsons Foundation Center of Excellence.
How Is Parkinsons Disease Dementia Diagnosed
No single test can diagnose Parkinsons disease dementia. Instead, doctors rely on a series or combination of tests and indicators.
Your neurologist will likely diagnose you with Parkinsons and then track your progression. They may monitor you for signs of dementia. As you get older, your risk for Parkinsons dementia increases.
Your doctor is more likely to conduct regular testing to monitor your cognitive functions, memory recall, and mental health.
Alzheimers Products & Market Analysis
some products are available in the market to control alzheimers disease.These Products are Color Cards Activity , Color-Coded Therapy are designed to stimulate the mind and sense. Alzheimers games and puzzles and eating dishes are available in the market for brain activity. Treatment with drug, non drug or medication and surgery sometimes shows side effetcs.But these alzheimers products may show a good results to cure memory loss.
Related Journals of Alzheimers Products & Market Analysis
Also Check: Can Parkinson’s Run In The Family
Symptoms Related To Brain Function Are Different
There is some overlap, but in general, the overall cognitive symptoms that people experience with Parkinsons disease dementia and Alzheimers are different. Alzheimers mainly affects language and memory at the outset, whereas Parkinsons affects problem-solving, speed of thinking, memory, and mood.6
Unlike in Alzheimers disease, people with Parkinsons-related dementia often experience hallucinations, delusions, and paranoid thoughts. Both conditions can lead to depression, anxiety, and sleep disturbances.4,6
How Is Parkinsons Dementia Different From Alzheimers Disease
The advanced cognitive changes that impact daily living in Alzheimers and Parkinsons disease are both types of dementia.
Parkinsons disease dementia can occur as Parkinsons advances, after several years of motor symptoms. Dementia with Lewy Bodies is diagnosed when cognitive decline happens first, or when Parkinsons motor symptoms and cognitive decline occur and progress closely together. Cognitive impairments in PDD, combined with the movement symptoms of the disease, produce a greater impact on social and occupational functioning than Alzheimers.
Alzheimers, a fatal brain disease, causes declines in memory, thinking and reasoning skills. Physicians can diagnose Alzheimers. Visit the Alzheimers Association to learn the 10 signs Alzheimers disease.
Fortunately for people with PD, Parkinsons disease dementia is less disabling than Alzheimers disease. People with Alzheimers have language difficulties earlier than people with Parkinsons, and no new memories are formed. People with PD also have more ability to compensate and adjust based on cues.
Recommended Reading: Parkinson’s Disease Life Expectancy
How Can We Support The Sleep/wake Cycle Of Pdd
For people with PDD who are confused about the day-night cycle, some daily strategies can be helpful. At night, starting a lights out routine that happens at the same hour every day, where all curtains are closed and lights are turned off, can help the person understand that it is sleep time. During the day, opening the curtains, allowing the person with PDD to spend as much time in the daylight as possible, avoiding naps, and organizing stimulating activities, can be helpful. Having lots of calendars and clocks in every room might also help a person with PDD be less confused about the time of day.
Support Groups For Parkinsons With Or Without Dementia
Parkinsons disease is tough to live with, both for the person affected and their family. Support groups are filled with people who are going through very similar experiences. Theyre a great place to safely vent frustrations, get new ideas for how to cope or solve problems, and learn about helpful resources.
Check with these organizations to find a support group in your area:
Read Also: Parkinson Awareness Ribbon Color
What Is Needed For A Parkinson’s Disease Dementia Diagnosis
There is no definitive medical test that confirms cognitive decline or dementia in Parkinson’s disease. The most accurate way to measure cognitive decline is through neuropsychological testing.
- The testing involves answering questions and performing tasks that have been carefully designed for this purpose. It is carried out by a specialist in this kind of testing.
- Neuropsychological testing addresses the individual’s appearance, mood, anxiety level, and experience of delusions or hallucinations.
- It assesses cognitive abilities such as memory, attention, orientation to time and place, use of language, and abilities to carry out various tasks and follow instructions.
- Reasoning, abstract thinking, and problem solving are tested.
- Neuropsychological testing gives a more accurate diagnosis of the problems and thus can help in treatment planning.
- The tests are repeated periodically to see how well treatment is working and check for new problems.
Imaging studies: Generally, brain scans such as CT scan and MRI are of little use in diagnosing dementia in people with Parkinson’s disease. Positron emission tomographic scan may help distinguish dementia from depression and similar conditions in Parkinson’s disease.
Parkinsons Disease Dementia Vs Lewy Body Dementia
Lewy body dementia is typically when:
- Dementia symptoms appear within 1 year after movement symptoms
- Both dementia symptoms and movement symptoms are present at the time of diagnosis
- Movement symptoms develop within a year of a Lewy body dementia diagnosis
Many experts now believe that Parkinsons disease dementia and dementia with Lewy bodies are caused by the same problems with brain processing of a specific protein . But they still recommend diagnosing dementia with Lewy bodies and Parkinsons dementia as separate diseases.
Read Also: What Is The Life Expectancy Of Someone With Parkinson’s Disease
Coping With A Parkinsons Diagnosis
A diagnosis of Parkinsons can be a frightening experience for both you and your loved ones. While there is currently no cure, there are treatments available for Parkinsons symptoms and lifestyle changes you can make to slow the progression of the disease and delay the onset of more debilitating symptoms, including Parkinsons disease dementia. Early diagnosis can prolong independence and help you to live life fully for much longer.
If youve been diagnosed with Parkinsons you may feel anger, deep sadness, or fear about what the future will bring. These feelings are all normal. Its also normal to grieve as you deal with this enormous adjustment.
Give yourself some time to adjust. As with any major change in life, dont expect that you will smoothly snap into this new transition. You may feel alright for a while, and then suddenly feel stressed and overwhelmed again. Take time to adjust to this new transition.
Learn all you can about Parkinsons disease and Parkinsons disease dementia. Educating yourself and making important decisions early can help you feel more in control during this difficult time.
Reach out for support. Living with Parkinsons presents many challenges, but there is help available for this journey. The more you reach out to others and get support, the more youll be able to cope with symptoms while continuing to enrich and find meaning in your life.
What Are Pd Dementia Safety Concerns
Safety issues should be considered and monitored from the time of diagnosis. As PDD progresses, ensure that your loved one is not left alone.
- Evaluate driving privileges before safety is a concern. Your doctor can make a driving evaluation referral.
- Work out legal and financial issues and safeguard finances. People with dementia are at greater risk of falling victim to scams and fraud.
- Minimize prescription risks. Confirm with the doctor the medication names and doses of the person with PD. If the person is in dementias early stages and capable, fill up their weekly pill box together and monitor use.
- Medical alert systems can be critical in case your loved one falls or wanders outside of the home. Many types of systems are available, from bracelets and pendants to smart watches with fall detection and one-button connections to 911.
- Evaluate gun safety. If your loved one owns a firearm or has one in the home, consider speaking with their doctor about the subject and taking appropriate safety precautions.
Don’t Miss: Is Parkinson’s Disease Fatal
Advances In Alzheimers Therapy
Recent studies indicating that therappeutic drugs and gene therapy are advanced techniques to control alzheimers diseaseGenomics therapy is most recent advances in AD research, when the disease was first described. Researchers are looking for new therapy treatments for dementia. Currently, there is no cure for Alzheimer’s But these alzheimers products may show a good results to cure memory loss.
Related Journals of Advances in Alzheimers Therapy
Journal of Dementia & Mental health, Rehabilitation in Movement Disorders, Stress Alzheimers, Neuron, American Journal of Occupational Therapy, Journal of Alzheimer’s & Dementia, Journal of the Alzheimer’s Association, Journal of Alzheimer’s Disease, Alzheimer’s Research & Therapy, Journal of Alzheimer’s Disease and Other Dementias, International journal of Alzheimer’s Disease & associated disorders, International Journal of Alzheimers Disease, Advances in Alzheimer’s Disease, American Journal of Alzheimers Disease, Current Alzheimer Research.
Key Brain Changes Are Different
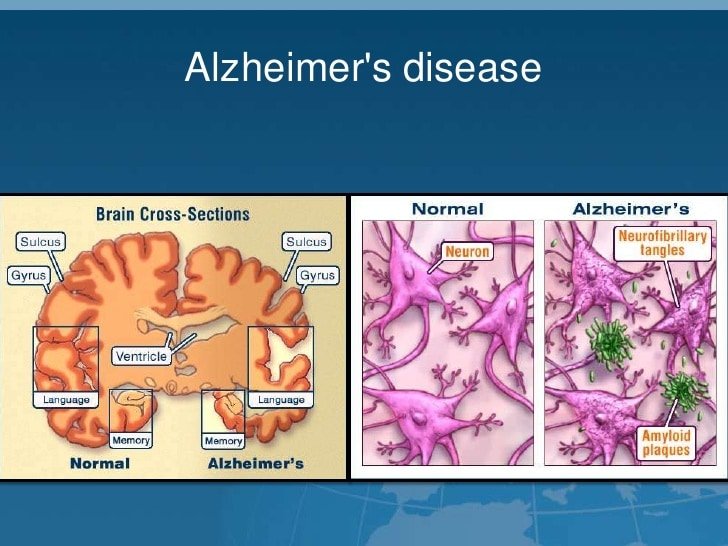
The key brain changes linked to Parkinsons disease and Parkinsons-related dementia are abnormal deposits of common brain proteins, called alpha-synuclein. These deposits are known as Lewy bodies, named after the doctor who discovered them. As more of these proteins clump in the brain, normal brain cells begin to die off.1
In Alzheimers disease, the key brain changes include the buildup of different brain proteins, called amyloid and tau. When amyloid proteins clump together, they form abnormal structures known as plaques. Abnormal groups of tau proteins form tangles.3 Over time, the buildup of these proteins causes normal brain cells to die, and affected parts of the brain may shrink.5
Read Also: What Is The Life Expectancy Of Someone With Parkinson’s Disease
What Are Parkinson’s Disease Dementia Medical Treatment And Medications
There is no specific therapy for dementia in Parkinson’s disease. Although cognitive symptoms initially may appear to respond to drugs that promote dopamine production, the improvement is mild and transient in contrast to the early responses to motor control improvement with medication in patients with Parkinson’s disease.
Parkinson’s disease dementia medications
Various medications are used to treat the movement disorders of Parkinson’s disease, some may exacerbate symptoms related to dementia.
- These include dopamine given in the form of levodopa medications known as dopamine agonists that act on the dopamine receptor and medications that slow down the metabolism of dopamine. They are often used in conjunction with monoamine oxidase inhibitors such as rasagiline. In addition, anticholinergic drugs are sometimes used.
- Unfortunately, these drugs may affect cognitive symptoms and mood disorders.
- The anticholinergic drugs, for example, help balance levels of dopamine and acetylcholine, another neurotransmitter, in the brain. These drugs can improve movement disorders but often make memory loss worse.
The dementia of Parkinson’s disease may respond to drugs used in patients with Alzheimer’s disease. However, these drugs, called cholinesterase inhibitors , lead to only small and temporary improvements in cognition.
Mood disorders and psychoses are usually treated with other medication.
How Parkinsons And Alzheimers Affect The Body And Brain Differently
Alzheimers and Parkinsons are both neurological illnesses. Both diseases are caused by damaged brain cells. Both conditions can involve dementia, as well as depression, anxiety, and sleep disturbances. Both conditions can lead to psychotic symptoms such as delusions and hallucinations.
While Alzheimers and Parkinsons share certain causes and effects, the two diseases are different. They impact the brain and progress in different ways. Both disorders affect people differently, manifest themselves differently, and progress at different rates.
I had a father with Parkinsons and a mother with dementia. My experience was that the Parkinsons progressed at a slower rate and was more motor-related than mental.
My father experienced tremors, as well as changes in his walking and facial expressions. But his cognitive ability was relatively intact up to the very last stages of the disease. My mothers dementia made her feeble and uncertain on her feet, but she remained active and mobile, even as her cognitive ability declined.
Don’t Miss: Final Stages Of Parkinson’s How Long
Statistical Analysis Of Clusters
Clinical data
Clinically observed differences between patient subgroups might be impaired by multiple confounding factors. To identify these confounders, we initially performed a stepwise multinomial logistic regression with the cluster indicator as response and several potential confounders as predictors. This approach was chosen to account for the fact that many clinical variables show a highly skewed distribution. Considered confounders included:
-
baseline diagnosis ,
-
coffee and alcohol consumption
-
ethnicity, including Spanish origin , and
-
prior neurological drug treatment , including L-DOPA for PD .
The Akaike Information Criterion was used for model selection, resulting in an optimal confounder set. It is worthwhile mentioning that none of the considered confounders demonstrated univariately significant association to cluster membership in any dataset according to a likelihood ratio test against the null model.
Brain imaging
Statistical analysis of features derived from MRI imaging in ADNI and DaTSCAN in PPMI in principle followed the same approach as those derived from for clinical data at baseline. The only difference was that for analysis of MRI imaging derive features we always used age and sex as confounders, and no further confounders were considered. Results of the statistical analysis are shown in Tables . For ADNI we used two types of imaging data:
Identification Of Common Molecular Mechanisms
Common molecular mechanisms between AD and PD were identified with the help of a systematic literature mining approach with post-hoc manual curation. More specifically, the text mining engine SCAIView was used to construct cause-effect relationships between molecules, pathways, biological processes and imaging features in both, AD and PD, see Domingo-Fernandez et al. and Kodamullil et al. for details, for details. After manual curation, two computable disease maps, one for AD and one PD were created. Finally, we have also made them interactively usable via a dedicated web application .
Calculation of the intersection of cause-effect relationships described in the AD and PD disease maps resulted into 27 genes grouped into 15 cause-effect relationship sub-graphs, called mechanisms from now on . While some of these mechanisms describe only posttranslational modifications of a single protein, others reflect more complex proteinprotein interactions and signaling cascades . Key proteins described in both diseases include e.g. APOE, TAU, SNCA and TOMM40. These proteins are involved into several known disease relevant processes that we have made computationally accessible via our earlier developed NeuroMMSig database.
We mapped 148 genetic variants measured in ADNI1, ADNI2/GO as well as PPMI to the 27 common AD/PD disease genes via a combination of two strategies: a) proximity and b) eQTL mapping, see details in Supplements on page 2.
Recommended Reading: Does Parkinson’s Cause Memory Issues
Parkinson’s Signs Linked To Alzheimer’s
Parkinson’s-like Symptoms Tied to Risk of Alzheimer’s Disease
April 22, 2003 — Older adults who rapidly develop the tremors and other classical symptoms of Parkinson’s disease may be up to eight times as likely to develop Alzheimer’s disease. A new study shows that the progression of symptoms traditionally associated with Parkinson’s disease, such as an irregular gait, muscle rigidity, tremors, and limited movement, are also linked to a decline in mental functioning and the development of Alzheimer’s disease.
Researchers say Parkinson’s disease-like symptoms are common in older people with and without Alzheimer’s disease, but the link between the progression or severity of these muscle-related symptoms and later development of Alzheimer’s disease has not been studied until now.
Their study, published in the April issue of The Archives of Neurology, tracked the progression of symptoms associated with Parkinson’s disease among 824 Catholic clergy members with an average age of 75 who had no signs of Alzheimer’s or Parkinson’s disease at the start of the study.
Researcher Robert Wilson, PhD, of Rush-Presbyterian-St. Luke’s Medical Center in Chicago, and colleagues, say the rate of progression of symptoms, especially worsening gait and rigidity, was also linked to scores on tests that measured mental function. As the person’s physical symptoms worsened, his or her mental functioning also declined, and more rapid physical decline was associated with more rapid mental decline.
Are There Medicines To Treat Pdd
Though there is no cure for PDD yet, there are medications that help manage the symptoms. These medications are called cholinesterase inhibitors, and they can help if a person with PDD is having memory problems. Some examples of these medicines are donepezil, rivastigmine and galantamine. Sleep problems may be managed by sleep medications such as melatonin.
Because people with PDD are usually very sensitive to medications, any new medication, even one that is not being used for the brain, needs to be reviewed with the persons provider to avoid potential contraindication.
Don’t Miss: Rso For Parkinson\’s
Association With Brain Imaging Derived Features In Ad And Pd
In ADNI, AD patients demonstrated highly significant pairwise differences when comparing 193 intracranial volume normalized subcortical brain structures of those patients which had a recent AD diagnosis at study baseline and correcting statistical differences for the confounding effects of age and sex. We found significant differences in several brain regions, such as the calcarine sulcus, the cuneus gyrus and the medial occipitotemporal gyrus .
Figure 5
Example of significant differences between clusters with respect to brain imaging derived features at study baseline/time of first disease diagnosis . left calcarine sulcus in AD patients left cuneus gyrus in AD patients volume of right medial occipitotemporal gyrus in AD patients DaTSCAN left Putamenratio to age expected value in healthy controls DaTSCAN Count Density Ratio: Caudate/Putamen DaTSCAN Count Density Ratio : Caudate contralateral/Putamen contralateral. The Figures shows statistical distributions as violin plots , and individual data points are shown as superimposed dots.
In PPMI, pairwise differences between the clusters were significant for in presynaptic dopaminergic imaging were identified in caudate and putamen . Also, the dopamine receptor density ratio of caudate versus putamen differed significantly between clusters.
Altogether, we concluded that our genetically derived clusters are associated with significant pathophysiological differences in the brain.
