Peripheral Neuropathy And Parkinsons Disease
Today I will address the potential link between Parkinsons disease and a common neurologic condition called peripheral neuropathy. This topic was submitted via the Suggest a Topic portal. I am grateful for your suggestions so please continue to let us know what youd like to learn more about!
In order to understand what peripheral neuropathy is and what symptoms it can cause, we will briefly review the components of the nervous system.
Urinary Function Tests: Urodynamic Study And Sphincter Electromyography
Cystometric analysis of the storage phase indicates reduced bladder capacity with detrusor overactivity in PD as well as uninhibited external sphincter relaxation. These findings may be major contributing factors to an overactive bladder in PD.
The pressureflow analysis of the voiding phase in PD has shown a weak detrusor in 40% of male and 66% of female patients. A subset of PD patients had detrusor overactivity during the storage phase but weak detrusor on voiding. This condition, known as detrusor hyperactivity with impaired contractile function, has recently been estimated to occur in 18% of PD patients.
Detrusorexternal sphincter dyssynergia or pseudo-dyssynergia may be detected in PD, but the prevalence is considered to be low. In contrast, a pressureflow analysis revealed that half of PD patients show mild urethral obstruction. Sphincter electromyography indicates that neurogenic changes in sphincter motor unit potentials are not common in PD.
Future Perspective And Concluding Remarks
There is considerable evidence that autonomic dysfunction is an early feature of PD but no single autonomic abnormality predicts the disease with good reliability and sensitivity. With the exception of constipation, the identification of autonomic symptoms as predictive biomarkers of PD is still insufficiently developed. Other autonomic symptoms, such as swallowing dysfunction, sweating abnormalities, or pupillary dysfunction have not been systematically studied yet in the premotor phase, and may be areas for future research.
Some important limitations must be noted when assessing autonomic symptoms as potential biomarkers of the premotor phase of PD. First, signs and symptoms of significant autonomic dysfunction are not always present in the early stages of PD and only appear later in the disease process, which may indicate a low sensitivity as early predictors. Also, the specificity of some autonomic symptoms is probably low: for example, in the elderly, the prevalence of constipation is around 30%, compared with a prevalence of PD of around 12%. Moreover, autonomic dysfunction frequently occurs in common conditions such as diabetes, or as a side effect of medications and this can markedly reduce their specificity as predictive biomarkers.
Accurate recognition of predictive biomarkers of PD will allow the study of potential neuroprotective drugs at a stage when they may actually prevent the development of the motor features of PD.
You May Like: Does Parkinson’s Cause Hair Loss
What Does The Autonomic Nervous System Do
Your autonomic nervous system breaks down into three divisions, each with its own job:
- Sympathetic nervous system: This system activates body processes that help you in times of need, especially times of stress or danger. This system is responsible for your bodys fight-or-flight response.
- Parasympathetic nervous system: This part of your autonomic nervous system does the opposite of your sympathetic nervous system. This system is responsible for the rest-and-digest body processes.
- Enteric nervous system: This part of your autonomic nervous system manages how your body digests food.
Factors Associated With Autonomic Dysfunction
Since the occurrence of AutD is associated with multiple clinical symptoms as shown in Figure 2, a multivariate logistic regression analysis was performed to investigate potential predictors for AutD. NMSS was removed from the logistic regression model as it has shared domains with autonomic dysfunction and was considered to be a confounder of AutD. Additionally, wearing-off was deleted from the variable list due to its high risk of multicollinearity. Detailed results are shown in Supplementary Table 6. Variables that are not present in the logistic regression model are shown in Supplementary Table 7. The logistic regression model demonstrated that age , UPDRS total score , RBD , hyposmia , depression , and fatigue may be linked to PD with AutD. All related factors are shown in Table 3. In conjunction with the correlation analysis shown in Figure 2, the consistent positive correlations between AutD and either RBD, depression, or fatigue indicate that these symptoms are inclined to occur simultaneously, which may suggest a similar underlying mechanism between AutD and these symptoms. Differing from the partial correlation analysis, age of onset, motor symptom severity, and motor complications were not significant AutD predictors in the multivariate logistic regression model.
Table 3. Multivariate logistic regression analysis showing factors that related to PD with AutD.
Also Check: Can Acupuncture Help With Parkinson’s
Parkinsons Disease: Causes Symptoms And Treatments
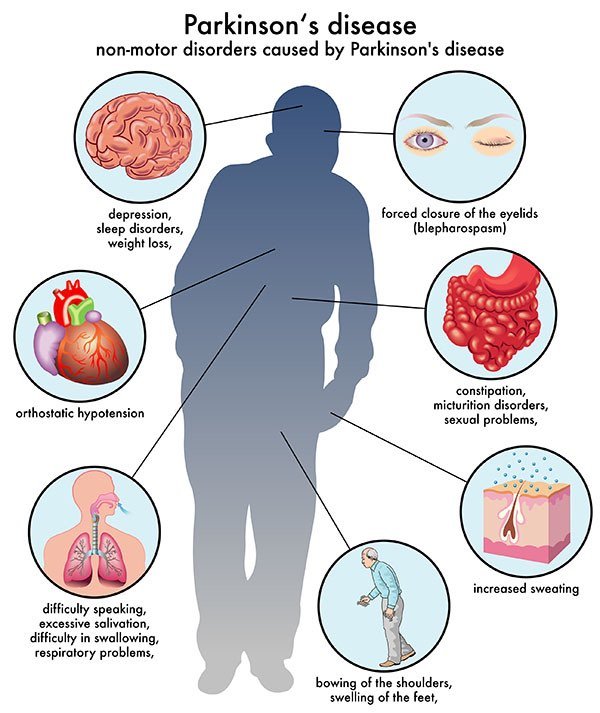
Parkinsons disease is a brain disorder that causes unintended or uncontrollable movements, such as shaking, stiffness, and difficulty with balance and coordination.
Symptoms usually begin gradually and worsen over time. As the disease progresses, people may have difficulty walking and talking. They may also have mental and behavioral changes, sleep problems, depression, memory difficulties, and fatigue.
While virtually anyone could be at risk for developing Parkinsons, some research studies suggest this disease affects more men than women. Its unclear why, but studies are underway to understand factors that may increase a persons risk. One clear risk is age: Although most people with Parkinsons first develop the disease after age 60, about 5% to 10% experience onset before the age of 50. Early-onset forms of Parkinsons are often, but not always, inherited, and some forms have been linked to specific gene mutations.
Definition Of Autonomic Dysfunction
Autonomic dysfunction was defined as a score greater than or equal to one in SCOPA-AUT. A score of zero was regarded as normal autonomic function. Each of the six autonomic domains was categorized as impaired when at least one of the related items was rated. Referring to Merola, patients were further divided into three subgroups according to the number of affected domains: without AutD, with single-domain AutD, and with multiple-domain AutD .
Also Check: Is Drooling A Symptom Of Parkinson’s Disease
The Peripheral Nervous System And Parkinsons Disease
It is well-established that the autonomic nervous system can be significantly affected in PD causing symptoms such as constipation, urinary dysfunction and orthostatic hypotension. The autonomic nerves that bring signals to the gut for example, can be directly affected by Lewy body-like accumulations and neurodegeneration.
What remains unclear is if motor and sensory nerves are also affected in PD.
Effect Of Deep Brain Stimulation On The Autonomic Nervous System
Deep brain stimulation of the subthalamic nucleus or the globus pallidus internus has become an established tool in the management of patients with advanced PD, and DBS of the STN allows reduction of the daily dose of antiparkinsonian drugs. DBS of the STN may improve autonomic dysfunction, such as bladder problems, gastric dysmotility and reduced emotional sweating. The improvement in autonomic dysfunction may be related to reduced antiparkinsonian drugs, improvement of motor disability and direct effects of DBS on STN and its neighbouring or connecting areas.
Read Also: Parkinson’s Disease And Muscle Spasms
What Are Some Interesting Facts About The Autonomic Nervous System
- Your sympathetic and parasympathetic systems create a balancing act. Your sympathetic nervous system activates body processes, and your parasympathetic deactivates or lowers them. That balance is key to your body’s well-being and your ongoing survival.
- It involves multiple forms of communication. Your nervous system uses chemical compounds produced by various glands in your body and brain as signals for communication. It also uses electrical energy in the neurons themselves. The neurons switch back and forth between electrical and chemical communication as needed.
- Your enteric nervous system is very complex. Some experts describe it as part of the overall nervous system instead of the autonomic nervous system. Thats because there are as many neurons in your enteric nervous system as there are in your spinal cord.
What Is Peripheral Neuropathy
Peripheral neuropathy is a condition in which there is damage to peripheral nerves. Symptoms depend on which type of nerves are affected and can result in:
- Pain or paresthesias in the limbs
The legs are more commonly affected than the arms because the nerves to the legs are longer than the arms and therefore more prone to damage.
Recommended Reading: What Causes Parkinson’s Disease
What Are Atypical Parkinsonian Disorders
Atypical Parkinsonian disorders are progressive diseases that present with some of the signs and symptoms of Parkinsons disease, but that generally do not respond well to drug treatment with levodopa. They are associated with abnormal protein buildup within brain cells.
The term refers to several conditions, each affecting particular parts of the brain and showing a characteristic course:
- Dementia with Lewy bodies, characterized by an abnormal accumulation of alpha-synuclein protein in brain cells
- Progressive supranuclear palsy, involving tau protein buildup affecting the frontal lobes, brainstem, cerebellum and substantia nigra
- Multiple system atrophy, another synucleinopathy that affects the autonomic nervous system , substantia nigra and at times the cerebellum
- Corticobasal syndrome, a rare tauopathy that typically affects one side of the body more than the other and makes it difficult for patients to see and navigate through space
What Is It Made Of
Your autonomic nervous system has a similar makeup to your overall nervous system. The main cell types are as follows, with more about them listed below:
- Neurons: These cells send and relay signals, and makeup parts of your brain, spinal cord and nerves. They also convert signals between the chemical and electrical forms.
- Glial cells: These cells dont transmit or relay nervous system signals. Instead, theyre helpers or support cells for the neurons.
- Nuclei: These are nerve cell clusters grouped together because they have the same jobs or connections.
- Ganglia: These, pronounced gang-lee-uh, are groups of related nerve cells . They usually dont all have the same jobs or connections, but theyre in roughly the same area or have connections to the same systems. Examples of this are the cochlear and vestibular ganglia, which are part of your senses of hearing and balance.
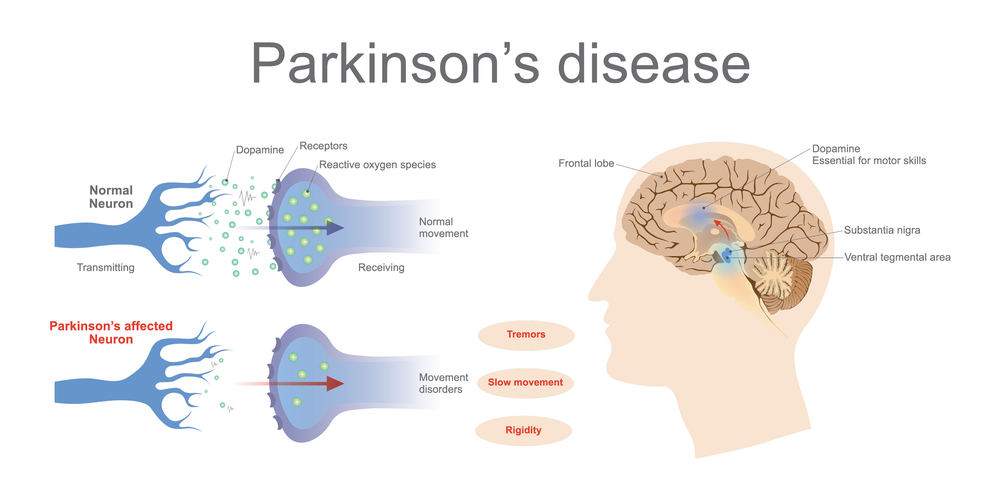
Neurons
Each neuron consists of the following:
- Cell body: This is the main part of the cell.
- Axon: This is a long, arm-like extension. At the end of an axon are several finger-like extensions where the electrical signal in the neuron becomes a chemical signal. These extensions, or synapses, connect with nearby nerve cells.
- Dendrites: These are small branch-like extensions on the cell body. Dendrites receive the chemical signals sent from synapses of other nearby neurons.
- Myelin: This is a thin layer composed of fatty compounds. Myelin is a protective covering that surrounds the axon of many neurons.
You May Like: How Do You Find Out If You Have Parkinson Disease
Parkinsonian Disorders And Levodopa
Various parkinsonian disorders can be categorized based on how they respond to the medication called levodopa. PD tends to respond well to levodopa therapies, while most atypical parkinsonian disorders do not. Sometimes people with parkinsonian symptoms who do not respond well to levodopa may be referred to as having parkinsonism. This can be confusing since parkinsonism technically refers to a set of movement symptoms, rather than a specific diagnosis.
Cardiovascular Symptoms And Signs
Postural symptoms
Orthostatic hypotension may cause considerable problems at various stages of PD and particularly in the advanced stages. It is defined as a fall in systolic blood pressure of 20mmHg or in diastolic blood pressure 10mmHg on either standing or head-up tilt to at least 60° degree within 3min. A drop of systolic blood pressure of 30mmHg has recently been suggested in patients with recumbent hypertension. Cerebral perfusion is maintained by autoregulation of cerebral blood flow if systemic blood pressure is within a certain range . Patients may not complain of postural symptoms due to cerebral hypoperfusion despite having orthostatic hypotension when their mean arterial pressure is above 60mmHg.
Supine hypertension
PD patients with orthostatic hypotension may also have supine hypertension, defined as a systolic blood pressure 150mmHg or diastolic blood pressure 90mmHg. This may be a problem, especially at night if they lie supine, with a reversal of the circadian change in blood pressure. Supine hypertension is usually asymptomatic, but some patients report headfullness or a throbbing headache while lying flat. It may contribute to ventricular hypertrophy, renal dysfunction and intracerebral haemorrhage. The mechanisms of supine hypertension include impaired baroreflex activity, inappropriate sympathetic tone while supine, altered endocrine systems and drugs used to reverse orthostatic hypotension.
Postprandial hypotension
Don’t Miss: How Can Parkinson’s Patients Gain Weight
Pathophysiological Basis Of Using Autonomic Dysfunction As Predictor Of Pd
Involvement of the dopaminergic nigrostriatal neurons underlies the motor deficits of PD. However, as shown by the staging system proposed by Braak and colleagues , the first stage of PD in the central nervous system involves deposition of -synuclein in the anterior olfactory nucleus and dorsal motor nucleus of the vagus. Peripheral autonomic ganglia may also be involved in this early stage 1. Stage 2 is characterized by involvement of the medulla oblongata and the pons. Stage 3 affects midbrain , and at Stages 46 cortical structures are affected. Additional studies suggest that peripheral postganglionic sympathetic denervation may occur even earlier , thus constituting the earliest stage of the disease, at least in certain patients . The fact that incidental LB may be present in peripheral autonomic neurons before a diagnosis of PD is made suggests that screening for specific autonomic abnormalities may detect the earliest stages of PD before it spreads to the CNS . This raises the possibility that tests of peripheral autonomic function may be used as clinical predictive biomarkers for PD.
Distribution of incidental Lewy bodies in elderly subjects without clinical evidence of parkinsonism or dementia
Data are those reported by Bloch and colleagues . Interestingly, the localization of Lewy bodies in this group was strikingly similar to those reported in PAF patients . Information regarding non-motor symptoms was not collected by Bloch et al.
Differentiating Premotor Pd From Premotor Msa
In up to 50% of patients with MSA severe autonomic abnormalities, most frequently OH and erectile dysfunction, precede the development of the movement disorder. This premotor, autonomic phase lasts on average 3 years followed by the insidious onset of parkinsonism, cerebellar ataxia or both. Only rarely this is the case in patients with PD, but when it occurs, premotor features of autonomic dysfunction are similar in PD to those preceding MSA. In contrast to PD, cardiac sympathetic innervation remains frequently intact in MSA, which can be ascertained by cardiac neuroimaging. Vocal cord palsy is frequent in patients with MSA and may lead to aspiration. Olfaction is usually preserved in MSA while it is frequently decreased early on, even in the premotor phase, in patients with PD.
Don’t Miss: Is Lewy Body Dementia Related To Parkinson’s
Effect Of Antiparkinsonian Treatment On The Autonomic Nervous System
Antiparkinsonian medication may cause autonomic dysfunction. In the periphery, a considerable amount of orally administrated L-dopa is transformed into dopamine, which is an important regulator of systemic blood pressure through vasodilation and decreased catecholamine release, and dopaminergic receptors are widely distributed throughout both the central and peripheral autonomic nervous systems. Therefore, L-dopa may affect cardiovascular function. However, the effect of oral levodopa, with or without a peripheral decarboxylase inhibitor , on blood pressure and orthostatic hypotension is controversial, although DCIs have been reported to have no effect on blood pressure. In healthy individuals, intravenous levodopa infusion has been reported to lower blood pressure whereas oral L-dopa with DCI does not. With regards to PD patients, in several previous studies, acute or chronic administration of oral L-dopa has not been shown to affect cardiovascular reflexes,, whereas some have shown that L-dopa produces mild orthostatic hypotension and lowers resting blood pressure., In contrast, one report has shown that orthostatic hypotension improved after 6months of oral L-dopa therapy.
Medication for non-motor symptoms may also affect autonomic function. -Adrenergic blockers, which may be used for urinary voiding problems, and antidepressants, also can aggravate orthostatic hypotension and constipation in PD patients.
Symptoms Of Peripheral Neuropathy
The symptoms of PN can be non-specific, and a person therefore may not be able to distinguish on their own whether his/her symptoms are due to PN or another condition. PN, however, often results in specific findings on a neurologic exam, such as decreased sensation to pin prick or vibration or the lack of ability to discern which way a toe is being pointed without looking. Other tests such as Electromyogram and Nerve conduction studies may be necessary to confirm the diagnosis. Small fiber neuropathy which typically causes pain, burning, tingling and/or numbness in the feet, may have normal EMG and NCS and a skin biopsy may be necessary to confirm the diagnosis. With the appropriate examination and supportive tests however, a neurologist should be able to distinguish the symptoms of peripheral neuropathy from other conditions, including PD, that may cause similar symptoms.
There are many known causes of PN including diabetes, vitamin deficiencies, certain infections, and autoimmune diseases. Many of these causes can be treated, so it is important to know if you do have PN and what the cause is. There are those people however, who have the signs and symptoms of PN, but no known cause can be identified.
Also Check: What Percentage Of Parkinson’s Patients Develop Dementia
Postural Orthostatic Tachycardia Syndrome
POTS affects anywhere from 1 to 3 million people in the United States. Nearly five times as many women have this condition compared to men. It can affect children, teenagers and adults. It can be also associated with other clinical conditions such as Ehlers-Danlos syndrome, an inherited condition of abnormal connective tissue.
POTS symptoms can range from mild to severe. Up to one out of four people with POTS have significant limitations in activity and are unable to work due to their condition.
Where Does The Autonomic Nervous System Fit In The Overall Structure Of The Nervous System
Your overall nervous system includes two main subsystems:
- Central nervous system: This includes your brain and spinal cord.
- Peripheral nervous system: This includes every part of your nervous system that isnt your brain and spinal cord.
Your peripheral nervous system also has two subsystems:
- Somatic nervous system: This includes muscles you can control, plus all the nerves throughout your body that carry information from your senses. That sensory information includes sound, smell, taste and touch. Vision doesnt fall under this because the parts of your eyes that manage your sight are part of your brain.
- Autonomic nervous system: This is the part of your nervous system that connects your brain to most of your internal organs.
Read Also: Is Vertigo A Symptom Of Parkinson’s Disease
