Human Ipsc Studies Of Pd Highlight Converging Molecular And Cellular Pathways Across Genetic Subgroups

Our analysis of 385 iPSC-derived cell lines from 67 published studies reveals that many PD neuronal phenotypes are shared between genetically heterogeneous familial and sporadic patients . Notably, impairments in mechanisms involved in cellular waste recycling, mitochondrial function, neuronal morphology and physiology, and sensitivity to reactive oxygen species are most common across patient lines with varying genetic predispositions . The studies measured cellular phenotypes that occurred either spontaneously or in response to chemicals mimicking cellular aging and stress . It is important to note that the frequency of reported phenotypes in our meta-analysis may be biased because only few studies reported negative results 31,32,36,37,40,45,48,52,59,64,74,76,86. In addition, most cell lines were not systematically phenotyped without prior hypothesis and thus, there is likely to be an ascertain bias in these phenotypes. Less hypothesis-driven multimodal or omics analysis will help to address such bias41,72,76,77,78,79,80,87,90. Phenotypes caused by genomic predispositions allude to crosstalk and impairments in multiple pathways that act collectively to mediate selective degeneration of dopaminergic neurons in the substantia nigra and will be discussed in detail below.
Fig. 4: Phenotypic insights from iPSC studies of Parkinson’s disease.
The Interplay Between Genomic Predispositions And Environmental Factors Leads To Parkinsons
In the mid-1990s, the connection between PD and underlying genetic mutations was established4,5,150. It is now evident that varying degrees of the interplay between genomic predispositions and aging and cellular stressors impose a risk for disease151 . Previous studies have shown vascular insults to the brain, repeated head trauma, neuroleptic drugs, exposure to pesticides, and manganese toxicity increase the risks of developing symptoms of PD152,153,154. In addition, advancing age can also cause a cascade of stressors within the substantia nigra, which weakens the neurons and their ability to respond to further insults155,156. Ultimately, the uniqueness of the interactions between genes and the environment makes the development of a single treatment for PD difficult as they give rise to a spectrum of neuronal phenotypes that can be unique to individual patients . The development of a model with the ability to replicate the genomic and epigenetic aspects of the disease is crucial . As increasing evidence suggests that genetic mutations are key modulators of disease initiation and progression, the identification and understanding of the various genomic predispositions are required for the development of better-targeted treatments to slow the disease progression.
Fig. 1: A combinatorial spectrum of genetic risks, cellular stressors, and brain cell dysfunctions causes Parkinson’s disease.Full size image
Quality Assistance For People With Parkinson’s Disease As A Result Of Paraquat Exposure
If you struggle with Parkinson’s disease as a consequence of frequently using paraquat, the team of Atraxia Law can provide you with the assistance you need to determine whether you qualify for filing a claim with the responsible manufacturers.
While the process is quite complex and tedious, it will require minimal involvement on your part, as we are aware that the majority of our clients are in great physical and emotional pain.
After you explain to our experts how you developed parkinsonism as a result of paraquat exposure we will thoroughly evaluate your case and subsequently tell you with certainty whether you can file a claim to obtain financial compensation. For additional information, do not hesitate to contact our company and we will gladly answer your questions.
Sidebar: Morris K Udall Centers Of Excellence For Parkinson’s Disease Research
The Morris K. Udall Parkinson’s Disease Research Act of 1997 authorized the NIH to greatly accelerate and expand PD research efforts by launching the NINDS Udall Centers of Excellence, a network of research centers that provide a collaborative, interdisciplinary framework for PD research. Udall Center investigators, along with many other researchers funded by the NIH, have made substantial progress in understanding PD, including identifying disease-associated genes; investigating the neurobiological mechanisms that contribute to PD, developing and improving PD research models, and discovering and testing potential therapeutic targets for developing novel treatment strategies.
The Udall Centers continue to conduct critical basic, translational, and clinical research on PD including: 1) identifying and characterizing candidate and disease-associated genes, 2) examining neurobiological mechanisms underlying the disease, and 3) developing and testing potential therapies. As part of the program, Udall Center investigators work with local communities of patients and caregivers to identify the challenges of living with PD and to translate scientific discoveries into patient care. The Centers also train the next generation of physicians and scientists who will advance our knowledge of and treatments for PD. See the full list of Udall Centers.
What Other Conditions Have Similar Symptoms And Signs Of Parkinsons Disease
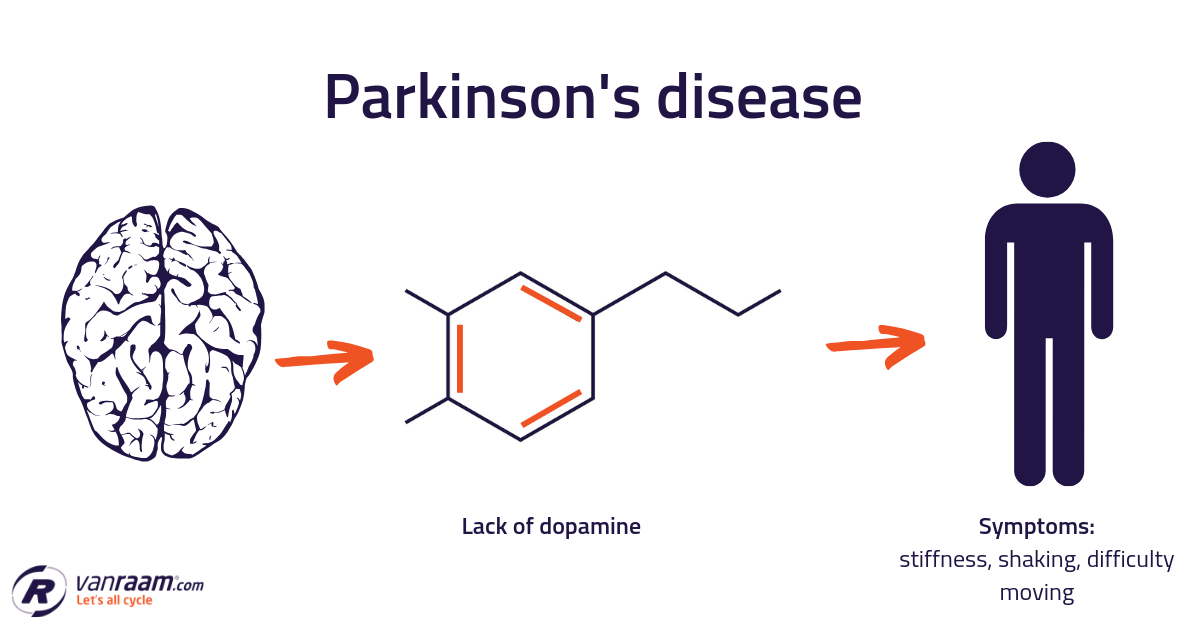
Other neurological diseases may cause symptoms similar to Parkinson’s disease. The term Parkinsonism refers to a patient that has symptoms similar to Parkinson’s.
Early in the disease process, it can be tough to make an assertive diagnosis and difference between Parkinson’s and Parkinson-like diseases.
Often the correct diagnosis is made after further symptoms develop, and the physician can monitor the course of the disease.
The development of additional symptoms and the course of the illness generally points towards the correct diagnosis. These are the most common neurological diseases that can produce Parkinson-like symptoms.
- Progressive Supranuclear Palsy
- Lewy Body disease or Dementia with Lewy bodies
- Corticobasal degeneration or corticobasal ganglionic degeneration
Nonetheless, doctors should think of other causes rather than Parkinson’s disease when events like this happen.
- Poor response to dopamine
- Early loss of balance or vision problems
- Prominent intellectual decline – dementia
- Rapid onset or progression of the disease
Actually, though it is a disease that is not clearly understood, there are specific organizations like Parkinson’s UK that dedicate themselves to doing research.
These organizations look forward to following the natural course of the disease and developing clinical trials for patients in an attempt to find a cure.
We Compiled The Most Popular Parkinsons Questions And Answers In One Place
As your Parkinson’s disease journey evolves, so do your questions about symptoms, treatment options, research and medications. Whether you live with Parkinson’s or care for someone who does, you are not alone in looking for answers to your big PD questions.
The Parkinson’s Foundation has recently released Frequently Asked Questions: A Guide to Parkinson’s Disease, a new and improved booklet that provides answers to the most frequently asked questions our Helpline receives. Pro tip: every section in the booklet provides additional free resources you can check out to learn more. Order the free book now, read it online or check out some questions and answers below:
Q: Can Parkinson’s be cured?
A: Not yet. However, many PD symptoms can be treated and researchers are making advances in understanding the disease, its causes and how to best treat it.
Q: What are the stages of Parkinson’s?
A: The stages of Parkinson’s correspond to the severity of movement symptoms and to how much the disease affects a person’s daily activities. At all stages of Parkinson’s, effective therapies are available to ease symptoms and make it possible for people with PD to live well.
Q: How can I find a doctor who can treat Parkinson’s?
Q: Is it okay to drink alcohol?
A: Consult your doctor first. Generally, moderate consumption should be acceptable for people with PD, if there are no medical conditions or medications that prohibit alcohol use.
Q: Are there any new Parkinson’s drugs on the horizon?
Parkinson’s Disease Is Often Misdiagnosed In People With Paraquat Exposure
Because the symptoms of Parkinson’s disease are very similar to those of other health problems, it is often misdiagnosed in people with a history of exposure to paraquat, which prevents victims of toxic exposure from recovering the financial compensation they deserve. According to medical studies, Parkinson’s disease is misdiagnosed in up to 30% of cases and the rate of misdiagnosis is even higher in people whose disease is in the early stages. 1 in 4 people with Parkinson’s disease will receive a wrong diagnosis
Therefore, seeking a second and even a third opinion is essential in being assigned a correct and accurate diagnosis. It is a known fact that frequent exposure to paraquat in agricultural workers increases the risk of developing Parkinson’s disease by 250%.
Thereby, if you have a history of paraquat exposure, it is crucial to keep a close eye on your health for the symptoms of Parkinson’s disease.
A poll from the American Journal of Managed Care found that over 26% of people with Parkinson’s disease were initially misdiagnosed and 21% had to see their general healthcare provider 3 times before being referred to a specialist to have their health problem correctly diagnosed.
What is more alarming is that 48% of the participants received treatment for the wrong health condition, with 36% being prescribed medication and 6% undergoing surgical procedures. Consequently, a significant decline in the quality of life was noted in the misdiagnosed patients.
Genetic Predispositions Reducing Differentiation Yield Of Mda Neurons
In vitro neural development was impaired in neural lines derived from patients carrying LRRK2, PRKN, SNCA, and sporadic mutations43,49,74,93. In four independent studies, the differentiation potential of neural progenitor cells derived from patients was significantly reduced, demonstrated by low yields of neurons in comparison with control lines43,49,74,81,94. A recent review presented the idea that PD is attributed to significant neurodevelopmental defects, which may increase the susceptibility for disease onset224. If confirmed, identifying genetic predispositions that contribute to early developmental defects in iPSC-PD may assist the development of novel PD therapies. However, these phenotypes may appear in conflict with other studies53,55,76 capable of generating functional neurons from cell lines with similar mutations. The differences could be due to varying protocols, which may be more or less stressful for the cells.
Will Findings From Pd Ipsc Models Translate To Human Clinical Trials
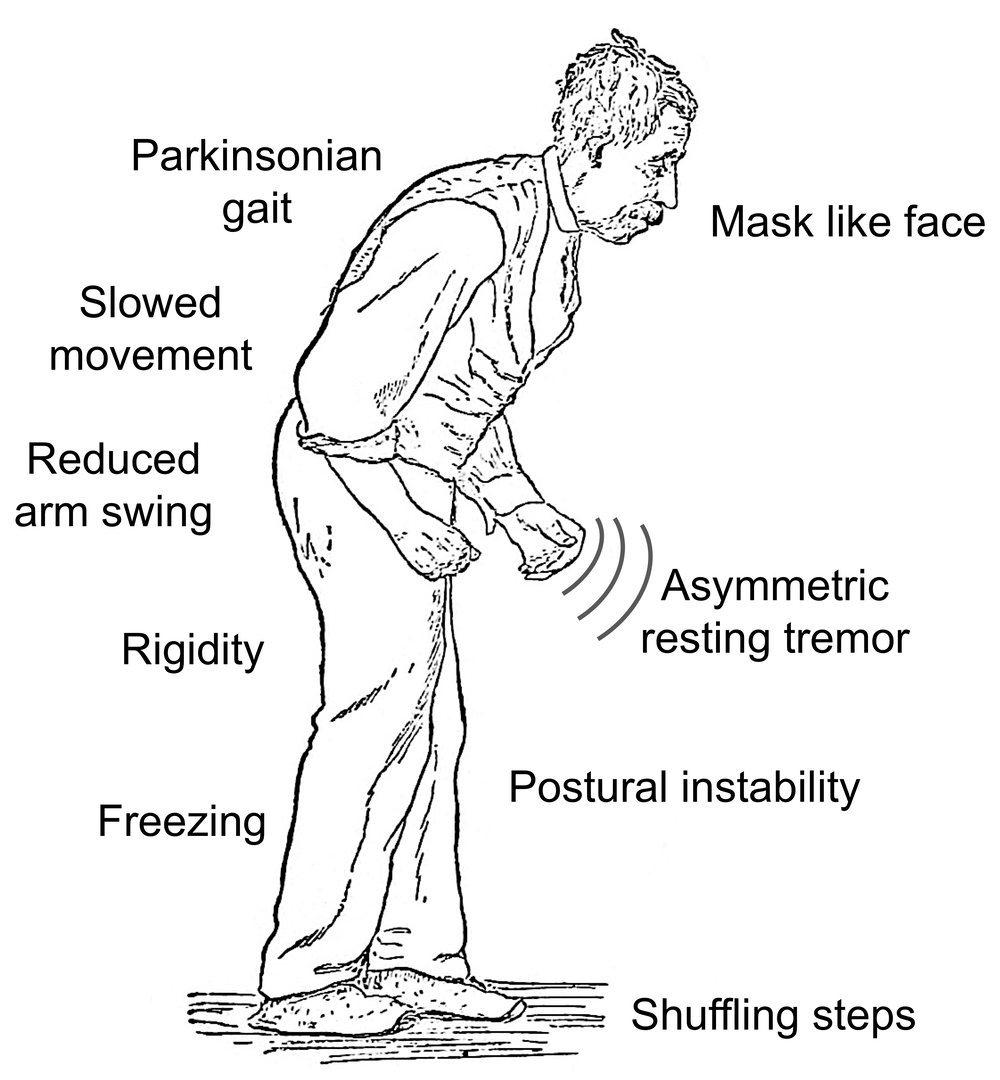
Given the apprehensions that in vitro studies may be too artificial, human iPSC-derived neural progenitors may be transplanted into animal brains244,245,246,247. Besides ethical barriers, xenografts also raise the possibility that the healthy host tissue compensate for the impairment of the transplanted cells. Yet, if the phenotypes observed in vitro are recapitulated in vivo, pharmacological treatments could be assessed in a systemic environment, with much more realistic dosage and administration methods.
What Is The Prognosis And Life Expectancy For Parkinson’s Disease
The severity of Parkinson’s disease symptoms and signs vary greatly from person to peson, and it is not possible to predict how quickly the disease will progress. Parkinson’s disease itself is not a fatal disease, and the average life expectancy is similar to that of people without the disease. Secondary complications, such as pneumonia, falling-related injuries, and choking can lead to death. Many treatment options can reduce some of the symptoms and prolong the quality of life.
How Environmental Factors And Aging Can Be Recapitulated In Vitro
An obvious limitation of in vitro models is the lack of environmental context. The influence of nongenetic factors is not recapitulated in the basal phenotype of patient-derived neurons. For example, the influence of head trauma of a boxer with sporadic PD will not be recapitulated by default in reprogrammed neurons. An alternative would be to transplant the patient-derived neurons in animals and simulate the trauma on the animal. Similarly, influence of decades of aging of the human brain is difficult to reproduce in vitro in a few months within the boundaries of feasible experimental design. Brains in a dish will always be an imperfect experimental model. However, many tricks can be used to recapitulate the environmental and aging stress in vitro. Table 2 summarizes a list of reagents that have already been used in iPSC neuronal culture to mimic oxidative stress, proteostatic stress, mitochondrial stress, synaptic stress, ER stress, inflammation, and cellular aging. An interesting example is progerin, a truncated form of lamin A associated with premature aging. Increasing the expression of progerin in iPSC neurons can recapitulate at least some aspect of cellular aging in vitro71. Human iPSC-derived dopamine neurons overexpressing progerin displayed specific phenotypes such as neuromelanin accumulation. In addition, PD patient-derived neurons revealed disease-related phenotypes that required both genetic susceptibility and induced-aging in vitro71.
What Health Conditions Mimic The Symptoms Of Parkinson’s Disease
Parkinsonism is a medical term that refers to the symptoms experienced by people with the disease, which include slowness of movements, stiffness of the joints, as well as tremor and imbalance. However, there are a series of conditions whose symptoms are very similar to those of Parkinson’s disease, which is why so many people are misdiagnosed.
Being aware of these health conditions is essential if you have a history of exposure to paraquat, as it may facilitate the assignment of a correct diagnosis. The following are some of the conditions that mimic the symptoms of Parkinson’s disease:
If you have a history of exposure to paraquat and were diagnosed with one of the above conditions, we strongly advise you to seek a second opinion from a specialist, as you may be in fact struggling with Parkinson’s disease, which qualifies you for compensation.
It is essential to receive a correct and precise diagnosis, as it will not only help you obtain the money you deserve from the liable companies but will also improve your quality of life.
For over 35 years, the team of experts at Atraxia Law has been helping people recover the compensation they were eligible for by evaluating their personal injury or product liability claims and are ready to provide you with quality assistance as well if your health was affected by exposure to paraquat.
Projected Estimates Of Parkinsons Disease With Aging Population
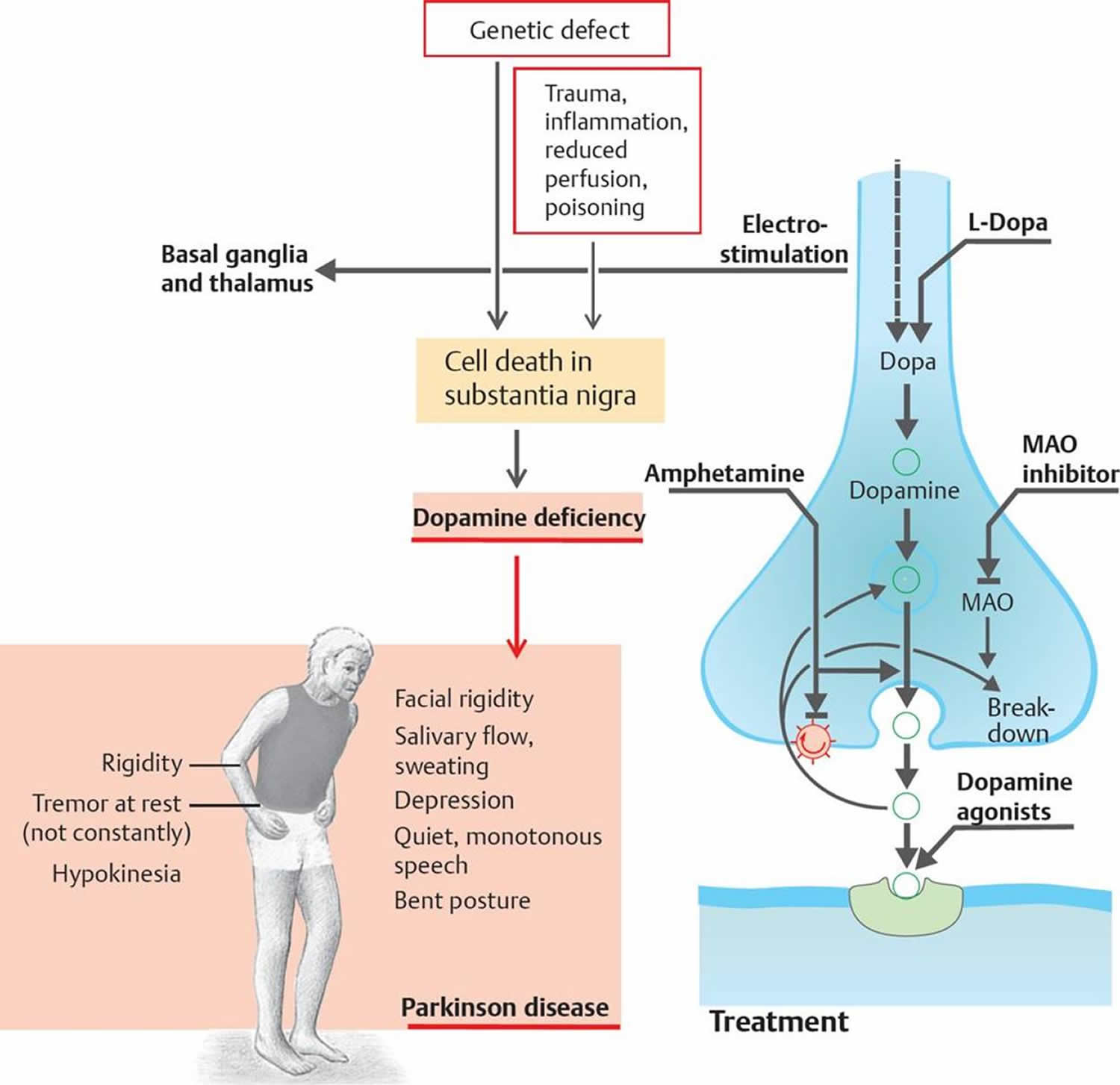
As the life expectancy has increased worldwide, it is expected that the burden of chronic diseases, like PD, will continue to grow. It is estimated that the number of people with PD in 2005 totaled between 4.1 million and 4.6 million and that number will more than double by 2030 to between 8.7 million and 9.3 million.7
Neuroinflammation Exacerbates Neurodegeneration In Sporadic Pd
Midbrain neurons derived from sporadic patients showed increased susceptibility to the effects of adaptive immune cells72. Sporadic patient neuronal lines co-cultured with T-lymphocytes exhibited substantial signs of cell death mediated by IL-17–IL-17R signaling and activation of NFkB72. Similarly, IL-17 treatment resulted in increased neuronal death72. Inflammation in the central nervous system and periphery are key hallmarks of PD220. Increasing evidence implicates the role of microglia in neuronal loss, though the underlying mechanisms remain to be determined221,222. RNA-seq analysis of astrocytes derived from LRRK2-G2019S iPSCs highlighted dysregulation in genes involved in the extracellular matrix, which may reduce the neuroprotective capacity of astrocytes in PD78. Investigating the role of neuroinflammation in patient-derived microglia may also contribute to the understanding of the selective vulnerability of mDA neurons in sporadic and late-onset PD223.
The Importance Of Establishing Parkinsons Prevalence Numbers
Parkinson’s Prevalence estimates will help the Parkinson’s Foundation attract the attention of federal and state government as well as the pharmaceutical industry to the growing need and urgency in addressing PD. This is an important first step to better understanding who develops PD and why.
The next phase of this study will be to determine the rate of PD diagnosis or incidence, how that has changed over time and what is the rate of mortality among those affected by PD. Determining the prevalence and incidence will allow the PD community to effectively advocate for additional money and resources necessary to support Parkinson’s research.
Parkinson’s Foundation Prevalence Project numbers highlight the growing importance of optimizing expert Parkinson’s care and treatment for people with Parkinson’s, which would help future caregivers and ease the strain on health and elder care systems.
Loading…
Toxic Substances That Have Been Linked To Parkinsons Disease
There are numerous environmental toxins that researchers have tied to the neurological disorders known as parkinson disease. Here are some that have been linked:
- Agent Orange– This was a chemical defoliant used in Vietnam that is already tied to cancer. While there is no definitive link with Parkinson’s, the VA at least believes that there is a possibility that the two are tied.
- Solvents– Some studies have shown a link between Trichloroethylene, a substance contained in many solvents, and Parkinson’s.
- PCBs– polychlorinated biphenyls were extensively used in the 1970s. They have been often found in the brains of people who have suffered from Parkinson’s.
- Pesticides and herbicides -substances such as insecticides, pesticides and herbicides contain chemicals that researchers have strongly linked with higher incidences of Parkinson’s. One of the leading contributors is considered to be Paraquat. For information on Paraquat Parkinson’s lawsuits, look here.
What Are The Symptoms/warning Signs Of Parkinsons Disease
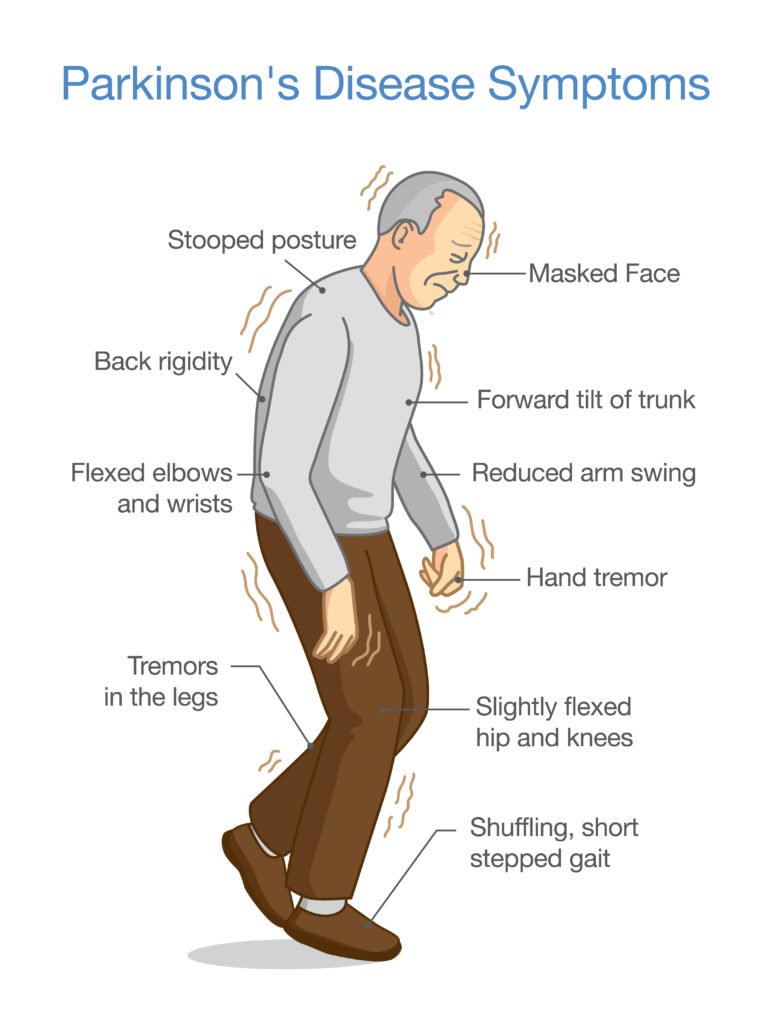
Parkinson’s disease belongs to a group of conditions called motor system disorders, which are the result of the loss of dopamine-producing brain cells. The four primary symptoms of PD are tremor, or trembling in hands, arms, legs, jaw, and face; rigidity, or stiffness of the limbs and trunk; bradykinesia, or slowness of movement; and postural instability, or impaired balance and coordination. As these symptoms become more pronounced, patients may have difficulty walking, talking, or completing other simple tasks. PD usually affects people over the age of 60. Early symptoms of PD are subtle and occur gradually. In some people the disease progresses more quickly than in others.
As the disease progresses, the shaking, or tremor, which affects most people with PD, may begin to interfere with daily activities including difficulty walking and talking. They may also have mental and behavioral changes, sleep problems, depression, memory difficulties, and fatigue.
One clear risk factor for Parkinson’s is age. Although most people with Parkinson’s first develop the disease at about age 60, about 5 to 10 percent of people with Parkinson’s have “early-onset” disease, which begins before the age of 50. Early-onset forms of Parkinson’s are often, but not always, inherited, and some forms have been linked to specific gene mutations.
Learning From Genetic Analyses Of Pd Casecontrol Studies
We analyzed the reports from 12 international studies94,157,158,159,160,161,162,163,164,165,166,167, totaling 5650 persons living with PD in North America, Europe, and Australia. We confirmed that globally only 15% of patients report a family history of PD symptoms, while the remaining 85% of the PD population are classified as sporadic PD . However, the distinction between genetic predispositions in familial and sporadic PD is blurry. No single-gene mutation in PD has a 100% penetrance. Instead, most likely, multiple genetic risk factors act in synergy to increase the chances of both familial and sporadic PD. Such genetic susceptibilities interplay with aging and environmental factors in both familial and sporadic PD.
Fig. 2: The genomics of Parkinson’s disease: prevalence and penetrance.
a In the world-wide population of people living with PD, ~85% of PD cases are sporadic and the remaining are familial . b Genetic mutations occur at low and varying frequencies in the PD world population . Data represented as the mean±SEM. c GWAS data suggests risk variants in fPD genes tend to be less prevalent in PD cases . d Single nucleotide polymorphisms in over 44 genomic regions show significant association to PD. Each point presents an independent SNP hit associated with PD.
How Environmental Factors Could Cause Parkinsons Disease
Scientists differ about the extent that brain cells are impacted by environmental factors. However, the statistics associated with the disease show that the environment can play a very large role in whether parkinson’s disease develops.
Most often, it is exposure to toxic chemicals that could play a role in the development of Parkinson’s disease. Usually, these combine with genetic factors to produce the conditions that cause Parkinson’s.
Increasing scientific evidence suggests that Parkinson’s may be caused by environmental factors such as exposure to herbicides such as Paraquat.
What Can You Do About Weight Loss Associated With Pd
If you do find yourself unable to maintain a healthy weight, discuss this with your doctor. The good news is that after a medical workup, he or she may suggest one or more of the following steps that can help you:
Tips and takeaways
- Despite a diagnosis of PD, weight loss should prompt a full medical workup.
- Weight loss that is attributed to PD can be caused by a variety of reasons including decreased appetite, increased energy expenditure, swallowing difficulties, and poor gut motility.
- Weight loss has been linked to a poorer quality of life in PD and may contribute to increasing frailty.
- There are steps you can take that may help. Depending on the causes contributing to weight loss, efforts to counteract weight loss could include consultation with a dietician, swallow evaluation and PD medication adjustment.
- As with all symptoms, discuss your concerns about weight loss with your doctor.
Do you have a question or issue that you would like Dr. Gilbert to explore?
Dr. Rebecca Gilbert
APDA Vice President and Chief Scientific Officer
The Differences Between Alzheimer’s And Parkinson’s
Do you know the differences between Alzheimer’s and Parkinson’s? First of all, we must say that both diseases constitute two of the causes of dementia. Now, let’s be a bit more specific. According to data from the WHO , dementia due to Alzheimer’s disease represents 60-70% of all cases of dementia in the world.
However, it’s important to keep in mind that they’re very different diseases. Additionally, we must make clear that having either condition doesn’t always lead to the development of dementia . In this sense, we know that between 20-60% of people with Parkinson’s disease end up developing dementia.
Buter et al. conducted a study that was published in the journal Neurology. It was conducted with 233 patients with Parkinson’s disease. The researchers were able to observe that about 60% of them developed Parkinson’s dementia in a period of 12 years.
So what’s dementia? It refers to the set of symptoms that arise as a consequence of neurological damage or disease. These symptoms involve the loss or weakening of the mental faculties and mainly affect three different areas: cognitive , behavioral , and personality .
How Many Persons Are Affected By Parkinsons Disease
Although estimates vary, about 50,000 people are diagnosed with PD in the U.S. each year and about half a million people have the disease. It is anticipated that nearly one million persons will be living with PD in the U.S. by 2020. Both men and women can have Parkinson’s disease. However, the disease affects about 50 percent more men than women. Because the rate of PD increases in older adults, the burden will increase unless prevention and treatment improve.
Estimated Healthcare Costs Related To Pd In The Us
The combined direct and indirect cost of Parkinson’s, including treatment, social security payments and lost income, is estimated to be nearly $52 billion per year in the United States alone.
Medications alone cost an average of $2,500 a year and therapeutic surgery can cost up to $100,000 per person.
The Impact Of Parkinsons Disease On Overall Health
Based on the Blue Cross Blue Shield Health Index, the overall health of those affected by Parkinson’s is significantly lower than the general population. In 2017, the average BCBS Health Index for someone aged 30-64 with Parkinson’s was 57, compared to 88 for the entire commercially insured population in this age range. This translates to an average of 10.7 years of healthy life lost for those with the condition compared to 3.4 years for the 30-64 population as a whole.4
Caring for someone with Parkinson’s Disease
The majority of Parkinson’s patients are cared for by informal caregivers, such as a family member. The physical, mental and emotional work this requires can be significant. The Impact of Caregiving on Mental and Physical Health found that caregivers have 26% poorer health compared to a benchmark population, as measured by the BCBS Health Index. In addition, a national survey conducted by the Blue Cross Blue Shield Association found that 1 in 4 unpaid caregivers are feeling more stress trying to balance work and family due to COVID-19.5
Sidebar: Ninds Steps Up Pursuit Of Pd Biomarkers

In 2012, the NINDS dramatically accelerated efforts to identify biomarkers by establishing the Parkinson’s Disease Biomarkers Program . This unprecedented program unites a range of stakeholders from basic and clinical researchers to healthcare professionals, the NINDS staff, information technology experts, and people living with PD and their families.
PDBP supports research and builds resources aimed at accelerating the discovery of biomarkers to ultimately slow the progression of PD. For example, the program has established a repository of biological specimens and a Data Management Resource system maintained by the NIH Center for Information Technology. The DMR allows researchers to access clinical, imaging, genetic, and biologic data, while a complementary PDBP-supported project develops statistical tools to analyze vast quantities of data so that patterns can be identified across these diverse sources of information.
Epigenomic Alterations Linked With Pd In Patient
The ability to capture unique epigenomic alterations associated with PD remains an important challenge. Reprogramming fibroblasts to iPSCs may erase age-associated225 and naive epigenetic signatures which could contribute to sporadic PD pathophysiology226. However, an epigenetic phenotype was reported in iPSC-derived PD patient neurons79,89. Neuronal lines derived from LRRK2 and sporadic patients exhibited epigenomic alterations when compared with healthy controls79. Hypermethylation was prominent in gene regulatory regions associated with the downregulation of transcription factors FOXA1, NR3C1, HNF4A, and FOSL279. Interestingly, LRRK2 mutant and sporadic PD patient neurons shared similar methylation patterns, which were absent in the original donor fibroblasts79. A spontaneous increase in the number of DNA strand breaks and genomic damage89 in PD patient-derived neurons could indirectly impact genomic regulation.
How Many People Does Parkinsons Disease Affect
Parkinson’s disease affects 1 in every 500 people in Canada. Over 100,000 Canadians are living with Parkinson’s today and approximately 6,600 new cases of PD are diagnosed each year in Canada . Most are diagnosed over the age of 60; however, at least 10% of the Parkinson’s population develops symptoms before the age of 50. Approximately four million people worldwide are living with the condition.
Diagnosis And Management Of Parkinsons Disease
There are no diagnostic tests for Parkinson’s. X-rays, scans and blood tests may be used to rule out other conditions. For this reason, getting a diagnosis of Parkinson’s may take some time.
No two people with Parkinson’s disease will have exactly the same symptoms or treatment. Your doctor or neurologist can help you decide which treatments to use.
People can manage their Parkinson’s disease symptoms through:
- seeing a Doctor who specialises in Parkinson’s
- medication
- multidisciplinary therapy provided for example, by nurses, allied health professionals and counsellors
- deep brain stimulation surgery .
Medications For People With Parkinsons Disease

Symptoms of Parkinson’s disease result from the progressive degeneration of nerve cells in the brain and other organs such as the gut, which produce a neurotransmitter called dopamine. This causes a deficiency in the availability of dopamine, which is necessary for smooth and controlled movements. Medication therapy focuses on maximising the availability of dopamine in the brain. Medication regimes are individually tailored to your specific need. Parkinson’s medications fit into one of the following broad categories:
- levodopa – dopamine replacement therapy
- dopamine agonists – mimic the action of dopamine
- COMT inhibitors – used along with levodopa. This medication blocks an enzyme known as COMT to prevent levodopa breaking down in the intestine, allowing more of it to reach the brain
- anticholinergics – block the effect of another brain chemical to rebalance its levels with dopamine
- amantadine – has anticholinergic properties and improves dopamine transmission
- MAO type B inhibitors – prevent the metabolism of dopamine within the brain.
Generating Relevant Neuronal Cell Types For Pd
The cellular reprogramming toolbox for researchers is rapidly expanding and includes a panoply of neuronal differentiation protocols to generate cells representing various brain regions21. PD is a debilitating motor system disorder resulting from the selective degeneration of midbrain dopamine neurons located in the substantia nigra pars compacta. Protocols have been established to specifically generate dopaminergic neurons and brain cells with a midbrain molecular profile195,196.
Why Worry About Weight Loss Associated With Pd
Weight loss has been linked to a poorer quality of life and more rapid progression of PD. The reasons for this are two-fold. On the one hand, as outlined in the list above, weight loss can be a hallmark of advancing disease – as it could be a consequence of more swallowing difficulties, worsened mobility, more impaired gut function etc.
On the other hand, having weight loss can further lead to poorer health. Inadequate food intake can contribute to malnutrition and vitamin deficiencies. Malnutrition can subsequently be the cause of increased susceptibility to infection, increased fatigue and increased frailty. The situation can spiral with more fatigue and frailty causing a further decrease in activity and function.
Osteoporosis, or porous and fragile bones, is more common in under-weight people since bone structure is dependent on weight-bearing. Since osteoporotic bones are more prone to fracture during a fall, this too can be a contributor to more disability and frailty. Bottom line is that it is important for your health to maintain a healthy weight.
