Complications Related To Parkinson’s Can Affect Survival
Claudia Chaves, MD, is board-certified in cerebrovascular disease and neurology with a subspecialty certification in vascular neurology. She is an associate professor of neurology at Tufts Medical School and medical director of the Lahey Clinic Multiple Sclerosis Center in Lexington, Massachusetts.
Parkinson’s is a common neurodegenerative disease, and although it is not fatal, research suggests it may influence life expectancy.
A 2012 study in Archives of Neurology examined the six-year survival of nearly 140,000 Medicare beneficiaries with Parkinson’s disease in the United States. During the six-year period, 64% of the participants with Parkinson’s disease passed away.
The risk of death of those with Parkinson’s was then compared to Medicare beneficiaries who did not have Parkinson’s or any other common diseases, including:
When controlling for variables like age, race, and gender, the six-year risk of death among people with Parkinson’s was found to be nearly four times greater than those Medicare beneficiaries without the disease or other common diseases.
At the same time, the rate of death among those with Parkinson’s disease was similar to those with hip fracture, Alzheimer’s dementia, or a recent heart attackalthough it was higher than those who had been newly diagnosed with either colorectal cancer, stroke, ischemic heart disease, or chronic obstructive pulmonary disease.
Signs Of Parkinsons Disease
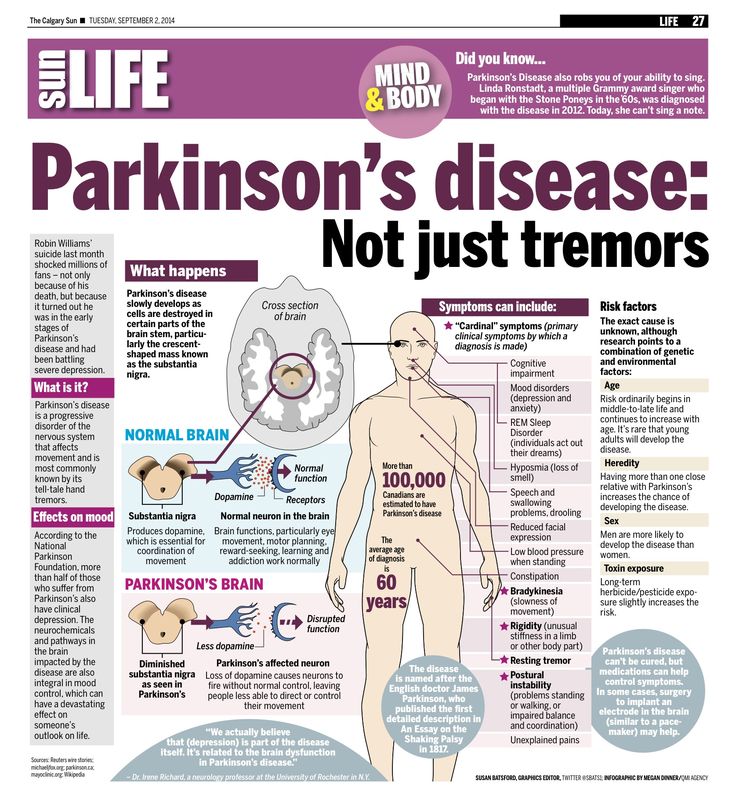
In 1817, Dr. James Parkinson published An Essay on the Shaking Palsy describing non-motor, as well as, motor symptoms of the illness that bears his name. Parkinsons is not just a movement disorder, explained Dr. Shprecher. Constipation, impaired sense of smell, and dream enactment can occur years before motor symptoms of Parkinsons. The latter, caused by a condition called REM sleep behavior disorder, is a very strong risk factor for both Parkinsons and dementia . This has prompted us to join a consortium of centers studying REM sleep behavior disorder.
What Makes Pd Hard To Predict
Parkinsonâs comes with two main buckets of possible symptoms. One affects your ability to move and leads to motor issues like tremors and rigid muscles. The other bucket has non-motor symptoms, like pain, loss of smell, and dementia.
You may not get all the symptoms. And you canât predict how bad theyâll be, or how fast theyâll get worse. One person may have slight tremors but severe dementia. Another might have major tremors but no issues with thinking or memory. And someone else may have severe symptoms all around.
On top of that, the drugs that treat Parkinsonâs work better for some people than others. All that adds up to a disease thatâs very hard to predict.
Don’t Miss: What Is Life Expectancy Of Parkinson’s Patients
What Causes Parkinson Disease
Parkinson disease arises from decreased dopamine production in the brain. The absence of dopamine makes it hard for the brain to coordinate muscle movements. Low dopamine also contributes to mood and cognitive problems later in the course of the disease. Experts don’t know what triggers the development of Parkinson disease most of the time. Early onset Parkinson disease is often inherited and is the result of certain gene defects.
Typical Timescale For Pdd
According to the Parkinsons Foundation, PDD is typically diagnosed when a person living with Parkinsons disease experiences cognitive decline after a year or more of motor symptoms. But in most cases, people experience many years of tremors, slowness of movement, and muscle cramps before showing signs of significant cognitive decline. The Weill Institute for Neurosciences estimates the average time from onset of movement problems to developing dementia is 10 years. An estimated 50% to 80% of people with Parkinsons will eventually experience Parkinsons disease dementia, says the Alzheimers Association.
Recommended Reading: Parkinson’s Dementia Prognosis
Coping With Cognitive Changes
Some medications used to treat Alzheimer’s disease also may be used to treat the cognitive symptoms of LBD. These drugs, called cholinesterase inhibitors, act on a chemical in the brain that is important for memory and thinking. They may also improve hallucinations, apathy, and delusions. The U.S. Food and Drug Administration has approved one Alzheimer’s drug, rivastigmine, to treat cognitive symptoms in Parkinson’s disease dementia. Several other drugs are being tested as possible treatments for LBD symptoms or to disrupt the underlying disease process.
Changes In Mood Emotions And Perceptions
Changes in mood remain in the later stages of dementia. Depression and apathy are particularly common.
Delusions and hallucinations are most common in the late stage of dementia. They are not always distressing but they can explain some changes in behaviour because the persons perception of reality is altered.
People with later stage dementia often respond more to senses than words. They may like listening to songs or enjoy textures. For example, they may like the feel of different types of material.
Don’t Miss: Can Boxing Cause Parkinson’s Disease
Treatment And Care For Lewy Body Dementia
While LBD currently cannot be prevented or cured, some symptoms may respond to treatment for a period of time. An LBD treatment plan may involve medications, physical and other types of therapy, and counseling. A plan to make any home safety updates and identify any equipment can make everyday tasks easier.
A skilled care team often can suggest ways to improve quality of life for both people with LBD and their caregivers.
How Can I Support Someone With Parkinson’s At The Advanced Or Palliative Stage
In the advanced stages of Parkinsons, your patients care needs may be more complex and require careful planning along with the patient, their family and other health and social care professionals involved.
Palliative care should be holistic, considering the whole person to support the personal, social, psychological and spiritual needs of your patient and their family. It should give your patient some control and choice over areas such as treatment options and where they will be cared for, as well as providing advice and support to all the people involved in their care.
Palliative care in Parkinsons may be supported by a number of professionals, including a Parkinsons nurse specialist, local hospice or specialist palliative care team, physiotherapist, occupational therapist, speech and language therapist or dietitian. Many people with Parkinson’s also find complementary therapies beneficial.
It is important that you find out whether the person has a care plan in place regarding their preferences for how the issues surrounding advanced Parkinsons should be managed. This could include legal documentation such as a Lasting Power of Attorney and an advance care plan. Advance care plans include information on what the persons wishes and preferences are for their care in the future. They may include decisions on any treatments the person doesnt want to have in the future this is called an Advance Directive, Advance Decision to Refuse Treatment or Living Will.
You May Like: What Is The Life Expectancy Of Someone With Parkinson’s Disease
How Long Does It Take For Parkinsons Disease To Progress
It is quite common for any individual suffering from Parkinsons disease to wonder about the unfolding of the condition. If you belong to the group that in search for the answers related to the progression of Parkinsons disease, then you will try to learn about the symptoms that you can acquire with the condition, when they start, and the changes the disease brings in the body.
The questions are basic, but Parkinsons disease is not. Like other illnesses, Parkinsons disease does not have a specific path of progression. Due to this, it is difficult to state or pin down the exact time or the path of the progression.
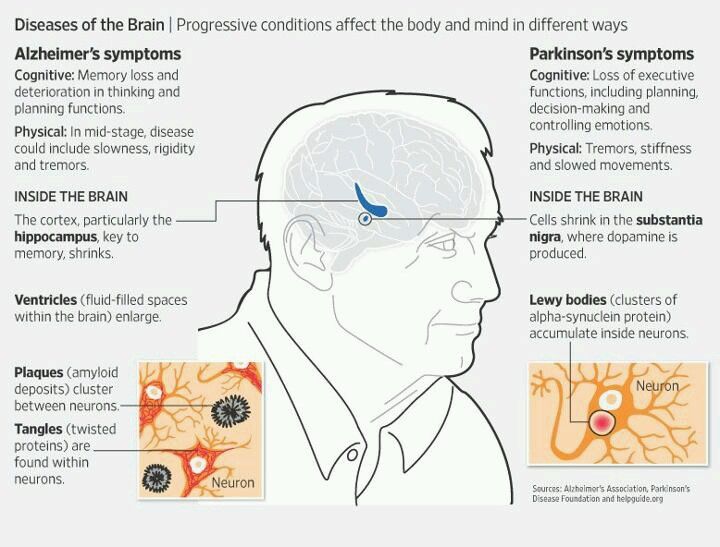
What Causes Parkinson Disease And Alzheimers
Parkinsons dementia is caused by impaired physical activities where the dopamine & serotonin gets damaged by the disease.
On the other hand, with Alzheimers, the two types of brain proteins tangles & plaques store up & kill the brain cells.
Moreover, the disease reduces learning capacity, comprehension & judgmental skills.
Well, distinguishing between the treatmentits necessary to determine the best treatment approach, though, Dr. Vivek Pratap Singhis known for the finestParkinsons disease treatment in Patna.
So, you must consult him once
Also Check: What Is The Life Expectancy Of Someone With Parkinson’s Disease
When Do Dementia Patients Stop Eating
When a patient stops or refuses to eat, things can be very depressing for the caregiver. Drinking and eating are complex and have to do with a control center that is within the brain, which controls the muscles in the throat and neck area.
Dementia affects this part of the brain as it progresses and things like choking, coughing, grimacing as one swallows, clearing the throat, movements that are exaggerated, especially of the tongue and mouth, refusing to swallow, and spitting the food can be seen. This usually happens in the later stages of the disease.
Behaviors Seen In Parkinsons Disease Dementia
As dementia progresses, managing disorientation, confusion, agitation, and impulsivity can be a key component of care.
Some patients experience hallucinations or delusions as a complication of Parkinsons disease. These may be frightening and debilitating. Approximately 50 percent of those with the disease may experience them.
The best thing to do when giving care to someone experiencing hallucinations or delusions from Parkinsons disease dementia is to keep them calm and reduce their stress.
Take note of their symptoms and what they were doing before they exhibited signs of hallucinating and then let their doctor know.
This element of the disease can be particularly challenging for caregivers. Patients may become unable to care for themselves or be left alone.
Some ways to make caregiving easier include:
- sticking to a normal routine whenever possible
- being extra comforting after any medical procedures
- limiting distractions
- using curtains, nightlights, and clocks to help stick to a regular sleep schedule
- remembering that the behaviors are a factor of the disease and not the person
Read Also: What Are Early Warning Signs Of Parkinson’s Disease
Signs And Symptoms Of Pdd
Common signs and symptoms of Parkinsons disease dementia include:
- Poor memory and concentration
- Depression
- Visual hallucinations
If youve noticed some of the above signs and symptoms in yourself or a loved one, its important to get them checked out. But dont jump to conclusions. People with Parkinsons often experience cognitive changes such as anxiety, lack of motivation, and slowed thinking. These symptoms do not automatically mean dementia.
How Does Parkinsons Affect The Brain
When the disease occurs, some nerve cells might break down or die gradually.
Though due to this the dopamine level of your brain decreases, & if the dopamine decreases, the brain will start behaving in an abnormal way.
Albeit, people often get confused over the two terms Alzheimers & Parkinsons well both the disease are caused by damaged brain cells..but there are huge differences.
You May Like: Can Parkinson’s Run In The Family
How Can We Support The Sleep/wake Cycle Of Pdd
For people with PDD who are confused about the day-night cycle, some daily strategies can be helpful. At night, starting a lights out routine that happens at the same hour every day, where all curtains are closed and lights are turned off, can help the person understand that it is sleep time. During the day, opening the curtains, allowing the person with PDD to spend as much time in the daylight as possible, avoiding naps, and organizing stimulating activities, can be helpful. Having lots of calendars and clocks in every room might also help a person with PDD be less confused about the time of day.
What Is Parkinson Disease
Parkinson disease is a movement disorder. It can cause the muscles to tighten and become rigid This makes it hard to walk and do other daily activities. People with Parkinsons disease also have tremors and may develop cognitive problems, including memory loss and dementia.
Parkinson disease is most common in people who are older than 50. The average age at which it occurs is 60. But some younger people may also get Parkinson disease. When it affects someone younger than age 50, it’s called early-onset Parkinson disease. You may be more likely to get early-onset Parkinson disease if someone in your family has it. The older you are, the greater your risk of developing Parkinson disease. It’s also much more common in men than in women.
Parkinson disease is a chronic and progressive disease. It doesn’t go away and continues to get worse over time.
Read Also: Parkinson’s Fatigue
Stage : Moderately Severe Dementia
When the patient begins to forget the names of their children, spouse, or primary caregivers, they are most likely entering stage 6 of dementia and will need full time care. In the sixth stage, patients are generally unaware of their surroundings, cannot recall recent events, and have skewed memories of their personal past. Caregivers and loved ones should watch for:
- Delusional behavior
When To Seek Hospice Care
When you or your loved one have a life expectancy of six months or less, you become eligible for hospice care a type of comfort care provided at the end of life for someone living with end-stage Parkinsons disease. Hospice provides extra support so your loved one can live as comfortably as possible.
If you have experienced a significant decline in your ability to move, speak, or participate in activities of daily living without caregiver assistance, its time to speak with a hospice professional.
Read more: What is hospice care?
Some of the things that determine whether your loved one with end-stage Parkinsons is eligible for hospice include: difficulty breathing, bed bound, unintelligible speech, inability to eat or drink sufficiently, and/or complications including pneumonia or sepsis.
If you live in South Jersey, our nurse care coordinator can answer your questions and decide if your loved one is ready for hospice care. Call us 24/7 at 229-8183.
Also Check: Can Parkinson’s Run In The Family
End Stage Of Dementia
The end stage of dementia is the most difficult stage for those suffering from the disease, and also for family members, caregivers, and healthcare professionals. Victims lose what is left of their intellectual and physical capabilities and become completely dependent on others. The model is still shifting in considering end stage dementia an end of life condition experts are pushing this model in order to advocate for better pain and distress management for those suffering at their end.
What Are The Symptoms Of End
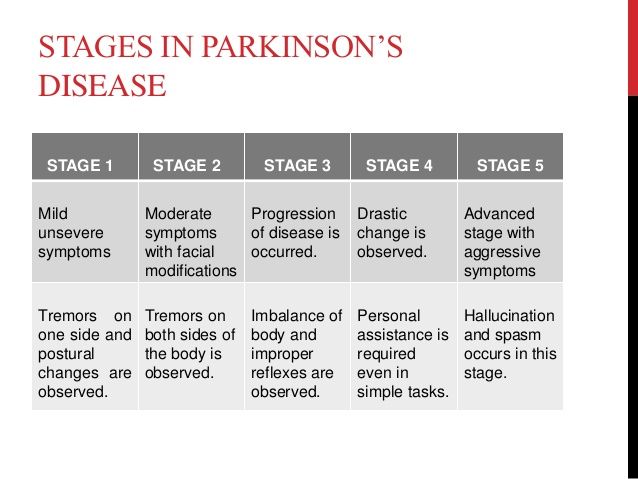
Stage four for Parkinsons disease is often called advanced Parkinsons disease because people in this stage experience severe and incapacitating symptoms. This is when medication doesnt help as much and serious disabilities set in.
Theres an increased severity in:
- How you speak a softer voice that trails off.
- Falling and trouble with balance and coordination.
- Freezing a sudden, but temporary inability to move, when you start to walk or change direction.
- Moving without assistance or a wheelchair.
- Other symptoms such as constipation, depression, loss of smell, low blood pressure when going to stand up, pain, and sleep issues.
Many times someone with advanced PD cant live on their own and needs help with daily tasks.
Stage five is the final stage of Parkinsons, and assistance will be needed in all areas of daily life as motor skills are seriously impaired. You may:
- Experience stiffness in your legs. It may make it impossible to walk or stand without help.
- Need a wheelchair at all times or are bedridden.
- Need round-the-clock nursing care for all activities.
- Experience hallucinations and delusions.
As Parkinsons disease progresses into these advanced stages, its symptoms can often become increasingly difficult to manage. Whether you or your loved one with end-stage Parkinsons lives at home, in an assisted living facility or a nursing home, hospice services can optimize your quality of life and that of your family members as well.
You May Like: How Long Do Parkinson’s Patients Live
How Is Parkinson Disease Diagnosed
Parkinson disease can be hard to diagnose. No single test can identify it. Parkinson can be easily mistaken for another health condition. A healthcare provider will usually take a medical history, including a family history to find out if anyone else in your family has Parkinson’s disease. He or she will also do a neurological exam. Sometimes, an MRI or CT scan, or some other imaging scan of the brain can identify other problems or rule out other diseases.
Life Expectancy And Vascular Dementia
Repeated small strokes can damage the brain and cause vascular dementia. Its the second most common cause of the disease. The pattern of disease progression is different from the gradual deterioration of Alzheimers disease. The symptoms may be steady for a while, then suddenly get worse followed by a further period of stability. This reflects times when blood clots interrupt the blood supply to the brain, causing damage.
Because people with vascular dementia is linked to strokes, people affected often have other illnesses and may have worse general health. Research suggests that the average life expectancy is around four years. However, sudden or severe deterioration can happen when there is a further stroke.
Recommended Reading: What Is The Life Expectancy Of Someone With Parkinson’s Disease
Early Signs And Symptoms Are Different
Parkinsons disease generally begins as a movement disorder. Early signs and symptoms include:2
- Tremor, which often begins in the hand or fingers
- Slowed movement, which may include foot dragging
- Rigidity
- Slowed automatic movements such as blinking, smiling, and swinging your arms when you walk
Alzheimers disease generally begins as noticeable memory loss. Early signs and symptoms include:3,4
- Trouble remembering familiar words
- Challenges performing everyday tasks such as balancing a checkbook
The Era Of Digital Cognitive Testing
The development of digital cognitive testing and the evolution of self-completed computerized assessments and wearable devices to assess cognitive functioning in daily life, provides an exciting opportunity to both improve clinical management and to obtain more sensitive outcome measures for clinical trials and will likely become a standard procedure in the future, given further technological improvements and increased access to the internet and digital devices. To reach this point, psychometric requirements , documentation and technical problems, as well as their relation to traditional tests, need to be well known.
You May Like: What Is The Life Expectancy Of Someone With Parkinson’s Disease
