Are You A Candidate
To be eligible for this treatment, you must answer yes to all of the following questions:
- Have you been diagnosed with essential tremor?
- Have you tried at least two medications for your tremor?
- Does your tremor affect your quality of life?
- Would you be comfortable lying still in an MRI scanner for two to three hours?
- Are you over the age of 22?
If you meet all five criteria, you may be a candidate for treatment with focused ultrasound. Please have your doctor fax or email us a referral and a copy of your insurance card. For more information, feel free to give us a call.
Read Also: End Stage Parkinson Disease Symptoms & Contorted Body
First Hospital Based Focused Ultrasound Incisionless Procedure For Parkinsons & Essential Tremors In The Region Takes Place At Delray Medical Center
Dr. Lloyd Zucker, neurosurgeon and medical director of neurosurgery, completes first case
Delray Beach, FL Delray Medical Center is now the first hospital in the region to treat a patient with the new MR-guided focused ultrasound by INSIGHTEC. This technology is a scalpel-free treatment for essential tremor and medication-refractory tremor-dominant Parkinsons disease. This device uses sound wave energy to treat brain tissue as the source of the tremor and there is no surgical incision or anesthesia necessary.
I am honored to be able to not only treat the first patient at Delray Medical Center with this new groundbreaking procedure, but the first in any hospital in the region. We are now able to give those who suffer from this disease a chance to get back to living their lives, and pursuing their daily activities, said Dr. Lloyd Zucker, medical director of neurosurgery for Delray Medical Center. We are at an exciting time in medicine when it comes to treating neuro-disorders, and this technology is a game changer for patients who have suffered from Parkinsons disease.
The MR-guided focused ultrasound combines two technologies, magnetic resonance imaging , which pinpoints the exact location in the brain responsible for the tremor, and ultrasound, which precisely delivers over 1,000 highly focused beams of acoustic energy at that exact location without damaging any surrounding brain tissue.
Some of the benefits to this technology include:
Three Advantages Of Mrgfus For Pd Tremor
MRgFUS is a noninvasive outpatient procedure. No scalpel is needed to cut skin, no drill is needed to bore a hole in the skull, and nothing is implanted in the brain. Its three main advantages for PD-related tremor are:
A few words of caution: MRgFUS is not effective in every case. As with MRgFUS for ET, treatment will be directed to the hand in which tremor is worse, since treating both hands increases the risk of side effects. Clinical studies show that some patients have short term side effect such as headaches, dizziness or nausea but these quickly resolve. However, the effect may not be durable. Patients who have suffered with significant tremor for years may experience less effective tremor control, or gradual recurrence of tremor. Finally, MRgFUS does not cure PD, nor will it have an effect on other PD-related problems.
However, the consensus among researchers is that MRgFUS is a very promising treatment for PD-related tremor, especially as an alternative to invasive surgical procedures. If you or a loved one suffers from severe PD tremors, contact the Sperling Medical Group for more information about MRgFUS.
- CATEGORY:
Recommended Reading: Sam Waterston Parkinsons
Don’t Miss: Alzheimer’s Vs Parkinson’s
Prevalence Incidence And Risk Factors For Motor Complications
Nearly all patients develop motor fluctuations and LID by 15 to 20 years from time of diagnosis . However, prevalence and incidence figures through the course of PD vary depending on the study methodology employed and by the predominant treatment strategies of the time. Early literature suggested that approximately 10% of patients per year following initiation of treatment with levodopa develop motor fluctuations, with 40% of patients developing these complications within 46 years of treatment . A large cross-sectional study of 617 patients with PD found an overall prevalence of wearing off of 57% as assessed by neurologists and 67% as assessed by a patient-completed questionnaire . Of patients with disease duration < 2.5 years, wearing off was identified in 41.8% by the WOQ-19 and in 21.8% by neurologists, indicating that motor fluctuations can emerge as early as several months to a few years after the initiation of levodopa, as has also been observed in other studies . A retrospective analysis of an incident cohort of PD found estimated rates of dyskinesia of 30% by 5 treatment years and 59% by 10 treatment years .
Continuous Subcutaneous Apomorphine Infusion
Apomorphine is a dopamine agonist with a mixed affinity for D1 and D2 receptors and an affinity for serotonergic and alpha-adrenergic receptors . While the motor efficacy of apomorphine is similar to that of levodopa, apomorphine cannot be administered orally due to its low oral bioavailability . Subcutaneous infusions have a similar pharmacokinetic profile to the intravenous route. Compared with intermittent subcutaneous injections, CSAI has a longer apparent plasma half-life and simulates the physiological stimulation of striatal neurons .
Clinical outcomes of CSAI
In the OPTIPUMP cohort study, the efficacy and safety of CSAI were assessed. The total UPDRS score showed significant improvement in all patients at 6 months. UPDRS-III decreased in the on-medication state by 16.3% . In the first prospective, randomized, placebo-controlled trial to investigate the efficacy and safety of apomorphine subcutaneous infusion in PD patients, a daily off time reduction of 1.89h from a baseline of 6.69h was seen in treated patients, while there was an increase of 1.97h in on time without TSD from a baseline of 8.52h . In a retrospective study, 230 patients were treated with CSAI over 10 years. In this cohort, the daily off hours were reduced from 5.4 to 1.2h .
Safety of CSAI
Patient considerations for CSAI
Also Check: How Does A Person Get Parkinson’s Disease
What Is Parkinsons Disease
Parkinsons disease is a nervous system disease that affects your ability to control movement. The disease usually starts out slowly and worsens over time. If you have Parkinsons disease, you may shake, have muscle stiffness, and have trouble walking and maintaining your balance and coordination. As the disease worsens, you may have trouble talking, sleeping, have mental and memory problems, experience behavioral changes and have other symptoms.
Recommended Reading: Parkinsons And Bad Taste In Mouth
Individuals With Pd At Risk For Nursing Home Placement
In clinical practice, a person with PD is frequently housed in a nursing home when nonmotor symptoms such as hallucinations, psychosis, and dementia, as well as motor symptoms progress to the point where they interfere with When an individual is diagnosed with Parkinsons disease, their long-term progess is heavily influenced by their stage of the disease, their overall health, and their age. Almost all people suffering from Parkinsons disease have a normal or near-normal life expectancy. Despite the fact that Parkinsons disease is still a serious and disabling illness, people who suffer from it should always consult with their healthcare providers about how to manage their symptoms and take care of their health.
You May Like: Skin Test For Parkinson’s Disease
Focused Ultrasound Vs Deep Brain Stimulation
Focused ultrasound and deep brain stimulation are both surgical procedures that aim to ease Parkinsons movement symptoms or dyskinesia. These therapies may be options for people who get a good response to levodopa but have complications, such as dyskinesia or off time. Or, they may be a consideration for people who have tremor that cannot be controlled with medication.
Focused ultrasound and DBS work in the same brain areas but in different ways. FUS destroys cells and DBS delivers small electrical pulses to those same cells to interrupt abnormal signaling. FUS is permanent and irreversible, while DBS may be reversed by removing the system or turning it off. Focused ultrasound is non-invasive there are no incisions and there is no hardware placed in the body. In DBS surgery, doctors insert thin wires into the brain and a battery below the collarbone. For both FUS and DBS, a patient typically is awake, but some centers now offer asleep DBS. FUS is a one-time procedure that does not require adjustment. DBS needs regular programming to find the right electrical stimulation settings to maximize benefit and limit side effects.
Focused Ultrasound For Parkinsons Disease
Although elective procedures are currently being postponed in hospitals across the country because of the necessary focus on COVID-19, eventually our hospitals will return to normal and non-emergent procedures will be performed again. This will include elective procedures for the treatment of Parkinsons disease .
Two brain procedures that are approved for use in PD are deep brain stimulation and high intensity focused ultrasound . I encourage you to read more about DBS and view our webinar which outlines the newest features of this procedure.
Recommended Reading: Does Parkinson’s Cause Headaches
Ultrasound Treatment For Essential Tremor Still Effective After Five Years
A scalpel-free, high-tech form of brain surgery pioneered at UVA Health offers long-term relief for patients with essential tremor, a common movement disorder, even five years after treatment, a study shows.
The study offers important insights into the long-term effectiveness of ultrasound treatments for essential tremor. Five years after treatment, clinical trial participants continued to see treated tremors reduced by more than 70%, the researchers report. There were no progressive or delayed complications.
It is exciting to see such durable results after an outpatient procedure for a sometimes-disabling problem like ET, said researcher Dr. Jeff Elias, a UVA Health neurosurgeon who served as the studys principal investigator. It is important to note that most of the patients had very long-lasting benefits, but there are some cases where tremor can recur.
Dr. Jeff Elias said he is excited by the results showing a more than 70% reduction in symptoms after five years, but noted that tremor can recur in some cases.
The focused ultrasound procedure focuses sound waves inside the brain to disrupt faulty brain circuits that cause unwanted movement. Unlike traditional brain surgery, it does not require incisions or opening the skull. The minimally invasive procedure is guided by magnetic resonance imaging, so doctors can pinpoint the exact right spot in the brain before delivering the treatment.
How Does Focused Ultrasound Work
We use ultrasound to ablate the part of your brain that causes tremor. Using ultrasound means:
- No incisions. This technology lets us perform brain surgery without any cutting. This means no risk of bruising, bleeding or infection.
- Precision and accuracy. This technology lets us create a small lesion in the exact right place. Thousands of ultrasound waves come together in one place smaller than a millimeter. This creates enough heat to cause a lesion.
- Immediate feedback. Throughout the procedure, we test for improvement of your tremor symptoms so we know exactly when the procedure is complete.
Also Check: Who Is At Risk For Parkinson’s Disease
A New Era For Parkinsons Disease Treatment
A diagnosis of Parkinsons disease no longer automatically portends a future of extremely limited physical capabilities. Thanks to the commitment of researchers like Dr. Eisenberg and Dr. Fishmanand clinical trial participants like Steve Squirestreatment has expanded to include non-invasive options that significantly reduce certain symptoms within minutes and transform the lives of people who had been living with debilitating symptoms, said Bert W. OMalley, MD, President and CEO of the University of Maryland Medical Center.
Our school of medicine researchers have established themselves as world leaders in pioneering MRI-guided focused ultrasound for many devastating brain diseases, including Parkinsons and essential tremors, said E. Albert Reece, MD, PhD, MBA, Executive Vice President for Medical Affairs, UM Baltimore, and the John Z. and Akiko K. Bowers Distinguished Professor and Dean, University of Maryland School of Medicine. The stellar work of Dr. Eisenberg and Dr. Fishman has led to a new era in which this breakthrough modality has now become the standard of care for patients looking for less invasive treatments for their symptoms.
Fda Approves Focused Ultrasound For Parkinsons Symptoms
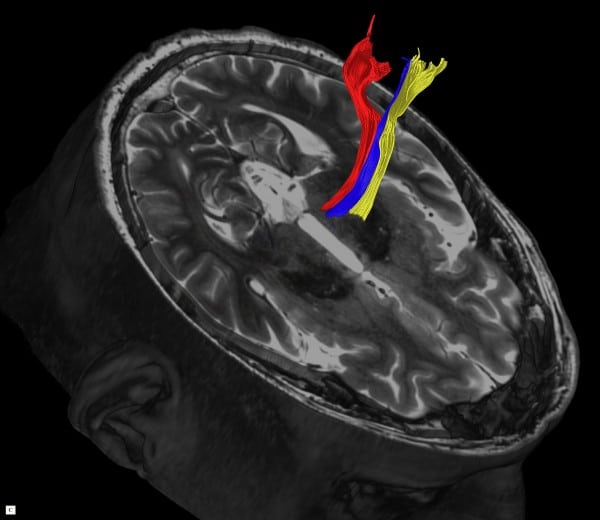
Jeff Elias, MD, pioneered the use of focused ultrasound for the treatment of essential tremor and Parkinsons disease.
The federal Food and Drug Administration has approved an incisionless form of brain surgery to treat advanced Parkinsons disease after successful testing at the School of Medicine and other sites.
The authorization allows the use of Insightecs Exablate Neuro focused ultrasound device to treat problems with mobility, rigidity and involuntary movements known as dyskinesias that are common in Parkinsons. UVA is one of only 37 medical centers in the country with the capacity to offer this minimally invasive treatment, according to the Charlottesville-based Focused Ultrasound Foundation, a longtime supporter of UVAs pioneering research into the many potential applications of the technology.
Prior to the approval, available treatments for the Parkinsons symptoms included drugs, which not all patients respond to, and invasive deep-brain surgeries. Focused ultrasound, in comparison, does not require incisions or cutting into the skull. Instead, the technology focuses sound waves inside the brain to interrupt faulty brain circuits, much like a magnifying glass can focus light to create heat. During the focused ultrasound procedure, doctors use magnetic-resonance imaging to peer inside the brain in real-time before making any permanent changes, helping ensure patients get the best possible outcomes.
Also Check: Treatment Of Dyskinesia In Parkinsons Disease
Also Check: How Does Parkinson’s Disease Affect Homeostasis
Symptomatic And Neuroprotective Therapy
Pharmacologic treatment of Parkinson disease can be divided into symptomatic and neuroprotective therapy. At this time, there is no proven neuroprotective or disease-modifying therapy.
Levodopa, coupled with carbidopa, a peripheral decarboxylase inhibitor , remains the gold standard of symptomatic treatment for Parkinson disease. Carbidopa inhibits the decarboxylation of levodopa to dopamine in the systemic circulation, allowing for greater levodopa distribution into the central nervous system. Levodopa provides the greatest antiparkinsonian benefit for motor signs and symptoms, with the fewest adverse effects in the short term however, its long-term use is associated with the development of motor fluctuations and dyskinesias. Once fluctuations and dyskinesias become problematic, they are difficult to resolve.
Monoamine oxidase -B inhibitors can be considered for initial treatment of early disease. These drugs provide mild symptomatic benefit, have excellent adverse effect profiles, and, according to a Cochrane review, have improved long-term outcomes in quality-of-life indicators by 20-25%.
Neuroprotective therapy aims to slow, block, or reverse disease progression such therapies are defined as those that slow underlying loss of dopamine neurons. Although no therapy has been proven to be neuroprotective, there remains interest in the long-term effects of MAO-B inhibitors. Other agents currently under investigation include creatine and isradipine.
Why Choose Us For Mri
The University of Kansas Health System is the only medical center in the region that provides MRI-guided focused ultrasound to treat essential tremor and Parkinsons disease with hand tremor as the primary symptom. Our health system is 1 of only 47 medical centers around the world that the Parkinsons Foundation has designated a Center of Excellence for Parkinsons disease care.
When you choose The University of Kansas Health System for MRI-guided focused ultrasound, you will be cared for by a team of neurologists who are specialists in their fields. A dedicated nurse navigator will help you as you go through the processes needed leading up to your treatment. Our neurology and neurosurgery program is nationally ranked by U.S. News and World Report.
Also Check: Parkinson’s Support Groups In My Area
Study Design And Patients
This was a prospective, single-arm, non-randomized, proof-of-concept, safety, and feasibility phase I trial of focal BBB disruption in patients with PDD. Power calculations were not performed to determine the number of patients as this was a pilot investigation. Since this was an exploratory study, the results are presented in a purely descriptive manner. All patients demonstrated neuroimaging abnormalities in the targeted area, and the right parieto-occipito-temporal cortex BBB opening sessions were separated by 23 weeks based on the patients availability. This study was approved by the Research Ethics Board at HM Hospitales and the Spanish Agency of Medicines and Medical Products number 627/17/EC, and registered at ClinicalTrial.gov number }NCT03608553. The study design and conduct complied with all relevant regulations regarding the use of human study participants and was conducted in accordance to the Declaration of Helsinki.
Anticholinergics For Early On
The first pharmacological agents used in PD therapy were anticholinergic drugs. They reduce the activity of acetylcholine by acting as antagonists at choline receptors, hoping to restore the balance between dopamine and acetylcholine levels that was disturbed by PD. These drugs have largely been replaced by L-DOPA and other centrally acting dopaminergic agonists, but they still remain available for use in the treatment of PD. Benztropine, biperiden, diphenhydramine, ethopropazine, orphenadrine, procyclidine, and trihexyphenidyl are included in this therapeutic class of drugs, though there is little pharmacokinetic information available on them because of their low plasma drug concentrations. Typically, anticholinergic drugs have a greater role in tremor-predominant PD and can be a monotherapy in early stages, but are usually done in adjunct with L-DOPA or other prescribed medications.
You May Like: At What Age Can You Get Parkinson’s
Clinical Outcomes And Adverse Events
Gamma knife thalamotomy has been shown to improve motor function in patients with PD. The radiation dose used in GK thalamotomy ranges from 120 to 180Gy, and it appears that doses less than 120Gy do not provide clinical benefits . In a prospective study of unilateral gamma knife thalamotomy for patients with PD and essential tremor , Ohye et al. reported an improvement in tremor scores , with 81.1% of patients evaluated as having good or excellent results at 24-month follow-up . A more recent prospective, single-blind study of unilateral GK thalamotomy for patients PD and ET reported a 54.2% improvement in the upper limb tremor score . GK pallidotomy has also been performed to treat PD, although only a few reports have described the procedure . The GPi is considered a high-risk target for GK radiosurgery due to its proximity to the optic tract and the risk of optic neuropathy . Likewise, the STN is not an advised target due to the risk of neurologic complications including hemiparesis, dysarthria, and gait disturbances .
Also Check: Does Nick Nolte Have Parkinsons Disease
