What Are Pd Dementia Safety Concerns
Safety issues should be considered and monitored from the time of diagnosis. As PDD progresses, ensure that your loved one is not left alone.
- Evaluate driving privileges before safety is a concern. Your doctor can make a driving evaluation referral.
- Work out legal and financial issues and safeguard finances. People with dementia are at greater risk of falling victim to scams and fraud.
- Minimize prescription risks. Confirm with the doctor the medication names and doses of the person with PD. If the person is in dementias early stages and capable, fill up their weekly pill box together and monitor use.
- Medical alert systems can be critical in case your loved one falls or wanders outside of the home. Many types of systems are available, from bracelets and pendants to smart watches with fall detection and one-button connections to 911.
- Evaluate gun safety. If your loved one owns a firearm or has one in the home, consider speaking with their doctor about the subject and taking appropriate safety precautions.
Are There Medicines To Treat Pdd
Though there is no cure for PDD yet, there are medications that help manage the symptoms. These medications are called cholinesterase inhibitors, and they can help if a person with PDD is having memory problems. Some examples of these medicines are donepezil, rivastigmine and galantamine. Sleep problems may be managed by sleep medications such as melatonin.
Because people with PDD are usually very sensitive to medications, any new medication, even one that is not being used for the brain, needs to be reviewed with the persons provider to avoid potential contraindication.
Management Of Dementia In Parkinsonism
There is some evidence that cholinesterase inhibitors may have antipsychotic properties for the management of behavioral symptoms in Parkinsonism. A number of open-label studies have documented the beneficial effects of donepezil and rivastigmine in the management of dementia in Parkinsonism. A large placebo-controlled study of rivastigmine found that the rivastigmine group had significant improvement of the neuropsychiatric symptoms than the control group and were less likely to develop hallucinations. Furthermore, patients who suffered from visual hallucination at the time of initiation of treatment benefited the most.
The management of psychosis in DLB is equally frustrating and only a prospective randomized study in this regard has been reported to date. Rivastigmine led to significant improvement in delusions, hallucinations, depression, and apathy; and therefore, cholinesterase inhibitors are now recommended as the first line of management for this condition. Mementine has also been found useful in one small retrospective study. However, cholinesterase inhibitors can increase tremor in Parkinsonism by their procholinergic actions.
One of the major problems of management of psychosis and related problems in Parkinsonism is that stopping drugs often lead to worsening of symptoms. However, some trials show that patients can be switched from clozapine to quetiapine after stability has been earned, provided they responded earlier to the latter agent.
What Is Needed For A Parkinson’s Disease Dementia Diagnosis
There is no definitive medical test that confirms cognitive decline or dementia in Parkinson’s disease. The most accurate way to measure cognitive decline is through neuropsychological testing.
- The testing involves answering questions and performing tasks that have been carefully designed for this purpose. It is carried out by a specialist in this kind of testing.
- Neuropsychological testing addresses the individual’s appearance, mood, anxiety level, and experience of delusions or hallucinations.
- It assesses cognitive abilities such as memory, attention, orientation to time and place, use of language, and abilities to carry out various tasks and follow instructions.
- Reasoning, abstract thinking, and problem solving are tested.
- Neuropsychological testing gives a more accurate diagnosis of the problems and thus can help in treatment planning.
- The tests are repeated periodically to see how well treatment is working and check for new problems.
Imaging studies: Generally, brain scans such as CT scan and are of little use in diagnosing dementia in people with Parkinson’s disease. Positron emission tomographic scan may help distinguish dementia from depression and similar conditions in Parkinson’s disease.
Where To Get Help

- Your local community health service
- Your local council
- National Dementia Helpline Dementia Australia Tel. 1800 100 500
- Aged Care Assessment Services Tel. 1300 135 090
- My Aged Care Tel. 1800 200 422
- Cognitive Dementia and Memory Service clinics Tel. 1300 135 090
- Carers Victoria Tel. 1800 242 636
- Commonwealth Respite and Carelink Centres Tel 1800 052 222
- Dementia Behaviour Management Advisory Service Tel. 1800 699 799 for 24-hour telephone advice for carers and care workers
How Can We Manage Hallucinations
It may not be necessary to treat all hallucinations of a person with PDD. Hallucinations are often harmless, and it is okay to allow them to happen, as long as they are not disruptive or upsetting to the person or surroundings. Sometimes, recognizing the hallucination and then switching the topic might be an efficient way of handling frustrations that occur because of a hallucination. If hallucinations need medical treatment, your provider may be able to discuss and suggest some options. However, many of the medications used to treat hallucinations may make movement symptoms worse.
What Is Parkinson Disease
Parkinson disease is a movement disorder. It can cause the muscles to tighten and become rigid This makes it hard to walk and do other daily activities. People with Parkinsons disease also have tremors and may develop cognitive problems, including memory loss and dementia.
Parkinson disease is most common in people who are older than 50. The average age at which it occurs is 60. But some younger people may also get Parkinson disease. When it affects someone younger than age 50, it’s called early-onset Parkinson disease. You may be more likely to get early-onset Parkinson disease if someone in your family has it. The older you are, the greater your risk of developing Parkinson disease. It’s also much more common in men than in women.
Parkinson disease is a chronic and progressive disease. It doesn’t go away and continues to get worse over time.
What Happens In Pdd
People with PDD may have trouble focusing, remembering things or making sound judgments. They may develop depression, anxiety or irritability. They may also hallucinate and see people, objects or animals that are not there. Sleep disturbances are common in PDD and can include difficulties with sleep/wake cycle or REM behavior disorder, which involves acting out dreams.
PDD is a disease that changes with time. A person with PDD can live many years with the disease. Research suggests that a person with PDD may live an average of 57 years with the disease, although this can vary from person to person.
Frontotemporal Dementia With Parkinsonism
One form of familial FTD, also known as frontotemporal dementia with Parkinsonism-17 , is caused by genetic changes in the gene for tau protein, located on chromosome 17. No other risk factors for this condition are known.
FTDP-17 is rare and accounts for only three per cent of all cases of dementia. Symptoms progressively get worse over time and usually appear between the ages of 40 and 60. The condition affects both thinking and behavioural skills and movements such as rigidity, lack of facial expression and problems with balance .
It can be distressing to be told that you have a genetic disorder or are at risk of having one. Genetic counselling provides the person and their family with information about a genetic disorder and its likely impact on their lives. This can assist a person with FTDP-17 to make informed medical and personal decisions about how to manage their condition and the challenges it presents to their health and wellbeing. Prenatal genetic counselling is also available for parents to help them decide about a pregnancy that may be at risk of FTDP-17.
Coping With Dietary Problems
Many people with Parkinsons experience various eating and dietary problems, such as constipation, chewing and swallowing difficulties, and upset stomach. The following tips can help you minimize the symptoms.
If you suffer from constipation Drink lots of water and eat fiber-rich foods, including beans, brown rice, whole grains, and fruit.
If you have trouble chewing or swallowing food Cut foods into smaller portions to avoid choking and to encourage digestion, and remain upright for 30 minutes after eating.
If youre struggling with fatigueLimit the amount of sugar youre eating. Also avoid alcohol and caffeine, especially before bed, as they can reduce the quality of your sleep.
If you take levodopa Dont eat meat or other protein-rich foods for at least 30-60 minutes after taking levodopa, as protein blocks your bodys ability to absorb the medication.
If your medication gives you an upset stomach Take your medication with a full glass of water and a small non-protein based snack, such as a piece of toast or fruit.
Some Parkinsons disease medications need to be taken promptly at specified times before or after eating, so it can also help to establish a regular routine for meal and medication times.
Lewy Body Dementia: A Common Yet Underdiagnosed Dementia
While its not a household word yet, Lewy body dementia is not a rare disease. It affects an estimated 1.4 million individuals and their families in the United States. Because LBD symptoms can closely resemble other more commonly known disorders like Alzheimers disease and Parkinsons, it is often underdiagnosed or misdiagnosed. In fact, many doctors or other medical professionals still are not familiar with LBD.
What Is Parkinsons Disease
Parkinsons disease is a condition in which a part of the brain called the substantia nigra loses nerve cells. This loss of nerve cells results in a reduction of a substance called dopamine which is important for the regulation of movement of the body. As the dopamine levels decrease the persons movements become slower. Most people with a diagnosis of Parkinsons do not go on to develop dementia although about a third will, usually in the later stages. This is known as Parkinsons disease with dementia and may also be referred to as Lewy body dementia.
It is estimated that Parkinsons disease affects about 1 in 500 people and it is currently thought that it may be due to a combination of genetic and environmental causes. About one fifth of people diagnosed with Parkinsons disease are under 40 years old but it is more common in the over 50s.
Do You Die From Pd Dementia
People with Parkinsons-related dementia often want to know how the disease can impact their lifespan. While people with Parkinsons can expect a similar lifespan to the general population, studies show both Parkinsons disease dementia and Lewy body dementia can shorten lifespan, generally due to medical complications from the disease, rather than the disease itself.
Parkinson’s Disease Dementia Follow
A person with Parkinson’s disease and dementia requires regular checkups with his or her health care professional.
- These checkups allow the health care professional to see how well treatment is working and make adjustments as necessary.
- They allow detection of new problems of cognition, mood, or behavior that could benefit from treatment.
- These visits also give the family caregiver an opportunity to discuss problems in the individual’s care.
Eventually, the person with Parkinson’s disease and dementia will likely become unable to care for himself or herself or even to make decisions about his or her care if the patient lives long enough with Parkinson’s disease and dementia.
- It is best for the person to discuss future care arrangements with family members as early as possible, so that his or her wishes can be clarified and documented for the future.
- A health care professional can advise patients and caregivers about legal arrangements that should be made to ensure that these wishes are observed.
Parkinson’s disease dementia prevention
There is no known way of preventing dementia in Parkinson’s disease. However, patients with Parkinson’s disease are urged to continue to exercise and live a healthy lifestyle as this may delay or reduce the onset of dementia, although there is no good data to indicate this will occur.
Parkinson’s disease dementia prognosis
How Is Parkinson Disease Treated
Parkinson disease can’t be cured. But there are different therapies that can help control symptoms. Many of the medicines used to treat Parkinson disease help to offset the loss of the chemical dopamine in the brain. Most of these medicines help manage symptoms quite successfully.
A procedure called deep brain stimulation may also be used to treat Parkinson disease. It sends electrical impulses into the brain to help control tremors and twitching movements. Some people may need surgery to manage Parkinson disease symptoms. Surgery may involve destroying small areas of brain tissue responsible for the symptoms. However, these surgeries are rarely done since deep brain stimulation is now available.
Parkinsons Disease Symptoms Of Dementia
Up to one-third of people living with Parkinson’s disease experience dementia, according to the Parkinson’s Disease Foundation. Problems with dementia may include trouble with memory, attention span, and what is called executive function the process of making decisions, organizing, managing time, and setting priorities.
RELATED: 12 Famous People With Parkinson’s Disease
What Is Lewy Body Dementia Causes Symptoms And Treatments
On this page:
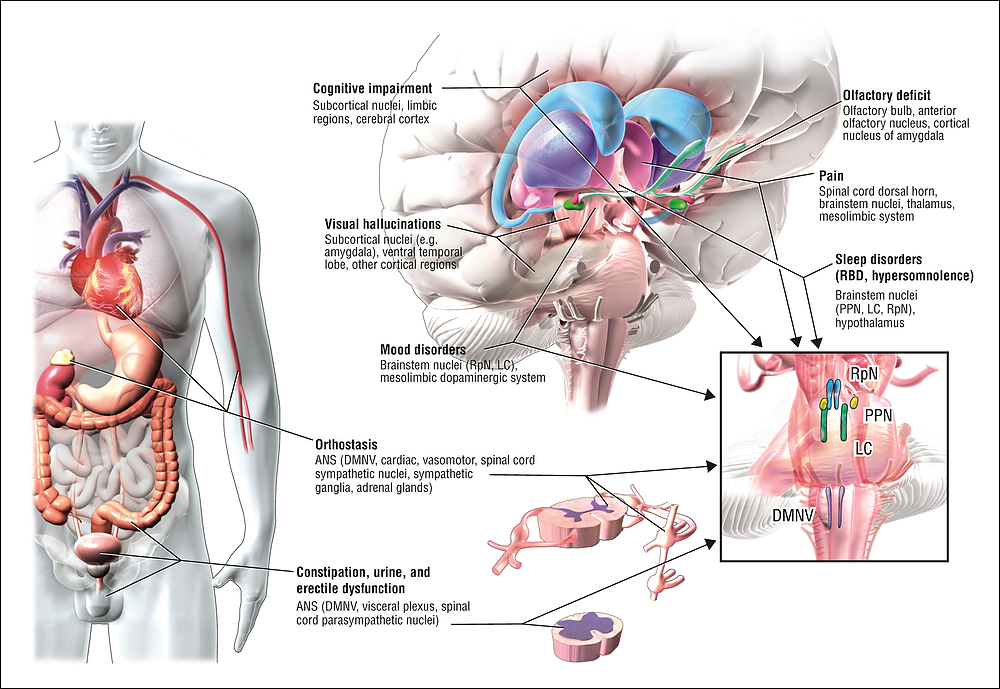
Lewy body dementia is a disease associated with abnormal deposits of a protein called alpha-synuclein in the brain. These deposits, called Lewy bodies, affect chemicals in the brain whose changes, in turn, can lead to problems with thinking, movement, behavior, and mood. Lewy body dementia is one of the most common causes of dementia.
LBD affects more than 1 million individuals in the United States. People typically show symptoms at age 50 or older, although sometimes younger people have LBD. LBD appears to affect slightly more men than women.
Diagnosing LBD can be challenging. Early LBD symptoms are often confused with similar symptoms found in other brain diseases or in psychiatric disorders. Lewy body dementia can occur alone or along with other brain disorders.
It is a progressive disease, meaning symptoms start slowly and worsen over time. The disease lasts an average of five to eight years from the time of diagnosis to death, but can range from two to 20 years for some people. How quickly symptoms develop and change varies greatly from person to person, depending on overall health, age, and severity of symptoms.
In the early stages of LBD, symptoms can be mild, and people can function fairly normally. As the disease advances, people with LBD require more help due to a decline in thinking and movement abilities. In the later stages of the disease, they often depend entirely on others for assistance and care.
Comparison With Other Dementias
Dementia is the result of physical changes in the brain that can lead to memory loss and an inability to think clearly.
Several types of dementia exist, including:
PD dementia has different symptoms to other types.
Alzheimers dementia, for example, impairs memory and language. PD dementiam on the other hand, affects problem-solving, the speed at which thoughts occur, memory, and mood, alongside other important cognitive functions.
Dementia with Lewy bodies and Parkinsons disease dementia are similar in that the Lewy Bodies might be present in both forms.
However, whether the disease causes Lewy bodies or if Lewy bodies cause the disease symptoms is unclear. Researchers also believe that the way the Lewy bodies form in Parkinsons disease dementia is different from those in Lewy body dementia.
What Other Things Help
There are various ways to help a person with PDD. Speech therapy may help improve communication between people with PDD and others. Physical therapy may help strengthen and stretch stiff muscles and help to prevent falls.
Research has shown that physical exercise helps to enhance brain health and improves mood and general fitness. A balanced diet, enough sleep and limited alcohol intake are other important ways to promote good brain health. Other illnesses that affect the brain, such as diabetes, high blood pressure and high cholesterol, should also be treated if present.
Living With Parkinsons Disease
Depending on severity, life can look very different for a person coping with Parkinsons Disease. As a loved one, your top priority will be their comfort, peace of mind and safety. Dr. Shprecher offered some advice, regardless of the diseases progression. Besides movement issues Parkinsons Disease can cause a wide variety of symptoms including drooling, constipation, low blood pressure when standing up, voice problems, depression, anxiety, sleep problems, hallucinations and dementia. Therefore, regular visits with a neurologist experienced with Parkinsons are important to make sure the diagnosis is on target, and the symptoms are monitored and addressed. Because changes in your other medications can affect your Parkinsons symptoms, you should remind each member of your healthcare team to send a copy of your clinic note after every appointment.
Dr. Shprecher also added that maintaining a healthy diet and getting regular exercise can help improve quality of life. Physical and speech therapists are welcome additions to any caregiving team.
Apda In Your Community
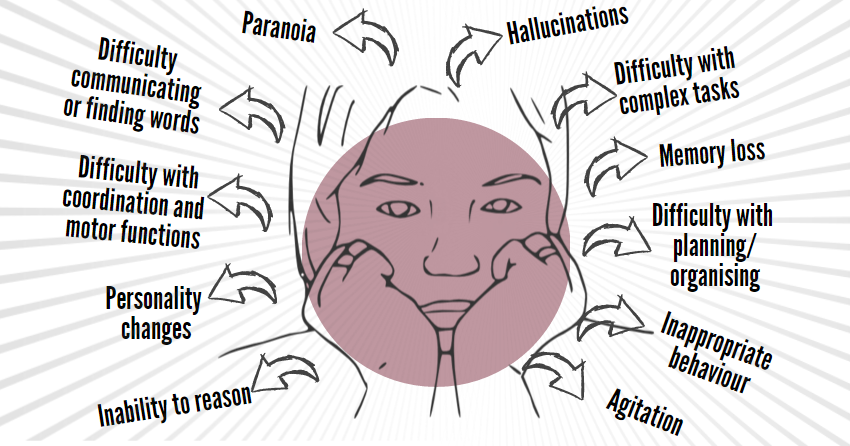
APDAParkinson’s Disease SymptomsLewy Bodies, Dementia, and Parkinsons What Does it all Mean?
Here are two common scenarios that may sound familiar:
Scenario 1A patient develops a series of neurologic symptoms, is evaluated by a neurologist and is told that she has Parkinsons disease . She then visits another neurologist for a second opinion and is told she has Lewy Body Dementia .
Scenario 2A patient has his first visit with his neurologist and is told that he has PD, at a subsequent visit the diagnosis is changed to Parkinsons disease dementia , and at a follow up visit the diagnosis is changed yet again to Dementia with Lewy Bodies .
Both of these situations understandably cause great uncertainty and frustration.
What Causes Lewy Body Dementia
The causes of LBD are not yet well understood, but research is ongoing in this area. There are probably multiple factors involved, including genetic and environmental risk factors that combine with natural aging processes to make someone susceptible to LBD.
For more information, visit www.lbda.org.
Modified with permission from the Lewy Body Dementia Association
To learn more about motor symptoms related to Parkinsons, visit here.
To learn more about non-motor symptoms related to Parkinsons, visit here.
Treatments For Dementia With Lewy Bodies
There’s currently no cure for dementia with Lewy bodies or any treatment that will slow it down.
But there are treatments that can help control some of the symptoms, possibly for several years.
Treatments include:
- medicines to reduce hallucinations, confusion, drowsiness, movement problems and disturbed sleep
- therapies such as physiotherapy, occupational therapy and speech and language therapy for problems with movement, everyday tasks, and communication
- psychological therapies, such as cognitive stimulation
- dementia activities, such as memory cafes
Diagnosis Of Probable Pdd
A diagnosis of probable PDD was made according to the Movement Disorder Society Level 1 criteria., Probable PDD was diagnosed when all the following five criteria were satisfied:
Diagnosis of PD according to United Kingdom Parkinsons Disease Society Brain Bank Criteria.
The development of PD prior to the onset of dementia: This information was gathered by clinicians involved in assessing participants.
PD associated with a decreased global cognitive efficiency: This was defined by a cut of score of 25 on the Mini Mental Status Examination .
Cognitive deficiency severe enough to impair daily life: The foundation of a PDD diagnosis is that the cognitive decline contributes to functional impairments most commonly observed in the activities of daily living . In the UK clinics, this was defined by the Clinical Impression of Severity Index for Parkinsons Disease . The cognitive status scale of this tool assesses the impact of cognitive decline on ADLs. The scale is scored 06, with 4 or higher suggesting that help is needed for ADLs, including help with basic daily activities. As such, any patient scoring 4 or higher met this criterion. In the Australian clinic, item 1.1 of the MDS-UPDRS was used. The scale is scored between 0 and 4 with a score of 2 or higher suggesting help is needed for ADLs, even if only minimal. As such, any patient scoring 2 or higher met this criterion.
Delusions From Parkinsons Disease
Delusions affect only about 8 percent of people living with PD. Delusions can be more complex than hallucinations. They may be more difficult to treat.
Delusions often start as confusion that develops into clear ideas that arent based on reality. Examples of the types of delusions people with PD experience include:
- Jealousy or possessiveness. The person believes someone in their life is being unfaithful or disloyal.
- Persecutory. They believe that someone is out to get them or harm them in some way.
- Somatic. They believe they have an injury or other medical problem.
- Guilt. The person with PD has feelings of guilt not based in real behaviors or actions.
- Mixed delusions. They experience multiple types of delusions.
Paranoia, jealousy, and persecution are the most commonly reported delusions. They can pose a safety risk to caregivers and to the person with PD themselves.
PD isnt fatal, though complications from the disease can contribute to a shorter expected life span.
Dementia and other psychosis symptoms like hallucinations and delusions do contribute to increased hospitalizations and increased rates of death .
One study from 2010 found that people with PD who experienced delusions, hallucinations, or other psychosis symptoms were about 50 percent more likely to die early than those without these symptoms.
But early prevention of the development of psychosis symptoms may help increase life expectancy in people with PD.
Dealing With Cognitive Impairments
In some circumstances medications can help to lessen cognitive symptoms. You should speak to your GP or specialist about the options available. There are also various other health professionals who can provide professional support for dealing with cognitive impairments.
Cognitive impairment can be a big challenge for family, friends and carers, as well as those with the symptoms. Some practical tips for dealing with the daily challenges of cognitive impairments include:
- Keep to a daily routine
- Try to use familiar objects and phrases
- Avoid unfamiliar environments
Parkinson’s Disease Symptoms: Life Expectancy
Even though Parkinson’s disease is a serious, progressive condition, it is not considered a fatal illness. People who have Parkinson’s disease usually have the same average life expectancy as people without the disease.
But when the disease is in its advanced stages, Parkinson’s symptoms can lead to life-threatening complications, including:
- Falls that lead to fractured bones
- Pneumonia
- Choking
Thinking about the progression of Parkinson’s disease can be frightening. But proper treatments can help you live a full, productive life for years to come. And researchers hope to one day find ways to halt the progression of Parkinson’s and restore lost functioning.
How Is Parkinsons Dementia Different From Alzheimers Disease
The advanced cognitive changes that impact daily living in Alzheimers and Parkinsons disease are both types of dementia.
Parkinsons disease dementia can occur as Parkinsons advances, after several years of motor symptoms. Dementia with Lewy Bodies is diagnosed when cognitive decline happens first, or when Parkinsons motor symptoms and cognitive decline occur and progress closely together. Cognitive impairments in PDD, combined with the movement symptoms of the disease, produce a greater impact on social and occupational functioning than Alzheimers.
Alzheimers, a fatal brain disease, causes declines in memory, thinking and reasoning skills. Physicians can diagnose Alzheimers. Visit the Alzheimers Association to learn the 10 signs Alzheimers disease.
Fortunately for people with PD, Parkinsons disease dementia is less disabling than Alzheimers disease. People with Alzheimers have language difficulties earlier than people with Parkinsons, and no new memories are formed. People with PD also have more ability to compensate and adjust based on cues.
What Are The Treatments For Lewy Body Dementia
There is no cure for LBD, but treatments can help with the symptoms:
- Medicines may help with some of the cognitive, movement, and psychiatric symptoms
- Physical therapy can help with movement problems
- Occupational therapy may help find ways to more easily do everyday activities
- Speech therapy may help with swallowing difficulties and trouble speaking loudly and clearly
- Mental health counseling can help people with LBD and their families learn how to manage difficult emotions and behaviors. It can also help them plan for the future.
- Music or art therapy may reduce anxiety and improve well-being
Support groups can also be helpful for people with LBD and their caregivers. Support groups can give emotional and social support. They are also a place where people can share tips about how to deal with day-to-day challenges.
NIH: National Institute of Neurological Disorders and Stroke
