What Are The Next Steps Following A Diagnosis Of Parkinsons
Once you have a diagnosis of Parkinsons, your doctor can begin developing a treatment plan. Parkinsons treatments aim to minimize symptoms and slow down progression.
Treatment plans will take into account such factors as symptoms, overall health, and response to treatment. Although theres no cure for Parkinsons, treatment can improve your quality of life.
Common treatments for Parkinsons include:
- Physical therapy: Physical therapy can help improve strength and balance.
- Speech therapy: Speech therapy can help reduce communication difficulties.
- Lifestyle changes: People with Parkinsons often benefit from adding exercise to their daily lives.
- Medication: There are several medications approved to treat the symptoms of Parkinsons. You might need to change medications as Parkinsons progresses.
- Deep brain stimulation:Deep brain stimulation is a surgical procedure. Surgeons place electrodes in your brain that are connected to a generator placed in your chest. These electrodes can help reduce the symptoms of Parkinsons.
Imaging The Pharmacology Of Depression In Pd
The prevalence of depression in PD has been reported to range from 10% to 45% . Because Lewy body pathology is known to affect serotonergic and noradrenergic as well as dopaminergic neurotransmission, dysfunction of any or all of these systems would seem to be a reasonable candidate for the functional substrate of depression . To date, functional imaging has failed to demonstrate a correlation between serotonergic dysfunction and depression in PD.
123ICIT binds with nanomolar affinity to dopamine, noradrenaline, and serotonin transporters. Although striatal uptake of 123ICIT 24 h after intravenous injection primarily reflects DAT binding, midbrain uptake 1 h after administration reflects serotonin transporter availability . Kim et al. have reported normal brain stem 123ICIT uptake in PD. They found no difference between uptake in depressed and nondepressed patients and no correlation between radiotracer uptake and Hamilton Depression Rating Scale scores .
Recommended Reading: Does Parkinsons Cause Hair Loss
Brain Mri Advances For Parkinsons Disease
In Parkinsons disease, the damage to brain cells begins long before any symptoms develop. Therefore, at-risk patients can benefit from early diagnosis, and efforts to slow the progression of the disease can start early.
Researchers are working on newer MRI approaches to precisely detect Parkinsons disease-related structural and metabolic activity in the brain and correlate it to the function of the organ. For example, scientists from Oxford University used a technique called the resting-state functional MRI to assess the strength of nerve cells in the a region of the brain called the basal ganglia to send and receive information. Because the physical signs of brain cell damage in Parkinsons disease are not recognizable by conventional MRI, this approach may help visualize the impact of the damage on the activity of brain cells and aid in early diagnosis.
Similarly, MRI is used to identify Parkinsons disease-specific biomarkers. Tracking the biomarkers using high-field and ultra-high field MRI can identify Parkinsons disease patients and help follow the progression of the condition.
Although many of these advancements are yet to be implemented in the clinical setting, such adaptations may help better understand the disease and develop new treatments.
Also Check: Parkinson’s Disease Linked To Herbicide
What Doctors Look For When Diagnosing Parkinsons
Certain physical signs and symptoms noticed by the patient or his or her loved ones are usually what prompt a person to see the doctor. These are the symptoms most often noticed by patients or their families:
-
Shaking or tremor: Called resting tremor, a trembling of a hand or foot that happens when the patient is at rest and typically stops when he or she is active or moving
-
Bradykinesia: Slowness of movement in the limbs, face, walking or overall body
-
Rigidity: Stiffness in the arms, legs or trunk
-
Posture instability: Trouble with balance and possible falls
Once the patient is at the doctors office, the physician:
-
Takes a medical history and does a physical examination.
-
Asks about current and past medications. Some medications may cause symptoms that mimic Parkinsons disease.
-
Performs a neurological examination, testing agility, muscle tone, gait and balance.
What Are The Risk Factors For Parkinsons
There are a few known risk factors for Parkinsons. These include:
- having a family history of Parkinsons
- being over 60 years
- having been exposed to herbicides, pesticides, and other toxins
Its important to note that these risk factors only cause a slight increase in risk. Having one or more risk factors isnt an indicator youll develop Parkinsons. However, if youre concerned about your risk for Parkinsons, talk with a doctor.
You May Like: How Is Treatment Used To Determine Parkinson’s Disease
Tests To Rule Out Other Conditions
Blood tests can help rule out other possible causes of the symptoms, such as abnormal thyroid hormone levels or liver damage.
An MRI or CT scan can check for signs of a stroke or brain tumor, which may cause similar symptoms.
Hydrocephalus due to atrophy can occur with some types of dementia and would be visible with one of these imaging tests. If the person has neurologic symptoms but a normal scan result, Parkinsons disease may be present.
The doctor a lumbar puncture to rule out inflammation or a brain infection.
Referral To A Specialist
If your GP suspects Parkinson’s disease, you’ll be referred to a specialist.
This will usually be:
- a neurologist, a specialist in conditions affecting the brain and nervous system
- a geriatrician, a specialist in problems affecting elderly people
The specialist will most likely ask you to perform a number of physical exercises so they can assess whether you have any problems with movement.
A diagnosis of Parkinson’s disease is likely if you have at least 2 of the 3 following symptoms:
- shaking or tremor in a part of your body that usually only occurs at rest
- slowness of movement
- muscle stiffness
If your symptoms improve after taking a medication called levodopa, it’s more likely you have Parkinson’s disease.
Special brain scans, such as a single photon emission computed tomography scan, may also be carried out in some cases to try to rule out other causes of your symptoms.
Recommended Reading: What To Do For Parkinson’s Cough
Correlation Between Lr And Neuroimaging Parameters
LR scores were found to significantly correlate with two MRI radiomics features the T2* kurtosis within the left SN , and T2* skewness within the red nuclei .
LR scores were significantly correlated with SBR values in six VOIs: left caudate , right caudate , left putamen , right putamen , left Globus pallidum , right Globus pallidum . No significant correlations were detected between LR and SBR values in the brainstem.
What Happens At The Exam
If your doctor thinks you might have Parkinsonâs disease, theyll recommend that you see a specialist who works with nervous system issues, called a neurologist. One whoâs also trained in movement disorders, like Parkinsonâs, may be able to make the right diagnosis faster.
Your neurologist will probably want to see how well your arms and legs move and check your muscle tone and balance.
They may ask you to get out of a chair without using your arms for support, for example. They also may ask a few questions:
- What other medical conditions do you have now or have you had in the past?
- What medications do you take?
- Has your handwriting gotten smaller?
- Do you have trouble with buttons or getting dressed?
- Do your feet feel âstuckâ to the floor when you try to walk or turn?
- Do people say your voice is softer or your speech is slurred?
Tell your doctor if youâve noticed a change in your sense of smell or you have trouble with sleep, memory, or mood.
Parkinsonâs disease can look different from person to person. Many people have some symptoms and not others.
Recommended Reading: How Is Parkinson’s Disease Inherited
Dementia With Lewy Bodies
Dementia with Lewy bodies is responsible for approximately 25% of dementias and belongs to the atypical Parkinson syndromes together with progressive supranuclear palsy and multi-system atrophy . The clinical manifestations can be similar to that of AD or dementia associated with Parkinsons disease. Patients typically present with one of three symptom complexes: detailed visual hallucinations, Parkinson-like symptoms and fluctuations in alertness and attention.Pathologically, the disease is characterized by the presence of Lewy bodies in various regions of the hippocampal complex, subcortical nuclei and neocortex with a variable number of diffuse amyloid plaques. Cholinesterase inhibitors are currently the treatment of choice for this condition.
The role of imaging is limited in Lewy body dementia.Usually the MR of the brain is normal, including the hippocampus. This finding is important as it enables us to differentiate this disease from Alzheimer s disease, the main differential diagnosis. Nuclear imaging can be used to demonstrate an abnormal dopaminergic system
PSP with midbrain atrophy
Dont Miss: Benzodiazepines And Parkinsons Disease
Clinical Application Of Brain Mri In The Diagnostic Work
aDepartment of Radiology and Nuclear Medicine, Radboud University Medical Center, Nijmegen, The NetherlandsbDepartment of Diagnostic Imaging, Medical Center of Postgraduate Education, Warsaw, PolandcDepartment of Neurology, Donders Institute for Brain, Cognition and Behaviour, Radboud University Medical Center, Nijmegen, The Netherlands
Keywords: Atypical parkinsonism, brain, magnetic resonance imaging, Parkinsons disease
ABSTRACT
Background: Differentiating Parkinsons disease and atypical parkinsonism on clinical parameters is challenging, especially in early disease courses. This is due to large overlap in symptoms and because the so called red flags, i.e. symptoms indicating atypical parkinsonism, have not developed. Brain MRI can aid to improve the accuracy and confidence about the diagnosis.Objective and Methods: In the current paper, we discuss when brain MRI should be performed in the diagnostic work-up of parkinsonism, our preferred brain MRI scanning protocol, and the diagnostic value of specific abnormalities.Results and Conclusions: The main purpose of brain MRI is to assess cerebrovascular damage, and to exclude other possible and sometimes treatable causes of parkinsonism, such as normal pressure hydrocephalus. Furthermore, brain MRI can support the possible or probable diagnosis of a specific form of atypical parkinsonism.
INTRODUCTION OF THE CLINICAL DILEMMA
DESCRIPTION OF THE TEST
DISCUSSION
ACKNOWLEDGMENTS
CONFLICT OF INTEREST
Read Also: How Is Parkinson Disease Currently Treated
What Causes Parkinsons Disease
We do not know what causes Parkinsons disease. There is some evidence to suggest that there is a genetic factor which increases the risk of Parkinsons disease within some families. Also, there might be an increased risk if people have come into contact with a particular toxin or toxins found in the environment via pesticides and other chemicals used in agriculture. The specific toxin or toxins have not yet been identified but there is ongoing research into this possible cause.
Mri In Parkinsons Testing
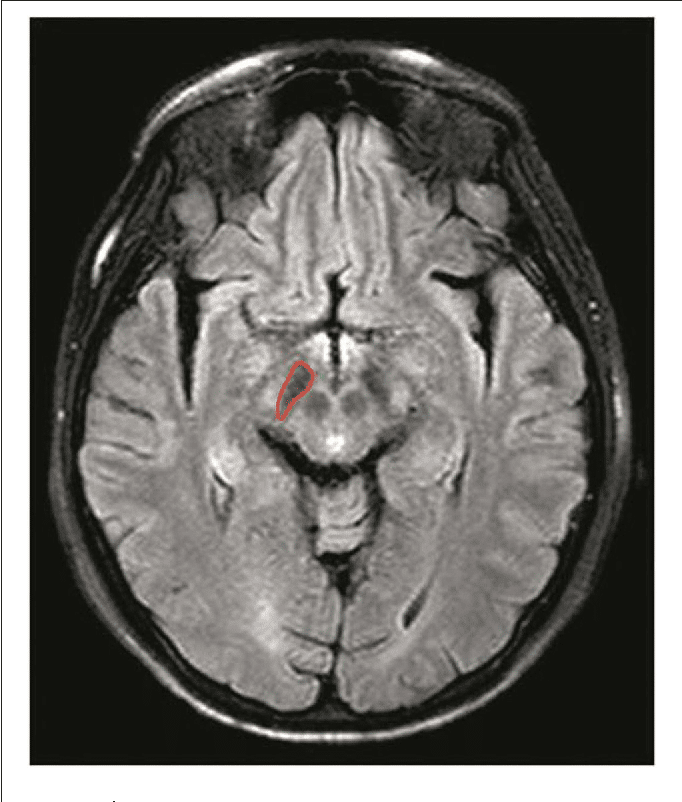
One of the more common tests done during a neurologic workup is an MRI scan and one may think that in the investigation of a disease that affects the brain such as Parkinsons, this imaging test would be a necessity. In the context of Parkinsons disease, however, an MRI is not particularly helpful. It looks at the structure of the brain which, for all intents and purposes, appears normal in this disease. An MRI may, however, be indicated when symptoms appear in younger people or if the clinical picture or the progression of symptoms is not typical for Parkinsons. In these situations, MRI can be used to rule out other disorders such as stroke, tumors, hydrocephalus , and Wilsons Disease .
Read Also: Can Parkinson’s Go Away
Is An Mri Exam Safe For Parkinsons Disease
Yes. The MRI exam poses no risk to the average person if appropriate safety guidelines are followed. But, if you have a deep brainstimulator to treat your Parkinsons disease, talk to your doctor before having an MRI since the stimulator may need to be turned off. It should be evaluated and turned on again after the MRI.
Some conditions may make an MRI exam inadvisable. Others mean that precautions need to be taken. Tell your doctor if you have any of the following conditions:
- Weigh more than 300 pounds
- Not able to lie on back for 30 to 60 minutes
What Can You Detect With A Parkinsons Mri
Generally, you can receive a Parkinsons diagnosis in a clinical setting, but an MRI can help to assess various aspects of the disease and its progress. In particular, a Parkinsons MRI can do the following for patients who have or are suspected to have Parkinsons disease:
- Evaluate tissue loss and how the brain is atrophying
- Check for changes to the basal ganglia region of the brain
- Find out if there are abnormal iron deposits in the basal ganglia or brainstem
- Look at changes to white matter
- Examine the diffusion of restricted tissues in acute infarction and neurodegenerative diseases
- Help to diagnose atypical parkinsonism
- Exclude treatable causes of parkinsonism such as normal pressure hydrocephalus
Read Also: Seroquel And Parkinsons Disease
Don’t Miss: What New In Parkinson Treatment
The First Full Body Mri Conditional Portfolio3
Medtronic offers the world’s first full-body MRI capable DBS device portfolio. People with Parkinsons with implanted DBS systems feel reassured knowing that with proper safeguards, MRI is an option for them.
PerceptTM PC neurostimulator is the first and only device to have full-body MR Conditional4 access anywhere on the body for both 1.5T and 3T MRI scans.
Is Early Diagnosis Possible
Experts are becoming more aware of symptoms of Parkinsons that precede physical manifestations. Clues to the disease that sometimes show up before motor symptoms and before a formal diagnosis are called prodromal symptoms. These include the loss of sense of smell, a sleep disturbance called REM behavior disorder, ongoing constipation thats not otherwise explained and mood disorders, such as anxiety and depression.
Research into these and other early symptoms holds promise for even more sensitive testing and diagnosis.
For example, biomarker research is trying to answer the question of who gets Parkinsons disease. Researchers hope that once doctors can predict that a person with very early symptoms will eventually get Parkinsons disease, those patients can be appropriately treated. At the very least, these advances could greatly delay progression.
Also Check: How To Take Care Of A Person With Parkinson Disease
Pd Diagnosis Disease Severity And Disease Progression
The diagnosis of PD is essentially clinical , and we believe that the clinical evaluation of patients will not be replaced by modern imaging techniques. Nevertheless, as pointed out earlier, misdiagnosis can approach 20% of cases . Recently, in line with the European Union, the U.S. FDA approved DAT scan as a diagnostic tool to help differentiate between PD and Essential Tremor. This is the only current FDA-approved subsidiary examination to aid in PD diagnosis.
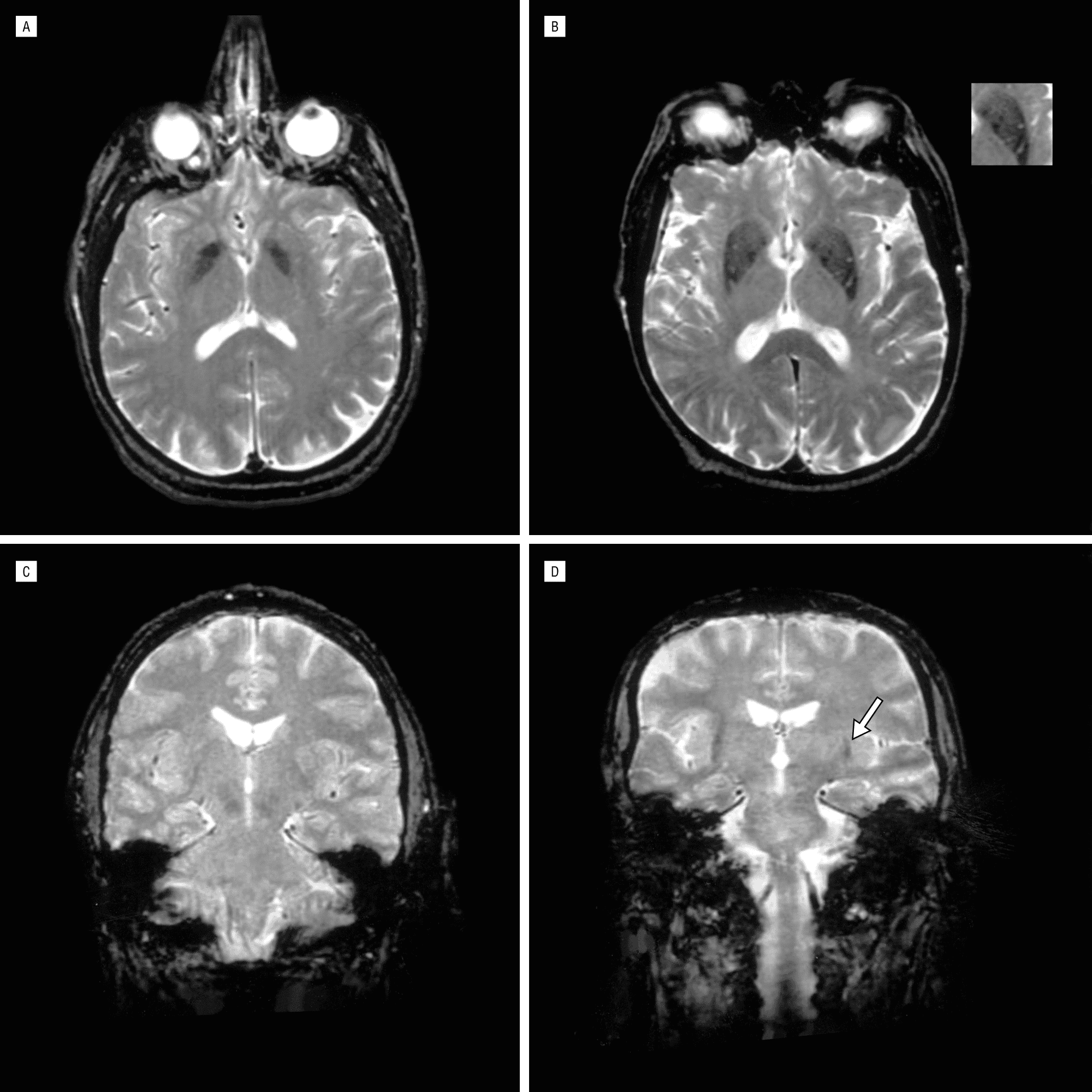
The role of magnetic resonance imaging in the diagnosis of PD is still not fully established. Traditionally, it has been seen as a means to potentially exclude alternate diagnoses such as vascular parkinsonism, or more importantly , atypical forms of degenerative parkinsonism such as MSA or progressive supranuclear palsy . Traditional structural MRI findings of these latter diagnoses such as increased pallidal iron, rim of putaminal hyperintensity, hot cross bun sign and/or cerebellar atrophy in MSA or the hummingbird or penguin sign in PSP may not be reliable, particularly in early disease.
Figure 5. Multimodal MRI in PD. Differences are noted between patients with PD and controls through voxel-based analysis of R2, mean diffusivity, and fractional anisotropy maps.
-
Low dopamine transporter uptake in basal ganglia demonstrated by SPECT or PET imaging.*
Brent A. Vogt, in, 2019
Preparing For A Parkinsons Mri
A Parkinsons MRI is completely painless, but you do have to lie still while being scanned. Some patients feel claustrophobic in this situation. If youre worried about that, talk with your doctor about the possibility of having an anti-anxiety medication before the procedure.
On the day of the appointment, follow any instructions provided to you by your doctor. Remove metal jewelry and dont wear make-up as that can also have metal in it. If you are in the advanced stages of Parkinsons or if you are taking a sedative, you should arrange transportation to and from the appointment.
You May Like: What Are The Cardinal Signs Of Parkinson’s Disease
T Mri Measures Changes In Brains Of Patients With Parkinsons Disease
Researchers at the University of Cambridge used a new ultra-high strength 7T MRI scanner at the Wolfson Brain Imaging Centre to measure changes in the brains of people with Parkinsons disease, progressive supranuclear palsy , or in good health. The study, published in Movement Disorders, suggests that 7T MRI scanners could be used to help identify those patients with Parkinsons disease and similar conditions most likely to benefit from new treatments for previously untreatable symptoms.
Patients with Parkinsons disease and PSP are often treated with drugs such as L-DOPA, which compensate for the severe loss of dopamine. But, dopamine treatment does little for many of the non-motor symptoms. That is why scientists have begun to turn their attention to noradrenaline, a chemical that plays a critical role in brain functions including attention and arousal, thinking and motivation.
Professor James Rowe from the Department of Clinical Neurosciences at the University of Cambridge, who led the study, said, Noradrenaline is very important for brain function. All of our brains supply comes from a tiny region at the back of the brain called the locus coeruleus which means the blue spot. Its a bit like two short sticks of spaghetti half an inch long: its thin, its small, and its tucked away at the very base of the brain in the brain stem.
-
New research indicates that blocking proteins with medications
Mri And Parkinsons Treatment
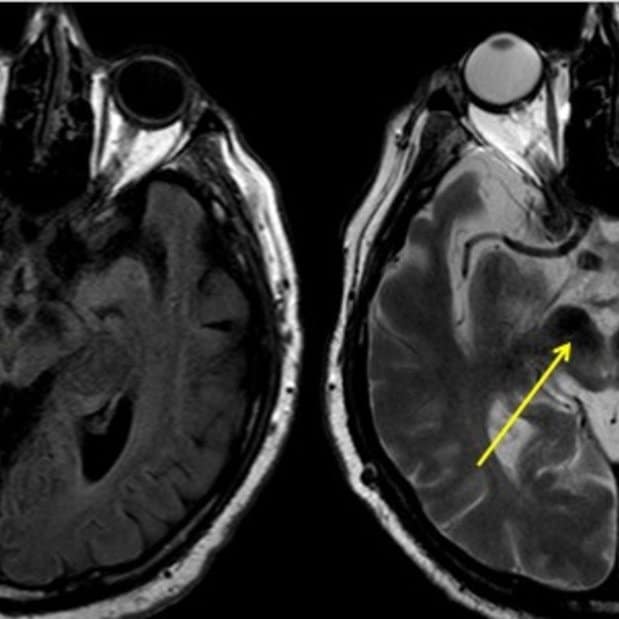
Tremors in hand or shaky legs are the first and most common signs of Parkinsons disease. Ignoring the initial signs make things worse and the problems get complicated as time passes by. Theres a hope given by a recent research. As per the findings published in the journal Brain suggests that theres a new MRI technique which claims to detect this disorder and treat without surgery.
MRI technology is used to closely monitor a part of the brain. This technique can also help in targeting the part of the brain which causes tremors and is linked to Parkinsons. This discovery can help in treating the problem without surgery and side-effects.
Also Read: Know How Living Near Highway Causes Dementia and Other Problems
Dr. Bhavya R. Shah is an M.D. and Assistant Professor of Radiology and Neurological Surgery at Peter ODonnell Jr. Brain Institute, UT Southwestern, Dallas, Texas. Shah who lead this research and said: The benefit for patients is that we will be better able to target the brain structures than we want. And because were not hitting the wrong target, well have fewer adverse effects.
Without opening the skull and conducting the surgery, Parkinsons patient can be given the treatment. However, this still needs to be tested thoroughly before it can be implemented to treat the patients.
Read Also: Very Early Parkinsons Symptoms
Recommended Reading: Parkinson’s Disease Bowel Problems
