Why Has My Neurologist Prescribed Levodopa To Confirm My Diagnosis
Depending on your symptoms, your neurologist may ask you to take levodopa for a period of time.
Parkinsons disease is characterized by a deficiency of dopamine in the brain and mainly in the substantia nigra.Taking levodopa, a precursor to dopamine, can reverse the symptoms of Parkinsons disease. One dose is not enough. You will need to take several weeks of treatment with increasing doses until you get a result that will confirm your diagnosis.This test, when negative, can also invalidate the trail of other diseases related to Parkinsons disease
What Happens At The Exam
If your doctor thinks you might have Parkinsonâs disease, theyll recommend that you see a specialist who works with nervous system issues, called a neurologist. One whoâs also trained in movement disorders, like Parkinsonâs, may be able to make the right diagnosis faster.
Your neurologist will probably want to see how well your arms and legs move and check your muscle tone and balance.
They may ask you to get out of a chair without using your arms for support, for example. They also may ask a few questions:
- What other medical conditions do you have now or have you had in the past?
- What medications do you take?
- Has your handwriting gotten smaller?
- Do you have trouble with buttons or getting dressed?
- Do your feet feel âstuckâ to the floor when you try to walk or turn?
- Do people say your voice is softer or your speech is slurred?
Tell your doctor if youâve noticed a change in your sense of smell or you have trouble with sleep, memory, or mood.
Parkinsonâs disease can look different from person to person. Many people have some symptoms and not others.
How Do I Prevent Falls From Common Hazards
- Floors: Remove all loose wires, cords, and throw rugs. Minimize clutter. Make sure rugs are anchored and smooth. Keep furniture in its usual place.
- Bathroom: Install grab bars and non-skid tape in the tub or shower. Use non-skid bath mats on the floor or install wall-to-wall carpeting.
- Lighting: Make sure halls, stairways, and entrances are well-lit. Install a night light in your bathroom or hallway and staircase. Turn lights on if you get up in the middle of the night. Make sure lamps or light switches are within reach of the bed if you have to get up during the night.
- Kitchen: Install non-skid rubber mats near the sink and stove. Clean spills immediately.
- Stairs: Make sure treads, rails, and rugs are secure. Install a rail on both sides of the stairs. If stairs are a threat, it might be helpful to arrange most of your activities on the lower level to reduce the number of times you must climb the stairs.
- Entrances and doorways: Install metal handles on the walls adjacent to the doorknobs of all doors to make it more secure as you travel through the doorway.
Recommended Reading: Life Expectancy After Parkinson’s Diagnosis
Gait & Balance Abnormalities
Parkinsons Disease Exam
Patients with Parkinsons disease can develop an alteration of the postural reflexes that causes instability in gait and balance control. Such alterations usually develop later in the course of the illness and are a major cause of disability, especially because of the high risk for falls that derives.
Using the exam to pick up postural instability is of the utmost importance for the management of patients with PD, since it will trigger either a medication adjustment or a physical therapy intervention both aimed at falls prevention.
We have three tests for this part of the PD exam:
1);;;; Standing up from a chair
2);;;; Free walking
3);;;; Provoked pull test maneuver for balance
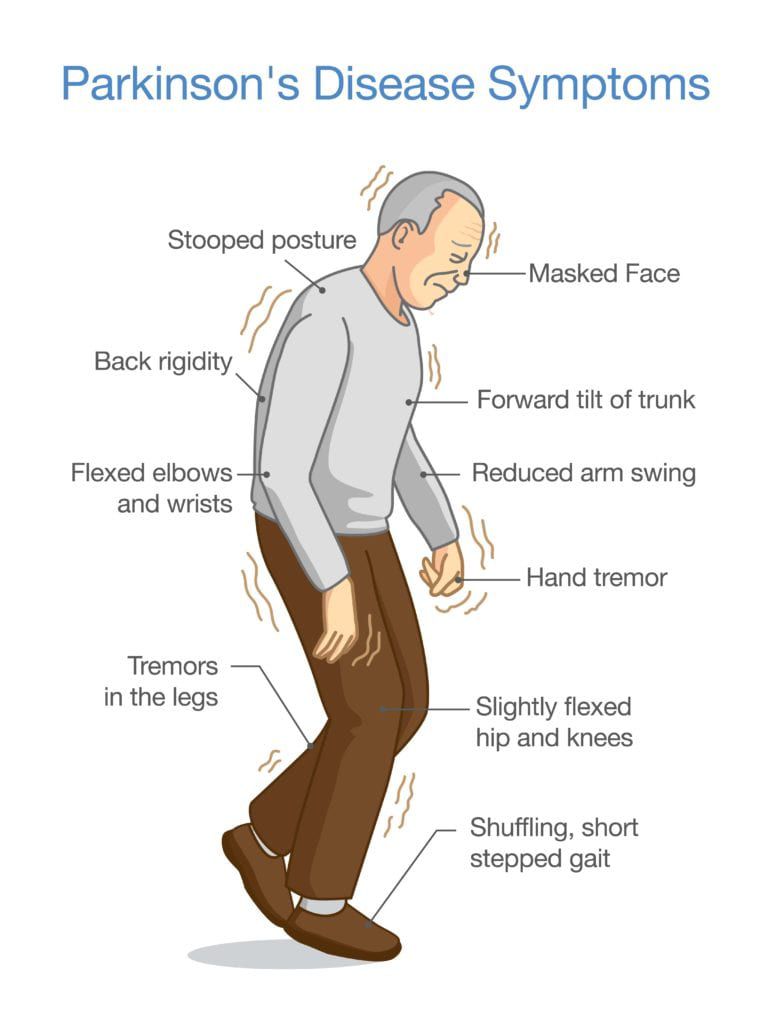
Parkinsons Disease Symptoms Diagnosis Stages And Treatment
April 23, 2019 By Heather
You cant speak coherently, the left side of your body is involuntarily shaking, and sudden random painful muscle spasms keep happening all at once. This is how stages 3 and 4 of Parkinsons disease can debilitate you.
Parkinsons disease may begin as an innocuous tremor that over time leaves a person completely debilitated. As of yet, there is no known cure. However, early recognition of the symptoms and proactive treatments can slow it down.
In this yourfootpalace.com article, we define and explain what Parkinsons disease is, how to identify its symptoms, how a diagnosis is made, and the stages a person passes through during the progression of the disease.
Read Also: What Is The Life Expectancy Of Someone With Parkinson’s Disease
Living With Parkinson’s Disease
As Parkinson’s develops, a person who has it may slow down and won’t be able to move or talk quickly. Sometimes, speech therapy and occupational therapy are needed. This may sound silly, but someone who has Parkinson’s disease may need to learn how to fall down safely.
If getting dressed is hard for a person with Parkinson’s, clothing with Velcro and elastic can be easier to use than buttons and zippers. The person also might need to have railings installed around the house to prevent falls.
If you know someone who has Parkinson’s disease, you can help by being a good friend.
Elimination Of Other Conditions
Although no test can diagnose Parkinson’s disease itself, your doctor may order blood tests or imaging studies to rule out other causes of your symptoms.
Your doctor will want to know about any medication or recreational drugs you take, since some drugs can cause symptoms similar to those of Parkinson’s.
Parkinson’s disease;doesn’t show up on radiological studies like;X-ray,;MRI;, or CT scans.
Doctors sometimes order;dopamine;transporter SPECT imaging to determine whether a person with suspected Parkinson’s has a different disorder called essential tremor.
Read Also: What Color Represents Parkinson’s Disease
How Can I Try To Get An Early Diagnosis
By the time Parkinsons causes noticeable motor symptoms, usually about 50 percent of the cells that produce dopamine in your substantia nigra have already died off. Non-motor symptoms, such as constipation, loss of smell, or restless sleep, often appear before motor symptoms.
Theres still debate among medical professionals on how long non-motor symptoms may appear before an individual has noticeable changes in their movement. Its thought that they could appear years to decades beforehand.
But a formal Parkinsons diagnosis requires the symptom slowness of movement. In the time before this symptom appears, your doctor cant make a Parkinsons diagnosis, but they may alert you that youre at a high risk of developing Parkinsons in the future if these or other symptoms appear at any point.
Likelihood Of Referral According To Final Diagnosis
Overall, 74% of all cases with a diagnosis of Parkinson’s disease had been seen by a specialist. However, when these cases were classified by final diagnosis , it was observed that, paradoxically, fewer cases with atypical disease had been seen by a specialist compared with those with classical Parkinson’s disease ; p = 0.02).
You May Like: What Is The Life Expectancy Of Someone With Parkinson’s Disease
Depression May Be An Early Symptom Of Parkinsons
Depression is one of the most common, and most disabling, non-motor symptoms of Parkinsons disease. As many as 50 per cent of people with Parkinsons experience the symptoms of clinical depression at some stage of the disease. Some people experience depression up to a decade or more before experiencing any motor symptoms of Parkinsons.
Clinical depression and anxiety are underdiagnosed symptoms of Parkinsons. Researchers believe that depression and anxiety in Parkinsons disease may be due to chemical and physical changes in the area of the brain that affect mood as well as movement. These changes are caused by the disease itself.
Here are some suggestions to help identify depression in Parkinsons:
- Mention changes in mood to your physician if they do not ask you about these conditions.
- Complete our;Geriatric Depression Scale-15;to record your feelings so you can discuss symptoms with your doctor. Download the answer key and compare your responses.
- delusions and impulse control disorders
Living With Parkinsons Disease
Without being proactive in seeking medical attention and treatment, later stages of Parkinsons disease can be a living nightmare full of uncertainty, confusion, and hallucinations.
In this article, you discovered the definition of Parkinsons disease, the symptoms that accompany it, how a diagnosis is made, its 5 stages, and its treatment options.
Dont allow minor symptoms to develop into major health issues. Ignoring little aches and pains and self-diagnosing could lead to life-long regrets. When there are signs of trouble, seek help from your primary care physician.
Also Check: Parkinson Disease Lifespan
Sensitivity Specificity And Predictive Value Of A Previous Diagnosis Of Parkinson’s Disease
Of 126 patients with a pre-existing clinical diagnosis of probable and possible Parkinson’s disease in the overall sample , 111 were confirmed as having Parkinson’s disease, resulting in a sensitivity of 88.1% ; similarly, it was confirmed that 54 of 74 patients did not have Parkinson’s disease, resulting in a specificity of 73.0% . The positive and negative predictive values of a previous clinical diagnosis of Parkinson’s disease were 84.7% and 78.3% . In other words, in 85% of patients with a previous diagnosis of Parkinson’s disease this diagnosis was confirmed, and 78% of patients with a diagnosis other than Parkinson’s disease did not have the disease .
When this was broken down by a specialist or other doctor diagnosis, the diagnostic validity was as follows. Neurologists and geriatricians had a sensitivity and specificity of 93.5% and 64.5% , respectively, compared with 73.5% and 79.1% for non-specialists. The positive predictive values were greater for specialists than for other doctors , but the negative predictive values were equivalent v non-specialist 79.1% ).
Who Are The Specialists In The Treatment Of Parkinson’s Disease In Quebec

The doctors who treat Parkinsons disease are neurologists. Some of them are specialized and work in clinics for movement disorders.
In these clinics, interdisciplinary teams made up of health professionals, such as physiotherapists, speech therapists, specialist nurses, can help you manage the symptoms of the disease as they appear.
Read Also: How Long Does It Take For Parkinson’s Disease To Progress
Is A Diagnostic Error Possible
About 25% of people who are diagnosed with Parkinsons disease do not have it. If your diagnosis was made by your general practitioner, it is important to see a neurologist.
If it was a general neurologist who made the diagnosis, you might be interested in meeting with a neurologist who specializes in movement disorders. Because they are trained to specifically diagnose and treat movement disorders. They are better equipped to distinguish Parkinsons disease from other related diseases with similar symptoms.
I Do My Best To Remain Optimistic And Cling To The Fact That The Parkinsons Diagnosis Is Overturned
Neurologists told me that the three drug components of Stalevo would be out of my system within a few weeks, but my brain only felt clear in February 2016 four months after Id stopped taking it. The huge range of motor and non-motor symptoms persists and other new ones have arrived since my body stopped receiving the added, yet unnecessary, dopamine. I do my best to remain optimistic and cling to the fact that the Parkinsons diagnosis is overturned.
Look out for another article by Joanne in the coming weeks, discussing the issue of misdiagnosis in more;depth. Joanne has written about her experiences on her blog here
Don’t Miss: How To Take Mannitol For Parkinson’s
What Medications Are Used To Treat Parkinsons Disease
Medications are the main treatment method for patients with Parkinsons disease. Your doctor will work closely with you to develop a treatment plan best suited for you based on the severity of your disease at the time of diagnosis, side effects of the drug class and success or failure of symptom control of the medications you try.
Medications combat Parkinsons disease by:
- Helping nerve cells in the brain make dopamine.
- Mimicking the effects of dopamine in the brain.
- Blocking an enzyme that breaks down dopamine in the brain.
- Reducing some specific symptoms of Parkinsons disease.
Levodopa: Levodopa is a main treatment for the slowness of movement, tremor, and stiffness symptoms of Parkinsons disease. Nerve cells use levodopa to make dopamine, which replenishes the low amount found in the brain of persons with Parkinsons disease. Levodopa is usually taken with carbidopa to allow more levodopa to reach the brain and to prevent or reduce the nausea and vomiting, low blood pressure and other side effects of levodopa. Sinemet® is available in an immediate release formula and a long-acting, controlled release formula. Rytary® is a newer version of levodopa/carbidopa that is a longer-acting capsule. The newest addition is Inbrija®, which is inhaled levodopa. It is used by people already taking regular carbidopa/levodopa for when they have off episodes .
Shifting Abilities Role Reversals
- People with PD often need more time to perform activities because of changes in hand coordination, muscle stiffness or slowness. Conflict may arise as it becomes necessary to reevaluate who is responsible for what tasks in the family and around the home.
- Changing abilities and assuming new roles can cause frustration and emotional upheaval.
- Stress makes PD symptoms worse.
What to do
- Maintain open communication with your loved ones.
- Prioritize daily tasks. Get outside help as needed for some tasks such as yard work, housecleaning or home maintenance.
- Regular exercise can help manage stress.
- Seek help from a counselor to resolve relationship conflicts.
Don’t Miss: Stages Of Parkinson Disease Life Expectancy
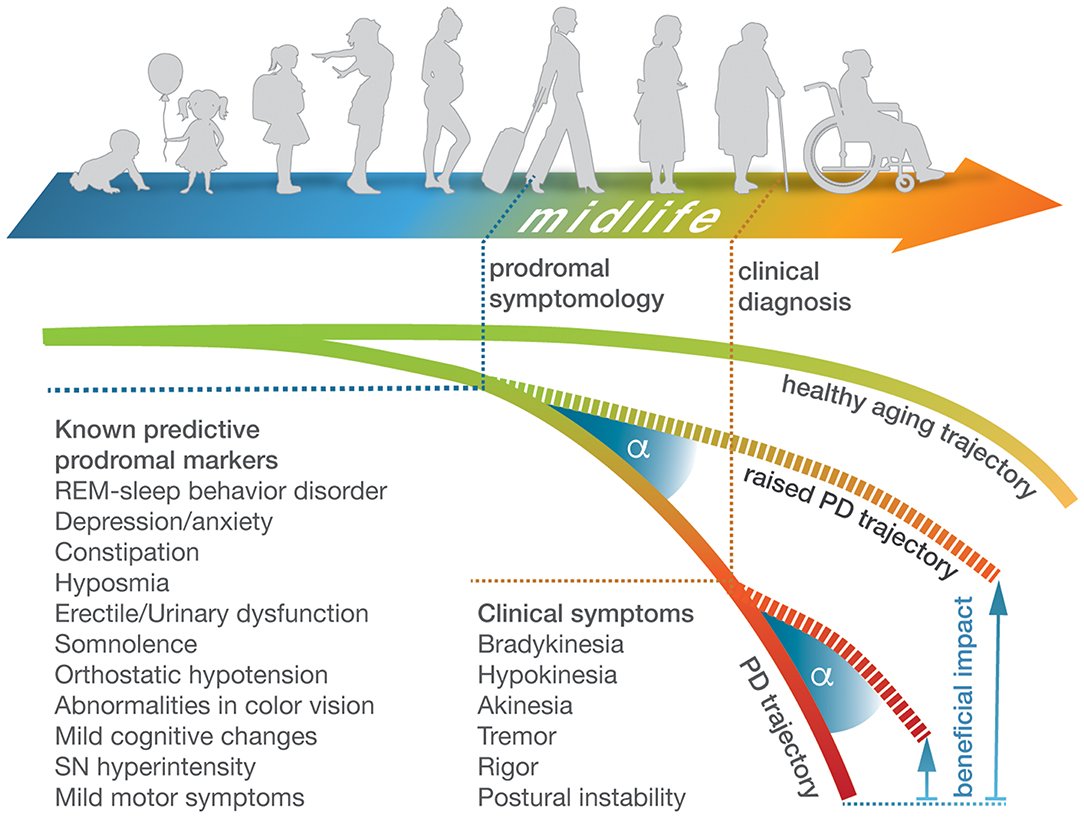
When Pd Starts: Can We Diagnose Parkinson Disease Before The Onset Of Motor Symptoms
A 53-year-old man, C.D., came to my clinic recently complaining of intermittent tremor of the right hand for the last six months. He had felt more tired than usual and was moving slowly during the previous year. His hand writing was getting small. When asked, he admitted that he had lost his sense of smell, and had constipation for at least a decade. He had experienced several episodes of violent nightmares during which he shouted and moved around and on one occasion hit his wife presumably thinking she was attacking him. Episodes like this had occurred frequently for more than 15 years. ;On examination, unilateral rest tremor was obvious and I diagnosed him with Parkinsons disease.
A decade ago, most neurologists, if asked, would have said that C.D.s PD had started about six months to one year before the onset of tremor. However, remarkable clinical investigations that have taken place in recent years have changed our minds and most of us would now establish the onset of PD in C.D.;at least 15 years before the onset of tremor.;
While advances in our understanding of pre-motor PD have been enormous, diagnosis of PD at this early stage still remains difficult, if not impossible.
__________________________________________________________
Ideas and opinions expressed in this post reflect that of the author solely. They do not necessarily reflect the opinions of the World Parkinson Coalition®
What Tests Will My Neurologist Do To Diagnose Parkinson’s Disease
First, your neurologist will ask you about your medical history and the symptoms you have observed.
Then, he will examine you by looking for common signs of the disease through simple activities such as:
- Writing
- The speech
- Dexterity exercises with your fingers
Your neurologist will also assess your tremors, the stiffness of your limbs, the speed of your movement, and test your ability to maintain your balance.
During this exam, your neurologist will also try to rule out other possible causes for your symptoms.
Also Check: Essential Oils Parkinsons
Testing For Parkinsons Disease
There is no lab or imaging test that is recommended or definitive for Parkinsons disease. However, in 2011, the U.S. Food and Drug Administration approved an imaging scan called the DaTscan. This technique allows doctors to see detailed pictures of the brains dopamine system.
A DaTscan involves an injection of a small amount of a radioactive drug and a machine called a single-photon emission computed tomography scanner, similar to an MRI.
The drug binds to dopamine transmitters in the brain, showing where in the brain dopaminergic neurons are.
The results of a DaTscan cant show that you have Parkinsons, but they can help your doctor confirm a diagnosis or rule out a Parkinsons mimic.
Passive Manipulation Of Limbs
To test for the presence of rigidity, we need to passively manipulate the limbs of the patient. However, If the disease is in its early stage or the symptoms are well controlled with medications, we may not be able to see rigidity. We will need to use some activation maneuvers, that basically consist in performing repetitive movements with the limb contralateral to the one that is being tested.
Also, there are two types of rigidity:
-;;;;;; Lead-pipe rigidity: where the tone is uniformly and smoothly increased throughout the entire range of movement
-;;;;;; Cogwheel rigidity: where a tremor is superimposed on the hypertonia, making the movement irregular due to intermittent increase and reduction of tone
Upper Extremity Testing
For the upper extremity the most sensitive joint where to check for rigidity is the wrist. To uncover rigidity, passively rotate the wrist and feel for a resistance to the movement. It is very important that the arm of the patient is fully relaxed when rotating the wrist. To do this, place your proximal hand under the patients forearm, while your distal hand grabs and rotates the wrist of the patient. When rigidity is present, the range of motion will be preserved but you will feel a resistance in performing the movement.
Wrist rotation with activation maneuver.
It is also possible to test for rigidity in the elbow by passively flexing and extending the forearm.
Elbow flexion-extension with activation maneuver.
Lower Extremity Testing
Also Check: What Is The Life Expectancy Of Someone With Parkinson’s Disease
How A Diagnosis Is Made
The bedside examination by a neurologist remains the first and most important diagnostic tool for Parkinsons disease . Researchers are working to develop a standard biological marker such as a blood test or an imaging scan that is sensitive and specific for Parkinsons disease.
A neurologist will make the diagnosis based on:
- A detailed history of symptoms, medical problems, current and past medications. Certain medical conditions, as well as some medications, can cause symptoms similar to Parkinsons.
- A detailed neurological examination during which a neurologist will ask you to perform tasks to assess the agility of arms and legs, muscle tone, gait and balance, to see if:
- Expression and speech are animated.
- Tremor can be observed in your extremities at rest or in action.
- There is stiffness in extremities or neck.
- You can maintain your balance and examine your posture.
