Conceptualization Of The Diseases Needs And Interventions
Both dementia and PD are incurable and progressive diseases with often complex problems and needs, for which tailored interventions are available . For dementia, experts agree that recognizing its eventual terminal nature is the basis for anticipating future problems and an impetus to the provision of adequate palliative care . Some advocate advanced dementia to be a terminal disease to support eligibility for palliative care. However, as about half of dementia patients never reach an advanced stage ; , it may be a late trigger to initiate palliative care. There is no consensus, however, at which stage palliative care in dementia should start .
Table 2. Conceptualization of the disease, needs of patients and family caregivers, and interventions.
For PD there are no curative treatments either, but the success of dopaminergic replacement therapy and deep brain stimulation has enabled the majority of patients to live independently with a relatively low symptom burden for the first 10 years after diagnosis-when they live up to a decade . This may contribute to PD generally not being recognized as an illness for which a palliative approach may be helpful . A US patient and caregivers council recommends palliative care to be available from diagnosis of PD . This is also the ideal of the European Parkinson’s Disease Association although they emphasize that when to start palliative care is an individual decision.
Parkinsons And Lewy Body Disease
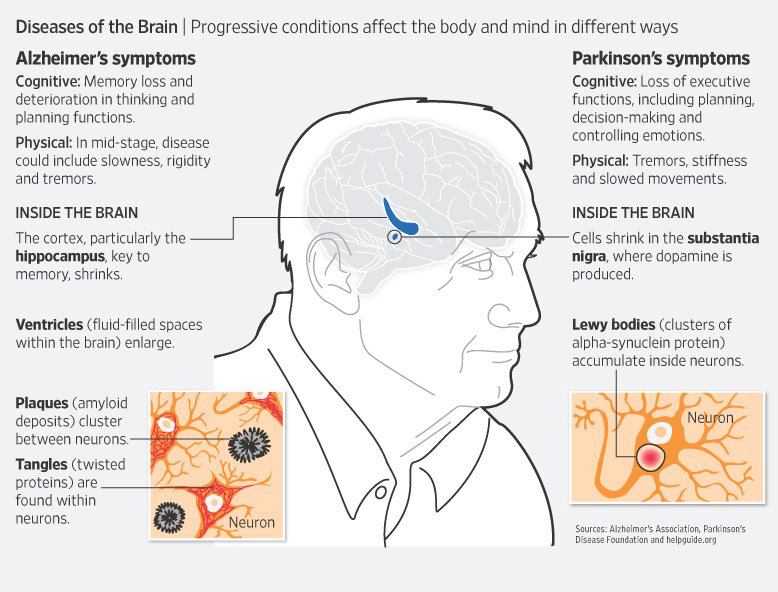
Lewy body disease occurs when there is an abnormal build up of a protein called alphasynuclein in the brain. Depending on where the proteins accumulate, Lewy body disease can lead to impairments in movement, thinking and behaviour.
Lewy body disease includes three overlapping disorders: ;;
- Dementia with Lewy bodies
- Parkinsons disease dementia
This overlap results in the disease being called a spectrum disease.
In people with Parkinsons a large number of Lewy bodies appear in an area of the brain known as the substantia nigra. This area of the brain is responsible for movement, so the Lewy bodies are likely to cause impairments in movement.
Some people may go on to develop dementia with Lewy bodies. In this form of the disease, the clumps of protein occur in the cortex . This part of the brain is responsible for many cognitive processes, so the Lewy bodies are likely to result in cognitive impairments like those described under the heading above. It can result in symptoms similar to those seen in Alzheimers.
Advice For Carers Family And Friends
Living with or caring for someone with Parkinsons disease dementia can be challenging. Sometimes help and support will be relied on heavily but there will be times when it will be better to step back and allow the person with dementia to do things for themselves. This balance will be difficult to judge at first, but with time and patience new routines and approaches to day-to-day living can be established.
It is important to encourage, stimulate and help the person with dementia, but remember too that rest is important.
Recommended Reading: What Is The Life Expectancy Of Someone With Parkinson’s Disease
Dementia With Lewy Body
Cortical Lewy bodies are found in different types of degenerative dementia, which are collectively called as LBD. Clinicopathologically, it encompasses PDD, DLB, and Lewy body variant of Alzheimer’s disease . The last of the three is characterized by cortical Lewy bodies and Alzheimer’s type neuropathological changes in the brain and constitutes about 70% of LBD. In different literatures the terms LBD and DLB have been used interchangeably and the term diffuse LBD has been used to denote classical DLB. Because 25%30% of PD patients develop dementia and most DLB patients have parkinsonism, it has been hypothesized that PD, PDD, and DLB are not distinct entities, but may exist along the spectrum of LBD. A DLB/PDD Working Group recently proposed the use of LBD as an umbrella for studying the biology of these disorders, although they also suggested that the three individual terms should be maintained for clinical needs. Consensus criteria artificially divide patients with PDD and DLB by the one year rule where dementia appears within 1 year of appearance of parkinsonian features in the latter condition.
DLB consensus criteria has been put forward by McKeith et al. see .
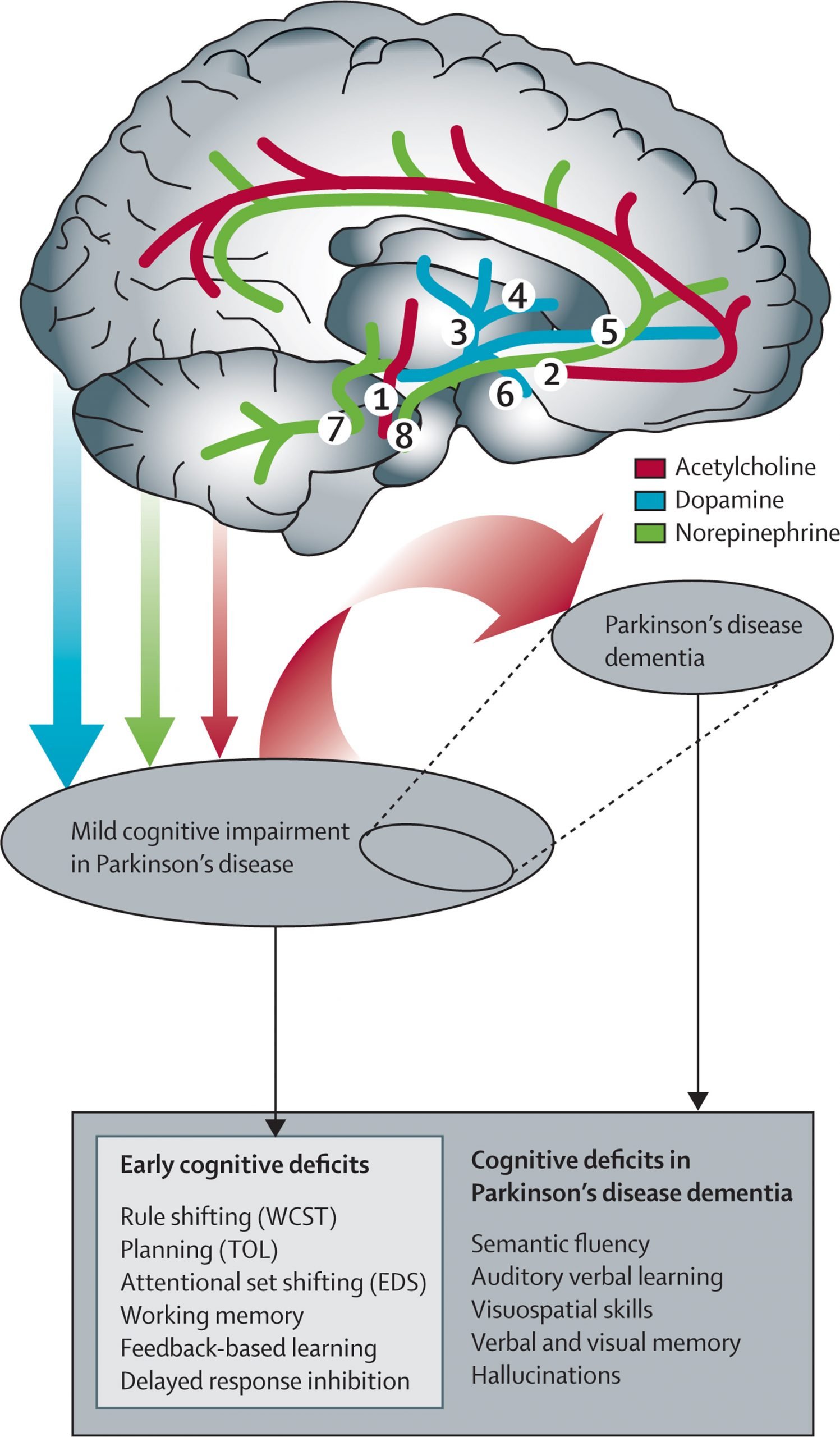
Concomitant Dysfunction In Frontal And Arousal Networks Contributes To Generation Of Visual Hallucinations
Overlapping dysfunctions in a number of other cognitive networks are also likely to contribute to the generation of visual hallucinations in PDD. For example, several functional MRI studies comparing patients with Parkinsons disease with hallucinations to those without during performance of visual paradigms have demonstrated not only dysfunction in visual cortical areas in the former, but also simultaneous disruption of activity in frontal areas . The presence of hallucinations in PDD is closely associated with worsening impairments on tests of attentional control , as well as impairments on tests of inhibitory control such as the Stroop Test and Go/No-Go Task , deficits that might in part be attributable to dysfunctions in the fronto-parietal and noradrenergic networks respectively . This therefore suggests that breakdown in these frontal networks may play a contributory role in the generation of visual hallucinations in PDD, perhaps by reducing attentional and inhibitory control of perceptual errors arising from dysfunction in posterior visual cortices, allowing them to enter conscious perception as hallucinations .
Read Also: What Is The Life Expectancy Of Someone With Parkinson’s Disease
What Is Parkinson Disease
Parkinson;disease is a movement disorder. It can cause the muscles to tighten and become rigid This makes it hard to walk and do other daily activities. People with Parkinsons disease also have tremors and may develop cognitive problems, including memory loss and dementia.
Parkinson;disease is most common in people who are older than 50. The average age at which it occurs is 60. But some younger people may also get Parkinson disease. When it affects someone younger than age 50, it’s called early-onset Parkinson disease. You may be more likely to get early-onset Parkinson disease if someone in your family has it. The older you are, the greater your risk of developing Parkinson disease. It’s also much more common in men than in women.
Parkinson disease is a chronic and progressive disease.; It doesn’t go away and continues to get worse over time.
What Are Parkinson’s Disease Dementia Medical Treatment And Medications
There is no specific therapy for dementia in Parkinson’s disease. Although cognitive symptoms initially may appear to respond to drugs that promote dopamine production, the improvement is mild and transient in contrast to the early responses to motor control improvement with medication in patients with Parkinson’s disease.
Parkinson’s disease dementia medications
Various medications are used to treat the movement disorders of Parkinson’s disease, some may exacerbate symptoms related to dementia.
- These include dopamine given in the form of levodopa; medications known as dopamine agonists that act on the dopamine receptor; and medications that slow down the metabolism of dopamine. They are often used in conjunction with monoamine oxidase inhibitors such as rasagiline. In addition, anticholinergic drugs are sometimes used.
- Unfortunately, these drugs may affect cognitive symptoms and mood disorders.
- The anticholinergic drugs, for example, help balance levels of dopamine and acetylcholine, another neurotransmitter, in the brain. These drugs can improve movement disorders but often make memory loss worse.
The dementia of Parkinson’s disease may respond to drugs used in patients with Alzheimer’s disease. However, these drugs, called cholinesterase inhibitors , lead to only small and temporary improvements in cognition.
Mood disorders and psychoses are usually treated with other medication.
Also Check: What Is The Life Expectancy Of Someone With Parkinson’s Disease
What Causes Parkinsons Disease Dementia
A chemical messenger in the brain called dopamine helps control and coordinate muscle movement. Over time, Parkinsons disease destroys the nerve cells that make dopamine.
Without this chemical messenger, the nerve cells cant properly relay instructions to the body. This causes a loss of muscle function and coordination. Researchers dont know why these brain cells disappear.
Parkinsons disease also causes dramatic changes in a part of your brain that controls movement.
Those with Parkinsons disease often experience motor symptoms as a preliminary sign of the condition. Tremors are one of the most common first symptoms of Parkinsons disease.
As the disease progresses and spreads in your brain, it can affect the parts of your brain responsible for mental functions, memory, and judgment.
Over time, your brain may not be able to use these areas as efficiently as it once did. As a result, you may begin experiencing symptoms of Parkinsons disease dementia.
You have an increased risk of developing Parkinsons disease dementia if:
- youre a person with a penis
- youre older
Dysexecutive Symptoms May Emerge When Inter
How dysfunction in the fronto-striatal and mesocortical dopaminergic networks may interact to cause dysexecutive symptoms in PDD is unclear. However the results of suggest that it is supervening dysfunction in the mesocortical projections to the insular upon existing fronto-striatal network disruption that heralds major executive impairment. Indeed there is limited evidence suggesting some redundancy between the two systems in early Parkinsons disease: in one study patients performing a set-shifting task did not display behavioural impairment despite fronto-striatal hypoactivation on functional MRI, possibly because they displayed concurrent hyper-activation in the insular and fronto-parietal networks, which was not present in controls . Using functional MRI, also noted a relative increase in blood-oxygen level-dependent activity within frontal regions in patients during a matching task. Although this evidence is indirect it suggests that the mesocortical network may partially compensate for fronto-striatal dysfunction in early disease, until it too is damaged, compensation is lost, and a full-blown dysexecutive syndrome develops. Such a proposal is compatible with, and extends, the hypothesis proposed by others that deficient interplay between the fronto-striatal and mesocortical dopamine networks underlies the dysexecutive syndrome of Parkinsons disease .
Read Also: What Is The Life Expectancy Of Someone With Parkinson’s Disease
Parkinson’s Disease Dementia Follow
A person with Parkinson’s disease and dementia requires regular checkups with his or her health care professional.
- These checkups allow the health care professional to see how well treatment is working and make adjustments as necessary.
- They allow detection of new problems of cognition, mood, or behavior that could benefit from treatment.
- These visits also give the family caregiver an opportunity to discuss problems in the individual’s care.
Eventually, the person with Parkinson’s disease and dementia will likely become unable to care for himself or herself or even to make decisions about his or her care if the patient lives long enough with Parkinson’s disease and dementia.
- It is best for the person to discuss future care arrangements with family members as early as possible, so that his or her wishes can be clarified and documented for the future.
- A health care professional can advise patients and caregivers about legal arrangements that should be made to ensure that these wishes are observed.
Parkinson’s disease dementia prevention
There is no known way of preventing dementia in Parkinson’s disease. However, patients with Parkinson’s disease are urged to continue to exercise and live a healthy lifestyle as this may delay or reduce the onset of dementia, although there is no good data to indicate this will occur.
Parkinson’s disease dementia prognosis
Is The Dementia Caused By Parkinsons Or Something Else
Indications that dementia may be caused by something other than Parkinsons disease include agitation, delusions , and language difficulties. If the onset of cognitive symptoms is sudden, theyre more likely due to something other than Parkinsons diseaseeven reversible causes such as infection, a vitamin B12 deficiency, or an underactive thyroid gland.
Depression can mimic dementia by causing similar symptoms such as apathy, memory problems, and concentration difficulties. Since depression is very common in Parkinsons patients, its important to recognize the signs and symptoms of depression in older adults.
Parkinsons disease dementia vs. other dementias
Other types of dementia that can be commonly mistaken for Parkinsons disease dementia include:
Lewy Body Dementia is characterized by fluctuations in alertness and attention, recurrent visual hallucinations, and Parkinsonian motor symptoms like rigidity and the loss of spontaneous movement. In this disorder, cognitive problems such as hallucinations tend to occur much earlier in the course of the disease and often precede difficulties with walking and motor control.
Alzheimers disease and Parkinsons disease are both common in the elderly, especially in those over 85. Patients with Parkinsons who develop dementia may even develop Alzheimers dementia as well. Therefore, its important to be aware of the signs of Alzheimers Disease and how its treated.
Don’t Miss: Parkinson’s Disease Life Span
How Can We Support The Sleep/wake Cycle Of Pdd
For people with PDD who are confused about the day-night cycle, some daily strategies can be helpful. At night, starting a lights out routine that happens at the same hour every day, where all curtains are closed and lights are turned off, can help the person understand that it is sleep time. During the day, opening the curtains, allowing the person with PDD to spend as much time in the daylight as possible, avoiding naps, and organizing stimulating activities, can be helpful. Having lots of calendars and clocks in every room might also help a person with PDD be less confused about the time of day.
Dementia Can Be Treated Through Medication But Its Progression Will Continue
Some of the problems caused by dementia are treatable, but there are no medications that slow the progression of this problem, just as there are no treatments that slow the progression of the rest of the Parkinsons Disease syndrome. We often use the same medications that are used in Alzheimers disease to improve concentration and memory, although only one, rivastigmine, has been approved by the Food and Drug Administration for dementia in PD. Most experts believe that each of the Alzheimer drugs are about as useful in dementia in Parkinsons Disease as they are in Alzheimers, which, unfortunately, is not great. As with all medications used in PD, whether for slowness, stiffness, tremor, depression or sleep disorders, if the medication is not helpful, one should either try a higher dose or stop it. Since the drugs used to treat dementia take several weeks to work, and the dose often requires increases, the family needs to allow a reasonable time period, usually around two months, to decide if it is helpful or not. Obviously this needs to be discussed with the prescribing doctor.
There is a lot of research being done to better understand and better treat dementia in PD.
You May Like: Is Parkinson Disease Fatal
Comparison With Other Dementias
Dementia is the result of physical changes in the brain that can lead to memory loss and an inability to think clearly.
Several types of dementia exist, including:
PD dementia has different symptoms to other types.
Alzheimers dementia, for example, impairs memory and language. PD dementiam on the other hand, affects problem-solving, the speed at which thoughts occur, memory, and mood, alongside other important cognitive functions.
Dementia with Lewy bodies and Parkinsons disease dementia are similar in that the Lewy Bodies might be present in both forms.
However, whether the disease causes Lewy bodies or if Lewy bodies cause the disease symptoms is unclear. Researchers also believe that the way the Lewy bodies form in Parkinsons disease dementia is different from those in Lewy body dementia.
Dementia With Lewy Bodies And Parkinson Disease Dementia
, MD, PhD, Department of Neurology, University of Mississippi Medical Center
Dementia with Lewy bodiesParkinson disease dementia
Dementia is chronic, global, usually irreversible deterioration of cognition.
Dementia with Lewy bodies is the 3rd most common dementia. Age of onset is typically > 60.
Lewy bodies are spherical, eosinophilic, neuronal cytoplasmic inclusions composed of aggregates of alpha-synuclein, a synaptic protein. They occur in the cortex of some patients who have dementia with Lewy bodies. Neurotransmitter levels and neuronal pathways between the striatum and the neocortex are abnormal.
Lewy bodies also occur in the substantia nigra of patients with Parkinson disease, and dementia may develop late in the disease. About 40% of patients with Parkinson disease develop Parkinson disease dementia, usually after age 70 and about 10 to 15 years after Parkinson disease has been diagnosed.
Because Lewy bodies occur in dementia with Lewy bodies and in Parkinson disease dementia, some experts think that the two disorders may be part of a more generalized synucleinopathy affecting the central and peripheral nervous systems. Lewy bodies sometimes occur in patients with Alzheimer disease, and patients with dementia with Lewy bodies may have neuritic plaques and neurofibrillary tangles. Dementia with Lewy bodies, Parkinson disease, and Alzheimer disease overlap considerably. Further research is needed to clarify the relationships among them.
Recommended Reading: How Long Do People Live With Parkinson’s
Caring For Someone With Parkinsons
Practice patience and understanding when dealing with Parkinsons. You may be very frustrated and challenged as a caregiver, but those with Parkinsons are just as frustrated. Their physical and mental conditions can be debilitating, depressing, and humiliating.
Diet and nutrition can have a huge impact on the health and comfort of a Parkinson patient. Eating well, getting more rest, sleeping well, fresh air, and exercise can make a difference. Getting the right medication and complementary therapies is also important.
As Parkinsons impacts a patients motor skills, modifications to the living environment may have to be made to accommodate wheelchairs and limited mobility issues. Professional in-home assistance for Parkinsons can allow Parkinson patients to remain independent and can enhance quality of life.
Most importantly, seek help and support from family, friends, and caregiving support groups. Take advantage of the resources in your community. Shouldering all the burden can take a toll on a caregiver.
Take care of yourself or you wont be able to take care of your loved one. Follow the preventive advice provided above for yourself as well, and take deep breaths!
Resources
Severity Of Motor Symptoms
Compared to those without dementia, PDD patients had more severe motor features with a greater impairment in balance. Of the 36 participants, 13 were characterised H & Y stage IV and V, whereas the others were between stages IIII. In particular, of the seven PDD participants, six were characterised by having H & Y stages IV and V.
You May Like: Which President Had Parkinson’s
