Parkinsons An Autoimmune Disease
Discovering the cause or etiology of diseases such as Parkinsons is essential to finding a treatment to prevent it. There are more and more advances in this field. And one of the latest ones is that Parkinsons could be an autoimmune disease.
Índice
Parkinsons Disease Found To Have Clear Genetic Signature
Parkinson’s disease is not usually seen as an autoimmune disease.
Researchers at the La Jolla Institute for Immunology say they have found that people with Parkinsons disease have a clear genetic signature of the disease in their memory T cells. The scientists, who published their study Transcriptional analysis of peripheral memory T cells reveals Parkinsons disease-specific gene signatures in npj Parkinsons Disease, hope that targeting these genes may open the door to new Parkinsons treatments and diagnostics.
Parkinsons disease is a multi-stage neurodegenerative disorder with largely unknown etiology. Recent findings have identified PD-associated autoimmune features including roles for T cells. To further characterize the role of T cells in PD, we performed RNA sequencing on PBMC and peripheral CD4 and CD8 memory T cell subsets derived from PD patients and age-matched healthy controls, write the investigators.
When the groups were stratified by their T cell responsiveness to alpha-synuclein as a proxy for an ongoing inflammatory autoimmune response, the study revealed a broad differential gene expression profile in memory T cell subsets and a specific PD associated gene signature. We identified significant enrichment of transcriptomic signatures previously associated with PD, including for oxidative stress, phosphorylation, autophagy of mitochondria, cholesterol metabolism and inflammation, and the chemokine signaling proteins CX3CR1, CCR5, and CCR1.
The Role Of Mhc Proteins In Pd Pathogenesis
T cells recognize a complex formed between MHC molecules and a peptide epitope. The epitope is presented to T cells as a result of a complex series of events termed antigen processing and presentation that involve the intracellular degradation of self and foreign proteins into peptides that are then loaded onto the antigen-binding groove of MHC molecules. In general, T cells recognize peptides derived from foreign molecules, but in disease some T cells also evade self-tolerance and can recognize self-peptides. MHC class I in general presents peptides derived from the same cell , while MHC class II typically present peptides derived from extracellular proteins .
Mature neurons are generally thought to lack MHC expression and so to not present antigens. However, SN and LC neurons recently have been shown to express MHC-I and co-localize with CD8+ T cells in response to stimuli such as IFN . Catecholamine neurons are particularly sensitive to inflammation in comparison to other neuron types. A lower amount of IFN is required by dopaminergic neurons to express MHC-I in comparison to other neuronal subtypes. The MHC-I presented by dopaminergic neurons is functional and can result in cytotoxicity in the presence of matching antigen and CD8+ T cells . Dopaminergic neuron sensitivity to inflammation and corresponding MHC-I upregulation could render them susceptible to infiltrating T cells versus neighboring, more resistant GABAergic neurons.
Read Also: How To Help People With Parkinson’s Disease
New Diagnostic Tests For Parkinsons
One day, researchers may be able to check people for genetic biomarkers for PD. This type of test could predict whether a person has a risk factor for developing autoimmune attacks on alpha-synuclein. It may even help with early diagnosis, detecting PD before it starts causing motor symptoms.
Nonetheless, before tests like this become available, large and long-term studies must provide scientists with evidence that monitoring an autoimmune reaction in a persons body is a good test for PD.
In Vitro Studies Of Ipsc
A recent in vitro study using induced-pluripotent stem cells -derived midbrain neurons and T cells from PD patients was the first to show that PD patient-derived T cells can kill dopamine neurons directly. Sommer et al. determined that PD patients contain significantly higher Th17 cells than healthy controls . The PD patient-derived Th17 cells exerted cytotoxic effects on neurons by releasing IL-17A, a cytokine detected by IL-17R expressed on neurons . The iPSC in vitro cultures lacked glia, which express MHC-II and can potentially interact with Th17 cells. In addition, T cells were activated non-specifically, and so the antigen specificity of Th17 cells remains unclear . While the study indicates that PD-derived T cells can directly kill dopaminergic neurons, the omission of professional antigen presenting cells, antigenicity, and neuronal specificity in the cultures in this initial study overlooks the role of multiple relevant in vivo factors important for disease progression. Moreover, the mode of action that garners specific vulnerability of dopaminergic neurons and avoids unaffected neurons was not resolved in this study. Nevertheless, the study indicates Th17 cells may participate in PD-related neuronal death.
Also Check: Early Onset Parkinsons Tremor
Also Check: What Is Used To Treat Parkinson’s Disease
Genetic Regulation Of Autoimmunity In Pd
In addition to these observations, DJ-1 has also been reported to affect the development of natural Tregs and induced Tregs . Mature Tregs with normal function, which modulate not only adaptive immunity but also innate immunity, are pivotal for maintaining thymic function, peripheral immune self-tolerance and immune system homeostasis. nTregs are generated in the thymus, while iTregs are derived from naïve CD4+ T cells encountering antigens in the peripheral organs. Both cell types are generally immunosuppressive through the suppression or downregulation of effector T cell proliferation . Their self-check function successfully prevents excessive effector cell reactions. On the other hand, the abnormal proliferation of both types of Tregs leads to the failure of self-/non-self-discrimination, resulting in autoimmune disease . Evidence reported by Singh et al. has demonstrated that DJ-1, one of the most classical key players responsible for PD pathogenesis, is strongly linked with neuroimmunology and multiple autoimmune responses in PD . In addition, DJ-1-deficient animal models have shown compromised iTreg induction, cell cycle progression, and cell survival and proliferation. DJ-1/ iTregs are more proliferative, more susceptible to cell death signals and deficient in cell division compared with wild type counterparts, as analyzed by flow cytometry and Western blotting.
Introduction: Parkinsons Disease And Inflammation
Multiple studies have highlighted an association between sustained inflammation and a number of neurodegenerative diseases including Alzheimers disease , Parkinsons disease , amyotropic lateral sclerosis , and frontal temporal dementia . The role of inflammation in the pathogenesis of these disorders, however, remains undetermined. Here, we focus on the inflammatory features in PD, the most common movement disorder, affecting more than 10 million people worldwide . PD patients manifest motor symptoms including bradykinesia, rest tremor, muscular rigidity, and postural and gait impairment, as well as non-motor symptoms . Non-motor symptoms include mood disorders, cognitive impairments, and autonomic dysfunction, such as orthostatic hypotension and constipation . While alleles of many genes are associated with the disorder, PD remains largely a sporadic disorder associated with older age and various genetic and environmental risk factors .
PD is diagnosed from motor symptoms , but non-motor symptoms are often manifest during a prolonged prodromal phase as much as 20 years prior to the onset of the motor features . These prodromal non-motor symptoms include constipation, rapid eye movement sleep behavior disorder, depression, anosmia, and excessive daytime sleepiness . The sensitivity and the specificity of these non-motor symptoms limits their utility in predicting the development of PD .
You May Like: I Have Parkinsons Disease
Don’t Miss: What Are Some Early Signs Of Parkinson’s Disease
Parkinsons: Autoimmune Attack May Start Years Before Diagnosis
A new study adds to evidence that autoimmunity plays a role in the development of Parkinsons disease. The research also offers hope that early preventive treatment could offset the damage.
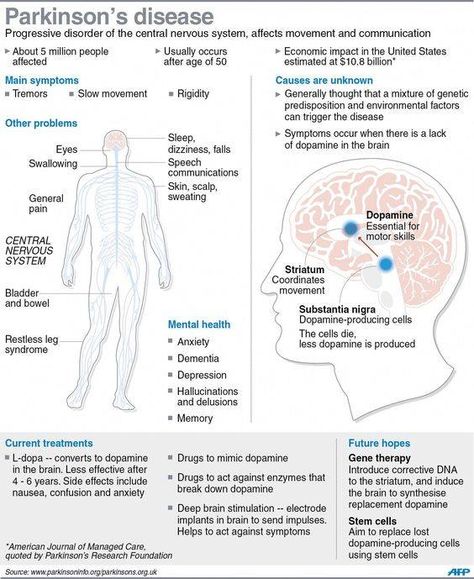
Parkinsons disease is a chronic, progressive disorder. Its characteristics tend to include tremor, rigidity, slowness of movement, and impaired balance.
Around 1 million people in the United States and 10 million people throughout the world have the disease.
Parkinsons results from a loss of nerve cells in a part of the brain called the substantia nigra. These cells produce dopamine, a chemical messenger, or neurotransmitter, involved in controlling movement.
Most people with Parkinsons are older than 50 when they receive the diagnosis, but some develop motor symptoms, involving problems with muscle control, at an earlier age.
Years before motor symptoms arise, other symptoms of Parkinsons can appear, including a reduced sense of smell, constipation, mood changes, and REM sleep behavior disorder, which involves physically acting out dreams.
The existence of these prediagnostic symptoms suggests that damage to dopamine-producing nerve cells begins long before the person experiences trouble with movement.
A new study spearheaded by researchers from the La Jolla Institute for Immunology , in California adds to evidence that the immune system may be responsible for the damage to nerve cells.
The Immune Response And Autoimmune Disease
Immune cells defend the body from outside invaders like toxins or germs that can cause infection. These outside substances that can harm the body are called antigens.
When the immune system detects an antigen, the normal immune response is to promote inflammation and produce small proteins called antibodies. The inflammatory reaction from the body helps to get immune cells moving, encouraging them to fight bacteria, respond to toxins, and heal injured tissue. Antibodies that recognize different types of antigens can bind with and neutralize their targets.
When the immune response becomes dysfunctional and starts to attack your tissues and cells, this is an autoimmune response. When an inflammatory reaction against your body becomes long term, autoimmune disorders can result.
Also Check: What Part Of The Brain Does Parkinson’s Disease Affect
What Are The Symptoms Of Parkinsons Disease
Imagine what it would feel like if you couldnât hold a fork, a glass of water, or a pen anymore due to extreme trembling. The first stages of Parkinsonâs are easily recognizable, beginning with slight tremors on one side of the body, a soft voice, a slow blink rate, loss of sense of smell, slow movements, and balance difficulties.
These are followed by subtle signs that affect daily living, such as a slight voice tremor, lip and jaw tremor, fixed facial expressions, and even tongue tremor, making it hard for the patients to speak properly. Usually, these symptoms appear when at least fifty percent of the neurons are lost, so the early stages of the disorder are harder to be recognized and have already begun affecting the patientâs quality of life.
Some of the most common Parkinsonâs disease symptoms are:
- Resting tremors
- Writing changes
- Balance problems
The late stages of the disease come with many health complications, such as gait freezing or even falling, dementia, delusions, or hallucinations. Patients in the last stage of Parkinsonâs are also susceptible to pneumonia, which can be deadly.
What Are The Early Warning Signs Of Parkinsons Disease
Parkinsons warning signs can be motor symptoms like slow movements, tremors or stiffness. However, they can also be non-motor symptoms. Many of the possible non-motor symptoms can appear years or even decades ahead of motor symptoms. However, non-motor symptoms can also be vague, making it difficult to connect them to Parkinsons disease.
Non-motor symptoms that might be early warning signs include:
Dont Miss: Does Sam Waterston Have Parkinson
You May Like: Sample Menu For Parkinson’s Disease
Talk With Others Who Understand
MyParkinsonsTeam is the social network for people with Parkinsons disease and their loved ones. On MyParkinsonsTeam, more than 88,000 members come together to ask questions, give advice, and share their stories with others who understand life with Parkinsons disease.
Do you still have questions about what causes Parkinsons? Share your experience in the comments below, or start a conversation by posting on your Activities page.
Evidence Of Autoimmunity In Parkinsons
Research by Columbia University and the La Jolla Institute for Allergy and Immunology in the United States has found evidence of the role that autoimmunity plays in Parkinsons disease. According to the study, the death of the neurons that cause this disease could be prevented by therapies that dampen the response of the immune system.
The researchers claim that two fragments of a protein that appears in the brain cells of people with Parkinsons, alpha-synuclein, can activate T cells. T cells play a role in autoimmune responses. Apparently, dopamine neurons, which play a role in the disease, are vulnerable to autoimmune attacks. This occurs because they have some proteins on the cell surface. These proteins help the immune system to recognise foreign substances. This confuses the T cells, which identify the neurons damaged by Parkinsons as invaders and attack them.
In the study, the researchers exposed 67 blood samples from patients with the disease and 36 healthy controls to alpha-synuclein fragments and other proteins found in neurons. In the blood of the controls, not much cellular immune activity was observed. However, in the patients samples, the T cells showed a strong response to the protein fragments.
Read Also: Does Exercise Help Parkinson’s
How Is It Treated And Is There A Cure
For now, Parkinsons disease is not curable, but there are multiple ways to manage its symptoms. The treatments can also vary from person to person, depending on their specific symptoms and how well certain treatments work. Medications are the primary way to treat this condition.
A secondary treatment option is a surgery to implant a device that will deliver a mild electrical current to part of your brain . There are also some experimental options, such as stem cell-based treatments, but their availability often varies, and many arent an option for people with Parkinsons disease.
Autoimmunity In Neurodegenerative Diseases And Its Relevance To Pd
Parkinson’s disease is actually an autoimmune disease. Autoimmunity occurs when immune homeostasis is broken by several main mechanisms shown in this figure, which directly result in an increase in error recognition and self-attack and a decrease in self-tolerance to autoantigens. Regarding PD, chronic autoimmune attack is not only its pathogenesis but also always involved throughout the entire disease process. Inflammation is the first step of this attack, with the subsequent participation of various immune cells and immunoglobulins they produce, ultimately leading to the death of dopaminergic neurons. PRRs, pattern recognition receptors CSF, cerebrospinal fluid SNpc, substantia nigra pars compacta IL, interleukin TNF, tumor necrosis factor.
You May Like: Does Parkinson’s Disease Run In Families
Implications For Diagnosis And Therapeutics
Understanding the extent of the role of the immune response in the pathogenesis of PD opens up new avenues of diagnosis and treatment for patients. Identifying people who are carriers of HLA alleles that place them at risk for -syn-specific T cells to be monitored can help early diagnosis and treatment of PD. In addition, -syn-specific T cells could be use as early biomarkers of the disease, identifying autoimmunity to self proteins prior to the onset of motor symptoms. Large-scale, longitudinal studies monitoring -syn reactivity and the development of PD would need to be conducted before establishing T cells as PD biomarkers.
Currently, new treatment avenues targeting the immune system are being tested on PD patients. Sargramostim is a human recombinant granulocyte-macrophage colony-stimulating factor approved by the Food and Drug Administration for the recovery of patients receiving bone marrow transplantation and cancer therapies . It functions by promoting myeloid recovery and inducing Treg responses . In a preliminary randomized, double-blind phase 1 clinical trial, Sargramostim-treated patients showed modest improvements after 6 and 8 weeks of treatment and increases in Treg numbers and function compared to PD patients receiving placebo . Further clinical investigation will shed light on the potential of immunomodulatory drugs for treatment of PD.
Blood Tests And Imaging
Blood tests and additional testing may help with diagnosis as they can identify elevated cholesterol levels and environmental toxins like carbon disulfide, herbicides, and pesticides present in the bloodstream.
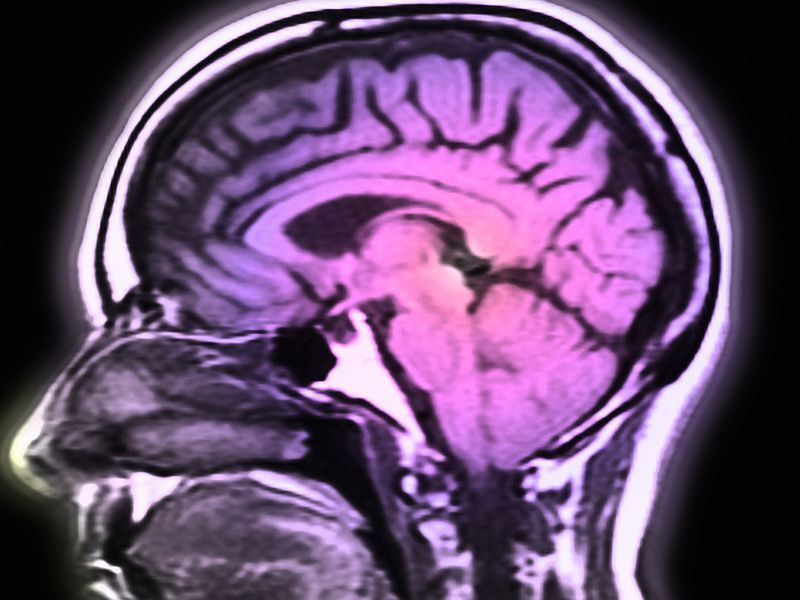
If a patient shows symptoms consistent with Parkinsonâs, their doctor may also order imaging tests such as MRI to search for neurological abnormalities and rule out other possible conditions. Head traumas, inflammation, and genetic mutations are also factors that can lead to the diagnosis of Parkinsonâs disease.
Read Also: What Are The Beginning Signs Of Parkinson’s
Inflammation In Pd Pathogenesis And Progression
Considering age is the greatest risk factor for many neurodegenerative diseases, the ageing of the immune system is the most underappreciated and understudied contributing factor in the neurodegeneration field. Immunosenescence is characterized by two primary features, namely an age-acquired immunodeficiency and . Inflammageing is characterized by excess low-level production of circulating inflammatory mediators, or cytokines most notably C-reactive protein , IL-6 and tumour necrosis factor from chronically stimulated innate and adaptive immune cells,,. Both the innate and adaptive immune systems lose competence with ageing and are also notably altered in PD, .
Fig. 2: Inflammatory manifestations in PD.
The figure highlights inflammatory manifestations that have been identified in patients with Parkinson disease . Intestinal dysbiosis and inflammation , increases in levels of circulating pro-inflammatory cytokines , innate and adaptive immune cell activation and changes in frequency , bloodbrain barrier permeability and peripheral immune cell infiltration of the central nervous system and neuroinflammation are hallmarks of a pro-inflammatory immune phenotype in PD. ROS, reactive oxygen species.
Facts About Parkinsons Disease
- Parkinsonâs disease is the second most common neurodegenerative disease after Alzheimerâs.
- Apart from motor symptoms that affect individuals with Parkinsonâs, non-motor symptoms include depression, constipation, genitourinary problems, and sleep problems.
- Drug-induced Parkinsonism is a condition that mimics the symptoms of Parkinsonâs disease and is typically induced by antipsychotic medication. While Parkinsonâs currently does not have a cure, symptoms of drug-induced parkinsonism subside within three months of cessation of treatment.
- Early-onset Parkinsonâs, or when symptoms set in before age 50, affects about four percent of Americans diagnosed with the condition and has been linked to specific genes in the individual, making it more likely to develop.
- Parkinsonâs symptoms can sometimes be confused with Essential Tremor , which causes uncontrollable shaking. ET is eighty times more common than Parkinsonâs, and though some scientists believe it to be linked to the future development of Parkinsonâs, more studies are still required.
You May Like: How Does Parkinson’s Disease Affect Homeostasis
