Differentiating Multiple Sclerosis Symptoms With Parkinsons Disease
Signs and symptoms of multiple sclerosis include numbness or weakness in one or more limbs, partial or complete vision loss, prolonged double vision, tingling or pain, electric-shock sensations, tremors and lack of coordination, fatigue, dizziness, slurred speech, and problems with bowel and bladder function.
Parkinsons disease symptoms typically begin with tremors followed by muscle stiffness, difficulty standing or walking, changes in speech, slow movements, impaired posture and balance, loss of automatic movements, and writing changes.
As you can see, Parkinsons disease and multiple sclerosis do have some symptoms in common, which can make early diagnosis difficult.
Read Also: Parkinsons Information For Patients
Maintaining Your Normal Pd Medication Schedule
Maintaining your PD medication schedule is crucial for anyone with PD. The correct timing and dosage are essential to your comfort and well-being. However, oftentimes when undergoing surgery, there may be restrictions regarding when you can and cannot take medications. Here are a few tips to navigate this issue:
Other Concerns To Be Aware Of
There are a few other possible concerns to be aware of when having surgery. Again, not everyone will experience these issues, but it is wise to understand them and be aware so that you can plan accordingly and be prepared.
- The effect of even mild dehydration may be exacerbated in PD.
- People with PD may have swallow dysfunction. This can be exacerbated by anesthesia and make people with PD at higher risk for aspiration, defined as the tendency for food or liquid to get into the airway. Therefore, it is best to introduce soft foods slowly after surgery.
- People with PD may have significant fluctuations of blood pressure which can be magnified in the post-operative period. Episodes of low blood pressure can cause dizziness and even fainting. This problem is most prominent when changing head position that is moving from lying down, to sitting to standing. Therefore, these changes should be made very slowly.
- Urinary dysfunction is common in PD, and people with PD may be particularly prone to urinary tract infections . It is important to note that UTIs or any infection may first manifest as an unexplained worsening of PD symptoms or initiation of hallucinations.
- People with PD are particularly prone to constipation and this can be exacerbated in the post-operative period. Taking a daily medication to prevent constipation may become necessary after surgery.
Tips and takeaways
You May Like: Anticholinergic Drugs For Parkinson’s
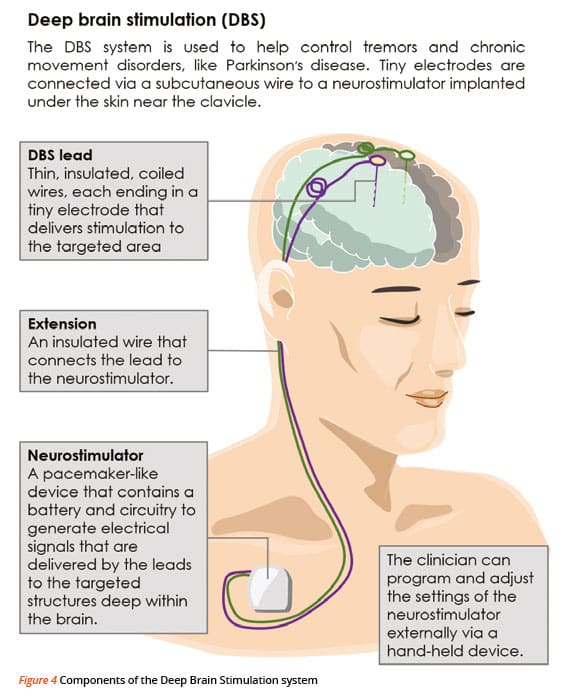
What Is Deep Brain Stimulation Surgery
Deep brain stimulation surgery involves implanting thin wires with electrodes on the ends into specific areas of your brain. Once in place, they produce mild electrical impulses that regulate abnormal brain activity a process known as neurostimulation. Dr. Watson can adjust these electrical pulses based on your condition and symptoms to achieve the best results.
To perform the surgery, the thin wires with the electrodes on the ends are inserted into different areas of the brain through tiny incisions in the skull. The internal pulse generator which provides the electrical current is implanted in the upper chest or abdomen. A single wire then connects the pulse generator to the wires with the electrodes on the end. This single wire is hidden underneath the skin of your head, neck, and shoulder.
After undergoing deep brain stimulation surgery, youll also receive a remote control, so youll be able to turn the device on or off. Deep brain stimulation surgery may provide significant relief from certain neurological symptoms. However, you should consider it an interventional therapy, not a cure.
Going Into Hospital For Surgery

If you are having surgery for something not connected to your Parkinsons, make sure the healthcare professionals involved know about your condition.
This will mean that anything about your Parkinsons that could create problems, such dystonia or a tremor, can be taken into account so you can still be treated properly.
If you need to have an emergency operation, it is important that the healthcare team looking after you know you have Parkinsons as soon as possible.
You will usually meet your anaesthetist on the ward before your surgery. It is very important that your anaesthetist knows you have Parkinsons and what medication you take for the condition.
Some anaesthetics may make Parkinsons symptoms worse or interfere with Parkinsons medication. The anaesthetist can plan your care appropriately around this.
When you meet the anaesthetist they will go through your answers to the pre-admission questions. They will also discuss your Parkinsons symptoms and how they may affect you during surgery, as well as explaining any risks or side effects of the drugs you might have.
Can I keep taking my Parkinson’s medication right up until the time of surgery?
Its important that you can keep taking your Parkinsons medication as close to your surgery as possible, and as soon as possible after the operation.
Organising your medication regime is also easier if you know what time your surgery will be in advance.
Levodopa
Apomorphine
Dopamine agonists
Low blood pressure
You May Like: Can Epilepsy Cause Parkinson’s Disease
Get A Good Nights Sleep
Studies show that about 3 in 4 people with Parkinsons also have sleep problems, but its crucial to your overall health to get a good nights sleep. Try strategies like creating a relaxing bedtime routine, going to bed at the same time every night, making your bedroom comfortable, dark and cool, and avoiding stimulants, such caffeine, alcohol, exercise and even watching TV, right before bedtime. If you are still having sleep problems, ask your doctor for a referral to a sleep specialist.
Take Care Of Your Mental Health
About half of all people with Parkinsons deal with some sort of mood disturbance, such as depression or anxiety, at some point. These mental disorders will only further compound the problems of Parkinsons, so its critical to get needed treatment, possibly medicine or counseling from a mental health professional.
You May Like: Can An Emg Diagnose Parkinson’s
Purpose Of Brain Surgery For Parkinsons Disease
Parkinsons disease surgery is used to treat motor effects of Parkinsons disease, such as tremor, but it does not help non-motor effects, such as reduced facial expression and dry skin.
Parkinsons disease can range from mild to severe, and it can be very disabling when the disease is severe. When high doses of medication are needed to control the symptoms, the medication can cause side effects such as dyskinesia , hallucinations, or both.
You might benefit from surgery if your symptoms do not improve adequately with medication or if you experience severe medication side effects.
Medications And Parkinsons Symptoms
Taking certain medicationsspecifically ones that block the action of dopaminecould cause Parkinsons disease symptoms. Its a condition called drug-induced parkinsonism, and while it isnt Parkinsons disease itself, it can look and feel a lot like it.
Here are some of the drugs can cause Parkinsons disease symptoms:
- Anti-nausea medications
- Drugs that treat hyperkinetic movement disorders
Keep in mind that even though these medications could cause symptoms similar to Parkinsons, they dont cause the disease itself. And most of the time, the symptoms go away within hours or days once you stop taking that drug, per the Parkinsons Disease Society.
In some cases, the Parkinsons symptoms dont go away after a person stops taking the medication that led to them, and theyre eventually diagnosed with Parkinsons disease.
Researchers dont think that the medication was the cause of Parkinsons in those cases, but that those individuals dopamine levels were already depleted, and the side effects of the drugs revealed their underlying Parkinsons disease. Put another way, the medication was the straw that broke the camels back, according to the American Parkinson Disease Association.
Research on what causes Parkinsons disease continues to grow. If you experience symptoms of Parkinsons, such as a tremor, slowed movement, balance problems, or changes in your speech or writing, connect with a doctor to diagnose the condition.
Read Also: How To Reverse Parkinson’s Disease Naturally
Work With An Occupational Therapist
An occupational therapist is an important member of your treatment team. Working closely with this medical professional will help improve your quality of life. An occupational therapist will typically meet with you in your home, review your daily routine, and provide you with techniques and tools that will help you carry out your activities of daily living more effectively, even with the challenges presented by your illness.
Mayo Clinic Q And A: Rate Of Progression Of Parkinsons Disease Hard To Predict
DEAR MAYO CLINIC: My father is 64 and was diagnosed with Parkinsons last year. So far his symptoms are very mild, but Im wondering what the typical progression of the disease is like. I have read that deep brain stimulation is sometimes recommended. When is this type of treatment usually considered? Is it safe?
ANSWER: The symptoms of Parkinsons disease, or PD, tend to begin very gradually and then become progressively more severe. The rate of progression is hard to predict and is different from one person to another. Treatment for PD includes a variety of options, such as exercise, medication and surgery. Deep brain stimulation is one surgical possibility for treating PD, but its usually only considered in advanced cases when other treatments dont effectively control symptoms.
Parkinsons disease is a syndrome which typically has no known cause. The diagnosis is based on symptoms. Neurologists who specialize in movement disorders typically have the most experience with PD diagnosis and treatment. There are many symptoms of parkinsonism. The most common include excessive slowness and lack of movement, as well as shaking or tremor.
As in your fathers situation, symptoms are often mild at the outset. How quickly they get worse varies substantially, perhaps because there may be multiple underlying causes of the disease. In most cases, symptoms change slowly, with substantive progression taking place over the space of many months or years.
You May Like: Do You Have Pain With Parkinson’s Disease
Methamphetamine And Amphetamine Abuse And Parkinsons Disease
The National Institute on Drug Abuse reports that methamphetamine and amphetamine abuse can increase the risk of developing Parkinsons disease.
A main insight from this research is that abuse of these types of drugs damages dopamine neurons in the brain. As Parkinsons disease is a dopamine-related disorder, it makes sense that individuals who abuse drugs, and thereby damage their dopamine neurons, may develop symptoms of Parkinsons disease. Since, as discussed earlier, dopamine plays a key role in muscle coordination and functionality, dopamine damage results in motor impairment, a hallmark of Parkinsons disease.
One research study found a near 300 percent increase in the risk of developing Parkinsons disease in people who have abused methamphetamine or amphetamine. This risk is alarming when one considers that despite public knowledge of the devastating effects of methamphetamine abuse, in 2014, an estimated 438,000 Americans in the 26+ age group were currently using this illicit drug. Note that the 2014 National Survey on Drug Use and health, from which this statistic is taken, did not expressly collect data on amphetamine use, so the estimated number of amphetamine abusers for that survey year is not available. When amphetamine abuse does occur, it is often in the form of prescription medications such as Adderall and Ritalin.
The good news is that recovery from substance abuse is always possible.
No One Definitive Cause Of Parkinsons
There are no biomarkers or objective screening tests that indicate one has Parkinsons. That said, medical experts have shown that a constellation of factors are linked to it.
Parkinsons causes are likely a blend of genetics and environmental or other unknown factors. About 10 to 20 percent of Parkinsons disease cases are linked to a genetic cause, says Ted Dawson, M.D., Ph.D., director of the Institute for Cell Engineering at Johns Hopkins. The types are either autosomal dominant or autosomal recessive .
But that leaves the majority of Parkinsons cases as idiopathic, which means unknown. We think its probably a combination of environmental exposure to toxins or pesticides and your genetic makeup, says Dawson.
Age. The biggest risk factor for developing Parkinsons is advancing age. The average age of onset is 60.
Gender. Men are more likely to develop Parkinsons disease than women.
Genetics. Individuals with a parent or sibling who is affected have approximately two times the chance of developing Parkinsons. Theres been an enormous amount of new information about genetics and new genes identified over the past 10 or 15 years that have opened up a greater understanding of the disease, says Dawson.
Read Also: What Is Dbs Surgery For Parkinson’s Disease
Parkinsons Disease And Cancer: Whats The Connection
Researchers have long tried to understand the relationship between Parkinsons disease and cancer, with multiple studies conducted over the years. Intuitively, PD and cancer are not at all similar, and can even be thought of as biochemically opposite in one disease , cells die unexpectedly and in the other , cells divide too often and are perpetuated for too long. In fact, there have been many epidemiological studies over past decades that have shown that patients who have had cancer have a lower risk of developing PD than the general population. Other studies have shown that people with PD have lower overall cancer risks than people without PD.
Despite many papers demonstrating this inverse relationship between PD and overall cancer risk, an occasional study has been conducted which concluded that people with PD have an increased risk of cancer. It can be confusing to understand the different studies and determine how the resulting information may or may not apply to you.
Here we highlight some of the more common cancer-related topics when it comes to PD:
Recommended Reading: Does Weed Help With Parkinsons
What Are Parkinsons Disease
Delusions are false beliefs that are not based on reality. These beliefs are fixed. People experiencing them are unlikely to change or abandon these beliefs, even when presented with evidence that they are false.
Delusions experienced by people with Parkinsons disease are usually of a common theme. These may include:
- Spousal infidelity
- Thinking that people are stealing their belongings
- Thinking people are trying to harm them
- Thinking people may put poison in their food
- Thinking people are switching out or substituting their medications
- Other beliefs based on paranoia
Recommended Reading: Are Intention Tremors Common In Parkinson’s
Parkinsonism Vs Parkinsons Disease
Parkinsonism refers to a cluster of symptoms that mimic the movement problems caused by Parkinsons disease. Its sometimes referred to as atypical Parkinsons disease, secondary parkinsonism, or Parkinsons plus.
Parkinsons disease is a chronic, neurodegenerative brain disorder. In addition to problems with movement, Parkinsons disease causes non-motor symptoms that arent caused by drug-induced parkinsonism. They include:
Another key difference between drug-induced parkinsonism and Parkinsons disease is symmetry. Drug-induced parkinsonism usually affects both sides of the body equally. Parkinsons disease affects one side of the body more than the other.
Parkinsonism can be caused by medications, repeated head trauma, and environmental toxins. It can also be caused by neurological disorders, including Parkinsons disease. Other neurological conditions that cause parkinsonism include:
- progressive supranuclear palsy
These medications dont cause resting tremors. Rather, they cause:
- Action tremors. These occur in a body part thats moving, not a body part thats resting.
- Postural tremors. These occur when a body part is forced to withstand gravity, such as when arms are outstretched or legs are raised.
Recommended Reading: How Long Does A Person Live With Parkinsons Disease
Diagnosis Of Parkinsons Disease
There are currently no blood or laboratory tests to diagnose non-genetic cases of Parkinsons. Doctors usually diagnose the disease by taking a persons medical history and performing a neurological examination. If symptoms improve after starting to take medication, its another indicator that the person has Parkinsons.
A number of disorders can cause symptoms similar to those of Parkinsons disease. People with Parkinsons-like symptoms that result from other causes, such as multiple system atrophy and dementia with Lewy bodies, are sometimes said to have parkinsonism. While these disorders initially may be misdiagnosed as Parkinsons, certain medical tests, as well as response to drug treatment, may help to better evaluate the cause. Many other diseases have similar features but require different treatments, so it is important to get an accurate diagnosis as soon as possible.
Also Check: Can Parkinson’s Patients Take Melatonin
Parkinsons Disease And Melanoma
Even in studies that have established a lower overall cancer risk in people with PD, the risk of certain specific types of cancers is higher than in the general population.
Melanoma is a type of skin cancer that has been consistently linked to PD. People who have had melanoma are at an increased risk for PD and people who have PD are at an increased risk of melanoma. The relationship between melanoma and PD is intriguing:
- The substantia nigra, or the black substance, is the area of the brain that contains the dopaminergic neurons that degenerate in PD. These neurons are full of neuromelanin, a dark pigment found in the brain which is related to melanin, a dark pigment found in the skin.
- Levodopa is a precursor for melanin and neuromelanin.
If a person regularly ingests Levodopa, he/she may be fueling the production of melanin, and possibly the production of melanin-containing cells, which in theory would increase the likelihood of melanoma. However, some studies have demonstrated that the increased melanoma risk is present in patients with PD even before Levodopa is started, suggesting that the relationship is not due to Levodopa intake but rather to a genetic link.
Epidemiological studies have shown an increased risk of non-melanoma skin cancers in PD patients as well.
What to do if you have an increased melanoma risk?
You should know what other melanoma risk factors you have. These include:
B Appropriate Prophylaxis And Other Measures To Prevent Readmission
Ensure adequate nutrition and safe swallowing.
Fall prevention and physical therapy to strengthen the patient.
If the patient is to return home on discharge, make sure the primary caregiver has adequate support systems and community resources available to assist in care.
No sponsor or advertiser has participated in, approved or paid for the content provided by Decision Support in Medicine LLC. The Licensed Content is the property of and copyrighted by DSM.
You May Like: How Is Parkinson’s Disease
